Abstract
This paper reviews the magnitude and empirical findings of social epidemiological neighborhood effects research. An electronic keyword literature search identified 1369 empirical and methodological neighborhood effects papers published in 112 relevant journals between 1990 and 2014. Analyses of temporal trends were conducted by focus, journal type (e.g., epidemiology, public health, or social science), and specific epidemiologic journal. Select papers were then critically reviewed. Results show an ever-increasing number of papers published, notably since the year 2000, with the majority published in public health journals. The variety of health outcomes analyzed is extensive, ranging from infectious disease to obesity to criminal behavior. Papers relying on data from experimental designs are thought to yield the most credible results, but such studies are few and findings are inconsistent. Papers relying on data from observational designs and multilevel models typically show small statistically significant effects, but most fail to appreciate fundamental identification problems. Ultimately, of the 1170 empirically focused neighborhood effects papers published in the last 24 years, only a handful have clearly advanced our understanding of the phenomena. The independent impact of neighborhood contexts on health remains unclear. It is time to expand the social epidemiological imagination.
Similar content being viewed by others
Introduction
Scholarship addressing the effect of the biologic environment on human health dates back 2500 years to Hippocratic medical corpus [1], but the idea of estimating the independent impact of a community’s social characteristics on the health of its members appears to date back to Durkheim’s 1897 study of suicide [2]. Since then, epidemiologists and other population scientists have systematically investigated the independent effect of social and environmental contexts on human thinking, behavior, and health [3]. The motivating question is: Above and beyond one’s background characteristics, how do contexts change outcomes? This question, however phrased, may be the Holy Grail of social science research for it speaks directly to the importance and impact of social and environmental contexts, above and beyond genetic predispositions or perhaps even human motivations and values. Consider the following questions: Does a selfish person become altruistic when she resides in an altruistic community? Do more socioeconomically equal neighborhoods prevent heart disease?
Within epidemiology, the contextual effect question illuminates the impact of the environment, both biological and social, on health outcomes, above and beyond the characteristics of the host. From a methodological perspective, contexts may be viewed as effect modifiers or yield biosocial interactions in their own right. For social epidemiology in particular, researchers have tended to focus more narrowly on the impact of the socioeconomic characteristics of residential neighborhoods on health.
It is not surprising that a vast amount has been written about contextual effects; theoretical, methodological, and empirical scholarship abounds. So as to better appreciate advances, gaps, and shortcomings, it is occasionally helpful to take stock and assess what the collective effort has produced. Although excellent empirical summaries for epidemiologists are available [4–17], none has been extensive, recent, and focused on the question: What have we learned from the last 20 years of empirical neighborhood effects research, broadly?
The aims of this paper are twofold. We first aim to describe the extent of contextual and neighborhood effects research. Second, we aim to assess the progress of epidemiological neighborhood effects research. Because methodological advances have been reviewed elsewhere [18], this paper focuses on empirical research. Importantly, we aim to summarize the literature in a general way, as if it were a map of a large state or region, leaving particular details and sub-group nuances to future investigations. The goal is to help epidemiologists gain perspective on the state of the literature by synthesizing findings and assessing accomplishments. We do not attempt to conduct a statistical meta-analysis with attendant effect sizes and p values; our effort is more of an evaluative synthesis.
This brief review is organized as follows. We first discuss our methodology, including strengths and weaknesses. Next, we offer a citation analysis of temporal trends. Third, we offer a critical review and synthesis of the empirical neighborhood effects literature, tailored for the practicing epidemiologist. Finally, we offer concluding remarks.
Methods
Given the diversity of the topic and the nuanced interdisciplinary approaches to it, it is impossible to simply and accurately identify contextual and/or neighborhood effects papers. Even if one were to read every potentially relevant paper, it would not always be obvious whether to include it in a database for analysis. What is more, with such a large number of papers published in a large number of journals, methods for tracking within-paper citations are unwieldy.
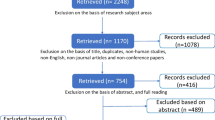
So as to gain purchase on the extent of contextual and neighborhood effect research, we conducted an electronic literature search of the PubMed and Social Science Citation Index databases. We searched title and abstract fields for the following keywords: neighborhood, context, contextual, multilevel, and multi-level. Incredibly, this rough cut produced over 400,000 citations in over 10,000 journals. We enhanced our focus by restricting year of publication from 1990 to present (October 2014) and excluding journals we did not think relevant to this investigation (e.g., The Spine Journal, The Journal of Chemical Physics). Further culling left 112 journals we subjectively believed relevant to this research. We classified the 112 journals as being primarily focused on epidemiology, public health, medicine, social science, or statistics. As disciplines overlap (e.g., epidemiology is often viewed as a subdiscipline of public health) and several interdisciplinary journals defy classification (e.g., Social Science and Medicine), we made subjective choices so as to prevent double counting. Next, we identified four top epidemiologic journals, where “top” implies importance for the empirical neighborhood effects research reviewed here. This list, and all attendant classifications, is available upon request. Finally, we identified several papers we believe are especially salient to this assessment, and summarized their findings below.
We concede the subjectivity of our data processing and classification efforts, and acknowledge the fact that other investigators may have made different keyword and/or classification decisions. However, reclassifications and informal sensitivity analyses revealed little impact on the conclusions offered here. Further, we concede error in our data. Although we tried to identify all contextual and neighborhood effect papers in the selected 112 relevant journals, we probably include some that others would reject and missed some that others would include. Accordingly, we believe it best to consider our results as first-order approximations to the truth, as is the case with any high-level map of terrain.
Citation Analysis
Figure 1 plots the trend of papers published in the selected set of 112 relevant journals, by whether a given paper is focused on contextual (general) or neighborhood (specific) effects. Because of the inexactness of our coding, we plot (12 bin) median splines instead of observed counts; this method smooths the trend lines while retaining the key information. General trends are thus more obvious and interpretable.
Since 1993, there have been 32,613 contextual effect papers published in relevant journals, of which 1369 (4.2 %) addressed neighborhood effects in particular. Of the 1369, we determined that 1170 (84.5 %) are empirically focused, while the remainder are methodologically focused. Figure 1 reveals a striking increase in contextual effect papers since the year 1992. It is impossible to explain this trend with our data, but we speculate that the 1992 publication of Bryk and Raudenbush’s [19] classic text on multilevel statistical models played a significant role, as did the release of SAS Proc Mixed (multilevel model) software, and the increasingly easy access to US Census data (which is typically used as a proxy for neighborhood contexts).
Figure 2 plots the trend in 1369 neighborhood effect papers published in 112 journals, by journal type. Since 1990, there have been 878, 226, 168, and 82 papers published in public health, epidemiology, medical, and social science journals, respectively. The remaining 15 papers (not plotted) were published in statistical journals. This figure reveals a striking increase in neighborhood effect papers published since 2000, especially in public health journals. While a slight increase is evident, the frequency of such papers in well-recognized social science journals is notably less than in the health journals. The reason for the disciplinary discrepancies is not clear, but we speculate that social scientists better appreciated the complexity of the identification problems associated with such analyses. In any case, it seems worth noting that increase in the number of empirically focused papers occurs after Oakes’s 2004 paper that questioned the validity and utility of naive multilevel investigations.
Figure 3 presents trends of empirically focused neighborhood effect papers published in four epidemiology journals: American Journal of Epidemiology (AJE), Journal of Epidemiology and Community Health (JECH), Annals of Epidemiology (Annal Epi), and Epidemiology (Epid). Overall, there were 171 empirically focused papers published in these four journals. Another seven papers were published in the International Journal of Epidemiology (n = 5) and Journal of Clinical Epidemiology (n = 2), respectively; given the low frequency, these papers were not displayed in Fig. 3. Along with empirical papers, there were 33 methodological papers, a disproportionate (n = 7) number appearing in Epidemiology. The rise in empirically focused neighborhood effect papers began in 2003 and has only tapered off slightly in the last 2 years. The reason for the rise is not clear.
Review and Synthesis
Observational Studies
The vast majority of empirically focused neighborhood effect papers are based on observational (i.e., non-experimental) data and rely on multilevel (i.e., mixed effect regression) models to separate the effects of neighborhood contexts from the background characteristics of residents—contexts from composition. Seminal work was by social scientists and includes a 1985 paper by Hogan and Kitagawa [20], who revealed that, after controlling for person-level socioeconomic factors, teenagers in disadvantaged neighborhoods had higher fertility rates than those in more advantaged neighborhoods. Next came a 1993 paper by Brooks-Gunn et al. [21], who argued that, after adjusting for individual socioeconomic status, children in affluent neighborhoods had better developmental outcomes compared to children in disadvantaged areas. Contributions from social epidemiology begin in 1997 with two papers: Diez-Roux et al. [22] suggested that living in deprived neighborhoods was independently associated with increased prevalence of heart disease, and O’Campo et al. [23] suggested that neighborhood income was independently related to the risk of low birthweight. Not long after came a flood of studies addressing a wide variety of outcome variables such as violence, blood pressure, alcohol use, preterm birth, tuberculosis, cancer, drug overdose, physical activity, happiness, functional limitations, fast-food consumption, initiation of sex, and mental health issues, to name a few [24–40]. By and large, these papers report small, statistically significant associations between neighborhood contexts and outcome variables. In papers that use multiple measures of neighborhood environment and/or multiple outcome variables, authors typically report mixed effects. Yet, incredibly, all of these papers concluded neighborhood contexts independently impacted outcomes. Unfortunately, few of these papers considered the challenges of multilevel causal inference and the implicit assumptions of the multilevel model [41]. It is for this reason that we do not summarize such papers here.
In the last few years, an increasing number of empirically oriented papers relying on observational data have used what one might call causal methods to better identify neighborhood effects. Following a seminal 2003 paper by the sociologist Harding [42], several social epidemiology papers have used propensity score methods to estimate neighborhood effects. Novak et al. [43] examined retail tobacco outlet density on youth cigarette smoking and found a small, barely discernable effect. Schootman et al. [44] studied the impact of neighborhood environments on depression among African Americans and found no appreciable effect. Johnson et al. [45] examined the effect of neighborhood poverty on American Indian infant mortality and discovered little overlap in exposure probabilities, leaving the effect unidentifiable. Hearst et al. [46] examined the effect of neighborhood black–white segregation on black infant mortality and found no statistically discernable effect. In a related approach, Oakes et al. [47] evaluated the impact of street connectivity on walkability and found no appreciable effect. Conversely, Ahern et al. [48] found that a neighborhood’s culture of alcohol use did impact an individual’s propensity to drink.
More recently, several authors have aimed to estimate neighborhood effects by exploiting longitudinal data. Glymour et al. [49] used a marginal structural model (MSM) to estimate the effect of neighborhood poverty on self-assessed health and disability, and found mixed effects. Cerda et al. [50] used a MSM to examine the relationship between neighborhood poverty and alcohol use and found that a one-unit increase in the proportion of residents living in poverty was associated with an 86 % increase in the odds of binge drinking. Do et al. [51] used a MSM and examined the effect of neighborhood poverty on mortality and found nonlinear effects. Nandi et al. [52] used a similar approach to examine the effect of neighborhood poverty on the probability of injection cessation and estimated a 44 % increase in the odds of injecting for a 20 % increase in neighborhood poverty. Finally, Jokela [53•] published a novel paper exploiting rich repeated measures data on persons/households who move from one neighborhood to another, and used fixed-effect models to disentangle self-selection from neighborhood effects. He found little impact of neighborhoods on measured outcomes, though some unresolved methodologic issues remain [54, 55].
It is not surprising that results from causal methods are more mixed than those from naive multilevel models. Methods that pay more attention to core identification requirements, such as exchangeability and positivity, would seem less prone to estimate off-support effects and suffer residual confounding, as is often the case when multilevel models are used. Broad differences between the findings from propensity score and inverse probability weight (IPW) methods (e.g., marginal structural models) merit further investigation. We wonder if IPW procedure’s inherent upweighting of observations that would be excluded in a propensity score analysis explains the divergent results.
Experiments
Experiments are advantageous because they entail both random assignment and exogenous interventions, minimizing assumptions for effect identification [56]. There are two types of neighborhood effect experiments [1]: those that move people to new neighborhoods and [2] those that change the neighborhoods in which people reside. Although costly and difficult to implement, there are a handful of neighborhood effect experiments.
The first type of neighborhood effect experiment is exemplified by the Moving To Opportunity (MTO) study [57]. In simplest terms, MTO was conducted in five large US cities and randomly assigned eligible low-income families in high-poverty neighborhoods to lower-poverty neighborhoods. The study has generated some controversy [58–60] but must be viewed a major contribution to the neighborhood effects literature. Although designed to assess economic outcomes, some health impacts were assessed. First, Leventhal and Brooks-Gunn [61] examined the relatively short-term (3 year postrandomization) effect of moving on the mental health of adult and child subjects in New York City and found positive effects for adults and boys but no effect for girls. Yet, more recently, Kessler et al. [62•] examined the long-term (10–15 years postrandomization) effects of moving on the mental health of adolescents and found harmful effects for boys and positive effects for girls, approximately the opposite of the earlier study. This changed and cross-directional gendered effect has generated considerable interest and some investigation [63–66, 67•, 68, 69]. Apart from mental health, Ludwig et al. [70] examined the long-term effect of mobility on adult obesity and diabetes and found small effects. Overall, the evidence from experimental housing relocation programs on health shows, generously, small and mixed, if not confusing, effects.
The second type of experimental study is best construed as a neighborhood randomized trial where some study neighborhoods receive a (health focused) treatment and others do not. Such studies have had a rocky past due to early methodological misunderstandings and muted effects [71], but today methodological questions are largely solved [72–77]. A few reviews of impacts are available (e.g., [78]), but a handful of studies merit attention here. First, Luepker et al. [79] aimed to reduce the delay time between the onset of symptoms of a heart attack to arrival at a proper hospital by intervening on community understanding and social norms. No appreciable impact was observed. Wagenaar et al. [80] organized communities to reduce their own underage alcohol problems with a highly innovative study that exemplifies the social organizing principal of social epidemiology. Yet, measurable impacts were somewhat mixed and modest. Finally, building on the promising work of Perry et al. [81] to prevent alcohol abuse in more rural areas, Komro et al. [82] reported that their tailored replication efforts in urban, low-income, and multiethnic settings were not successful. Overall, despite methodological advances and the great advantage of the design to assess neighborhood effects [41], the effect of neighborhood interventions on health remain modest, if not nonreplicable, at best.
Natural Experiments
The final type of study considered here is the natural experiment, which exploits exogenous interventions and arbitrary (random-like) assignment to conditions. Few social epidemiological natural experiment neighborhood effect studies exist, though it appears that their frequency is increasing. Three are worth mentioning here. Cohen et al. [83] exploited changes associated with the 1992 Los Angeles riots to examine the effect neighborhood alcohol outlet density on neighborhood gonorrhea rates. They found that a one-unit decrease in the number of alcohol outlets per mile of roadway was associated with 21 fewer gonorrhea cases per 100,000. Cerda et al. [84•] exploited change in transportation structures in Medellin, Columbia, to assess the impact of neighborhood infrastructure investment on violence. They found that investment decreased violence at the neighborhood level. Vortuba and King [85] used data from the Gautreaux housing relocation program to assess the effect of neighborhood socioeconomic characteristics on the mortality of young low-income black men and found that all-cause and homicide mortality rates were lower among those who moved to more educated neighborhoods. Overall, it appears that published natural experiments of neighborhood effects show that changes to neighborhood conditions impact select health outcomes.
Conclusion
As currently conceived, social epidemiological neighborhood effects research aims to identify and estimate the independent impact of changing neighborhood contexts on health outcomes. Such research is important because it illuminates avenues for enhancing community and population health without directly intervening on individuals, the presumption being that health may be more efficiently and effectively improved by changing biosocial structures. Yet, the scientific evidence for such effects is elusive. Definitive results require researchers to either move randomly selected persons from one neighborhood context to another (a MTO-like design) or exogenously alter randomly selected neighborhoods in which people reside (a GRT-like design), and compare outcomes. These designs are not only daunting and expensive, but without extensive evidence of demonstrable impact. Consequently, it seems that the vast amount of neighborhood effects research relies on observational data. Yet, as frequently explained, methodological challenges such as endogeneity, dependency, exchangeability, and structural confounding make it very difficult to identify the desired parameters with observational data; the multilevel statistical model is no panacea.
This paper has shown that neighborhood effects research, and especially the broader contextual effects research, remains ascendant. A previous report [18] suggested that the torrent of multilevel studies purporting to reveal independent effects of neighborhoods on health outcomes appeared to be subsiding, but this study suggests that this may not be the case, at least with respect to public health journals. The temporal trends matter because it is not clear how much we are learning, or whether such lessons are improving population health. As discussed above, experimental evidence of neighborhood effects is mixed, and observational studies too often report mere correlations, side-stepping critical effect identification issues. Since epidemiologists have long known that disadvantaged environments are not healthy, the utility of studies that do not face the difficult methodological challenges is questionable.
There is more. Like all research, neighborhood effects research consumes scarce resources, including investigator time, data collection costs, overhead fees (e.g., electricity), and the like. There are also the opportunity costs of not devoting attention to other important questions. To be sure, such consumption is not necessarily a bad thing. After all, extensive resources have been devoted to the development and testing of important, and sometimes failed, vaccines, surgical techniques, basic science, educational innovations, and so forth. However, an occasional accounting is often helpful. To this end, we queried NIH’s RePORTER database for funded grants with key words neighborhood and multilevel in the abstract field. We identified 147 grants (66 of which were R01s) funded since 1993. The total sum of these grants is $141 million and the per-year expenditures tracks with Fig. 2 above. Yet, given the limited search terms, this seems like a substantial underestimate of resources devoted to neighborhood effects research. If nothing else, such an amount does not include the expensive NIH supported community-randomized trials or research supported by other (non-NIH) government agencies or philanthropies, such as the Robert Wood Johnson Foundation, which has supported health-related neighborhood effects research. Nevertheless, it is clear that a large amount of our collective resources have been devoted to neighborhood effects research. While paltry compared to resources devoted to genetics or proteomics, the benefit of which is also questionable, the amount devoted to neighborhood effects appears to represent a significant proportion of the resources devoted to social epidemiology.
Given the findings of this report, it is fair to ask whether social epidemiologists should devote any more time and resources to estimating neighborhood effects. Perhaps ironically, our answer is a resounding yes: Social epidemiologists should stay focused on the estimating impact of biosocial contexts (e.g., neighborhoods) on health. The basic idea that biosocial contexts affect health is patently obvious. It is the idea of an independent, separate, neighborhood effect that seems foolish. The error lies in efforts to disentangle people from places. Paraphrasing Macintyre and Ellaway [86], the fact is that neighborhoods make people, and people make neighborhoods. It is not composition or context, but composition and contexts. Efforts to disentangle mutually constitutive, inextricably linked, synergistic, and coevolving elements are doomed to fail.
Simply put, there is more work to do on how contexts, especially neighborhoods, impact health. Social epidemiologists interested in the effects of neighborhoods on health may benefit from the models and metaphors of ecology. Macintyre and Ellaway [87] are McLaren and Hawe [88] are good places to start learning about such ideas. But more importantly, if we accept the consequentialist summons [89], then we must endeavor to do things to improve health by changing neighborhood contexts if not compositions (e.g., desegregation). Substantial resources should be devoted to multilevel neighborhood/community interventions that address poverty, child abuse, racism, and so forth. Such interventions must be rigorously evaluated and findings dispassionately reported.
Moreover, we recommend that more attention be paid to the short- and long-term consequences of neighborhood effects research. Beyond focusing on theoretically supported interventions and paying more attention to methodological challenges in observational designs, innovations such as cloud-based (contextual) data warehouses, data sharing agreements, and the collective support for replication studies are needed. In a related point, we urge epidemiologists to explore the existing social science literature on neighborhood effects. There is a long-standing debate within and between the social sciences about the meaning of contextual effects, as well as an abundant empirical literature estimating the impact of different contexts, neighborhoods included, on a variety of (non-health) outcomes. Such scholarship would surely enhance the social epidemiological imagination.
References
Papers of particular interest, published recently, have been highlighted as: • Of importance
Jones WHS, Withington ET. Hippocrates: with an English translation. Harvard University Press; 1952.
Durkheim E. Suicide: a study in sociology [1897]. Translated by JA Spaulding and G Simpson (Glencoe, Illinois: The Free Press, 1951) 1951.
Kawachi I, Berkman LF, editors. Neighborhoods and health. New York: Oxford; 2002.
Curtis S, Pain R, Fuller S, Khatib Y, Rothon C, Stansfeld SA, et al. Neighbourhood risk factors for common mental disorders among young people aged 10-20 years: a structured review of quantitative research. Health Place. 2013;20:81–90.
Kim D. Blues from the neighborhood? Neighborhood characteristics and depression. Epidemiol Rev. 2008;30(1):101–17.
Mair C, Diez Roux AV, Galea S. Are neighbourhood characteristics associated with depressive symptoms? A review of evidence. J Epidemiol Community Health. 2008;62:940–6.
March D, Hatch SL, Morgan C, Kirkbride JB, Bresnahan M, Fearon P, et al. Psychosis and place. Epidemiol Rev. 2008;30:84–100.
Ding D, Sallis JF, Kerr J, et al. Neighborhood environment and physical activity among youth: a review. Am J Prev Med. 2011;41(4):442–55.
McCormack GR, Shiell A. In search of causality: a systematic review of the relationship between the built environment and physical activity among adults. Int J Behav Nutr Phys Act. 2011;8:125.
Feng J, Glass TA, Curriero FC, Stewart WF, Schwartz BS. The built environment and obesity: a systematic review of the epidemiologic evidence. Health Place. 2010;16(2):175–90.
Lovasi GS, Hutson MA, Guerra M, Neckerman KM. Built environments and obesity in disadvantaged populations. Epidemiol Rev. 2009;31:7–20.
Foster S, Giles-Corti B. The built environment, neighborhood crime and constrained physical activity: an exploration of inconsistent findings. Prev Med. 2008;47(3):241–51.
Papas MA, Alberg AJ, Ewing R, Helzlsouer KJ, Gary TL, Klassen AC. The built environment and obesity. Epidemiol Rev. 2007;29:129–43.
Meijer M, Rohl J, Bloomfield K, Grittner U. Do neighborhoods affect individual mortality? A systematic review and meta-analysis of multilevel studies. Soc Sci Med. 2012;74(8):1204–12.
Yen IH, Michael YL, Perdue L. Neighborhood environment in studies of health of older adults: a systematic review. Am J Prev Med. 2009;37(5):455–63.
Pickett KE, Pearl M. Multilevel analyses of neighbourhood socioeconomic context and health outcomes: a critical review. J Epidemiol Community Health. 2001;55(2):111–22.
Kramer MR, Hogue CR. Is segregation bad for your health? Epidemiol Rev. 2009;31:178–94.
Oakes JM, Andrade KN. Methodologic innovations and advances in social epidemiology. Curr Epidemiol Rep. 2014;1(1):38–44.
Bryk A, Raudenbush S. Hierarchical linear models: applications and data analysis methods. Newbury Park, CA: Sage; 1992.
Hogan DP, Kitagawa EM. The impact of social status, family structure, and neighborhood on the fertility of black adolescents. American journal of Sociology 1985:825-855.
Brooksgunn J, Duncan GJ, Klebanov PK, Sealand N. Do neighborhoods influence child and adolescent development. Am J Sociol. 1993;99(2):353–95.
Diez-Roux AV, Nieto FJ, Muntaner C, Tyroler HA, Comstock GW, Shahar E, et al. Neighborhood environments and coronary heart disease: a multilevel analysis. Am J Epidemiol. 1997;146(1):48–63.
O’Campo P, Xue X, Wang MC, Caughy M. Neighborhood risk factors for low birthweight in Baltimore: a multilevel analysis. Am J Public Health. 1997;87(7):1113–8.
Galea S, Karpati A, Kennedy B. Social capital and violence in the United States, 1974–1993. Soc Sci Med. 2002;55(8):1373–83.
Diez Roux AV, Chambless L, Merkin SS, Arnett D, Eigenbrodt M, Nieto FJ, et al. Socioeconomic disadvantage and change in blood pressure associated with aging. Circulation. 2002;106(6):703–10.
Wechsler H, Lee JE, Hall J, Wagenaar AC, Lee H. Secondhand effects of student alcohol use reported by neighbors of colleges: the role of alcohol outlets. Soc Sci Med. 2002;55(3):425–35.
Kaufman JS, Dole N, Savitz DA, Herring AH. Modeling community-level effects on preterm birth. Ann Epidemiol. 2003;13(5):377–84.
Acevedo-Garcia D. Zip code-level risk factors for tuberculosis: neighborhood environment and residential segregation in New Jersey, 1985-1992. Am J Public Health. 2001;91(5):734–41.
Eschbach K, Mahnken JD, Goodwin JS. Neighborhood composition and incidence of cancer among Hispanics in the United States. Cancer. 2005;103(5):1036–44.
Hembree C, Galea S, Ahern J, Tracy M, Piper TM, Miller J, et al. The urbant built environment and overdose mortality in New York City neighborhoods. Health Place. 2005;11(2):147–56.
Li F, Fisher KJ, Brownson RC, Bosworth M. Multilevel modelling of built environment characteristics related to neighbourhood walking activity in older adults. J Epidemiol Community Health. 2005;59(7):558–64.
Subramanian SV, Kim D, Kawachi I. Covariation in the socioeconomic determinants of self rated health and happiness: a multivariate multilevel analysis of individuals and communities in the USA. J Epidemiol Community Health. 2005;59(8):664–9.
Schootman M, Andresen EM, Wolinsky FD, Malmstrom TK, Miller JP, Miller DK. Neighborhood conditions and risk of incident lower-body functional limitations among middle-aged African Americans. Am J Epidemiol. 2006;163(5):450–8.
Cradock AL, Kawachi I, Colditz GA, Gortmaker SL, Buka SL. Neighborhood social cohesion and youth participation in physical activity in Chicago. Soc Sci Med. 2009;68(3):427–35.
Moore LV, Diez Roux AV, Nettleton JA, Jacobs DR, Franco M. Fast-food consumption, diet quality, and neighborhood exposure to fast food: the multi-ethnic study of atherosclerosis. Am J Epidemiol. 2009;170(1):29–36.
Cubbin C, Brindis CD, Jain S, Santelli J, Braveman P. Neighborhood poverty, aspirations and expectations, and initiation of sex. J Adolesc Health. 2010;47(4):399–406.
Ahern J, Galea S. Collective efficacy and major depression in urban neighborhoods. Am J Epidemiol. 2011;173(12):1453–62.
Gilman SE, Fitzmaurice GM, Bruce ML, Ten Have T, Glymour MM, Carliner H, et al. Economic inequalities in the effectiveness of a primary care intervention for depression and suicidal ideation. Epidemiology. 2013;24(1):14–22.
Messer LC, Kaufman JS, Dole N, Savitz DA, Laraia BA. Neighborhood crime, deprivation, and preterm birth. Ann Epidemiol. 2006;16(6):455–62.
Yen IH, Kaplan GA. Neighborhood social environment and risk of death: multilevel evidence from the Alameda County Study. Am J Epidemiol. 1999;149(10):898–907.
Oakes JM. The (mis)estimation of neighborhood effects: causal inference for a practicable social epidemiology. Soc Sci Med. 2004;58(10):1929–52.
Harding DJ. Counterfactual models of neighborhood effects: the effect of neighborhood poverty on dropping out and teenage pregnancy. Am J Sociol. 2003;109(3):676–719.
Novak SP, Reardon SF, Raudenbush SW, Buka SL. Retail tobacco outlet density and youth cigarette smoking: a propensity-modeling approach. Am J Public Health. 2006;96(4):670–6.
Schootman M, Andresen EM, Wolinsky FD, Malmstrom TK, Miller JP, Miller DK. Neighbourhood environment and the incidence of depressive symptoms among middle-aged African Americans. J Epidemiol Community Health. 2007;61(6):527–32.
Johnson PJ, Oakes JM, Anderton DL. Neighborhood poverty and American Indian infant death: are the effects identifiable? Ann Epidemiol. 2008;18(7):552–9.
Hearst MO, Oakes JM, Johnson PJ. The effect of racial residential segregation on black infant mortality. Am J Epidemiol. 2008;168(11):1247–54.
Oakes JM, Forsyth A, Schmitz KH. The effects of neighborhood density and street connectivity on walking behavior: the Twin Cities walking study. Epidemiol Perspect Innov. 2007;4:16.
Ahern J, Galea S, Hubbard A, Midanik L, Syme SL. “Culture of drinking” and individual problems with alcohol use. Am J Epidemiol. 2008;167(9):1041–9.
Glymour MM, Mujahid M, Wu Q, et al. Neighborhood disadvantage and self-assessed health, disability, and depressive symptoms: longitudinal results from the health and retirement study. Ann Epidemiol. 2010;20(11):856–61.
Cerda M, Diez-Roux AV, Tchetgen ET, Gordon-Larsen P, Kiefe C. The relationship between neighborhood poverty and alcohol use: estimation by marginal structural models. Epidemiology. 2010;21(4):482–9.
Do DP, Wang L, Elliott MR. Investigating the relationship between neighborhood poverty and mortality risk: a marginal structural modeling approach. Soc Sci Med. 2013;91:58–66.
Nandi A, Glass TA, Cole SR, Chu H, Galea S, Celentano DD, et al. Neighborhood poverty and injection cessation in a sample of injection drug users. Am J Epidemiol. 2010;171(4):391–8.
Jokela M. Are neighborhood health associations causal? A 10-year prospective cohort study with repeated measurements. American Journal of Epidemiology 2014. This paper presents results from remarkably rich repeated measures data on the independent impacts of neighborhood environments on health. The associated commentary and response illuminate important issues.
Jokela M. Jokela responds to “Repeated measures and effect identification”. Am J Epidemiol. 2014;180(8):788–9.
Oakes JM. Invited commentary: repeated measures, selection bias, and effect identification in neighborhood effect studies. Am J Epidemiol 2014:kwu231.
Oakes M. Effect identification in comparative effectiveness research. eGEMs (Generating Evidence & Methods to Improve Patient Outcomes). 2013;1(1):4.
de Souza Briggs X, Popkin SJ, Goering J. Moving to opportunity: the story of an American experiment to fight ghetto poverty. Oxford University Press; 2010.
Ludwig J, Liebman JB, Kling JR, et al. What can we learn about neighborhood effects from the Moving to Opportunity experiment. Am J Sociol. 2008;114(1):144–88.
Clampet‐Lundquist S, Massey DS. Neighborhood effects on economic self‐sufficiency: a reconsideration of the moving to opportunity experiment. Am J Sociol. 2008;114(1):107–43.
Sobel ME. What do randomized studies of housing mobility demonstrate?: causal inference in the face of interference. J Am Stat Assoc. 2006;101(476):1398–407.
Leventhal T, Brooks-Gunn J. Moving to opportunity: an experimental study of neighborhood effects on mental health. Am J Public Health. 2003;93(9):1576–82.
Kessler RC, Duncan GJ, Gennetian LA, Katz LF, Kling JR, Sampson NA, et al. Associations of housing mobility interventions for children in high-poverty neighborhoods with subsequent mental disorders during adolescence. JAMA. 2014;311(9):937–48. This paper presents experimental evidence from the MTO housing relocation study on adolescent mental health outcomes. It is methodological and substantively critical to the contemporary understanding of neighborhood effects.
Clampet-Lundquist S, Edin K, Kling JR, et al. Moving teenagers out of high-risk neighborhoods: how girls fare better than boys. Am J Sociol. 2011;116(4):1154–89.
Jackson L, Langille L, Lyons R, et al. Does moving from a high-poverty to lower-poverty neighborhood improve mental health? A realist review of ‘Moving to Opportunity’. Health Place. 2009;15(4):961–70.
Leventhal T, Dupéré V. Moving to Opportunity: does long-term exposure to ‘low-poverty’ neighborhoods make a difference for adolescents? Soc Sci Med. 2011;73(5):737–43.
DeLuca S, Dayton E. Switching social contexts: the effects of housing mobility and school choice programs on youth outcomes. Annu Rev Sociol. 2009;35:457–91.
DeLuca S, Duncan GJ, Keels M, et al. The notable and the null: using mixed methods to understand the diverse impacts of residential mobility programs. Neighbourhood effects research: New perspectives: Springer, 2012:195-223. This chapter is a model for investigating neighborhood impacts with both quantitative and qualitative methods.
Nguyen QC, Schmidt NM, Glymour MM, Rehkopf DH, Osypuk TL. Were the mental health benefits of a housing mobility intervention larger for adolescents in higher socioeconomic status families? Health Place. 2013;23:79–88.
Osypuk TL, Schmidt NM, Bates LM, Tchetgen-Tchetgen EJ, Earls FJ, Glymour MM. Gender and crime victimization modify neighborhood effects on adolescent mental health. Pediatrics. 2012;130(3):472–81.
Ludwig J, Sanbonmatsu L, Gennetian L, Adam E, Duncan GJ, Katz LF, et al. Neighborhoods, obesity, and diabetes—a randomized social experiment. N Engl J Med. 2011;365(16):1509–19.
Susser M. The tribulations of trials—intervention in communities. Am J Public Health. 1995;85(2):156–8.
Hannan PJ. Experimental social epidemiology: controlled community trials. In: Oakes JM, Kaufman JS, editors. Methods in Social Epidemiology. San Francisco: Jossey-Bass / Wiley; 2006. p. 335–64.
Feldman HA, McKinlay SM. Cohort versus cross‐sectional design in large field trials: precision, sample size, and a unifying model. Stat Med. 1994;13(1):61–78.
Donner A, Klar N. Pitfalls of and controversies in cluster randomization trials. Am J Public Health. 2004;94(3):416–22.
Campbell M, Donner A, Klar N. Developments in cluster randomized trials and statistics in medicine. Stat Med. 2007;26(1):2–19.
Campbell MK, Elbourne DR, Altman DG. CONSORT statement: extension to cluster randomised trials. BMJ. 2004;328(7441):702–8.
Murray DM, Varnell SP, Blitstein JL. Design and analysis of group-randomized trials: a review of recent methodological developments. Journal Information 2004;94(3).
Simpson JM, Klar N, Donnor A. Accounting for cluster randomization: a review of primary prevention trials, 1990 through 1993. Am J Public Health. 1995;85(10):1378–83.
Luepker RV, Raczynski JM, Osganian S, et al. Effect of a community intervention on patient delay and emergency medical service use in acute coronary heart disease: the Rapid Early Action for Coronary Treatment (REACT) Trial. JAMA. 2000;284(1):60–7.
Wagenaar AC, Murray DM, Gehan JP, et al. Communities mobilizing for change on alcohol: outcomes from a randomized community trial. J Stud Alcohol. 2000;61(1):85–94.
Perry CL, Williams CL, Veblen-Mortenson S, et al. Project Northland: outcomes of a communitywide alcohol use prevention program during early adolescence. Am J Public Health. 1996;86(7):956–65.
Komro KA, Perry CL, Veblen‐Mortenson S, et al. Outcomes from a randomized controlled trial of a multi‐component alcohol use preventive intervention for urban youth: Project Northland Chicago. Addiction. 2008;103(4):606–18.
Cohen DA, Ghosh-Dastidar B, Scribner R, Miu A, Scott M, Robinson P, et al. Alcohol outlets, gonorrhea, and the Los Angeles civil unrest: a longitudinal analysis. Soc Sci Med. 2006;62(12):3062–71.
Cerda M, Morenoff JD, Hansen BB, Tessari Hicks KJ, Duque LF, Restrepo A, et al. Reducing violence by transforming neighborhoods: a natural experiment in Medellin, Colombia. Am J Epidemiol. 2012;175(10):1045–53. This paper presents the impacts of a large public transportation investment program on violence. It offers important substantive insights and raises important methodological questions.
Votruba ME, Kling JR. Effects of neighborhood characteristics on the mortality of black male youth: evidence from Gautreaux, Chicago. Soc Sci Med. 2009;68(5):814–23.
Macintyre S, Ellaway A. Neighborhoods and health: an overview. Neighborhoods and health 2003:20-42.
Macintyre S, Ellaway A. Ecological approaches: rediscovering the role of the physical and social environment. Social epidemiology 2000:332-348.
McLaren L, Hawe P. Ecological perspectives in health research. J Epidemiol Community Health. 2005;59(1):6–14.
Galea S. An argument for a consequentialist epidemiology. American journal of epidemiology 2013:kwt172.
Acknowledgments
This paper was supported in paper by a funding from the University of Minnesota’s Clinical and Translational Research Institute.
Compliance with Ethics Guidelines
ᅟ
Conflict of Interest
JM Oakes, KE Andrade, IM Biyoow, and LT Cowan all declare no conflicts of interest.
Human and Animal Rights and Informed Consent
All studies by JM Oakes involving animal and/or human subjects were performed after approval by the appropriate institutional review boards. When required, written informed consent was obtained from all participants.
Author information
Authors and Affiliations
Corresponding author
Additional information
This article is part of the Topical Collection on Social Epidemiology
Rights and permissions
About this article
Cite this article
Oakes, J.M., Andrade, K.E., Biyoow, I.M. et al. Twenty Years of Neighborhood Effect Research: An Assessment. Curr Epidemiol Rep 2, 80–87 (2015). https://doi.org/10.1007/s40471-015-0035-7
Published:
Issue Date:
DOI: https://doi.org/10.1007/s40471-015-0035-7