Abstract
Purpose of review
Recurrent post-prandial metabolic imbalances are important contributing factors to the development of cardiovascular disease (CVD). This study evaluated whether anthocyanin consumption attenuates the deleterious postprandial response of high-fat meals on CVD risk factors including blood pressure, vascular endothelial function, lipid profile and biomarkers related to oxidative stress, antioxidant status and immune response.
Recent findings
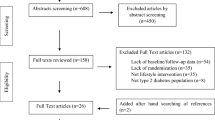
Five electronic databases were searched up to the period of 1 February 2020, yielding 13 eligible studies, including randomised or cross-over clinical trials (18–59 years of age), using PRISMA guidelines (PROSPERO registration: CRD42019126265). Potential bias was assessed using the revised Cochrane risk-of-bias tool for randomised trials. Beneficial effects of anthocyanins were reported in biomarkers of oxidative stress and antioxidant status in 6 out of 9 studies, and in 3 out of 6 studies for inflammatory response. Two positive results were found concerning attenuation of post-prandial endothelial dysfunction, increased triacylglycerol and total cholesterol exerted by the high fat meal. Blood pressure and lipoproteins were the parameters with least beneficial results.
Summary
Our systematic literature review revealed beneficial effects of dietary anthocyanin interventions on CVD risk factors following a HFM challenge; however, heterogeneity in results exists. The most promising results were for the attenuation of deleterious postprandial effects on oxidative stress and antioxidant status, triacylglycerol and total cholesterol concentrations, vascular endothelial function and inflammatory biomarkers. Post-prandial changes in blood pressure and lipoproteins were least affected by anthocyanins. Further studies are required in order to better elucidate the post-prandial effects of anthocyanins and CVD risk factors.

Similar content being viewed by others
References
Papers of particular interest, published recently, have been highlighted as: • Of importance •• Of major importance
Cardiovascular diseases (CVDs) [Internet]. [cited 2019 May 14]. Available from: https://www.who.int/news-room/fact-sheets/detail/cardiovascular-diseases-(cvds).
Slawson DL, Fitzgerald N, Morgan KT. Position of the academy of nutrition and dietetics: the role of nutrition in health promotion and chronic disease prevention. J Acad Nutr Diet. 2013;113:972–9.
•• Wallace JP, Johnson B, Padilla J, Mather K. Postprandial lipaemia, oxidative stress and endothelial function: a review. Int J Clin Pract. 2010;64:389–403. Important paper focused in the postprandial state and how oxidative stress mediates the adverse effects of postprandial lipaemia on endothelial function
Bravo E, Napolitano M, Botham KM. Postprandial lipid metabolism: the missing link between life-style habits and the increasing incidence of metabolic diseases in Western countries?~!2009-09-30~!2010-01-26~!2010-03-30~! Open Transl Med J. 2010;2:1–13.
Botham KM, Wheeler-Jones CPD. Postprandial lipoproteins and the molecular regulation of vascular homeostasis. Prog Lipid Res. 2013;52:446–64.
Wu JHY, Micha R, Mozaffarian D. Dietary fats and cardiometabolic disease: mechanisms and effects on risk factors and outcomes. Nat Rev Cardiol. 2019;16:581–601.
Polley KR, Kamal F, Paton CM, Cooper JA. Appetite responses to high-fat diets rich in mono-unsaturated versus poly-unsaturated fats. Appetite. 2019;134:172–81.
Masson CJ, Mensink RP. Exchanging saturated fatty acids for (n-6) polyunsaturated fatty acids in a mixed meal may decrease postprandial lipemia and markers of inflammation and endothelial activity in overweight men. J Nutr. 2011;141:816–21.
Muñoz A, Costa M. Nutritionally mediated oxidative stress and inflammation. Oxidative Med Cell Longev. 2013;2013:1–11.
Burton-Freeman B. Postprandial metabolic events and fruit-derived phenolics: a review of the science. Br J Nutr. 2010;104:S1–14.
•• Reis JF, VVS M, de Souza Gomes R, do Carmo MM, da Costa GV, Ribera PC, et al. Action mechanism and cardiovascular effect of anthocyanins: a systematic review of animal and human studies. J Transl Med. 2016;14:315. Relevant evidence of the effect of anthocyanins in cardiovascular diseases and underlying mechanisms
Smeriglio A, Barreca D, Bellocco E, Trombetta D. Chemistry, pharmacology and health benefits of anthocyanins. Phytother Res PTR. 2016;30:1265–86.
Cassidy A, Mukamal KJ, Liu L, Franz M, Eliassen AH, Rimm EB. High anthocyanin intake is associated with a reduced risk of myocardial infarction in young and middle-aged women. Circulation. 2013;127:188–96.
Cassidy A, Bertoia M, Chiuve S, Flint A, Forman J, Rimm EB. Habitual intake of anthocyanins and flavanones and risk of cardiovascular disease in men. Am J Clin Nutr. 2016;104:587–94.
Fairlie-Jones L, Davison K, Fromentin E, Hill A. The effect of anthocyanin-rich foods or extracts on vascular function in adults: a systematic review and meta-analysis of randomised controlled trials. Nutrients. 2017;9:908.
Traustadóttir T, Davies SS, Stock AA, Su Y, Heward CB, Roberts LJ, et al. Tart cherry juice decreases oxidative stress in healthy older men and women. J Nutr. 2009;139:1896–900.
Davinelli S, Bertoglio JC, Zarrelli A, Pina R, Scapagnini G. A randomized clinical trial evaluating the efficacy of an anthocyanin-Maqui berry extract (Delphinol®) on oxidative stress biomarkers. J Am Coll Nutr. 2015;34(Suppl 1):28–33.
Li D, Zhang Y, Liu Y, Sun R, Xia M. Purified anthocyanin supplementation reduces dyslipidemia, enhances antioxidant capacity, and prevents insulin resistance in diabetic patients. J Nutr. 2015;145:742–8.
Basu A, Betts NM, Ortiz J, Simmons B, Wu M, Lyons TJ. Low-calorie cranberry juice decreases lipid oxidation and increases plasma antioxidant capacity in women with metabolic syndrome. Nutr Res N Y N. 2011;31:190–6.
Kuntz S, Kunz C, Herrmann J, Borsch CH, Abel G, Fröhling B, et al. Anthocyanins from fruit juices improve the antioxidant status of healthy young female volunteers without affecting anti-inflammatory parameters: results from the randomised, double-blind, placebo-controlled, cross-over ANTHONIA (ANTHOcyanins in nutrition investigation Alliance) study. Br J Nutr. 2014;112:925–36.
Kardum N, Konić-Ristić A, Savikin K, Spasić S, Stefanović A, Ivanišević J, et al. Effects of polyphenol-rich chokeberry juice on antioxidant/pro-oxidant status in healthy subjects. J Med Food. 2014;17:869–74.
• Wallace TC, Slavin M, Frankenfeld CL. Systematic review of anthocyanins and markers of cardiovascular disease. Nutrients. 2016;8. Evidence of longer supplementation (not acute/postprandial) of anthocyanins in markers of cardiovascular disease
• Mora S, Rifai N, Buring JE, Ridker PM. Fasting compared with nonfasting lipids and apolipoproteins for predicting incident cardiovascular events. Circulation. 2008;118:993–1001. Important information distinguishing the implications of fasting and postprandial lipid in predicting cardiovascular events
Bansal S, Buring JE, Rifai N, Mora S, Sacks FM, Ridker PM. Fasting compared with nonfasting triglycerides and risk of cardiovascular events in women. JAMA. 2007;298:309–16.
Zhu Y, Ling W, Guo H, Song F, Ye Q, Zou T, et al. Anti-inflammatory effect of purified dietary anthocyanin in adults with hypercholesterolemia: a randomized controlled trial. Nutr Metab Cardiovasc Dis. 2013;23:843–9.
Edirisinghe I, Banaszewski K, Cappozzo J, Sandhya K, Ellis CL, Tadapaneni R, et al. Strawberry anthocyanin and its association with postprandial inflammation and insulin. Br J Nutr. 2011;106:913–22.
Liberati A, Altman DG, Tetzlaff J, Mulrow C, Gøtzsche PC, Ioannidis JPA, et al. The PRISMA statement for reporting systematic reviews and meta-analyses of studies that evaluate health care interventions: explanation and elaboration. PLoS Med. 2009;6:e1000100.
Sterne JAC, Savović J, Page MJ, Elbers RG, Blencowe NS, Boutron I, et al. RoB 2: a revised tool for assessing risk of bias in randomised trials. BMJ [Internet]. 2019;366:l4898 [cited 2020 Mar 4]; Available from: https://www.bmj.com/content/366/bmj.l4898.
Alqurashi RM, Galante LA, Rowland IR, Spencer JP, Commane DM. Consumption of a flavonoid-rich açai meal is associated with acute improvements in vascular function and a reduction in total oxidative status in healthy overweight men. Am J Clin Nutr. 2016;104:1227–35.
Miglio C, Peluso I, Raguzzini A, Villaño DV, Cesqui E, Catasta G, et al. Fruit juice drinks prevent endogenous antioxidant response to high-fat meal ingestion. Br J Nutr. 2014;111:294–300.
Peluso I, Raguzzini A, Villano VD, Cesqui E, Toti E, Catasta G, et al. High fat meal increase of IL-17 is prevented by ingestion of fruit juice drink in healthy overweight subjects. Curr Pharm Des. 2012;18:85–90.
Polley KR, Oswell NJ, Pegg RB, Cooper JA. Tart cherry consumption with or without prior exercise increases antioxidant capacity and decreases triglyceride levels following a high-fat meal. Appl Physiol Nutr Metab Physiol Appl Nutr Metab. 2019;44:1209–18.
Huebbe P, Giller K, de Pascual-Teresa S, Arkenau A, Adolphi B, Portius S, et al. Effects of blackcurrant-based juice on atherosclerosis-related biomarkers in cultured macrophages and in human subjects after consumption of a high-energy meal. Br J Nutr. 2012;108:234–44.
Ono-Moore KD, Snodgrass RG, Huang S, Singh S, Freytag TL, Burnett DJ, et al. Postprandial inflammatory responses and free fatty acids in plasma of adults who consumed a moderately high-fat breakfast with and without blueberry powder in a randomized placebo-controlled trial. J Nutr. 2016;146:1411–9.
Park E, Edirisinghe I, Wei H, Vijayakumar LP, Banaszewski K, Cappozzo JC, et al. A dose-response evaluation of freeze-dried strawberries independent of fiber content on metabolic indices in abdominally obese individuals with insulin resistance in a randomized, single-blinded, diet-controlled crossover trial. Mol Nutr Food Res. 2016;60:1099–109.
Huang Y, Park E, Edirisinghe I, Burton-Freeman BM. Maximizing the health effects of strawberry anthocyanins: understanding the influence of the consumption timing variable. Food Funct. 2016;7:4745–52.
Kay CD, Holub BJ. The effect of wild blueberry (Vaccinium angustifolium) consumption on postprandial serum antioxidant status in human subjects. Br J Nutr. 2002;88:389–97.
Richter CK, Skulas-Ray AC, Gaugler TL, Lambert JD, Proctor DN, Kris-Etherton PM. Incorporating freeze-dried strawberry powder into a high-fat meal does not alter postprandial vascular function or blood markers of cardiovascular disease risk: a randomized controlled trial. Am J Clin Nutr. 2017;105:313–22.
Cerletti C, Gianfagna F, Tamburrelli C, De Curtis A, D’Imperio M, Coletta W, et al. Orange juice intake during a fatty meal consumption reduces the postprandial low-grade inflammatory response in healthy subjects. Thromb Res. 2015;135:255–9.
Urquiaga I, Ávila F, Echeverria G, Perez D, Trejo S, Leighton F. A Chilean berry concentrate protects against postprandial oxidative stress and increases plasma antioxidant activity in healthy humans. Oxidative Med Cell Longev. 2017;2017:1–13.
Prior RL. Oxygen radical absorbance capacity (ORAC): new horizons in relating dietary antioxidants/bioactives and health benefits. J Funct Foods. 2015;18:797–810.
Ras RT, Streppel MT, Draijer R, Zock PL. Flow-mediated dilation and cardiovascular risk prediction: a systematic review with meta-analysis. Int J Cardiol. 2013;168:344–51.
Inaba Y, Chen JA, Bergmann SR. Prediction of future cardiovascular outcomes by flow-mediated vasodilatation of brachial artery: a meta-analysis. Int J Card Imaging. 2010;26:631–40.
•• Emerson SR, Kurti SP, Harms CA, Haub MD, Melgarejo T, Logan C, et al. Magnitude and timing of the postprandial inflammatory response to a high-fat meal in healthy adults: a systematic review. Adv Nutr Int Rev J. 2017;8:213–25. Evidence of how high-fat meal challenges exert effects of in the post-prandial inflammatory response in humans
Volpato S, Guralnik JM, Ferrucci L, Balfour J, Chaves P, Fried LP, et al. Cardiovascular disease, interleukin-6, and risk of mortality in older women: the Women’s health and aging study. Circulation. 2001;103:947–53.
Su D, Li Z, Li X, Chen Y, Zhang Y, Ding D, et al. Association between serum interleukin-6 concentration and mortality in patients with coronary artery disease. Mediat Inflamm. 2013;2013:1–7.
Bacchiega BC, Bacchiega AB, Usnayo MJG, Bedirian R, Singh G, Pinheiro GRC. Interleukin 6 inhibition and coronary artery disease in a high-risk population: a prospective community-based clinical study. J Am Heart Assoc [Internet]. 2017;6(3):e005038 [cited 2019 May 25]; Available from: https://www.ahajournals.org/doi/10.1161/JAHA.116.005038.
Morais CA, de Rosso VV, Estadella D, Pisani LP. Anthocyanins as inflammatory modulators and the role of the gut microbiota. J Nutr Biochem. 2016;33:1–7.
Kaori M, Makiko T, Shuhei O, Shigetaka F, Manabu S, Hideki M, et al. Association between onterleukin-6 levels and first-ever cerebrovascular events in patients with vascular risk factors. Arterioscler Thromb Vasc Biol American Heart Association. 2013;33:400–5.
Wainstein MV, Mossmann M, Araujo GN, Gonçalves SC, Gravina GL, Sangalli M, et al. Elevated serum interleukin-6 is predictive of coronary artery disease in intermediate risk overweight patients referred for coronary angiography. Diabetol Metab Syndr [Internet]. 2017;9:67 [cited 2020 May 30]; Available from: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5585915/.
Danesh J, Kaptoge S, Mann AG, Sarwar N, Wood A, Angleman SB, et al. Long-term interleukin-6 levels and subsequent risk of coronary heart disease: two new prospective studies and a systematic review. PLoS Med [Internet]. 2008;5(4):e78 [cited 2020 May 30]; Available from: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC2288623/.
Zhang B, Li X-L, Zhao C-R, Pan C-L, Zhang Z. Interleukin-6 as a predictor of the risk of cardiovascular disease: a meta-analysis of prospective epidemiological studies. Immunol Invest Taylor & Francis. 2018;47:689–99.
Williams ES, Shah SJ, Ali S, Na BY, Schiller NB, Whooley MA. C-reactive protein, diastolic dysfunction, and risk of heart failure in patients with coronary disease: heart and soul study. Eur J Heart Fail. 2008;10:63–9.
Ridker PM, Kastelein JJP, Genest J, Koenig W. C-reactive protein and cholesterol are equally strong predictors of cardiovascular risk and both are important for quality clinical care. Eur Heart J. 2013;34:1258–61.
Cozlea DL, Farcas DM, Nagy A, Keresztesi AA, Tifrea R, Cozlea L, et al. The impact of C reactive protein on global cardiovascular risk on patients with coronary artery disease. Curr Health Sci J. 2013;39:225–31.
Hein TW, Singh U, Vasquez-Vivar J, Devaraj S, Kuo L, Jialal I. Human C-reactive protein induces endothelial dysfunction and uncoupling of eNOS in vivo. Atherosclerosis. 2009;206:61–8.
Devaraj S, Kumaresan PR, Jialal I. C-reactive protein induces release of both endothelial microparticles and circulating endothelial cells in vitro and in vivo: further evidence of endothelial dysfunction. Clin Chem. 2011;57:1757–61.
Urschel K, Cicha I. TNF-α in the cardiovascular system: from physiology to therapy [Internet]. Int J Interferon Cytokine Mediat Res. 2015;7:9–25 [cited 2019 May 29]. Available from: https://www.dovepress.com/tnf-alpha-in-the-cardiovascular-system-from-physiology-to-therapy-peer-reviewed-fulltext-article-IJICMR.
Zhang H, Park Y, Wu J, Ping CX, Lee S, Yang J, et al. Role of TNF-α in vascular dysfunction. Clin Sci Lond Engl 1979. 2009;116:219–30.
Robert M, Miossec P. Effects of interleukin 17 on the cardiovascular system. Autoimmun Rev. 2017;16:984–91.
Ding H-S, Yang J, Yang J, Ding J-W, Chen P, Zhu P. Interleukin-17 contributes to cardiovascular diseases. Mol Biol Rep. 2012;39:7473–8.
Li Q, Wang Y, Chen K, Zhou Q, Wei W, Wang Y, et al. The role of oxidized low-density lipoprotein in breaking peripheral Th17/Treg balance in patients with acute coronary syndrome. Biochem Biophys Res Commun. 2010;394:836–42.
Giera M, Lingeman H, Niessen WMA. Recent advancements in the LC- and GC-based analysis of malondialdehyde (MDA): a brief overview. Chromatographia. 2012;75:433–40.
Fedorova M, Bollineni RC, Hoffmann R. Protein carbonylation as a major hallmark of oxidative damage: update of analytical strategies. Mass Spectrom Rev. 2014;33:79–97.
Boligon AA. Technical evaluation of antioxidant activity. Med Chem [Internet]. 2014;4(7):517–522 [cited 2019 Aug 26]; Available from: https://www.omicsonline.org/open-access/technical-evaluation-of-antioxidant-activity-2161-0444.1000517.php?aid=28118.
Gaggini M, Sabatino L, Vassalle C. Conventional and innovative methods to assess oxidative stress biomarkers in the clinical cardiovascular setting. BioTech Future Sci. 2020;68:223–31.
Ok EJ, Kim K, Park SB. Association between serum uric acid and oxidative stress in Korean adults. Korean J Fam Med. 2018;39:295–9.
Jansen E, Ruskovska T. Serum biomarkers of (anti) oxidant status for epidemiological studies. Int J Mol Sci. 2015;16:27378–90.
Lairon D, Lopez-Miranda J, Williams C. Methodology for studying postprandial lipid metabolism. Eur J Clin Nutr. 2007;61:1145–61.
Combs GF, Trumbo PR, McKinley MC, Milner J, Studenski S, Kimura T, et al. Biomarkers in nutrition: new frontiers in research and application. Ann N Y Acad Sci. 2013;1278:1–10.
Acknowledgements
The authors thank the University of Wollongong and the School of Medicine for providing access to article databases.
Author information
Authors and Affiliations
Contributions
All authors were involved in the creation, analyses, writing and reviewing of the article. The study quality rating, data extraction and synthesis were conducted by V.A.R. and J.S.
Corresponding author
Ethics declarations
Conflict of Interest
The authors declare that there is no conflict of interest regarding the publication of this article.
Human and Animal Rights and Informed Consent
This study did not collect any personal, sensitive or confidential information. Accessible documents were used as evidence.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
do Rosario, V.A., Spencer, J., Weston-Green, K. et al. The Postprandial Effect of Anthocyanins on Cardiovascular Disease Risk Factors: a Systematic Literature Review of High-Fat Meal Challenge Studies. Curr Nutr Rep 9, 381–393 (2020). https://doi.org/10.1007/s13668-020-00328-y
Published:
Issue Date:
DOI: https://doi.org/10.1007/s13668-020-00328-y