Abstract
Purpose of Review
Actinic keratosis (AK) is the most common sun-induced preneoplastic lesion, and together with photo-aging and skin cancer, it places a huge burden on healthcare systems. The clinical distinction between AK and incipient squamous cell carcinoma (SCC) can be difficult, and therefore, clinical diagnosis is not always reliable and certain. Skin biopsies are sometimes mandatory, and physicians must be aware of the importance of accurate diagnosis and management, as other malignant neoplasms (melanoma, basal cell carcinoma) cannot always be reliably distinguished from AK, especially when pigmented and inflamed.
Recent Findings
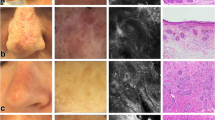
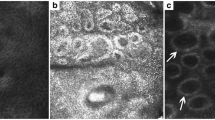
Although histopathology remains the gold standard for differentiation of AK from SCC, some non-invasive optical technologies such as dermoscopy and reflectance confocal microscopy have recently been applied to enhance clinical diagnosis accuracy and to obtain an in vivo characterization of these lesions.
Summary
The combination of dermoscopy with reflectance confocal microscopy improves the clinical assessment and diagnosis of equivocal keratinizing tumors, allows the selection of the most suspicious areas for biopsy, and permits non-invasive determination of treatment outcomes.




Similar content being viewed by others
References
Papers of particular interest, published recently, have been highlighted as: • Of importance •• Of major importance
Callen JP, Bickers DR, Moy RL. Actinic keratoses. J Am Acad Dermatol. 1997;36:650–3.
•• Pellacani G, Ulrich M, Casari A, et al. Grading keratinocyte atypia in actinic keratosis: a correlation of reflectance confocal microscopy and histopathology. J Eur Acad Dermatol Venereol. 2015;29(11):2216–21. This study provides a thorough description of keratinocyte atypia in dermoscopy and reflectance confocal microscopy and correlates the findigngs in order to establish criteria that could help to distinguish AK from SCC.
Ackerman AB, Mones JM. Solar (actinic) keratosis is squamous cell carcinoma. Br J Dermatol. 2006;155(1):9–22.
•• Peppelman M, Nguyen KP, Hoogedoorn L, van Erp PEJ, Gerritsen M-JP. Reflectance confocal microscopy: non-invasive distinction between actinic keratosis and squamous cell carcinoma. J Eur Acad Dermatol Venereol. 2015;29(7):1302–9. This study provides some clues that might help to distinguish AK from SCC in reflectance confocal microscopy.
Marks R, Rennie G, Selwood T. Malignant transformation of solar keratoses to squamous cell carcinoma. Lancet. 1988;331(8589):795–7.
Quaedvlieg PJF, Tirsi E, Thissen MRTM, Krekels GA. Actinic keratosis: how to differentiate the good from the bad ones? Eur J Dermatology. 2006;16(4):335–9.
Ulrich M, Stockfleth E, Roewert-Huber J, Astner S. Noninvasive diagnostic tools for nonmelanoma skin cancer. Br J Dermatol. 2007;157(157 Suppl):56–8.
Warszawik-Hendzel O, Olszewska M, Maj M, Rakowska A, Czuwara J, Rudnicka L. Non-invasive diagnostic techniques in the diagnosis of squamous cell carcinoma. J Dermatol Case Rep. 2015;9(4):89–97.
Moscarella E, Rabinovitz H, Zalaudek I, Piana S, Stanganelli I, Oliviero MC, et al. Dermoscopy and reflectance confocal microscopy of pigmented actinic keratoses: a morphological study. J Eur Acad Dermatol Venereol. 2015;29(2):307–14.
Rosendahl C, Cameron A, Argenziano G, Zalaudek I, Tschandl P, Kittler H. Dermoscopy of squamous cell carcinoma and keratoacanthoma. Arch Dermatol. 2012;148(12):1386–92.
Zalaudek I, Giacomel J, Argenziano G, Hofmann-Wellenhof R, Micantonio T, di Stefani A, et al. Dermoscopy of facial nonpigmented actinic keratosis. Br J Dermatol. 2006;155(5):951–6.
• Zalaudek I, Giacomel J, Schmid K, et al. Dermatoscopy of facial actinic keratosis, intraepidermal carcinoma, and invasive squamous cell carcinoma: a progression model. J Am Acad Dermatol. 2012;66(4):589–97. This study illustrates the cancerization field concept, where AKs and SCCs might represent extreme ends of the same disease spectrum.
Peris K, Calzavara-Pinton PG, Neri L, Girolomoni G, Malara G, Parodi A, et al. Italian expert consensus for the management of actinic keratosis in immunocompetent patients. J Eur Acad Dermatol Venereol. 2016;30(7):1077–84.
Cuellar F, Vilalta A, Puig S, Palou J, Salerni G, Malvehy J. New dermoscopic pattern in actinic keratosis and related conditions. Arch Dermatol. 2009;145(6):732.
Pan Y, Chamberlain AJ, Bailey M, Chong AH, Haskett M, Kelly JW. Dermatoscopy aids in the diagnosis of the solitary red scaly patch or plaque-features distinguishing superficial basal cell carcinoma, intraepidermal carcinoma, and psoriasis. J Am Acad Dermatol. 2008;59(2):268–74.
Hofmann-Wellenhof R, Pellacani G, Malvehy J, Soyer HP. Reflectance confocal microscopy for skin diseases; 2012.
Carrera C, Puig S, Malvehy J. In vivo confocal reflectance microscopy in melanoma. Dermatol Ther. 2012;25(5):410–22.
Rajadhyaksha M, González S, Zavislan JM, Anderson RR, Webb RH. In vivo confocal scanning laser microscopy of human skin II: advances in instrumentation and comparison with histology. J Invest Dermatol. 1999;113(3):293–303.
Scope A, Benvenuto-Andrade C, Agero ALC, Malvehy J, Puig S, Rajadhyaksha M, et al. In vivo reflectance confocal microscopy imaging of melanocytic skin lesions: consensus terminology glossary and illustrative images. J Am Acad Dermatol. 2007;57(4):644–58.
Pellacani G, Vinceti M, Bassoli S, Braun R, Gonzalez S, Guitera P, et al. Reflectance confocal microscopy and features of melanocytic lesions: an internet-based study of the reproducibility of terminology. Arch Dermatol. 2009;145(10):1137–43.
Rishpon A, Kim N, Scope A, Porges L, Oliviero MC, Braun RP, et al. Reflectance confocal microscopy criteria for squamous cell carcinomas and actinic keratoses. Arch Dermatol. 2009;145(7):766–72.
Malvehy J, Hanke-Martinez M, Costa J, Salerni G, Carrera C, Puig S Semiology and pattern analysis in nonmelanocytic lesions. In: Reflectance Confocal Microscopy for Skin Diseases; 2012:237–252.
Seyed Jafari SM, Timchik T, Hunger RE. In vivo confocal microscopy efficacy assessment of daylight photodynamic therapy in actinic keratosis patients. Br J Dermatol. 2016;175(2):375–81.
Funding
Research at the Melanoma Unit in Barcelona is partially funded by Spanish Fondo de Investigaciones Sanitarias grants 15/00956 and 15/00716; co-financed by European Development Regional Fund “A way to achieve Europe” ERDF; AGAUR 2014_SGR_603 of the Catalan Government, Spain; the European Commission under the 6th Framework Programme, Contract No. LSHC-CT-2006-018702 (GenoMEL); the European Commission under the 7th Framework Programme, Diagnoptics; the National Cancer Institute (NCI) of the US National Institute of Health (NIH) (CA83115); and a grant from “Fundació La Marató de TV3, 201331-30,” Catalonia, Spain and a Research Grant from Asociación Española Contra el Cancer.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of Interest
The authors declare that they have no conflict of interest.
Human and Animal Rights and Informed Consent
This article does not contain any studies with human or animal subjects performed by any of the authors.
Additional information
This article is part of the Topical Collection on Skin Cancer
Rights and permissions
About this article
Cite this article
Combalia, A., Fustà-Novell, X., Alejo, B. et al. Actinic Keratosis—Can Dermoscopy or RCM Differentiate AK (Not Full Thickness Atypia) from Full-Thickness Atypia/Invasive SCC?. Curr Derm Rep 7, 75–83 (2018). https://doi.org/10.1007/s13671-018-0219-8
Published:
Issue Date:
DOI: https://doi.org/10.1007/s13671-018-0219-8