Abstract
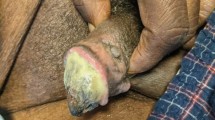
Calciphylaxis presents with painful purpura and intractable skin ulcers on the trunk and particularly the distal extremities, and it mainly occurs in patients on chronic dialysis. A 66-year-old man with renal failure due to diabetic nephropathy was on peritoneal dialysis alone for 1 year, followed by peritoneal dialysis combined with hemodialysis for 3 years. He developed calciphylaxis of the penis, which was diagnosed from the skin biopsy findings and clinical observation. To treat this condition, PD was stopped and HD was performed three times a week. In addition, warfarin therapy was discontinued and infusion of sodium thiosulfate was performed. The penile ulcers decreased in size and pain was markedly improved, so the patient was discharged from hospital. Following discharge, PD was resumed after changing the peritoneal dialysis fluid to bicarbonate-buffered dialysate. The penile ulcers eventually resolved completely. There have been very few reports about calciphylaxis in patients on combined dialysis modalities. In our patient, penile calciphylaxis progressed when lactate-buffered peritoneal dialysis fluid was used and resolved after switching to bicarbonate-buffered fluid together with cessation of warfarin therapy and infusion of sodium thiosulfate.

Similar content being viewed by others
References
Rogers NM, Coates PT. Calcific uraemic arteriolopathy: an update. Curr Opin Nephrol Hypertens. 2008;17(6):629–34.
Weenig RH. Pathogenesis of calciphylaxis: Hans Selye to nuclear factor k-B. J Am Acad Dermatol. 2008;58(3):458–71.
Daudén E, Oñate MJ. Calciphylaxis. Dermatol Clin. 2008;26(4):557–68.
Ng AT, Peng DH. Calciphylaxis. Dermatol Ther. 2011;24(2):256–62.
New N, Mohandas J, John GT, et al. Calcific uremic arteriolopathy in peritoneal dialysis populations. Int J Nephrol. 2011;2011:982854.
Ramani R, Ramachandran A, Ravindran S, Kurian GA. Erythrocyte membrane bound atpase and antioxidant enzyme changes associated with vascular calcification is reduced by sodium thiosulfate. Indian J Clin Biochem. 2017;32(4):487–92.
Bleyer AJ, Choi M, Igwemezie B, de la Torre E, White WL. A case–control study of proximal calciphylaxis. Am J Kidney Dis. 1998;32(3):376–83.
Mazhar AR, Johnson RJ, Gillen D, Stivelman JC, Ryan MJ, Davis CL, Stehman-Breen CO. Risk factors and mortality associated with calciphylaxis in end-stage renal disease. Kidney Int. 2001;60(1):324–32.
Fine A, Zacharias J. Calciphylaxis is usually nonulcerating: risk factors, outcome and therapy. Kidney Int. 2002;61(6):2210–7.
Weenig RH, Sewell LD, Davis MD, McCarthy JT, Pittelkow MR. Calciphylaxis: natural history, risk factor analysis, and outcome. J Am Acad Dermatol. 2007;56(4):569–79.
Ando R. Skin complications associated with dialysis 3. Calciphylaxis. Jpn J Clin Dial 2009;25(7):126–34 (in Japanese).
Paul S, Carlos AR, Vedak P, et al. The role of bone scintigraphy in the diagnosis of calciphylaxis. JAMA Dermatol. 2017;153(1):101–3.
Pliquentt RU, Schwock J, Padchke R, Achenbach H. Calciphylaxis in chronic, non-dialysis-dependent renal disease. BMC Nephrol. 2003;4:8.
Zhang Y, Corapi KM, Luongo M, Nigwekar SU. Calciphylaxis in peritoneal dialysis patients: a single cohort study. Int J Nephrol Renovasc Dis. 2016;9:235–41.
Angelis M, Wong LL, Myers SA, Wong LM. Calciphylaxis in patients on hemodialysis: a prevalence study. Surgery. 1997;122(6):1083–9.
Dosanjh A, Kebebew E. Calciphylaxis. Rare but Fatal. Curr Surg. 2005;62(5):455–8.
Chen W, Abramowitz MK. Treatment of metabolic acidosis in patients with CKD. Am J Kidney Dis. 2014;63(2):311–7.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors have no financial conflicts of interest to declare.
Human rights
All procedures performed in studies involving this participant was in accordance with the ethical standards of the institutional and national research committee at which the studies were conducted and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards.
Informed consent
Informed consent was obtained from the patient included in this study.
About this article
Cite this article
Kasai, T., Washida, N., Muraoka, H. et al. Penile calciphylaxis in a patient on combined peritoneal dialysis and hemodialysis. CEN Case Rep 7, 204–207 (2018). https://doi.org/10.1007/s13730-018-0327-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s13730-018-0327-0