Abstract
Purpose
The objective of this study was to ascertain vital status of patients considered lost to follow-up at an HIV clinic in Guinea-Bissau, and describe reasons for loss to follow-up (LTFU).
Methods
This study was a cross-sectional sample of a prospective cohort, carried out between May 15, 2013, and January 31, 2014. Patients lost to follow-up, who lived within the area of the Bandim Health Project, a demographic surveillance site (DSS), were eligible for inclusion. Active follow-up was attempted by telephone and tracing by a field assistant. Semi-structured interviews were done face to face or by phone by a field assistant and patients were asked why they had not shown up for the scheduled appointment. Patients were included by date of HIV testing and risk factors for LTFU were assessed using Cox proportional hazard model.
Results
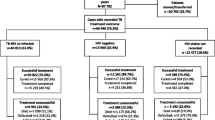
Among 561 patients (69.5 % HIV-1, 18.0 % HIV-2 and 12.6 % HIV-1/2) living within the DSS, 292 patients had been lost to follow-up and were, therefore, eligible for active follow-up. Vital status was ascertained in 65.9 % of eligible patients and 42.7 % were alive, while 23.2 % had died. Information on reasons for LTFU existed for 103 patients. Major reasons were moving (29.1 %), travelling (17.5 %), and transferring to other clinics (11.7 %).
Conclusion
A large proportion of the patients at the clinic were lost to follow-up. The main reason for this was found to be the geographic mobility of the population in Guinea-Bissau.

Similar content being viewed by others
References
WHO/UNICEF/UNAIDS. Global update on HIV treatment 2013: results, impact and opportunities. Geneva: World Health Organization; 2013.
Mills EJ, Bakanda C, Birungi J, Chan K, Ford N, Cooper CL, et al. Life expectancy of persons receiving combination antiretroviral therapy in low-income countries: a cohort analysis from Uganda. Ann Intern Med. 2011;155:209–16. doi:10.7326/0003-4819-155-4-201108160-00358.
Cohen MS, Chen YQ, McCauley M, Gamble T, Hosseinipour MC, Kumarasamy N, et al. Prevention of HIV-1 infection with early antiretroviral therapy. N Engl J Med. 2011;365:493–505. doi:10.1056/NEJMoa1105243.
Loutfy MR, Wu W, Letchumanan M, Bondy L, Antoniou T, Margolese S, et al. Systematic review of HIV transmission between heterosexual serodiscordant couples where the HIV-positive partner is fully suppressed on antiretroviral therapy. PLoS One. 2013;8:e55747. doi:10.1371/journal.pone.0055747.
Nsanzimana S, Remera E, Kanters S, Chan K, Forrest JI, Ford N, et al. Life expectancy among HIV-positive patients in Rwanda: a retrospective observational cohort study. Lancet Glob Health. 2015;3:e169–77. doi:10.1016/S2214-109X(14)70364-X.
Jean K, Gabillard D, Moh R, Danel C, Fassassi R, Desgrees-du-Lou A, et al. Effect of early antiretroviral therapy on sexual behaviors and HIV-1 transmission risk among adults with diverse heterosexual partnership statuses in Cote d’Ivoire. J Infect Dis. 2014;209:431–40. doi:10.1093/infdis/jit470.
WHO/UNAIDS. Global report: UNAIDS report on the global AIDS epidemic 2012. Geneva: World Health Organization; 2012.
WHO/UNAIDS. UNAIDS World AIDS Day Report Results. Geneva: World Health Organization; 2012. p. 2012.
UNAIDS. GAP report: HIV estimates with uncertainty bounds 1990–2012. http://www.unaids.org/en/dataanalysis/knowyourepidemic/epidemiologypublications/. Accessed 22 April 2014.
da Silva ZJ, Oliveira I, Andersen A, Dias F, Rodrigues A, Holmgren B, et al. Changes in prevalence and incidence of HIV-1, HIV-2 and dual infections in urban areas of Bissau, Guinea-Bissau: is HIV-2 disappearing? AIDS. 2008;22:1195–202. doi:10.1097/QAD.0b013e328300a33d.
Bartlett JA, Shao JF. Successes, challenges, and limitations of current antiretroviral therapy in low-income and middle-income countries. Lancet Infect Dis. 2009;9:637–49. doi:10.1016/s1473-3099(09)70227-0.
Brinkhof MW, Dabis F, Myer L, Bangsberg DR, Boulle A, Nash D, et al. Early loss of HIV-infected patients on potent antiretroviral therapy programmes in lower-income countries. Bull World Health Organ. 2008;86:559–67.
Larson BA, Brennan A, McNamara L, Long L, Rosen S, Sanne I, et al. Early loss to follow up after enrolment in pre-ART care at a large public clinic in Johannesburg, South Africa. Trop Med Int Health. 2010;15:43–7. doi:10.1111/j.1365-3156.2010.02511.x.
Amuron B, Namara G, Birungi J, Nabiryo C, Levin J, Grosskurth H, et al. Mortality and loss-to-follow-up during the pre-treatment period in an antiretroviral therapy programme under normal health service conditions in Uganda. BMC Public Health. 2009;9:290. doi:10.1186/1471-2458-9-290.
Togun T, Peterson I, Jaffar S, Oko F, Okomo U, Peterson K, et al. Pre-treatment mortality and loss-to-follow-up in HIV-1, HIV-2 and HIV-1/HIV-2 dually infected patients eligible for antiretroviral therapy in The Gambia, West Africa. AIDS Res Ther. 2011;8:24. doi:10.1186/1742-6405-8-24.
Castelnuovo B, Musaazi J, Musomba R, Ratanshi RP, Kiragga AN. Quantifying retention during pre-antiretroviral treatment in a large urban clinic in Uganda. BMC Infect Dis. 2015;15:252. doi:10.1186/s12879-015-0957-1.
Ahonkhai AA, Banigbe B, Adeola J, Onwuatuelo I, Bassett IV, Losina E, et al. High rates of unplanned interruptions from HIV care early after antiretroviral therapy initiation in Nigeria. BMC Infect Dis. 2015;15:397. doi:10.1186/s12879-015-1137-z.
Rosen S, Fox MP, Gill CJ. Patient retention in antiretroviral therapy programs in sub-Saharan Africa: a systematic review. PLoS Med. 2007;4:e298. doi:10.1371/journal.pmed.0040298.
Colubi MM, Perez-Elias MJ, Elias L, Pumares M, Muriel A, Zamora AM, et al. Missing scheduled visits in the outpatient clinic as a marker of short-term admissions and death. HIV Clin Trials. 2012;13:289–95. doi:10.1310/hct1305-289.
Sterne JA, May M, Costagliola D, de Wolf F, Phillips AN, Harris R, et al. Timing of initiation of antiretroviral therapy in AIDS-free HIV-1-infected patients: a collaborative analysis of 18 HIV cohort studies. Lancet. 2009;373:1352–63. doi:10.1016/s0140-6736(09)60612-7.
Bastard M, Nicolay N, Szumilin E, Balkan S, Poulet E, Pujades-Rodriguez M. Adults receiving HIV care before the start of antiretroviral therapy in sub-Saharan Africa: patient outcomes and associated risk factors. J Acquir Immune Defic Syndr. 2013;64:455–63. doi:10.1097/QAI.0b013e3182a61e8d.
Mugisha V, Teasdale CA, Wang C, Lahuerta M, Nuwagaba-Biribonwoha H, Tayebwa E, et al. Determinants of mortality and loss to follow-up among adults enrolled in HIV care services in Rwanda. PLoS One. 2014;9:e85774. doi:10.1371/journal.pone.0085774.
Geng EH, Bangsberg DR, Musinguzi N, Emenyonu N, Bwana MB, Yiannoutsos CT, et al. Understanding reasons for and outcomes of patients lost to follow-up in antiretroviral therapy programs in Africa through a sampling-based approach. J Acquir Immune Defic Syndr. 2010;53:405–11. doi:10.1097/QAI.0b013e3181b843f0.
Ware NC, Wyatt MA, Geng EH, Kaaya SF, Agbaji OO, Muyindike WR, et al. Toward an understanding of disengagement from HIV treatment and care in sub-Saharan Africa: a qualitative study. PLoS Med. 2013;10:e1001369. doi:10.1371/journal.pmed.1001369.
Mugglin C, Estill J, Wandeler G, Bender N, Egger M, Gsponer T, et al. Loss to programme between HIV diagnosis and initiation of antiretroviral therapy in sub-Saharan Africa: systematic review and meta-analysis. Trop Med Int Health. 2012;17:1509–20. doi:10.1111/j.1365-3156.2012.03089.x.
Asiimwe SB, Kanyesigye M, Bwana B, Okello S, Muyindike W. Predictors of dropout from care among HIV-infected patients initiating antiretroviral therapy at a public sector HIV treatment clinic in sub-Saharan Africa. BMC Infect Dis. 2016;16:43. doi:10.1186/s12879-016-1392-7.
Ulett KB, Willig JH, Lin HY, Routman JS, Abroms S, Allison J, et al. The therapeutic implications of timely linkage and early retention in HIV care. AIDS Patient Care STDs. 2009;23:41–9. doi:10.1089/apc.2008.0132.
Oliveira I, Andersen A, Furtado A, Medina C, da Silva D, da Silva ZJ, et al. Assessment of simple risk markers for early mortality among HIV-infected patients in Guinea-Bissau: a cohort study. BMJ Open. 2012;2:e001587. doi:10.1136/bmjopen-2012-001587.
Honge BL, Jespersen S, Nordentoft PB, Medina C, da Silva D, da Silva ZJ, et al. Loss to follow-up occurs at all stages in the diagnostic and follow-up period among HIV-infected patients in Guinea-Bissau: a 7-year retrospective cohort study. BMJ Open. 2013;3:e003499. doi:10.1136/bmjopen-2013-003499.
The official Bandim Health Project website. http://www.bandim.org/about-bhp.aspx. Accessed April 2014.
Chi BH, Yiannoutsos CT, Westfall AO, Newman JE, Zhou J, Cesar C, et al. Universal definition of loss to follow-up in HIV treatment programs: a statistical analysis of 111 facilities in Africa, Asia, and Latin America. PLoS Med. 2011;8:e1001111. doi:10.1371/journal.pmed.1001111.
Poulsen AG, Aaby P, Larsen O, Jensen H, Naucler A, Lisse IM, et al. 9-year HIV-2-associated mortality in an urban community in Bissau, west Africa. Lancet. 1997;349:911–4.
Wubshet M, Berhane Y, Worku A, Kebede Y. Death and seeking alternative therapy largely accounted for lost to follow-up of patients on ART in northwest Ethiopia: a community tracking survey. PLoS One. 2013;8:e59197. doi:10.1371/journal.pone.0059197.
Marson KG, Tapia K, Kohler P, McGrath CJ, John-Stewart GC, Richardson BA, et al. Male, mobile, and moneyed: loss to follow-up vs. transfer of care in an urban African antiretroviral treatment clinic. PLoS One. 2013;8:e78900. doi:10.1371/journal.pone.0078900.
Shastri S, Sathyanarayna S, Nagaraja SB, Kumar AM, Rewari B, Harries AD, et al. The journey to antiretroviral therapy in Karnataka, India: who was lost on the road? J Int AIDS Soc. 2013;16:18502. doi:10.7448/ias.16.1.18502.
Tweya H, Gugsa S, Hosseinipour M, Speight C, Ng’ambi W, Bokosi M, et al. Understanding factors, outcomes and reasons for loss to follow-up among women in Option B+ PMTCT programme in Lilongwe, Malawi. Trop Med Int Health. 2014;19:1360–6. doi:10.1111/tmi.12369.
Lubega M, Musenze IA, Joshua G, Dhafa G, Badaza R, Bakwesegha CJ, et al. Sex inequality, high transport costs, and exposed clinic location: reasons for loss to follow-up of clients under prevention of mother-to-child HIV transmission in eastern Uganda–a qualitative study. Patient Preference Adherence. 2013;7:447–54. doi:10.2147/ppa.s19327.
Myer L, el-Sadr W. Expanding access to antiretroviral therapy through the public sector-the challenge of retaining patients in long-term primary care. S Afr Med J. 2004;94:273–4.
Torpey KE, Kabaso ME, Mutale LN, Kamanga MK, Mwango AJ, Simpungwe J, et al. Adherence support workers: a way to address human resource constraints in antiretroviral treatment programs in the public health setting in Zambia. PLoS One. 2008;3:e2204. doi:10.1371/journal.pone.0002204.
Lester RT, Ritvo P, Mills EJ, Kariri A, Karanja S, Chung MH, et al. Effects of a mobile phone short message service on antiretroviral treatment adherence in Kenya (WelTel Kenya1): a randomised trial. Lancet. 2010;376:1838–45. doi:10.1016/s0140-6736(10)61997-6.
Losina E, Toure H, Uhler LM, Anglaret X, Paltiel AD, Balestre E, et al. Cost-effectiveness of preventing loss to follow-up in HIV treatment programs: a Cote d’Ivoire appraisal. PLoS Med. 2009;6:e1000173. doi:10.1371/journal.pmed.1000173.
Acknowledgments
The authors would like to thank the staff and patients at the HIV clinic. Special thanks to João Paulo Nanque, Joana Mendes and Quintino Lopes Ié for their work with tracing patients and to Zacarias da Silva and the laboratory staff working in the TB and HIV sections at the National Public Health Laboratory and to the office staff at the Bandim Health Project for making this study possible.
The Bissau HIV Cohort study group comprises: Amabelia Rodrigues, David da Silva, Zacarias da Silva, Candida Medina, Ines Oliviera-Souto, Lars Østergaard, Alex Laursen, Bo Hønge, Peter Aaby, Anders Fomsgaard, Christian Erikstrup, Sanne Jespersen and Christian Wejse (chair).
Funding was provided by Institut for Klinisk Medicin, and National Institutes of Health (Grant No. U01AI069919) through IeDEA.
Author information
Authors and Affiliations
Consortia
Corresponding author
Ethics declarations
Ethical statement
The HIV cohort at the outpatient clinic was approved by the National Ethics Committee in Guinea-Bissau in 2007 (Parecer NCP/No. 15/2007). Upon inclusion, patients sign a voluntary, informed consent, using fingerprint if illiterate. The cohort has an open approval to use data from patients’ records as long as patient confidentiality is not broken. This study was approved separately by the ethical committee in Guinea-Bissau (No. Ref. 060/CNES/INASA/2013). At all times field assistants were cautious not to disclose HIV status to anyone.
Conflict of interest
PBN has received funding from Institute of Clinical Medicine, Aarhus University, Denmark. WAPHIR and IeDEA supported data collection in Bissau. For the remaining authors none were declared.
Rights and permissions
About this article
Cite this article
Nordentoft, P.B., Engell-Sørensen, T., Jespersen, S. et al. Assessing factors for loss to follow-up of HIV infected patients in Guinea-Bissau. Infection 45, 187–197 (2017). https://doi.org/10.1007/s15010-016-0949-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s15010-016-0949-0