Abstract
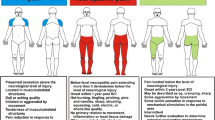
Chronic pain affects most people with spinal cord injury (SCI). It often impedes performance of activities of daily living and negatively impacts quality of life. Pain after SCI can be classified into subtypes through use of the International SCI Pain Classification with key attributes of the pain necessary for effective monitoring and treatment collected within the International SCI Pain Basic Data Set. Many nociceptive causes of pain seen after SCI are potentially treatable and preventable through the implementation of strategies for preventing overuse injuries. Neuropathic pain, in contrast, has been historically difficult to treat. Options for the treatment of neuropathic pain types which have demonstrated some effectiveness include various adjuvant pharmacological agents, neuromodulatory techniques, and psychological approaches.
Similar content being viewed by others
References
Papers of particular interest, published recently, have been highlighted as: • Of importance
Loeser JD, Treede RD. The Kyoto protocol of IASP basic pain terminology. Pain. 2008;137:473–7.
Cardenas DD, Bryce TN, Shem K, Richards JS, Elhefni H. Gender and minority differences in the pain experience of people with spinal cord injury. Arch Phys Med Rehabil. 2004;85:1774–81.
Stormer S, Gerner HJ, Gruninger W, et al. Chronic pain/dysaesthesiae in spinal cord injury patients: results of a multicentre study. Spinal Cord. 1997;35:446–55.
Jensen TS, Baron R, Haanpaa M, et al. A new definition of neuropathic pain. Pain. 2011;152(10):2204–5.
• Bryce TN, Biering-Sorensen F, Finnerup NB, et al. International spinal cord injury pain classification: part I. Background and description. Spinal Cord. 2012;50:413–17. This manuscript describes the classification of pain after SCI.
Widerstrom-Noga E, Biering-Sorensen F, Bryce TN, et al. The international spinal cord injury pain basic data set (version 2.0). Spinal Cord. 2014;52:282–6.
International Spinal Cord Society (ISCoS). International SCI Data Sets. http://www.iscos.org.uk/international-sci-data-sets. Accessed 15 Apr 2015.
Dyson-Hudson TA, Kirshblum SC. Shoulder pain in chronic spinal cord injury, part I: epidemiology, etiology, and pathomechanics. J Spinal Cord Med. 2004;27:4–17.
Bayley JC, Cochran TP, Sledge CB. The weight-bearing shoulder. The impingement syndrome in paraplegics. J Bone Joint Surg Am. 1987;69:676–8.
Gellman H, Sie I, Waters RL. Late complications of the weight-bearing upper extremity in the paraplegic patient. Clin Orthop Relat Res. 1988;233:132–5.
Sie IH, Waters RL, Adkins RH, Gellman H. Upper extremity pain in the postrehabilitation spinal cord injured patient. Arch Phys Med Rehabil. 1992;73:44–8.
Curtis KA, Tyner TM, Zachary L, et al. Effect of a standard exercise protocol on shoulder pain in long-term wheelchair users. Spinal Cord. 1999;37:421–9.
Serra-Ano P, Pellicer-Chenoll M, Garcia-Masso X, Morales J, Giner-Pascual M, Gonzalez LM. Effects of resistance training on strength, pain and shoulder functionality in paraplegics. Spinal Cord. 2012;50(11):827–31.
• Van Straaten MG, Cloud BA, Morrow MM, Ludewig PM, Zhao KD. Effectiveness of home exercise on pain, function, and strength of manual wheelchair users with spinal cord injury: a high-dose shoulder program with telerehabilitation. Arch Phys Med Rehabil. 2014;95:1810–17.e2. This article describes an effective program for addressing shoulder pain after SCI.
Samuelsson K, Larsson H, Thyberg M, Tropp H. Back pain and spinal deformity-common among wheelchair users with spinal cord injuries. Scand J Occup Ther. 1996;3(1):28–32.
Bryce TN, Ragnarsson KT. Epidemiology and classification of pain after spinal cord injury. Top Spinal Cord Inj Rehabil. 2001;7:1–17.
Siddall PJ, McClelland JM, Rutkowski SB, Cousins MJ. A longitudinal study of the prevalence and characteristics of pain in the first 5 years following spinal cord injury. Pain. 2003;103:249–57.
Finnerup NB, Norrbrink C, Trok K, et al. Phenotypes and predictors of pain following traumatic spinal cord injury: a prospective study. J Pain. 2014;15:40–8.
Finnerup NB, Baastrup C. Spinal cord injury pain: mechanisms and management. Curr Pain Headache Rep. 2012;16:207–16.
Kerns RD, Turk DC, Rudy TE. The west haven-yale multidimensional pain inventory (WHYMPI). Pain. 1985;23:345–56.
Widerstrom-Noga EG, Duncan R, Turk DC. Psychosocial profiles of people with pain associated with spinal cord injury: identification and comparison with other chronic pain syndromes. Clin J Pain. 2004;20:261–71.
Widerstrom-Noga EG, Turk DC. Exacerbation of chronic pain following spinal cord injury. J Neurotrauma. 2004;21:1384–95.
Wilkie DJ, Huang HY, Reilly N, Cain KC. Nociceptive and neuropathic pain in patients with lung cancer: a comparison of pain quality descriptors. J Pain Symptom Manag. 2001;22:899–910.
• Finnerup NB, Attal N, Haroutounian S, et al. (2015) Pharmacotherapy for neuropathic pain in adults: a systematic review and meta-analysis. Lancet Neurol. 4:162–73. This is a comprehensive review of the pharmacological treatments of neuropathic pain including after SCI.
Cardenas DD, Nieshoff EC, Suda K, et al. A randomized trial of pregabalin in patients with neuropathic pain due to spinal cord injury. Neurology. 2013;80:533–9.
Vranken JH, Hollmann MW, van der Vegt MH, et al. Duloxetine in patients with central neuropathic pain caused by spinal cord injury or stroke: a randomized, double-blind, placebo-controlled trial. Pain. 2011;152:267–73.
Barrera-Chacon JM, Mendez-Suarez JL, Jauregui-Abrisqueta ML, Palazon R, Barbara-Bataller E, Garcia-Obrero I. Oxycodone improves pain control and quality of life in anticonvulsant-pretreated spinal cord-injured patients with neuropathic pain. Spinal Cord. 2011;49:36–42.
Ray WA, Meredith S, Thapa PB, Hall K, Murray KT. Cyclic antidepressants and the risk of sudden cardiac death. Clin Pharmacol Ther. 2004;75:234–41.
Fischer B, Jones W, Urbanoski K, Skinner R, Rehm J. Correlations between prescription opioid analgesic dispensing levels and related mortality and morbidity in Ontario, Canada, 2005–2011. Drug Alcohol Rev. 2014;33:19–26.
Bohnert AS, Ilgen MA, Trafton JA, et al. Trends and regional variation in opioid overdose mortality among veterans health administration patients, fiscal year 2001 to 2009. Clin J Pain. 2014;30:605–12.
Tan G, Rintala DH, Thornby JI, Yang J, Wade W, Vasilev C. Using cranial electrotherapy stimulation to treat pain associated with spinal cord injury. J Rehabil Res Dev. 2006;43:461–74.
Fregni F, Boggio PS, Lima MC, et al. A sham-controlled, phase II trial of transcranial direct current stimulation for the treatment of central pain in traumatic spinal cord injury. Pain. 2006;122:197–209.
Soler MD, Kumru H, Pelayo R, et al. Effectiveness of transcranial direct current stimulation and visual illusion on neuropathic pain in spinal cord injury. Brain. 2010;133:2565–77.
Wrigley PJ, Gustin SM, McIndoe LN, Chakiath RJ, Henderson LA, Siddall PJ. Longstanding neuropathic pain after spinal cord injury is refractory to transcranial direct current stimulation: a randomized controlled trial. Pain. 2013;154:2178–84.
Ngernyam N, Jensen MP, Arayawichanon P, et al. The effects of transcranial direct current stimulation in patients with neuropathic pain from spinal cord injury. Clin Neurophysiol. 2015;126:382–90.
Tasker RR, DeCarvalho GT, Dolan EJ. Intractable pain of spinal cord origin: clinical features and implications for surgery. J Neurosurg. 1992;77:373–8.
Cioni B, Meglio M, Pentimalli L, Visocchi M. Spinal cord stimulation in the treatment of paraplegic pain. J Neurosurg. 1995;82:35–9.
Cruccu G, Aziz TZ, Garcia-Larrea L, et al. EFNS guidelines on neurostimulation therapy for neuropathic pain. Eur J Neurol. 2007;14:952–70.
Robert R, Perrouin-Verbe B, Albert T, Bussel B, Hamel O. Chronic neuropathic pain in spinal cord injured patients: what is the effectiveness of surgical treatments excluding central neurostimulations? Ann Phys Rehabil Med. 2009;52:194–202.
Falci S, Best L, Bayles R, Lammertse D, Starnes C. Dorsal root entry zone microcoagulation for spinal cord injury-related central pain: operative intramedullary electrophysiological guidance and clinical outcome. J Neurosurg Spine. 2002;97:193–200.
Gault D, Morel-Fatio M, Albert T, Fattal C. Chronic neuropathic pain of spinal cord injury: what is the effectiveness of psychocomportemental management? Ann Phys Rehabil Med. 2009;52:167–72.
Norrbrink Budh C, Kowalski J, Lundeberg T. A comprehensive pain management programme comprising educational, cognitive and behavioural interventions for neuropathic pain following spinal cord injury. J Rehabil Med. 2006;38:172–80.
Boninger ML, Cooper RA, Baldwin MA, Shimada SD, Koontz A. Wheelchair pushrim kinetics: body weight and median nerve function. Arch Phys Med Rehabil. 1999;80:910–5.
Boninger ML, Impink BG, Cooper RA, Koontz AM. Relation between median and ulnar nerve function and wrist kinematics during wheelchair propulsion. Arch Phys Med Rehabil. 2004;85:1141–5.
Author information
Authors and Affiliations
Corresponding author
Additional information
This article is part of the Topical Collection on Spinal Cord Injury Rehabilitation.
Rights and permissions
About this article
Cite this article
Bryce, T.N., Gomez, J. Management of Pain After Spinal Cord Injury. Curr Phys Med Rehabil Rep 3, 189–196 (2015). https://doi.org/10.1007/s40141-015-0092-3
Published:
Issue Date:
DOI: https://doi.org/10.1007/s40141-015-0092-3