Abstract
Background
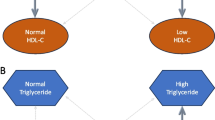
The clinical features of diabetic dyslipidemia are low levels of high-density lipo protein cholesterol (HDL-C) associated with hypertriglyceridemia. However, isolated low HDL-C, defined as low HDL-C in the absence of other lipid abnormalities, has not been well studied among patients with type 2 diabetes (T2DM).
Objective
We studied the prevalence of isolated low HDL-C and combined low HDL-C (i.e. low HDL-C combined with other lipid abnormalities) among patients with T2DM, compared clinical features, and studied the effect on coronary artery disease (CAD) risk for patients with the two types of low HDL-C.
Methods
The study population was 398 patients (238 men, 160 women) with T2DM. Their glucose, lipid metabolism, and atherosclerosis profiles were analyzed. The prevalence of CAD among those with low HDL-C was then studied for 173 male patients with T2DM.
Results
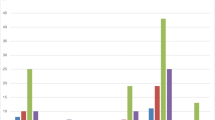
The prevalence of low HDL-C (HDL <40 mg/dL, for both sexes) was 33.7 % (n = 134); 12.6 % of the patients (n = 50) had isolated low HDL-C and 21.1 % (n = 84) had combined low HDL-C. Clinical indicators of diabetes and atherosclerosis were no different between patients with isolated or combined low HDL-C. Among the 173 male patients evaluated, it was re-confirmed that low HDL-C was an independent risk factor for CAD which did not depend on triglycerides and other risk factors. Risks for CAD were similar for men with isolated or combined low-HDL-C (34.1 vs. 32.4 %, respectively; no significant difference).
Conclusions
Although the prevalence of isolated low HDL-C in T2DM was the same as among the general population, it was clearly shown that prevalence of the combined type was higher. In limited analysis of male patients, CAD risk for both was shown to be equal. The risk associated with low HDL-C among the T2DM patients was assumed to be because of an increase in the combined type.




Similar content being viewed by others
Abbreviations
- LDL-C:
-
Low-density lipoprotein cholesterol
- CAD:
-
Coronary artery disease
- HDL-C:
-
High-density lipoprotein cholesterol
- TG:
-
Triglyceride
- UKPDS:
-
United Kingdom Prospective Diabetes Study
- T2DM:
-
Type 2 diabetes mellitus
- WHO:
-
World Health Organization
- JDCS:
-
Japan Diabetes Complications Study
- ABCA1:
-
ATP-binding cassette transporter A1
- JAS:
-
Japan Atherosclerosis Society
- TC:
-
Total cholesterol
- CAG:
-
Cardio-angiography
- SD:
-
Standard deviation
- ANOVA:
-
Analysis of variance
- BMI:
-
Body mass index
- CPR:
-
C-peptide immunoreactivity
- IRI:
-
Immunoreactive insulin
- IMT:
-
Intima media thickness
- H-CRP:
-
Highly sensitive C-reactive protein
- ABI:
-
Ankle brachial index
- PWV:
-
Pulse wave velocity
- HSL:
-
Hormone-sensitive lipase
- VLDL:
-
Very-low-density lipoprotein
- SREBP-1c:
-
Sterol regulatory element-binding protein 1c
- miRNA:
-
Micro ribonucleic acid
References
Baigent C, Keech A, Kearney PM, Blackwell L, Buck G, Pollicino C, Kirby A, Sourjina T, Peto R, Collins R, Simes R. Cholesterol treatment trialists’ (CTT) collaborators. Efficacy and safety of cholesterol-lowering treatment: prospective meta-analysis of data from 90,056 participants in 14 randomised trials of statins. Lancet. 2005;366:1267–78.
Jafri H, Alsheikh-Ali AA, Karas RH. Meta-analysis: statin therapy does not alter the association between low levels of high-density lipoprotein cholesterol and increased cardiovascular risk. Ann Intern Med. 2010;153:800–8.
Gordon T. Castelli WP, Hjortland MC, Kannel WB, and Dawber TR: high density lipoprotein as a protective factor against coronary heart disease. The Framingham Study. Am J Med. 1977;62:707–14.
Emerging Risk Factors Collaboration, Di Angelantonio E, Sarwar N, Perry P, Kaptoge S, Ray KK, Thompson A, Wood AM, Lewington S, Sattar N, Packard CJ, Collins R, Thompson SG, Danesh J. Major lipids, apolipoproteins, and risk of vascular disease. JAMA. 2009;302:1993–2000.
Khera AV, Cuchel M, de la Llera-Moya M, Rodrigues A, Burke MF, Jafri K, French BC, Phillips JA, Mucksavage ML, Wilensky RL, Mohler ER, Rothblat GH, Rader DJ. Cholesterol efflux capacity, high-density lipoprotein function, and atherosclerosis. N Engl J Med. 2011;364:127–35.
Mahdy AK, Wonnerth A, Huber K, Wojta J. Cardiovascular disease risk reduction by raising HDL cholesterol-current therapies and future opportunities. Br J Pharmacol. 2012;167:1177–94.
Taskinen MR. Diabetic dyslipidaemia: from basic research to clinical practice. Diabetologia. 2003;46:733–49.
Mooradian AD. Dyslipidemia in type 2 diabetes mellitus. Nat Clin Prac Endocrinol Metabol. 2009;5:150–9.
Turner RC, Millns H, Neil HA, Stratton IM, Manley SE, Matthews DR, Holman RR. Risk factors for coronary artery disease in non-insulin dependent diabetes mellitus: United Kingdom Prospective Diabetes Study (UKPDS: 23). BMJ. 1998;316:823–8.
Fredrichson DS, Lees RS. A system for phenotyping hyperlipoproteinemia. Circulation. 1965;131:321–7.
Sone H, Yamada N. Complications of diabetes mellitus. In: Clinical epidemiologic investigation and international comparison about diabetes and its complications in Japan Diabetes Complications Study (JDCS) vol.19(2); 2005. pp 114–22,
Miller M. Differentiating the effects of raising low levels of high-density lipoprotein cholesterol versus lowering normal triglycerides: further insights from the veterans affairs high-density lipoprotein intervention trial. Am J Cardiol. 2000;21(86):23L–7L.
Yokoyama S. ABCA1 and biogenesis of HDL. J Atheroscler Thromb. 2006;13:1–15.
Fitzgerald ML, Mujawar Z, Tamehiro N. ABC transporters, atherosclerosis and inflammation. Atherosclerosis. 2010;211:361–70.
Guideline for Diagnosis and Prevention of Atherosclerotic Cardiovascular Diseases in Japan, 2012 Version.
Huxley RR, Barzi F, Lam TH, Czernichow S, Fang X, Welborn T, Shaw J, Ueshima H, Zimmet P, Jee SH, Patel JV, Caterson I, Perkovic V, Woodward M. Asia Pacific cohort studies collaboration and the obesity in Asia collaboration: isolated low levels of high-density lipoprotein cholesterol are associated with an increased risk of coronary heart disease: an individual participant data meta-analysis of 23 studies in the Asia-Pacific region. Circulation. 2011;124:2056–64.
Zhang J, Hupfeld CJ, Taylor SS, Olefsky JM, Tsien RY. Insulin disrupts beta-adrenergic signalling to protein kinase A in adipocytes. Nature. 2005;437:569–73.
Lamarche B, Uffelman KD, Carpentier A, Cohn JS, Steiner G, Barrett PH, Lewis GF. Triglyceride enrichment of HDL enhances in vivo metabolic clearance of HDL apo A-I in healthy men. J Clin Invest. 1999;103:1191–9.
Horie T, Ono K, Horiguchi M, Nishi H, Nakamura T, Nagao K, Kinoshita M, Kuwabara Y, Marusawa H, Iwanaga Y, Hasegawa K, Yokode M, Kimura T, Kita T. MicroRNA-33 encoded by an intron of sterol regulatory element-binding protein 2 (Srebp2) regulates HDL in vivo. Proc Natl Acad Sci USA. 2010;107:17321–6.
Mauldin JP, Nagelin MH, Wojcik AJ, Srinivasan S, Skaflen MD, Ayers CR, McNamara CA, Hedrick CC. Reduced expression of ATP-binding cassette transporter G1 increases cholesterol accumulation in macrophages of patients with type 2 diabetes mellitus. Circulation. 2008;117:2785–92.
Mauldin JP, Srinivasan S, Mulya A, Gebre A, Parks JS, Daugherty A, Hedrick CC. Reduction in ABCG1 in Type 2 diabetic mice increases macrophage foam cell formation. J Biol Chem. 2006;281:21216–24.
Boes E, Coassin S, Kollerits B, Heid IM, Kronenberg F. Genetic-epidemiological evidence on genes associated with HDL cholesterol levels: a systematic in-depth review. Exp Gerontol. 2009;44:136–60.
Martin LJ, Woo JG, Daniels SR, Goodman E, Dolan LM. The relationships of adiponectin with insulin and lipids are strengthened with increasing adiposity. J Clin Endocrinol Metab. 2005;90:4255–9.
Verges B, Petit JM, Duvillard L, Dautin G, Florentin E, Galland F, Gambert P. Adiponectin is an important determinant of apoA-I catabolism. Arterioscler Thromb Vasc Biol. 2006;26:1364–9.
Schneider JG, von Eynatten M, Schiekofer S, Nawroth PP, Dugi KA. Low plasma adiponectin levels are associated with increased hepatic lipase activity in vivo. Diabetes Care. 2005;28:2181–6.
Nogueira JP, Maraninchi M, Béliard S, Lorec AM, Berthet B, Bégu-Le Corroller A, Dubois N, Grangeot R, Mattei C, Gaudart J, Nicolay A, Portugal H, Vialettes B, Valéro R. Unacylated Ghrelin is associated with the isolated low HDL-cholesterol obese phenotype independently of insulin resistance and CRP level. Nutr Metab Lond. 2012;9:17.
Beaumont NJ, Skinner VO, Tan TM, Ramesh BS, Byrne DJ, MacColl GS, Keen JN, Bouloux PM, Mikhailidis DP, Bruckdorfer KR, Vanderpump MP, Srai KS. Ghrelin can bind to a species of high density lipoprotein associated with paraoxonase. J Biol Chem. 2003;278:8877–80.
Idei M, Hirayama S, Miyake N, Kon M, Horiuchi Y, Ueno T, Miyake K, Satoh N, Yoshii H, Yamashiro K, Onuma T, Miida T. Mean postprandial triglyceride concentration is an independent risk factor for carotid atherosclerosis in patients with type 2 diabetes. Clin Chim Acta. 2014;430:134–9.
Conflict of interest
All authors, Matsumura K, Kimura Y, Hiroshi Murakami-1 H, Yamashita M, Matsuk i K, Tanabe J, Murakami-2 H, Matsui J, Tamasawa N, and Daimon M, declare that they have no conflict of interest.
Human rights statement and informed consent
All procedures followed were in accordance with the ethical standards of the responsible committee on human experimentation (Hirosaki University Graduate School of Medicine) and with the Helsinki Declaration of 1964 and later revision.
Author information
Authors and Affiliations
Corresponding author
About this article
Cite this article
Matsumura, K., Kimura, Y., Murakami, H. et al. Isolated low-HDL cholesterol in Japanese patients with type 2 diabetes. Diabetol Int 6, 290–299 (2015). https://doi.org/10.1007/s13340-014-0200-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s13340-014-0200-0