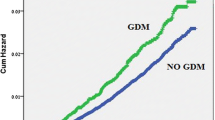
Abstract
Diabetes mellitus has reached epidemic proportions in both the USA and worldwide with most authorities reporting a doubling in the prevalence of diabetes over the last 20–30 years. While this epidemic is closely tied to obesity, diabetes mellitus presents potential clinical challenges over and above that observed with obesity alone. From a women’s healthcare prospective, this rise in diabetes may impact a woman’s health across her lifespan. More specifically, diabetes impacts not only pregnancy as well as other medical conditions but increases the risk for the development of various malignancies. From a gynecologic cancer standpoint, diabetes is most closely associated with endometrial adenocarcinomas, although increasing attention is being placed upon diabetes and ovarian cancer. Attention is also being placed on the potential role of metformin and its impact on outcomes in diabetics with cancer, as well as a potential preventative and/or adjunctive therapy for gynecologic cancer.
Similar content being viewed by others
References
Papers of particular interest, published recently, have been highlighted as: • Of importance
Organization W.H. Global status report on noncommunicable diseases 2014. Geneza: World Health Organization; 2014.
Zimmet PZ et al. Diabetes: a 21st century challenge. Lancet Diabet Endocrinol. 2014;2(1):56–64.
Chen L, Magliano DJ, Zimmet PZ. The worldwide epidemiology of type 2 diabetes mellitus—present and future perspectives. Nat Rev Endocrinol. 2012;8(4):228–36.
Siegel RL, Miller KD, Jemal A. Cancer statistics, 2015. CA Cancer J Clin. 2015;65(1):5–29.
Romero IL et al. Relationship of type II diabetes and metformin use to ovarian cancer progression, survival, and chemosensitivity. Obstet Gynecol. 2012;119(1):61–7. Although containing a limited number of diabetics receiving metformin, 16 of 44 diabetic patients, the marked difference in outcomes when compared to both non-diabetics as well as diabetics not on metformin was quite provocative.
Shah MM et al. Diabetes mellitus and ovarian cancer: more complex than just increasing risk. Gynecol Oncol. 2014;135(2):273–7. More recent series that again demonstrates inferior ovarian cancer survival for diabetics, with generally similar clinical covariates, when compared to non-diabetics.
Bakhru A, Buckanovich RJ, Griggs JJ. The impact of diabetes on survival in women with ovarian cancer. Gynecol Oncol. 2011;121(1):106–11.
Prevention C.f.D.C.a. National Diabetes Statistics Report: Estimates of Diabetes and Its Burden in the United States, 2014. 2014; Available from: http://www.cdc.gov/diabetes/pubs/statsreport14/national-diabetes-report-web.pdf.
Stine JE, Bae-Jump V. Metformin and gynecologic cancers. Obstet Gynecol Surv. 2014;69(8):477–89.
Friberg E et al. Diabetes mellitus and risk of endometrial cancer: a meta-analysis. Diabetologia. 2007;50(7):1365–74.
Liu X, et al. Cancer risk in patients with type 2 diabetes mellitus and their relatives. Int J Cancer. 2015.
Luo J et al. Association between diabetes, diabetes treatment and risk of developing endometrial cancer. Br J Cancer. 2014;111(7):1432–9.
Stocks T, et al. Metabolic risk score and cancer risk: pooled analysis of seven cohorts. Int J Epidemiol. 2015.
Trabert B et al. Metabolic syndrome and risk of endometrial cancer in the United States: a study in the SEER-medicare linked database. Cancer Epidemiol Biomarkers Prev. 2015;24(1):261–7.
Esposito K et al. Metabolic syndrome and endometrial cancer: a meta-analysis. Endocrine. 2014;45(1):28–36.
Zanders MM et al. Effect of diabetes on endometrial cancer recurrence and survival. Maturitas. 2013;74(1):37–43.
Bailey CJ, Turner RC. Metformin. N Engl J Med. 1996;334(9):574–9.
Quinn BJ et al. Repositioning metformin for cancer prevention and treatment. Trends Endocrinol Metab. 2013;24(9):469–80.
Evans JM et al. Metformin and reduced risk of cancer in diabetic patients. BMJ. 2005;330(7503):1304–5.
Soffer D et al. Metformin and breast and gynecological cancer risk among women with diabetes. BMJ Open Diabetes Res Care. 2015;3(1):e000049.
Currie CJ et al. Mortality after incident cancer in people with and without type 2 diabetes: impact of metformin on survival. Diabetes Care. 2012;35(2):299–304.
Nevadunsky NS et al. Metformin use and endometrial cancer survival. Gynecol Oncol. 2014;132(1):236–40.
Ko EM et al. Metformin and the risk of endometrial cancer: a population-based cohort study. Gynecol Oncol. 2015;136(2):341–7.
Tabrizi AD et al. Antiproliferative effect of metformin on the endometrium—a clinical trial. Asian Pac J Cancer Prev. 2014;15(23):10067–70.
Cantrell LA et al. Metformin is a potent inhibitor of endometrial cancer cell proliferation—implications for a novel treatment strategy. Gynecol Oncol. 2010;116(1):92–8.
Mitsuhashi A et al. Effects of metformin on endometrial cancer cell growth in vivo: a preoperative prospective trial. Cancer. 2014;120(19):2986–95.
Hanna RK et al. Metformin potentiates the effects of paclitaxel in endometrial cancer cells through inhibition of cell proliferation and modulation of the mTOR pathway. Gynecol Oncol. 2012;125(2):458–69.
Uehara T et al. Metformin potentiates the anticancer effects of cisplatin under normoxic conditions in vitro. Oncol Rep. 2015;33(2):744–50.
Morgan Jr RJ et al. Ovarian cancer, version 2.2013. J Natl Compr Canc Netw. 2013;11(10):1199–209.
Tewari D et al. Long-term survival advantage and prognostic factors associated with intraperitoneal chemotherapy treatment in advanced ovarian cancer: a gynecologic oncology group study. J Clin Oncol. 2015;33(13):1460–6.
Landrum LM et al. Prognostic factors for stage III epithelial ovarian cancer treated with intraperitoneal chemotherapy: a Gynecologic Oncology Group study. Gynecol Oncol. 2013;130(1):12–8.
Olsen CM et al. Obesity and the risk of epithelial ovarian cancer: a systematic review and meta-analysis. Eur J Cancer. 2007;43(4):690–709.
Protani MM, Nagle CM, Webb PM. Obesity and ovarian cancer survival: a systematic review and meta-analysis. Cancer Prev Res (Phila). 2012;5(7):901–10.
Yang HS et al. Effect of obesity on survival of women with epithelial ovarian cancer: a systematic review and meta-analysis of observational studies. Int J Gynecol Cancer. 2011;21(9):1525–32.
Collaborative Group on Epidemiological Studies of Ovarian, C. Ovarian cancer and body size: individual participant meta-analysis including 25,157 women with ovarian cancer from 47 epidemiological studies. PLoS Med. 2012;9(4):e1001200.
Ma X et al. Anthropometric measures and epithelial ovarian cancer risk among Chinese women: results from the Shanghai Women’s Health Study. Br J Cancer. 2013;109(3):751–5.
Kalli KR, Conover CA. The insulin-like growth factor/insulin system in epithelial ovarian cancer. Front Biosci. 2003;8:d714–22.
Lukanova A, Kaaks R. Endogenous hormones and ovarian cancer: epidemiology and current hypotheses. Cancer Epidemiol Biomarkers Prev. 2005;14(1):98–107.
Howe LR et al. Molecular pathways: adipose inflammation as a mediator of obesity-associated cancer. Clin Cancer Res. 2013;19(22):6074–83.
Joung KH, Jeong JW, Ku BJ. The association between type 2 diabetes mellitus and women cancer: the epidemiological evidences and putative mechanisms. Biomed Res Int. 2015;2015:920618.
Nagle CM, et al. Obesity and survival among women with ovarian cancer: results from the Ovarian Cancer Association Consortium. Br J Cancer. 2015.
Nagle CM et al. Carbohydrate intake, glycemic load, glycemic index, and risk of ovarian cancer. Ann Oncol. 2011;22(6):1332–8.
Lee JY et al. Diabetes mellitus and ovarian cancer risk: a systematic review and meta-analysis of observational studies. Int J Gynecol Cancer. 2013;23(3):402–12.
Febbraro T, Lengyel E, Romero IL. Old drug, new trick: repurposing metformin for gynecologic cancers? Gynecol Oncol. 2014;135(3):614–21.
Lengyel E et al. Metformin inhibits ovarian cancer growth and increases sensitivity to paclitaxel in mouse models. Am J Obstet Gynecol. 2015;212(4):479. e1-479 e10.
Bodmer M et al. Use of metformin and the risk of ovarian cancer: a case–control analysis. Gynecol Oncol. 2011;123(2):200–4.
Kumar S et al. Metformin intake is associated with better survival in ovarian cancer: a case–control study. Cancer. 2013;119(3):555–62. Well designed case–control study again noting differential impacts on survival in women utilizing metformin with superior survival in those on metformin therapy.
Compliance with Ethics Guidelines
Conflict of Interest
Brittany Lees declares no conflict of interest.
Charles A. Leath, III declares contracted research in Ovarian Cancer from Novartis and from Astra Zeneza, outside the submitted work.
Human and Animal Rights and Informed Consent
This article does not contain any studies with human or animal subjects performed by any of the authors.
Support
Funding support was provided in part by NIH to CAL 5K12HD0012580-15.
Author information
Authors and Affiliations
Corresponding author
Additional information
This article is part of the Topical Collection on Gynecologic Oncology
Rights and permissions
About this article
Cite this article
Lees, B., Leath, C.A. The Impact of Diabetes on Gynecologic Cancer: Current Status and Future Directions. Curr Obstet Gynecol Rep 4, 234–239 (2015). https://doi.org/10.1007/s13669-015-0127-x
Published:
Issue Date:
DOI: https://doi.org/10.1007/s13669-015-0127-x