Abstract
Purpose of Review
Breast cancer is the most common cancer diagnosed among US women. Air pollution is a pervasive mixture of chemicals containing carcinogenic compounds and chemicals with endocrine-disrupting properties. In the present review, we examine the epidemiologic evidence regarding the association between air pollution measures and breast cancer risk.
Recent Findings
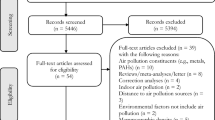
We identified 17 studies evaluating the risk of breast cancer associated with air pollution. A higher risk of breast cancer has been associated with nitrogen dioxide (NO2) and nitrogen oxide (NOx) levels, both of which are proxies for traffic exposure. However, there is little evidence supporting a relationship for measures of traffic count or distance to nearest road, or for measures of particulate matter (PM), except potentially for nickel and vanadium, which are components of PM10. Hazardous air toxic levels and sources of indoor air pollution may also contribute to breast cancer risk. There is little existing evidence to support that the relationship between air pollution and breast cancer risk varies by either menopausal status at diagnosis or combined tumor hormone receptor subtype defined by the estrogen receptor (ER) and progesterone receptor (PR).
Summary
Epidemiologic evidence to date suggests an association between breast cancer risk and NO2 and NOx, markers for traffic-related air pollution, although there was little evidence supporting associations for proxy measures of traffic exposure or for PM. More research is needed to understand the role of specific PM components and whether associations vary by tumor receptor subtype and menopausal status at diagnosis.
Similar content being viewed by others
References
Papers of particular interest, published recently, have been highlighted as: • Of importance •• Of major importance
Siegel RL, Miller KD, Jemal A. Cancer statistics, 2017. CA Cancer J Clin. 2017;67(1):7–30.
IOM. Washington, DC: Institute of Medicine, the National Academies. Breast cancer and the environment: a life course approach. 2011. Available: https://www.nap.edu/catalog/13263/breast-cancer-and-the-environment-a-life-course-approach. Accessed 22 March 2018.
Hamra GB, Laden F, Cohen AJ, Raaschou-Nielsen O, Brauer M, Loomis D. Lung cancer and exposure to nitrogen dioxide and traffic: a systematic review and meta-analysis. Environ Health Perspect. 2015;123(11):1107–12.
Loomis D, Grosse Y, Lauby-Secretan B, El Ghissassi F, Bouvard V, Benbrahim-Tallaa L, et al. The carcinogenicity of outdoor air pollution. Lancet Oncol. 2013;14(13):1262–3.
Hill P, Wynder EL. Nicotine and cotinine in breast fluid. Cancer Lett. 1979;6(4–5):251–4.
White AJ, Bradshaw PT, Herring AH, Teitelbaum SL, Beyea J, Stellman SD, et al. Exposure to multiple sources of polycyclic aromatic hydrocarbons and breast cancer incidence. Environ Int. 2016;90:185–92.
International Agency for Research on Cancer. Some non-heterocyclic polycyclic aromatic hydrocarbons and some related exposures. IARC Monogr Eval Carcinog Risks Hum. 2010;92:35–818.
Sievers CK, Shanle EK, Bradfield CA, Xu W. Differential action of monohydroxylated polycyclic aromatic hydrocarbons with estrogen receptors alpha and beta. Toxicol Sci. 2013;132(2):359–67.
Byrne C, Divekar SD, Storchan GB, Parodi DA, Martin MB. Metals and breast cancer. J Mammary Gland Biol Neoplasia. 2013;18(1):63–73.
Wang T, Feng W, Kuang D, Deng Q, Zhang W, Wang S, et al. The effects of heavy metals and their interactions with polycyclic aromatic hydrocarbons on the oxidative stress among coke-oven workers. Environ Res. 2015;140:405–13.
Adams K, Greenbaum DS, Shaikh R, van Erp AM, Russell AG. Particulate matter components, sources, and health: systematic approaches to testing effects. J Air Waste Manage Assoc. 2015;65(5):544–58.
Chen ST, Lin CC, Liu YS, Lin C, Hung PT, Jao CW, et al. Airborne particulate collected from Central Taiwan induces DNA strand breaks, poly(ADP-ribose) polymerase-1 activation, and estrogen-disrupting activity in human breast carcinoma cell lines. J Environ Sci Health A Tox Hazard Subst Environ Eng. 2013;48(2):173–81.
Huff JE, Haseman JK, DeMarini DM, Eustis S, Maronpot RR, Peters AC, et al. Multiple-site carcinogenicity of benzene in Fischer 344 rats and B6C3F1 mice. Environ Health Perspect. 1989;82:125–63.
White AJ, Chen J, Teitelbaum SL, McCullough LE, Xu X, Hee Cho Y, et al. Sources of polycyclic aromatic hydrocarbons are associated with gene-specific promoter methylation in women with breast cancer. Environ Res. 2016;145:93–100.
Binachon B, Dossus L, Danjou AM, Clavel-Chapelon F, Fervers B. Life in urban areas and breast cancer risk in the French E3N cohort. Eur J Epidemiol. 2014;29(10):743–51.
Reynolds P, Hurley S, Goldberg DE, Anton-Culver H, Bernstein L, Deapen D, et al. Regional variations in breast cancer among California teachers. Epidemiology. 2004;15(6):746–54.
Parikh PV, Wei Y. PAHs and PM2.5 emissions and female breast cancer incidence in metro Atlanta and rural Georgia. Int J Environ Health Res. 2016;26(4):458–66.
Chen F, Bina WF. Correlation of white female breast cancer incidence trends with nitrogen dioxide emission levels and motor vehicle density patterns. Breast Cancer Res Treat. 2012;132(1):327–33.
Wei Y, Davis J, Bina WF. Ambient air pollution is associated with the increased incidence of breast cancer in US. Int J Environ Health Res. 2012;22(1):12–21.
Goldberg MS, Labreche F, Weichenthal S, Lavigne E, Valois MF, Hatzopoulou M, et al. The association between the incidence of postmenopausal breast cancer and concentrations at street-level of nitrogen dioxide and ultrafine particles. Environ Res. 2017;158:7–15.
Mordukhovich I, Beyea J, Herring AH, Hatch M, Stellman SD, Teitelbaum SL, et al. Vehicular traffic-related polycyclic aromatic hydrocarbon exposure and breast cancer incidence: the Long Island breast cancer study project (LIBCSP). Environ Health Perspect. 2016;124(1):30–8.
•• Hystad P, Villeneuve PJ, Goldberg MS, Crouse DL, Johnson K. Exposure to traffic-related air pollution and the risk of developing breast cancer among women in eight Canadian provinces: a case-control study. Environ Int. 2015;74:240–8. Used three different modeling approaches for ambient NO2 concentrations and found consistent associations across all three assessments.
White AJ, Teitelbaum SL, Stellman SD, Beyea J, Steck SE, Mordukhovich I, et al. Indoor air pollution exposure from use of indoor stoves and fireplaces in association with breast cancer: a case-control study. Environ Health. 2014;13(108):13–108.
Crouse DL, Goldberg MS, Ross NA, Chen H, Labreche F. Postmenopausal breast cancer is associated with exposure to traffic-related air pollution in Montreal, Canada: a case-control study. Environ Health Perspect. 2010;118(11):1578–83.
Nie J, Beyea J, Bonner MR, Han D, Vena JE, Rogerson P, et al. Exposure to traffic emissions throughout life and risk of breast cancer: the western New York exposures and breast cancer (WEB) study. Cancer Causes Control. 2007;18(9):947–55.
Bonner MR, Han D, Nie J, Rogerson P, Vena JE, Muti P, et al. Breast cancer risk and exposure in early life to polycyclic aromatic hydrocarbons using total suspended particulates as a proxy measure. Cancer Epidemiol Biomark Prev. 2005;14(1):53–60.
Lewis-Michl EL, Melius JM, Kallenbach LR, Ju CL, Talbot TO, Orr MF. Breast cancer risk and residence near industry or traffic in Nassau and Suffolk counties, Long Island, New York. Arch Environ Health: Int J. 1996;51(4):255–65.
•• Andersen ZJ, Stafoggia M, Weinmayr G, Key T. Long-term exposure to ambient air pollution and incidence of postmenopausal breast cancer in 15 European cohorts within the ESCAPE project. 2017. Pooled analysis of European cohort studies with extensive exposure information including novel consideration of PM elemental composition.
Shmuel S, White AJ, Sandler DP. Residential exposure to vehicular traffic-related air pollution during childhood and breast cancer risk. Environ Res. 2017;159:257–63.
Andersen ZJ, Ravnskjær L, Andersen KK, Loft S, Brandt J, Becker T et al. Long-term exposure to fine particulate matter and breast cancer incidence in the Danish nurse cohort study. Cancer epidemiology and prevention biomarkers. 2016:cebp 0578.2016
• Hart JE, Bertrand KA, DuPre N, James P, Vieira VM, Tamimi RM, et al. Long-term particulate matter exposures during adulthood and risk of breast cancer incidence in the Nurses’ health study II prospective cohort. Cancer Epidemiol Biomarkers Prev. 2016;25(8):1274–6. Large US cohort study with menopausal status and hormone receptor subtype information and multiple air pollution measurements.
• Reding KW, Young MT, Szpiro AA, Han CJ, DeRoo LA, Weinberg C, et al. Breast Cancer risk in relation to ambient air pollution exposure at residences in the sister study cohort. Cancer Epidemiol Biomarkers Prev. 2015;24(12):1907–9. Large US cohort study with menopausal status and hormone receptor subtype information and multiple air pollution measurements.
Liu R, Nelson DO, Hurley S, Hertz A, Reynolds P. Residential exposure to estrogen disrupting hazardous air pollutants and breast cancer risk: the California teachers study. Epidemiology. 2015;26(3):365–73.
Garcia E, Hurley S, Nelson DO, Hertz A, Reynolds P. Hazardous air pollutants and breast cancer risk in California teachers: a cohort study. Environ Health. 2015;14(14):14.
• White AJ, Sandler DP. Indoor wood-burning stove and fireplace use and breast Cancer in a prospective cohort study. Environmental health perspectives. 2017;125(7):077011. First prospective study on indoor air pollution and breast cancer risk.
Raaschou-Nielsen O, Andersen ZJ, Hvidberg M, Jensen SS, Ketzel M, Sørensen M, et al. Air pollution from traffic and cancer incidence: a Danish cohort study. Environ Health. 2011;10(1):67.
Jerrett M, Arain A, Kanaroglou P, Beckerman B, Potoglou D, Sahsuvaroglu T, et al. A review and evaluation of intraurban air pollution exposure models. J Expo Sci Environ Epidemiol. 2005;15(2):185–204.
Ahlm L, Liu S, Day DA, Russell LM, Weber R, Gentner DR, et al. Formation and growth of ultrafine particles from secondary sources in Bakersfield, California. J Geophys Res: Atmos. 2012;117(D21)
Beckerman B, Jerrett M, Brook JR, Verma DK, Arain MA, Finkelstein MM. Correlation of nitrogen dioxide with other traffic pollutants near a major expressway. Atmos Environ. 2008;42(2):275–90.
Gullett BK, Touati A, Hays MD. PCDD/F, PCB, HxCBz, PAH, and PM emission factors for fireplace and woodstove combustion in the San Francisco Bay region. Environ Sci Technol. 2003;37(9):1758–65.
Garcia E, Hurley S, Nelson DO, Gunier RB, Hertz A, Reynolds P. Evaluation of the agreement between modeled and monitored ambient hazardous air pollutants in California. Int J Environ Health Res. 2014;24(4):363–77.
Bonjour S, Adair-Rohani H, Wolf J, Bruce NG, Mehta S, Pruss-Ustun A, et al. Solid fuel use for household cooking: country and regional estimates for 1980-2010. Environ Health Perspect. 2013;121(7):784–90. https://doi.org/10.1289/ehp.1205987.
Environmental Protection Agency Research Triangle Park, NC: office of air quality, planning, and standards. An overview of methods for EPA's national-scale air toxics assessment. 2011. Available: https://www.epa.gov/sites/production/files/2015-10/documents/2005-nata-tmd.pdf. Accessed 22 March 2018.
Hiatt RA, Haslam SZ, Osuch J. The breast cancer and the environment research centers: transdisciplinary research on the role of the environment in breast cancer etiology. Environ Health Perspect. 2009;117(12):1814–22.
Colditz GA, Rosner BA, Chen WY, Holmes MD, Hankinson SE. Risk factors for breast cancer according to estrogen and progesterone receptor status. J Natl Cancer Inst. 2004;96(3):218–28.
Cheraghi Z, Poorolajal J, Hashem T, Esmailnasab N, Doosti Irani A. Effect of body mass index on breast cancer during premenopausal and postmenopausal periods: a meta-analysis. PLoS One. 2012;7(12):7.
Hu H, Dailey AB, Kan H, Xu X. The effect of atmospheric particulate matter on survival of breast cancer among US females. Breast Cancer Res Treat. 2013;139(1):217–26.
Tagliabue G, Borgini A, Tittarelli A, van Donkelaar A, Martin RV, Bertoldi M, et al. Atmospheric fine particulate matter and breast cancer mortality: a population-based cohort study. BMJ Open. 2016;6(11):e012580. https://doi.org/10.1136/bmjopen-2016-012580.
Wong CM, Tsang H, Lai HK, Thomas GN, Lam KB, Chan KP, et al. Cancer mortality risks from long-term exposure to ambient fine particle. Cancer Epidemiol Biomark Prev. 2016;25(5):839–45.
Huo Q, Cai C, Yang Q. Atmospheric particulate matter and breast cancer survival: estrogen receptor triggered? Tumour Biol: J Int Soc Oncodevelop Biol Med. 2015;36(5):3191–3. https://doi.org/10.1007/s13277-015-3291-8.
Acknowledgements
This research was supported by the Intramural Research Program of the NIH.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of Interest
The authors declare that they have no conflicts of interest.
Human and Animal Rights and Informed Consent
This article does not contain any studies with human or animal subjects performed by any of the authors.
Additional information
This article is part of the Topical Collection on Environmental Epidemiology
Rights and permissions
About this article
Cite this article
White, A.J., Bradshaw, P.T. & Hamra, G.B. Air Pollution and Breast Cancer: a Review. Curr Epidemiol Rep 5, 92–100 (2018). https://doi.org/10.1007/s40471-018-0143-2
Published:
Issue Date:
DOI: https://doi.org/10.1007/s40471-018-0143-2