Abstract
The WHO has declared COVID-19 illness a global health concern which is caused by 2019-nCoV, causing severe respiratory tract infections in humans. Transmissibility among individual to individual have been reported through droplets and probably also via contaminated surfaces and hands. Human coronaviruses can persist on inanimate surfaces such as plastic, glass, fibers and metals up to nine days. 2019-nCoV remains infectious in air for 3 h and on inanimate surfaces such as cardboard, copper, plastic and steel up to 24, 4, 72 and 48 h respectively. Disinfectant activity of various biocidal agents against coronaviruses like ethanol (62–71%), sodium hypochlorite (0.1%) and hydrogen peroxide (0.5%) can be regarded effective against 2019-nCoV as well. As no vaccine and antiviral therapies have been discovered for 2019-nCoV, prevention of further spread will viable option to control the ongoing and future outbreaks.
Similar content being viewed by others
Introduction
Earliest case of novel coronavirus 2019-nCoV detected on 17 November 2019 from Wuhan China, has killed over 25,000 people and infected more than 500,000 globally as of March 28, 2020 (WHO, 2020). It has been spread to at least 202 countries and territories [1]. United States is now on the top with 107,463 confirmed cases followed by Italy and Spain as of March 28, 2020 (www.covidvisualizer.com). Research has explained person to person transmission both in hospital and family settings [2]. Some reports have described by local news channels and WHO. In Italy, at least 2,629 health workers have been infected by coronavirus since the onset of the outbreak in February 2020, representing 8.3 percent of total cases. In Pakistan, earliest case was reported in a group of people who travelled to Iran for visit purposes. Soon after this, virus transmitted to other people and healthcare professionals with great speed. In Thailand, a taxi driver was detected positive with COVID 19 who had no travel history to china [2]. Common signs and symptoms of infection include fever, coughing and labored breathing. In severe cases, it can cause pneumonia, multiple organ failure and death [3]. The incubation period of COVID-19 is thought to be between 1 and 14 days [4]. It is contagious before symptoms appear, which is why so many people get infected. Infected patients can be also asymptomatic, meaning they do not display any symptoms despite having the virus in their systems. It is therefore, dire need of time to prevent or slow down the spread of this virus among public and healthcare settings.
Survivability of coronaviruses on inanimate surfaces
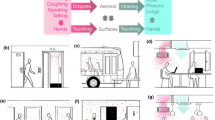
Contamination of dry surfaces could be serve as transmission route of coronaviruses. Moreover, it is proposed that viruses can be transmitted through self-inoculation of mucous membranes of nose, eyes and mouth [5, 6]. Not many scientific studies have conducted to examine the survivability of 2019-nCoV on various surfaces and seasons, because it was discovered so recently. Most data will be taken from endemic human corona virus strain (HCoV-229E). Some studies reported that it can survive on metals, glass, plastic and fibers for as long as 9 days. Some veterinary coronaviruses can even hang around for up to 28 days in low temperatures. 2019-nCoV causes COVID-19 can live in the air and on surfaces between several hours and several days. 2019-nCoV is viable for up to 72 h on plastics, 48 h on stainless steel and 24 h on cardboard. Copper surfaces tend to kill the virus in about 4 h. Research further revealed that the virus could survive in droplets for up to 3 h after being coughed out into the air [7]. Furthermore, governments worldwide are quarantining bank notes, as the coronavirus pandemic puts the spotlight on the germ-spreading properties of ‘real’ money. The US, South Korea and China have all been taking action amid concerns that the disease could be spread by paper money and coins. In addition, HCoV-229E strain persists better at 50% relative humidity at room temperature [8] (Table 1).
Inactivation of coronaviruses by disinfectant agents in suspension and carrier tests
Use of 78–95% Ethanol, 70–100% iso-propanol, 0.5–2.5% glutaraldehyde, 0.7–1.0% formaldehyde, and 0.23–7.5% povidone iodine either individually or simultaneously inactivates coronaviruses infectivity in suspension tests. Other disinfectants such as 0.21% Sodium hypochlorite, 0.5% Hydrogen peroxide, and 0.05% Benzalkonium could also kill coronaviruses effectively on recommended concentrations illustrated in Table 2 [9].
In carrier tests, ethanol (62–71%), Sodium hypochlorite (0.1–0.5%), Glutardialdehyde (2.0%), Glutardialdehyde (0.04%) and Sodium hypochlorite (0.06%) proved effective against coronaviruses presented in Table 3 [9].
Concluding remarks
Human coronaviruses remain infectious on dry surfaces for 2–9 days at room temperature. Duration can be shorter at a temperature of 30 °C or more. Unlike of human, veterinary coronaviruses persists even longer for 28 days. Contamination of frequent use surfaces in healthcare and home settings are potential source of viral transmission. Transmission of coronaviruses from contaminated surfaces was not supported with research but it could be observed in case of Influenza A and Parainfluenza virus 3 cases, as 31.6% and 1.5% viral load can transfer to hands in 5 and 3 s respectively [10, 11]. During outbreak situations, viral load of SARC COV-2 is not known on frequent touch surfaces, it seems plausible to disinfect them to reduce the chances of disease incidence. The WHO recommends thoroughly cleaning of surfaces with water, detergent and commonly used disinfectants are effective to clean the environment [12]. The dilution of 1:100 of 5% bleach (sodium hypochlorite) seems appropriate to recommend in the coronavirus setting. 70% concertation of ethanol could be effective for the disinfestation of small surfaces for coronavirus [13]. The WHO recommends alcohol-based hand rubs for the decontamination of hands, e.g. after removing gloves. Formulations based on 80% ethanol or 75% 2-propanol proved very effective against SARS-CoV and MERS-CoV and recommended by WHO [14]. No study has reported in-vitro efficacy of hand washing against coronavirus contaminations on hands. However, in Taiwan, installation of hand wash stations in the healthcare settings protected the healthcare professionals from acquiring the SARS-COV infection, indicating that hand hygiene can have protective effects [15]. Furthermore, virus is highly sensitive to high temperature and it is hypnotized that it could significantly change COVID-19 transmission. 2019-nCoV can survive in air for 3 h and on inanimate objects for more than 72 h. Disinfection of frequent touch surfaces with 62–71% ethanol, 0.1% sodium hypochlorite, 0.5% hydrogen peroxide can be considered effective against 2019-nCoV as other coronaviruses become ineffective with 1 min exposure time.
References
WHO. Coronavirus Disease 2019 (COVID-19). 2020; Situation Report 67.
Chan JF-W, Yuan S, Kok K-H, To KK-W, Chu H, Yang J, et al. A familial cluster of pneumonia associated with the 2019 novel coronavirus indicating person-to-person transmission: a study of a family cluster. Lancet. 2020;395:514–23.
Zhang J, Dong X, Cao Y, Yuan Y, Yang Y, Yan Y, et al. Clinical characteristics of 140 patients infected with SARS-CoV-2 in Wuhan, China. Allergy. 2020. https://doi.org/10.1111/all.14238.
Hoehl S, Rabenau H, Berger A, Kortenbusch M, Cinatl J, Bojkova D, et al. Evidence of SARS-CoV-2 infection in returning travelers from Wuhan, China. N Engl J Med. 2020;382:1278–80.
Otter JA, Donskey C, Yezli S, Douthwaite S, Goldenberg SD, Weber DJ. Transmission of SARS and MERS coronaviruses and influenza virus in healthcare settings: the possible role of dry surface contamination. J Hosp Infect. 2016;92:235–50.
Dowell SF, Simmerman JM, Erdman DD, Wu J-SJ, Chaovavanich A, Javadi M, et al. Severe acute respiratory syndrome coronavirus on hospital surfaces. Clin Infect Dis. 2004;39:652–7.
van Doremalen N, Bushmaker T, Morris DH, Holbrook MG, Gamble A, Williamson BN, et al. Aerosol and surface stability of SARS-CoV-2 as compared with SARS-CoV-1. N Engl J Med. 2020;382:1564–7.
Ijaz MK, Brunner AH, Sattar SA, Nair RC, Johnson-Lussenburg CM. Survival characteristics of airborne human coronavirus 229E. J Gen Virol. 1985;66:2743–8.
Kampf G, Todt D, Pfaender S, Steinmann E. Persistence of coronaviruses on inanimate surfaces and its inactivation with biocidal agents. J Hosp Infect. 2020;104:246–51.
Ansari SA, Springthorpe VS, Sattar SA, Rivard S, Rahman M, et al. Potential role of hands in the spread of respiratory viral infections: studies with human parainfluenza virus 3 and rhinovirus 14. J Clin Microbiol. 1991;29:2115–9.
Bean B, Moore BM, Sterner B, Peterson LR, Gerding DN, Balfour HH Jr. Survival of influenza viruses on environmental surfaces. J Infect Dis. 1982;146:47–51.
WHO. Infection prevention and control during health care when novel coronavirus (nCoV) infection is suspected. WHO; 2020. Interim guidance. 25 January 2020.
WHO. Annex G. Use of disinfectants: alcohol and bleach. Infection prevention and control of epidemic-and pandemic-prone acute respiratory infections in health care. Geneva: WHO; 2014. p. 65e6.
Siddharta A, Pfaender S, Vielle NJ, Dijkman R, Friesland M, Becker B, et al. Virucidal activity of World Health Organization–recommended formulations against enveloped viruses, including zika, ebola, and emerging coronaviruses. J Infect Dis. 2017;215:902–6.
Yen M-Y, Lu Y-C, Huang P-H, Chen C-M, Chen Y-C, Lin YE. Quantitative evaluation of infection control models in the prevention of nosocomial transmission of SARS virus to healthcare workers: implication to nosocomial viral infection control for healthcare workers. Scand J Infect Dis. 2010;42:510–5.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The author declares that there is no conflict of interest.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Akram, M.Z. Inanimate surfaces as potential source of 2019-nCoV spread and their disinfection with biocidal agents. VirusDis. 31, 94–96 (2020). https://doi.org/10.1007/s13337-020-00603-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s13337-020-00603-0