Abstract
Background
Using non-statin lipid-modifying agents in combination with statin therapy provides additional benefits for cardiovascular disease (CVD) risk reduction, but their value for money has only been evaluated in high-income countries (HICs). Furthermore, studies mainly derive effectiveness data from a single trial or older meta-analyses.
Objectives
Our study used data from the most recent network meta-analysis (NMA) and local parameters to assess the cost effectiveness of non-statin agents in statin-treated patients with a history of CVD.
Methods
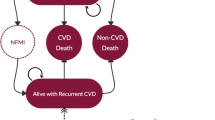
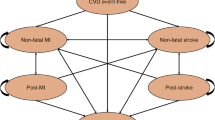
A published Markov model was adopted to investigate lifetime outcomes: (1) number of recurrent CVD events prevented, (2) quality-adjusted life-years (QALYs) gained, (3) costs and (4) incremental cost-effectiveness ratios (ICERs) of proprotein convertase subtilisin/kexin type 9 inhibitors (PCSK9i) and ezetimibe added to statin therapy. Event rates and effectiveness inputs were obtained from the NMA. Cost and utility data were gathered from published studies conducted in Thailand. A series of sensitivity analyses were performed.
Results
Patients receiving PCSK9i and ezetimibe experienced fewer recurrent CVD events (number needed to treat [NNT] 17 and 30) and more QALYs (0.168 and 0.096 QALYs gained per person). However, under the societal perspective and at current acquisition costs in 2018, ICERs of both agents were $US1,223,995 and 27,361 per QALY gained, respectively. Based on threshold analyses, the costs need to be reduced by 97 and 85%, respectively, for PCSK9i and ezetimibe to be cost-effective.
Conclusions
Despite the proven effectiveness of PCSK9i and ezetimibe, the costs of these agents need to reduce to a much greater extent than in HICs to be cost-effective in Thailand.





Similar content being viewed by others
References
Gersh BJ, Sliwa K, Mayosi BM, Yusuf S. Novel therapeutic concepts: the epidemic of cardiovascular disease in the developing world: global implications. Eur Heart J. 2010;31(6):642–8.
Roth GA, Huffman MD, Moran AE, et al. Global and regional patterns in cardiovascular mortality from 1990 to 2013. Circulation. 2015;132(17):1667–78.
Grundy SM, Stone NJ, Bailey AL, et al. 2018 AHA/ACC/AACVPR/AAPA/ABC/ACPM/ADA/AGS/APhA/ASPC/NLA/PCNA Guideline on the Management of Blood Cholesterol: A Report of the American College of Cardiology/American Heart Association Task Force on Clinical Practice Guidelines. J Am Coll Cardiol. 2018.
Piepoli MF, Hoes AW, Agewall S, et al. 2016 European Guidelines on cardiovascular disease prevention in clinical practice: The Sixth Joint Task Force of the European Society of Cardiology and Other Societies on Cardiovascular Disease Prevention in Clinical Practice (constituted by representatives of 10 societies and by invited experts)Developed with the special contribution of the European Association for Cardiovascular Prevention & Rehabilitation (EACPR). Eur Heart J. 2016;37(29):2315–81.
Silverman MG, Ference BA, Im K, et al. Association between lowering LDL-C and cardiovascular risk reduction among different therapeutic interventions: a systematic review and meta-analysis. Jama. 2016;316(12):1289–97.
Schwartz GG, Steg PG, Szarek M, et al. Alirocumab and cardiovascular outcomes after acute coronary syndrome. N Engl J Med. 2018;379(22):2097–107.
Sabatine MS, Giugliano RP, Keech AC, et al. Evolocumab and clinical outcomes in patients with cardiovascular disease. N Engl J Med. 2017;376(18):1713–22.
Cannon CP, Blazing MA, Giugliano RP, et al. Ezetimibe added to statin therapy after acute coronary syndromes. N Engl J Med. 2015;372(25):2387–97.
Korman MJ, Retterstol K, Kristiansen IS, Wisloff T. Are PCSK9 inhibitors cost effective? PharmacoEconomics. 2018;36(9):1031–41.
Kazi DS, Moran AE, Coxson PG, et al. Cost-effectiveness of PCSK9 inhibitor therapy in patients with heterozygous familial hypercholesterolemia or atherosclerotic cardiovascular disease. Jama. 2016;316(7):743–53.
Kazi DS, Penko J, Coxson PG, et al. Updated cost-effectiveness analysis of PCSK9 inhibitors based on the results of the FOURIER trial. Jama. 2017;318(8):748–50.
Korman M, Wisloff T. Modelling the cost-effectiveness of PCSK9 inhibitors vs ezetimibe through LDL-C reductions in a Norwegian setting. Eur Heart J Cardiovasc Pharmacother. 2018;4(1):15–22.
Villa G, Lothgren M, Kutikova L, et al. Cost-effectiveness of evolocumab in patients with high cardiovascular risk in Spain. Clin Ther. 2017;39(4):771–86.
Kumar R, Tonkin A, Liew D, Zomer E. The cost-effectiveness of PCSK9 inhibitors—The Australian healthcare perspective. Int J Cardiol. 2018;267:183–7.
Chaiyasothi T, Nathisuwan S, Dilokthornsakul P, et al. Effects of non-statin lipid-modifying agents on cardiovascular morbidity and mortality among statin-treated patients: a systematic review and meta-analysis. Front Pharmacol. 2019; Article in press.
Srimahachota S, Boonyaratavej S, Kanjanavanit R, et al. Thai Registry in Acute Coronary Syndrome (TRACS)–an extension of Thai Acute Coronary Syndrome registry (TACS) group: lower in-hospital but still high mortality at one-year. J Med Assoc Thailand. 2012;95(4):508–18.
Subcommittee on Developing National List of Essential Medicines. Handbook for health technology assessment in Thailand. 2nd ed. Nonthaburi: Health Intervention and Technology Assessment Program (HITAP); 2013.
Sritara P, Cheepudomwit S, Chapman N, et al. Twelve-year changes in vascular risk factors and their associations with mortality in a cohort of 3499 Thais: the Electricity Generating Authority of Thailand Study. Int J Epidemiol. 2003;32(3):461–8.
Office of Insurance Commission. Mortality table for Thai population. 2017; http://www.oic.or.th/th/consumer/25.
Anukooksawat P, Sritara P, Teerawattananon Y. Costs of lifetime acute coronary syndrome treatment at Ramathibodi hospital. Thai Heart J. 2006;19:132–43.
Tamteeranon Y, Khonputsa P, Teerawattananon Y, Lim S. Economic evaluation of HMG-CoA reductase inhibitor (statin) for primary prevention of cardiovascular diseases among Thai population. Bangkok. 2008.
Youngkong S. Cost of cerebral infarction from societal perspective: a case study at Prasat Neurological Institute. MS thesis in Pharmacy. 2001; Mahidol University. Faculty of Graduate Studies.
National Drug System Development Committee. Royal Thai Government Gazette: National Drug Prices. 2018; http://dmsic.moph.go.th/dmsic/force_down.php?f_id=735.
Subcommittee on Developing National List of Essential Medicines. Handbook for health technology assessment in Thailand. Nonthaburi: Health Intervention and Technology Assessment Program (HITAP); 2009.
Ministry of Commerce. Report for Consumer Price Index of Thailand. 2018; http://www.price.moc.go.th/price/cpi/index_new_all.asp.
Bank of Thailand. Exchange Rate of US Dollar between 3 January 2018 and 3 December 2018. 2018; https://www.bot.or.th/thai/statistics/financialmarkets/exchangerate/_layouts/application/exchangerate/ExchangeRateAgo.aspx.
Jarungsuccess S, Taerakun S. Cost-utility analysis of oral anticoagulants for nonvalvular atrial fibrillation patients at the police general hospital, Bangkok, Thailand. Clin Ther. 2014;36(10):1389–94.
Yamwong S, Permsuwan U, Tinmanee S, Sritara P. Long-term cost effectiveness of ticagrelor in patients with acute coronary syndromes in Thailand. Health Econ Rev. 2014;4(1):17.
Thavorncharoensap M, Teerawattananon Y, Natanant S, Kulpeng W, Yothasamut J, Werayingyong P. Estimating the willingness to pay for a quality-adjusted life year in Thailand: does the context of health gain matter? ClinicoEcon Outcomes Res CEOR. 2013;5:29–36.
Permsuwan U, Guntawongwan K, Buddhawongsa P. Handling time in economic evaluation studies. J Med Assoc Thailand. 2014;97(Suppl 5):S50–8.
Hammerschmidt T, Goertz A, Wagenpfeil S, Neiss A, Wutzler P, Banz K. Validation of health economic models: the example of EVITA. Value Health. 2003;6(5):551–9.
Gandra SR, Villa G, Fonarow GC, et al. Cost-effectiveness of LDL-C lowering with evolocumab in patients with high cardiovascular risk in the United States. Clin Cardiol. 2016;39(6):313–20.
Tice J, Ollendorf D, Chapman R, et al. Evolocumab for treatment of high cholesterol: effectiveness and value. ICER-report; September 11 2017.
Fonarow GC, Keech AC, Pedersen TR, et al. Cost-effectiveness of evolocumab therapy for reducing cardiovascular events in patients with atherosclerotic cardiovascular disease. JAMA Cardiol. 2017;2(10):1069–78.
Paavola A. Amgen cuts list price of $14 K-a-year cholesterol drug nearly 60%. 2018; https://www.beckershospitalreview.com/pharmacy/amgen-cuts-list-price-of-14k-a-year-cholesterol-drug-nearly-60.html.
Goldberg AC, Sapre A, Liu J, Capece R, Mitchel YB. Efficacy and safety of ezetimibe coadministered with simvastatin in patients with primary hypercholesterolemia: a randomized, double-blind, placebo-controlled trial. Mayo Clin Proc. 2004;79(5):620–9.
Permsuwan U, Chaiyakunapruk N, Nathisuwan S, Sukonthasarn A. Cost-effectiveness analysis of fondaparinux vs enoxaparin in non-ST elevation acute coronary syndrome in Thailand. Heart Lung Circ. 2015;24(9):860–8.
Author information
Authors and Affiliations
Contributions
All authors contributed to the study concept and design and the acquisition, analysis, or interpretation of data, and the critical revision of the manuscript for important intellectual content. KK drafted the manuscript. ZA, DL and NC contributed to study supervision.
Corresponding author
Ethics declarations
Funding
No sources of funding were used to conduct this study or prepare this manuscript.
Conflict of interest
DL has received research grants and consulting fees and from companies for work unrelated to this study. ZA and EZ have received grants for the assessment of evolocumab from an Australian perspective. KK, TC, SN, and NC have no conflicts of interest that are directly relevant to the content of this review/study.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Kongpakwattana, K., Ademi, Z., Chaiyasothi, T. et al. Cost-Effectiveness Analysis of Non-Statin Lipid-Modifying Agents for Secondary Cardiovascular Disease Prevention Among Statin-Treated Patients in Thailand. PharmacoEconomics 37, 1277–1286 (2019). https://doi.org/10.1007/s40273-019-00820-6
Published:
Issue Date:
DOI: https://doi.org/10.1007/s40273-019-00820-6