Abstract
Although transdermal drug delivery would be very useful for the treatment of many diseases, in practice it is difficult to accomplish for the obstruction of the stratum corneum. The application of cold atmospheric plasma (CAP) as a pretreatment to the skin surface helps to enhance the delivery of topically applied drugs into the skin and the systemic circulation. CAP can change the skin properties to improve drug penetration by various different effects based on its multiple components. This review first introduces the skin barrier properties and some traditional transdermal drug delivery strategies. Next what is known about the application of CAP in transdermal drug delivery has been summarized, including the mechanisms and possible side effects. We believe that CAP could be developed as a non-invasive and efficient pretreatment to improve the transdermal permeation of drugs in clinical practice, although more research needs to be done to overcome the challenges.

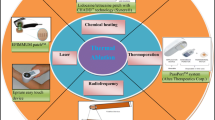
Graphical Abstract



Similar content being viewed by others
References
Lade S, Kosalge S, Shaikh S. Transdermal drug delivery system: a tool for novel drug delivery system: an overview. World Journal of Pharmaceutical Research. 2014;3(2):1892–908.
Singh D, Pradhan M, Nag M, Singh MR. Vesicular system: versatile carrier for transdermal delivery of bioactives. Artificial cells, nanomedicine, and biotechnology. 2015;43(4):282–90.
Sobanko JF, Miller CJ, Alster TS. Topical anesthetics for dermatologic procedures: a review. Dermatol Surg. 2012;38(5):709–21.
Eyerich S, Eyerich K, Traidl-Hoffmann C, Biedermann T. Cutaneous barriers and skin immunity: differentiating a connected network. Trends Immunol. 2018;39(4):315–27.
Zhou X, Hao Y, Yuan L, Pradhan S, Shrestha K, Pradhan O, et al. Nano-formulations for transdermal drug delivery: a review. Chin Chem Lett. 2018;29(12):1713–24.
Trommer H, Neubert RH. Overcoming the stratum corneum: the modulation of skin penetration. A review Skin Pharmacology and Physiology. 2006;19(2):106–21.
Marwah H, Garg T, Goyal AK, Rath G. Permeation enhancer strategies in transdermal drug delivery. Drug Delivery. 2014;23(2):564–78.
Benbow TV, Campbell J. Microemulsions as transdermal drug delivery systems for nonsteroidal anti-inflammatory drugs (NSAIDs): a literature review. Drug Dev Ind Pharm. 2019:1–16.
Ita KB. Prodrugs for transdermal drug delivery - trends and challenges. J Drug Target. 2016;24(8):671–8.
Schoellhammer CM, Blankschtein D, Langer R. Skin permeabilization for transdermal drug delivery: recent advances and future prospects. Expert opinion on drug delivery. 2014;11(3):393–407.
Banga AK, Bose S, Ghosh TK. Iontophoresis and electroporation: comparisons and contrasts. Int J Pharm. 1999;179(1):1–19.
Waghule T, Singhvi G, Dubey SK, Pandey MM, Gupta G, Singh M, et al. Microneedles: a smart approach and increasing potential for transdermal drug delivery system. Biomed Pharmacother. 2019;109:1249–58.
von Woedtke T, Metelmann HR, Weltmann KD. Clinical plasma medicine: state and perspectives of in vivo application of cold atmospheric plasma. Contributions to Plasma Physics. 2014;54(2):104–17.
Graves DB. Low temperature plasma biomedicine: a tutorial review. Physics of Plasmas. 2014;21(8):080901.
Weltmann KD, Kindel E, Brandenburg R, Meyer C, Bussiahn R, Wilke C, et al. Atmospheric pressure plasma jet for medical therapy: plasma parameters and risk estimation. Contributions to Plasma Physics. 2009;49(9):631–40.
Weltmann K, Von Woedtke T. Plasma medicine—current state of research and medical application. Plasma Physics and Controlled Fusion. 2016;59(1):014031.
Daeschlein G, Napp M, Lutze S, Arnold A, von Podewils S, Guembel D, et al. Skin and wound decontamination of multidrug-resistant bacteria by cold atmospheric plasma coagulation. JDDG: Journal der Deutschen Dermatologischen Gesellschaft. 2015;13(2):143–9.
Haertel B, Von Woedtke T, Weltmann K-D, et al. Non-thermal atmospheric-pressure plasma possible application in wound healing. Biomol Ther. 2014;22(6):477–90.
Zhong S, Dong Y, Liu D, et al. Surface air plasma-induced cell death and cytokine release of human keratinocytes in the context of psoriasis. Br J Dermatol. 2016;174(3):542–52.
Bekeschus S, Rödder K, Fregin B, et al. Toxicity and immunogenicity in murine melanoma following exposure to physical plasma-derived oxidants. Oxidative Med Cell Longev. 2017;2017:4396467.
Kalghatgi S, Tsai C, Gray R, et al. Transdermal drug delivery using cold plasmas. 22nd International Symposium on Plasma Chemistry 2015:5–10.
Shimizu K, Hayashida K, Blajan M. Novel method to improve transdermal drug delivery by atmospheric microplasma irradiation. Biointerphases. 2015;10(2):029517.
Gan L, Zhang S, Poorun D, Liu D, Lu X, He M, et al. Medical applications of nonthermal atmospheric pressure plasma in dermatology. JDDG: Journal der Deutschen Dermatologischen Gesellschaft. 2018;16(1):7–13.
Kalghatgi S, Juluri A. Louis JS, et al. Google Patents: Methods and systems for trans-tissue substance delivery using plasmaporation; 2017.
Kristof J, Miyamoto H, Tran AN, et al. Feasibility of transdermal delivery of cyclosporine A using plasma discharges. Biointerphases. 2017;12(2):02B402.
Shimizu K, Tran AN, Kristof J, et al. Investigation of atmospheric microplasma for improving skin permeability. Proceedings of the 2016 Electrostatics joint conference, Lafayette 2016:13–18.
Bos JD, Meinardi MM. The 500 Dalton rule for the skin penetration of chemical compounds and drugs. Exp Dermatol. 2000;9(3):165–9.
Fluhr JW, Sassning S, Lademann O, Darvin ME, Schanzer S, Kramer A, et al. In vivo skin treatment with tissue-tolerable plasma influences skin physiology and antioxidant profile in human stratum corneum. Exp Dermatol. 2012;21(2):130–4.
Machado M, Salgado TM, Hadgraft J, Lane ME. The relationship between transepidermal water loss and skin permeability. Int J Pharm. 2010;384(1–2):73–7.
Stoffels E, Sakiyama Y, Graves DB. Cold atmospheric plasma: charged species and their interactions with cells and tissues. IEEE Transactions on Plasma Science. 2008;36(4):1441–57.
Tian W, Kushner MJ. Atmospheric pressure dielectric barrier discharges interacting with liquid covered tissue. J Phys D Appl Phys. 2014;47(16):165201.
Van der Paal J, Aernouts S, van Duin ACT, et al. Interaction of O and OH radicals with a simple model system for lipids in the skin barrier: a reactive molecular dynamics investigation for plasma medicine. J Phys D Appl Phys. 2013;46(39):395201.
Marschewski M, Hirschberg J, Omairi T, Höfft O, Viöl W, Emmert S, et al. Electron spectroscopic analysis of the human lipid skin barrier: cold atmospheric plasma-induced changes in lipid composition. Exp Dermatol. 2012;21(12):921–5.
Suda Y, Tero R, Yamashita R, et al. Reduction in lateral lipid mobility of lipid bilayer membrane by atmospheric pressure plasma irradiation. Japanese Journal of Applied Physics. 2016;55(3S2):03DF05.
Choi JH, Nam SH, Song YS, Lee HW, Lee HJ, Song K, et al. Treatment with low-temperature atmospheric pressure plasma enhances cutaneous delivery of epidermal growth factor by regulating E-cadherin-mediated cell junctions. Arch Dermatol Res. 2014;306(7):635–43.
Lee HY, Choi JH, Hong JW, Kim GC, Lee HJ. Comparative study of the Ar and he atmospheric pressure plasmas on E-cadherin protein regulation for plasma-mediated transdermal drug delivery. J Phys D Appl Phys. 2018;51(21):215401.
Tunggal JA, Helfrich I, Schmitz A, Schwarz H, Günzel D, Fromm M, et al. E-cadherin is essential for in vivo epidermal barrier function by regulating tight junctions. EMBO J. 2005;24(6):1146–56.
Daeschlein G, Scholz S, Ahmed R, Majumdar A, von Woedtke T, Haase H, et al. Cold plasma is well-tolerated and does not disturb skin barrier or reduce skin moisture. JDDG: Journal der Deutschen Dermatologischen Gesellschaft. 2012;10(7):509–15.
Isbary G, Shimizu T, Zimmermann JL, Heinlin J, al-Zaabi S, Rechfeld M, et al. Randomized placebo-controlled clinical trial showed cold atmospheric argon plasma relieved acute pain and accelerated healing in herpes zoster. Clinical Plasma Medicine. 2014;2(2):50–5.
Shimizu K. Biological effects and enhancement of percutaneous absorption on skin by atmospheric microplasma irradiation. Plasma Medicine. 2015;5(2–4).
Lademann J, Richter H, Alborova A, et al. Risk assessment of the application of a plasma jet in dermatology. Journal of biomedical optics.14(5):054025.
Lademann O, Richter H, Patzelt A, Alborova A, Humme D, Weltmann KD, et al. Application of a plasma-jet for skin antisepsis: analysis of the thermal action of the plasma by laser scanning microscopy. Laser Phys Lett. 2010;7(6):458–62.
Roy S. Impact of UV radiation on genome stability and human health. Adv Exp Med Biol. 2017;996:207–19.
Ahmad SI, Christensen L, Baron E. History of UV lamps, types, and their applications. Adv Exp Med Biol. 2017;996:3–11.
Merle C, Laugel C, Baillet-Guffroy A. Effect of UVA or UVB irradiation on cutaneous lipids in films or in solution. Photochem Photobiol. 2010;86(3):553–62.
Funding
MRH was supported by US NIH Grants R01AI050875 and R21AI121700.
Author information
Authors and Affiliations
Corresponding authors
Ethics declarations
Conflict of interest
MRH declares the following potential conflicts of interest. Scientific Advisory Boards: Transdermal Cap Inc., Cleveland, OH; BeWell Global Inc., Wan Chai, Hong Kong; Hologenix Inc. Santa Monica, CA; LumiThera Inc., Poulsbo, WA; Vielight, Toronto, Canada; Bright Photomedicine, Sao Paulo, Brazil; Quantum Dynamics LLC, Cambridge, MA; Global Photon Inc., Bee Cave, TX; Medical Coherence, Boston MA; NeuroThera, Newark DE; JOOVV Inc., Minneapolis-St. Paul MN; AIRx Medical, Pleasanton CA; FIR Industries, Inc. Ramsey, NJ; UVLRx Therapeutics, Oldsmar, FL; Ultralux UV Inc., Lansing MI; Illumiheal & Petthera, Shoreline, WA; MB Lasertherapy, Houston, TX; ARRC LED, San Clemente, CA; Varuna Biomedical Corp. Incline Village, NV; Niraxx Light Therapeutics, Inc., Boston, MA. Consulting; Lexington Int, Boca Raton, FL; USHIO Corp, Japan; Merck KGaA, Darmstadt, Germany; Philips Electronics Nederland B.V. Eindhoven, Netherlands; Johnson & Johnson Inc., Philadelphia, PA; Sanofi-Aventis Deutschland GmbH, Frankfurt am Main, Germany. Stockholdings: Global Photon Inc., Bee Cave, TX; Mitonix, Newark, DE.
The other authors declare no conflicts of interest.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Xiang Wen and Yue Xin are co-first authors
Rights and permissions
About this article
Cite this article
Wen, X., Xin, Y., Hamblin, M.R. et al. Applications of cold atmospheric plasma for transdermal drug delivery: a review. Drug Deliv. and Transl. Res. 11, 741–747 (2021). https://doi.org/10.1007/s13346-020-00808-2
Published:
Issue Date:
DOI: https://doi.org/10.1007/s13346-020-00808-2