Abstract
Multiple sclerosis (MS) is an autoimmune demyelinating disorder of the central nervous system. Only a few biomarkers are available in MS clinical practice, such as cerebrospinal fluid oligoclonal bands and immunoglobulin index, serum anti-aquaporin 4 antibodies, and serum anti-John Cunningham virus antibodies. Thus, there is a significant unmet need for biomarkers to assess prognosis, response to therapy, or potential treatment complications. Here we describe emerging biomarkers that are in development, focusing on those from peripheral blood. There are several limitations in the process of discovery and validation of a good biomarker, such as the pathophysiological complexity of MS and the technical difficulties in globally standardizing methods for sampling, processing, and conserving biological specimens. In spite of these limitations, ongoing international collaborations allow the exploration of many interesting molecules and markers to validate diagnostic, prognostic, and therapeutic-response biomarkers.
Similar content being viewed by others
Introduction
Inflammatory neurologic diseases encompass infectious, postinfectious, autoimmune, and vasculitic diseases. Even neurodegenerative neurologic diseases such as Alzheimer’s disease, Parkinson’s disease, and amyotrophic lateral sclerosis have an inflammatory component. For the purpose of this review, we will focus on multiple sclerosis (MS), an autoimmune demyelinating disorder of the central nervous system (CNS). Clinically, the MS course may be relapsing-remitting (RRMS) or progressive and is called secondary progressive (SPMS) when it follows a RRMS onset, or primary progressive MS (PPMS) when it is progressive from onset [1]. The earliest clinical stage of the disease is detectable after a single episode of neurological dysfunction [clinically isolated syndrome (CIS)]. MS is considered a predominantly T-cell-mediated autoimmune disorder, although B cells have an important contribution in disease pathogenesis [2]. Myelin-specific CD4+ T-helper (Th) cells type 1 and Th17 cells, as well as CD8+ T cells enter the CNS where they encounter their cognate ligand and initiate an immune response leading to recruitment of other cells B cells, macrophages, and natural killer cells [3–5], resulting in tissue damage and neurologic dysfunction [6]. Alterations in apoptosis of autoreactive immune cells have also been described, leading to persistence of these proinflammatory cells [7, 8]. Pathologically, inflammation, demyelination, and axonal loss are observed [9–11], and although MS is classically described as a white matter disease, the gray matter is significantly involved [12–14]. Biomarkers may be used to support the diagnosis, and identify potential converters from CIS to MS so treatment could be initiated early. As more effective but potentially more toxic therapies become available we need biomarkers that predict disease severity and response to treatment so we can select the appropriate therapy. We also need biomarkers for predicting risk of adverse events.
There are some biomarkers already in clinical use for MS; cerebrospinal fluid (CSF) oligoclonal bands and immunoglobulin production have been in use for many years to support the diagnosis and may help predict conversion of CIS to MS [15]. Levels of anti-aquaporin 4 antibodies in the serum are used to differentiate MS from neuromyelitis optica (NMO) [16], while serum anti-John Cunningham virus (JCV) antibodies are useful in risk stratification during natalizumab therapy [17].
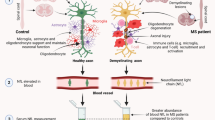
The pathophysiology of MS involves 3 principal compartments: 1) the peripheral blood, where immune processes are initiated in the relapsing-remitting phase; 2) the blood–brain barrier (BBB), which becomes overpermeable to autoreactive immune cells entering the CNS; 3) the CNS, where acute lesions indicate sites of inflammation and neural damage, leading to the manifestation of symptoms and disability. These compartments can be evaluated via blood tests, CSF studies, CNS imaging, and sampling of tissue through biopsies. Peripheral blood sampling and neuroimaging techniques are the most feasible and innocuous methods for repeated testing in MS, but the latter lack pathological specificity and are relatively expensive.
In this review we will focus on emerging blood biomarkers that have shown reproducible results and may be closer to clinical implementation (Table 1). We included emerging blood biomarkers validated in 2 independent cohorts of patients, or recent data on known biomarkers proposed to answer different clinical questions. For biomarkers to become clinically applicable they have to go through discovery, verification, clinical validation, then multicenter validation before being available for implementation. Proximity to clinical application was assessed based on the completion phase of this process. Given the significant heterogeneity in the research on blood biomarkers, and the fact that many validation studies investigated simultaneously blood and CSF concentrations of the same biomarkers, some data CSF biomarker data are considered as worth mentioning.
Description of an “Ideal” Biomarker
A biomarker is “a characteristic that is objectively measured and evaluated as an indicator of normal biologic or pathogenic processes, or pharmacological responses to a therapeutic intervention” [18, 19]. An ideal biomarker should be precise, reliable, and differ between healthy controls and patients with MS. It should be easily studied in a body fluid that is practical to obtain and measurable with affordable laboratory procedures. It should be involved in the disease pathogenesis, and correlate with clinical disease activity and disability progression. Ideally, it should have a high sensitivity in detecting relevant disease activity, conserving a high specificity as well. It is even better if it correlates with radiologic disease activity markers, such as magnetic resonance imaging (MRI) findings. In the case of a biomarker of inflammation, it should undergo rapid normalization under therapy in responders but no normalization under therapy in nonresponders.
Many of these characteristics of an ideal biomarker depend on the relationship between the pathogenesis of MS and the biological sample tested. The majority of MS lesions are usually located in the periventricular white matter of the brain and superficial regions of the spinal cord, being anatomically close to the CSF space [20]. Because brain biopsies are typically not feasible in these cases, CSF is used for measurements of soluble markers and cell populations by flow cytometry analysis, polymerase chain reaction studies, and cell functional analyses. However, CSF collection is relatively invasive, being usually collected during the diagnostic phase of MS [19].
Biomarkers measurable in the peripheral blood through noninvasive methods are of significant clinical importance in MS. The main drawback is that much of the disease pathology occurs in the CNS, which is separated from the periphery by the BBB. Therefore, events associated with CNS lesions may not be easily detectable in peripheral blood. Furthermore, there might be significant variations in many of the soluble markers, owing to circadian fluctuations, systemic infections, degradation in the liver, or excretion through the kidney. However, blood biomarkers provide information about immune triggers in MS and some of the effects of disease-modifying drugs [19–21]. Notably, the majority of protein content of the CSF is blood-derived, while the rest is derived from the brain or produced intrathecally [20].
Biomarkers to Support the Diagnosis of MS and MS Subtypes
The diagnosis of RRMS requires evidence of dissemination in time and space, as well as absence of any other explanation of the clinical findings (usually called MS mimickers). In this respect there have been significant advances in the diagnostic criteria merging clinical and radiologic features to diagnose confidently RRMS [1, 22]. However, progressive forms of MS could be difficult to diagnose early on, and having a good biomarker to support the diagnosis would be very useful.
Epidermal and Hepatocyte Growth Factors, CCL4, and CCL11
Tejera et al. [23] analyzed a set of 30 different plasma cytokines, chemokines, and growth factors in blood of 129 patients with MS with different clinical forms (RRMS, SPMS, and PPMS) and 53 healthy controls, across 2 independent cohorts, using Luminex xMAP technology. They showed that different MS forms are associated with distinct profiles of circulating plasma protein biomarkers, with distinct signatures being composed of chemokines and growth/angiogenic factors, and proposed the evaluation of a set of 4 circulating biomarkers (hepatocyte growth factor, eotaxin/CCL11, epidermal growth factor, and macrophage inflammatory protein-1β/CCL4) as a tool in the diagnosis and more personalized therapeutic targeting of patients with MS [23].
Noncoding microRNAs
In another recent study 3 microRNAs (miRNAs) were differentially expressed in the serum of patients with RRMS compared with patients with PPMS, and were validated in 2 other independent small cohorts within the study, and were useful to differentiate RRMS from PPMS [24]. Notably miR-223 has been implicated in the regulation of CNS inflammasomes [25], and miR-15b has been described as a promoter for neurogenesis [26].
Other noncoding miRNAs in peripheral blood, such as miR-20a-5p [27, 28] and miR-22-5p [28, 29], which are involved in T-cell regulation, could be promising novel biomarkers to identify CIS converters and support early MS diagnosis. However, further replication in larger cohorts is still needed.
Anti-myelin Oligodendrocyte Antibodies
Anti-myelin oligodendrocyte (MOG) antibodies have been studied as an early predictor of the subsequent course of demyelination in children, showing that its presence is suggestive of acute disseminated encephalomyelitis rather than MS in the pediatric population (using a serum dilution of 1:160 as a cut-off for positivity) [30]. However, the usefulness of anti-MOG antibodies in the adult population is not as clear. In a study of adults with NMO and suspected limited forms of MS (optic neuritis and myelitis), MOG antibody titers through full-length MOG cell-based assay could not help in differentiating between the different clinical phenotypes, including monophasic and relapsing diseases. Furthermore, low MOG antibody titers were not always associated with a monophasic course or better outcome, and persistence of antibodies for several years was reported in patients with clinical symptom resurgence [31]. Moreover, the presence of MOG IgG in the serum of patients with NMO has been described, with inconsistent data regarding the coexistence of aquaporin 4 IgG and MOG IgG in these patients. As MOG IgG has been consistently absent in MS, it still can be a promising biomarker to help in differentiating between MS and aquaporin 4 IgG-negative NMO, which is a common clinical scenario [32–34].
Antigen Array Signatures
Quintana et al. [35] studied IgG antigen arrays signatures based on low-affinity autoantibody patterns. Informative patterns emerged from autoantibodies that bound peptides of myelin molecules and heat shock proteins, proteins and lipids that were detectable at 1:10, but not at higher dilutions (low affinity). They showed that SPMS samples have an immune reactivity closer to that observed in patients with PPMS. Later they also showed a significantly higher number of antibodies in pediatric MS compared with other neurologic disorders, attributing this to the phenomenon of epitope spreading [36]. In the same study they evaluated the performance of IgG antigen array reactivity classifiers in discriminating a monophasic acute demyelinating episode from MS at the time of an acute demyelinating attack, with an area under the curve of 0.872 [36]. The use of antigen arrays has not yet been replicated and has not shown usefulness in early diagnosis.
Neurofilaments and Other Neurodegenerative Biomarkers
Neurodegenerative biomarkers usually consist of neuron-specific proteins released following axonal damage. Several studies have shown elevated CSF levels of neurofilaments in MS [37–39]. In CIS, serum and CSF levels of neurofilament light subunit (NfL) were not associated with fast conversion to clinically definite MS (CDMS), but were significantly higher in CIS compared with healthy controls [40]. The axonal Tau protein was found to be upregulated in patients with RRMS and those with PPMS [41–46]. Furthermore, CSF levels of Tau tended to be highest in the early stage of the disease [43, 47]. However, these markers are not specific to MS as they are upregulated in many other degenerative, ischemic, and infectious CNS disorders.
Anti-KIR4.1 Channel Antibodies
Some authors have reported a high prevalence of antibodies directed against the glial inwardly rectifying potassium channel KIR4.1 (anti-KIR4.1) in serum of adults with MS and almost 50 % of children with MS [48, 49]. However, 2 other studies using a comparable enzyme-linked immunosorbent assay technique could not reproduce these findings [50, 51]. Levels of anti-KIR4.1 antibodies could not differentiate between MS and NMO, although higher levels of these antibodies were found in patients with MS during relapses [52]. Thus, more studies are needed to validate anti-KIR4.1 antibody levels as a biomarker in MS.
Serum 24-Hydroxycholesterol
There is recent interest in 24-hydroxycholesterol as a biomarker of MS, as modestly decreased levels of this lipid in serum have been reported in MS—more so in patients with PPMS and older patients with RRMS than in healthy controls [53–55], but further replication studies are needed.
Biomarkers to Predict the Conversion from CIS to Definite MS
Serum Anti-MOG and Antimyelin Basic Protein Antibodies
There is general agreement that early initiation of treatment after CIS could delay conversion to definite MS and mitigate future disability, so biomarkers that allow identification of patients at the highest and lowest risk of further attacks and disability are needed to personalize the treatment plan. In an initial study, Berger et al. [56] showed that the presence of serum IgM anti-MOG and anti-myelin basic protein antibodies could predict the risk of conversion from CIS to clinically definite MS. However, further investigations revealed that anti-MOG antibodies were only detectable in cases of acute disseminated encephalomyelitis [30, 57].
Chitinase 3-Like-1 and Chitinase 3-Like-2 Proteins
Chitinase 3-like-1 (CHI3L1) is a member of the family of chitinases and chitinase-like proteins containing a highly conserved glyco-18 domain as common feature. For these proteins, chitin is the only documented substrate. CHI3L1 can bind chitin but lacks chitinolytic activity. In the CNS, CHI3L1 expression has been mainly observed in astrocytes of monkeys and humans with lentiviral encephalitis, and patients with brain infarcts. Increased circulating levels of CHI3L1 have been reported in a wide variety of heterogeneous conditions characterized by chronic inflammation such as rheumatoid arthritis, inflammatory bowel disease, systemic lupus erythematous, asthma, and sarcoidosis; nonetheless, its mechanism of action remains poorly understood, beyond a suggestion that CHI3L1 may be a tissue remodeling factor. In patients with CIS, increased CSF CHI3L1 levels was a risk factor for conversion to definite MS, independent of strong predictors of conversion to MS such as brain MRI abnormalities and the presence of IgG oligoclonal bands [58]. Furthermore, patients with CIS with high CSF CHI3L1 had a shorter time to definite MS [58]. Interestingly, patients with CIS with higher serum levels of CHI3L1 and chitinase 3-like-1 (CHI3L2) have a higher conversion rate to definite MS, and converted much faster as well [59].
Chemokines and Their Receptors: C-X-C Motif Ligand 13
Chemokines and their receptors play an important role in the recruitment of autoreactive immune cells from the periphery to the CNS and are detectable in MS plaques [60]. Among these molecules, chemokine (C-X-C motif) ligand (CXCL)13 was found to be upregulated in patients with active MS. Furthermore, elevated levels of CXCL13 also predict CIS conversion to clinically definite MS [61–65].
25-OH Vitamin D
Among several studies that suggested a relationship between vitamin D deficiency and risk of MS, a group studying 100 patients with CIS showed that those with very low (below the tenth percentile) and low (below the twenty-fifth percentile) 25-hydroxy (OH) vitamin D levels in serum were at higher risk of conversion to definite MS after a median follow-up of 7.7 years [66].
A large multicenter study of > 1000 CIS cases, with a median follow up of 4.3 years, showed that lower 25-OH vitamin D levels in serum were associated with conversion to definite MS in a univariate analysis, but this association was mitigated at the multivariate level when controlling for the presence of oligoclonal bands in the CSF, number of T2 lesions on MRI, and age [15].
Biomarkers of Disease Activity
Serum Apoptotic Molecules and Cytokines
In a study to identify biomarkers of disease activity and progression in MS, Hagman et al. [67] analyzed the serum profiles of cytokines, chemokines, and apoptotic molecules in CIS, RRMS, PPMS, SPMS, and healthy controls (72 patients with MS, 17 with CIS, and 21 healthy controls). They correlated their levels with clinical and MRI findings acquired over a 1-year follow-up. They found increased levels of the apoptotic serum Fas (sFas) molecule in patients with MS with worsening Expanded Disability Status Scale (EDSS) score and accumulation of hypointense lesions on MRI. In these patients, the levels of macrophage migration-inhibitory factor were higher than in clinically stable patients. The authors suggested that sFas and migration-inhibitory factor can be candidate biomarkers of disability progression due to neurodegeneration. They also found that increased levels of serum tumor necrosis factor (TNF)-α and CCL2 seemed to reflect MS-related inflammatory responses, especially in PPMS, but stated that their role as biomarkers of clinical disease activity needs to be evaluated in a long-term study involving a larger cohort [67].
Neurofilaments and Anti-neurofilament Antibodies
Neurofilaments are important axonal cytoskeletal proteins where the 68-kDa NfL forms the core of the neurofilament, while the 190- to 210-kDa heavy neurofilaments (NfH) are located more peripherally. NF in the serum and CSF were suggested to correlate with damage to axons and disease activity in MS [37, 68].
Anti-neurofilament antibodies have also been suggested to be markers of tissue damage. Anti-neurofilament antibodies are detected both in serum and CSF of patients with MS and they are shown to correlate with brain parenchymal fraction, T2 and T2 lesion load [69, 70]. In another study, serum anti-neurofilament antibodies were significantly elevated in PPMS [71].
Lately, CSF NfL levels showed some prognostic value in MS, as the levels at diagnosis correlated with MS severity score, and patients with NfL levels above the median had 5-fold increased odds of severe MS, including conversion to SPMS at 8 to 20 years after disease onset [72]. In another cohort of patients with CIS, NfH levels in the CSF correlated with physical disability and brain volume loss over 1 year [73]. In another cohort of patients with RRMS followed up for a median of 14 years, CSF NfL levels at diagnosis correlated with the MS Severity Score in the long term, while cases with high NfL levels (>386 ng/l) were more likely to convert into SPMS than those with low levels (<60 ng/l) [74]. In a cohort of patients with progressive MS, NfH was a predictor of continuing disability, and NfL was a predictor of EDSS annual increase [75]. There is currently a new promising sensitive immunoassay for quantification of NfL in serum [76]. Serum NfL levels were reported to predict recovery after an episode of myelitis in RRMS [72, 77]. Moreover, patients with CIS had higher levels of serum NfL than controls, which was also associated with the number of T2-hyperintense and gadolinium-enhancing lesions, as well as with increased disability [40].
Although the data on neurofilament proteins as biomarkers show promise, their prognostic value in individual patients needs a more extensive validation through prospective cohort studies.
CHI3L1 and CHI3L2 Proteins
In a prospective study CSF CHI3L1 level was a strong predictor of disability progression and, in fact, it was the only significant independent risk factor associated with the development of disability in multivariate Cox regression models [58]. CSF CHI3L1 levels above the 170 ng/ml cut-off were conferring, as a unique predictor, a 4-fold increased risk for the development of disability. High CSF CHI3L1 levels were associated with earlier disability progression (5-year difference in median time to reach EDSS 3.0 vs patients with low-protein values) with a sensitivity > 70 % [58]. In another study, CSF CHI3L1 levels were associated with brain MRI abnormalities at baseline and disability progression during follow-up [78]. Moreover, other authors reported that higher serum and CSF CHI3L1 and CHI3L2 were found in progressive MS than in RRMS and CIS [59].
Proapoptotic Molecules: Fas and Fas Ligand
Several studies demonstrated downregulation of proapoptotic molecules in active MS, indicating abnormalities in the apoptotic cell death of lymphocytes in MS [79–81]. Increased mRNA expression of Fas and Fas ligand has been regularly reported in peripheral blood mononuclear cells in RRMS, but the data on the sFas have been inconsistent [82–86].
Adhesion Molecules: Soluble Platelet Endothelial Cell Adhesion Molecule 1, sP-Selectin, and sE-Selectin
Migration of immune cells into the CNS is mediated by adhesion molecules, normally expressed at very low levels on vascular endothelial cells but increase after cytokine stimulation in MS [87]. There are soluble forms of adhesion molecules as well, released from endothelial cells, immune cells, and platelets. The soluble adhesion molecules soluble platelet endothelial cell adhesion molecule 1, sP-selectin, and sE-selectin have been shown to be upregulated in patients with RRMS when compared with PPMS. The levels of these molecules were also found to be upregulated during MS exacerbations, suggesting their potential as biomarkers for disease activity [88]. Larger longitudinal studies are needed to confirm the clinical usefulness of these markers.
Metalloproteases and Nitric Oxide
Matrix metalloproteinases have been shown to contribute to the inflammatory injury to the BBB and CNS myelin. An elevated level of matrix metalloproteinase 9 was associated with active gadolinium-enhancing lesions on MRI in patients with MS [89, 90]. Similarly, free radicals such as nitric oxide (NO) that contribute to the neurodegenerative cascade in the CNS through oligodendrocyte injury, axonal degeneration, and impairment of nerve conduction were increased in some acute demyelinating lesions [11]. Elevated levels of NO metabolites nitrite and nitrate are associated with disease activity [91, 92]. NO synthase was also increased in patients with MS [93].
Neurotrohpins
The expression of some neurotrophins that can stimulate regeneration and promote repair has been described in MS lesions [94]. Low levels of brain-derived neurotrophic factor have been reported in blood and CSF [95, 96]. The levels of brain-derived neurotrophic factor, neural cell adhesion molecule, and ciliary neurotrophic factor in the CSF of patients with MS have been associated with disease activity [96, 97].
NfL
CSF levels of NfL are elevated in all stages of MS, without initial marked differences between RRMS and progressive MS. However, in RRMS the concentration of NfL is CSF and serum is consistently higher in patients who are in clinical exacerbation or who have gadolinium-enhancing lesions on MRI, while in progressive MS, NfL levels are elevated, irrespective of MRI activity, but this information still needs to be replicated in larger cohorts [40].
RNA Profiles: “MSa and MSb” Gene Signatures
In a transcriptomics study, an RNA profile (from peripheral mononuclear cells) identified 2 subsets of patients with MS differing in disease activity. An increased expression of genes involved in the “T-cell receptor” and “B-cell receptor” signaling pathways was found in a subset of patients called “MSa” as compared with their counterpart, the “MSb”. The MSa signature included genes found in the nuclear factor of activated T cells, integrin-linked kinase, phosphatidylinositol 3-kinase, and epidermal growth factor. The MSa and MSb gene signatures were associated with disease outcome, with the MSb patients being 40 % less likely to have a relapse. None of the available clinical and paraclinical data was different between the 2 MS subsets after correcting for testing of multiple hypotheses, except for a difference in disease duration at the time of sampling in patients treated with glatiramer acetate [98].
Noncoding miRNAs
Several noncoding RNAs in serum were also explored as biomarkers of disease activity in MS. A recent study reported that elevated levels of miR-92a-1 and miR-454 correlated with increasing disease severity disability [99, 100].
Cholesterol
Some researchers reported in patients with MS a relationship between disease progression and elevated serum levels of triglycerides, low-density lipoprotein, and total cholesterol, while high-density lipoprotein levels correlated with lower lesion volume load on MRI [101]. Furthermore, others showed a positive correlation between serum LDL levels and the number of active white matter lesions in patients with CIS [102]. However, the normal biological variability of the lipid profile in serum makes it difficult to validate these molecules as biomarkers in MS [103].
Tryptophan Metabolism and the Kynurenine Pathway
Alterations in tryptophan metabolism through the kynurenine pathway have been reported in patients with MS and other neurologic disorders [104, 105]. Some researchers examined the transcription of the tryptophan-depleting enzyme indoleamine 2,3 dioxygenase (IDO) in sera of stable patients with MS, patients during an acute MS relapse before and after treatment with corticosteroids, and healthy controls. IDO expression was increased during a relapse (before treatment with corticosteroids) compared with stable patients with MS. After treatment with glucocorticoids, clinical improvement occurred along with a significant reduction in IDO gene expression and IDO catalytic activity [106].
25-OH Vitamin D
Among other studies, an analysis of > 450 patients with CIS followed up to 5 years in 1 of the Betaferon/Betaseron trials showed that higher serum 25-OH vitamin D predicted less disease activity. They suggested that a 20 ng/ml increment in the mean serum vitamin D levels within the first year predicted a 57 % lower rate of new active lesions, 57 % lower relapse rate, 25 % lower increase in yearly T2 lesion volume, and 0.41 % lower loss in yearly brain volume [107]. Another group explored the data of 65 patients of the phase II CIS trial of atorvastatin (STAyCIS) and reported that each 25 nmol/l higher 25-OH vitamin D level was associated with 7.8 ml higher gray matter volume (95 % confidence interval 1.0–14.6), suggesting a potential impact on neurodegeneration and disability progression [108].
Biomarkers of Therapeutic Response
Anti-Interferon Neutralizing Antibodies
It has been established in clinical practice that anti-interferon (IFN)-β antibodies herald a lack of therapeutic effect of interferons in RRMS, although this biomarker identifies only a group of nonresponders to MS treatments [109]. Interestingly several human leukocyte antigen class II alleles and short nucleotide polymorphisms have been associated with anti-IFN-β neutralizing antibody titers [110, 111], although these data still need to be validated for use at the individual level. A recent prospective European MS cohort suggested that an early increase in binding antibody titers could reliably predict the development of anti-IFN-β neutralizing antibodies; moreover, the authors reported CXCL10 as a promising predictor of neutralizing antibody-associated IFN-β response attenuation [112]. Furthermore, some patients develop such neutralizing antibodies only transiently, making the judgment of their future response to IFN debatable. However, in a post hoc retrospective analysis of the BENEFIT trial it was shown that in early MS, early high levels of anti-IFN-β1b neutralizing antibodies predicted a high rate of persistence of the antibodies later on, suggesting an early differentiation of persistently neutralizing antibody-positive patients from transiently positive patients [113].
Concentrations of Interleukin-17 in Serum
There has been mounting evidence for involvement of interleukin (IL)-17 in the pathogenesis of MS [114, 115]. High concentrations of IL-17F before initiation of therapy were reported to be associated with lack of response to IFN-β [116]. However, in a better-powered study, levels of IL-17F measured at baseline and at 6 months after initiation of treatment did not correlate with clinical or radiologic failure on treatment after 2 years [117]. Only extremely high levels of IL-17F (>200 pg/ml), which were found in few patients (4.4 %), were associated with nonresponsiveness to IFN-β treatment.
Noncoding miRNAs
Levels of miRNAs in the blood also might be potential biomarkers of response to IFN-β [118, 119]. A prospective study showed that changes in miR-26a-5p concentrations in serum could serve as biomarkers of the effects of IFN-β therapy, and could have a good predictive value in identifying responders at the individual patient level [120].
Anti-natalizumab Antibodies
Several groups reported the clinical relevance of persisting antibodies against natalizumab [121, 122]. These antibodies are formed early during treatment, persist in around 6 % of patients, and are related to a decrease in treatment efficacy and adverse reactions to natalizumab. However, any new disease activity would generally be obvious clinically and radiologically in this group of patients, as relapses and new active or enhancing lesions rarely occur during such treatment in daily practice; therefore, there might be a limited role for anti-natalizumab antibodies as a biomarker in clinical practice [123].
Serum TNF-Related Apoptosis-Inducing Ligand
TNF-related apoptosis-inducing ligand (TRAIL) is a member of the TNF superfamily expressed in soluble and membrane bound forms from lymphocytes and monocytes in an activation-dependent manner [124]. It has been shown that soluble TRAIL inhibits proliferation of activated T cells [125, 126], and inhibition of TRAIL outside the CNS worsened experimental autoimmune encephalomyelitis [127]. Increased expression of TRAIL mRNA has been reported in peripheral blood mononuclear cellss of patients with RRMS treated with IFN-β who responded to treatment. Based on these observations it has been suggested that TRAIL could be used as a biomarker reflective of response to treatment with IFN-β in MS [128, 129].
B-Cell Activating Factor
As a member of the TNF family, B-cell activating factor (BAFF) is a major survival factor for B cells, which, classically, has been postulated to be involved in the development of many autoimmune and inflammatory conditions [130]. One prospective study of 170 patients with RRMS and 49 healthy controls, with a mean follow-up of 2.3 years, reported that plasma BAFF levels were significantly higher in stable patients with MS compared with controls. Nevertheless, stable patients with MS had significantly higher serum BAFF levels than patients with recent preceding relapses. Interestingly, treatment with IFN-β but not glatiramer acetate raised BAFF levels, and treatment of the relapses with high-dose intravenous steroids did not significantly change plasma BAFF levels in 65 % of patients [130]. Notably, a previous study in 73 patients with RRMS, 8 patients with melanoma treated with IFN-α, and 26 healthy controls, showed that IFN-β significantly increases serum BAFF levels [131].
Biomarkers to Predict the Risk of Adverse Effects of Disease-Modifying Therapy
Anti-JCV Antibodies in Serum
During treatment with natalizumab, the presence of anti-JCV antibodies in blood is associated with the development of progressive multifocal leukoencephalopathy (PML) [132, 133]. JCV antibody serum index enables stratification of the risk of PML in JCV-seropositive patients [134], as is currently used in clinical practice. In patients without immunosuppressant use prior to natalizumab, a low anti-JCV antibody index confers a low risk of PML. Increasing titers of anti-JCV antibodies, exposure to a previous immunosuppressant, and prolonged use of natalizumab increase dramatically the risk of PML, especially after 2 years of treatment. Therefore, anti-JCV antibodies in serum currently have an established role as a biomarker for risk stratification in patients treated with natalizumab.
L-Selectin-Expressing CD4+ T Cells in Peripheral Blood
Aiming to advance the ability to predict PML risk during treatment with natalizumab, the results of a study using flow cytometry in peripheral mononuclear blood cells suggested that the frequency of L-selectin-expressing CD4+ T cells was lower in patients who had received long-term treatment with natalizumab than in those patients not exposed to natalizumab, or healthy controls [135]. Furthermore, among a subgroup of patients who developed PML, a significant 9-fold decrease in the number of L-selectin-expressing CD4+ T cells was found in their blood samples taken before development of PML. Through a validation study in an independent cohort of patients, the same group reported that a low frequency of L-selectin-expressing CD4+ T cells in patients treated with natalizumab increased a patient’s relative risk of PML 55-fold [136]. However, recent data from a cohort of patients treated with natalizumab indicated that L-selectin is not a useful biomarker of PML risk [137]. Future research would have to clarify the usefulness of such a biomarker to predict the risk of PML in patients treated with natalizumab.
Discussion
MS biomarker research is an area of intense interest, as is evident by the number of publications on the subject. In this review we focused specifically on peripheral blood as an easily accessible tissue that is amenable to repeat sampling. A large number of interesting molecules and markers are emerging that have not been discussed in this review as we focused on the few biomarkers that have been replicated in more than 1 study.
Clinical implementation is clearly the goal of biomarker research, but several steps have to occur between discovery and implementation: namely, the finding must be verified, replicated, and then clinically validated. Technical aspects related to the methods of collection, measurement, and quality controls have to be instituted. Ideally, the techniques should be easily standardizable and affordable. Recently, there have been efforts to standardize the tools necessary for biomarker research and creating guidelines for biobanking [138–140] and quality controls [International Society for Biological and Environmental Repositories, http://www.isber.org]. The creation of these guidelines and multicenter collaborations will pave the way for more rapid implementation of biomarkers for MS and other inflammatory neurologic diseases.
Important limitations for the development of biomarkers include the critical need for quantitative, standardized outcome measures for MS disease activity and progression, and validated definitions of treatment response. Using only clinical evidence of disease activity is clearly insensitive as we know from MRI studies that inflammation can be present in the absence of clinical signs. Future studies may need to include MRI to distinguish groups with active versus stable disease. Multicenter collaborative efforts and the use of well-characterized cohorts that include banked longitudinal blood and other bio-fluid samples would go a long way towards advancing the field.
Advances in understanding the pathophysiologic mechanisms of MS are helping to identify novel candidate biomarkers. However, technological advances (e.g., proteomics, molecular profiling, immunophenotyping, and microarray gene and antigen analysis) allow simultaneous testing of multiple biomarkers. Implementation of international exchange of biological samples for the purpose of cross-validation and the use bioinformatics may lead to the developments of biomarkers panels that could be clinically useful.
Conclusion
MS is a complex disease where the primary area of pathology is not easily accessible, thus requiring investigators to sample surrogate material such as the CSF or the blood. But, in spite of these limitations, some biomarkers are emerging that may have value for diagnosis, predicting disease progression, and therapeutic response. Validation and replication studies are still needed, but ongoing collaborations will help move the field forward.
References
Polman CH, Reingold SC, Banwell B, et al. Diagnostic criteria for multiple sclerosis: 2010 revisions to the McDonald criteria. Ann Neurol 2011;69:292–302.
Awad A, Hemmer B, Hartung HP, Kieseier B, Bennett JL, Stuve O. Analyses of cerebrospinal fluid in the diagnosis and monitoring of multiple sclerosis. J Neuroimmunol 2010;219:1–7.
Sospedra M, Martin R. Immunology of multiple sclerosis. Annu Rev Immunol 2005;23:683–747.
Kasper LH, Shoemaker J. Multiple sclerosis immunology: the healthy immune system vs the MS immune system. Neurology 2010;74:S2–S8.
Selmi C, Mix E, Zettl UK. A clear look at the neuroimmunology of multiple sclerosis and beyond. Autoimmun Rev 2012;11:159–162.
Wekerle H. Lessons from multiple sclerosis: models, concepts, observations. Ann Rheum Dis 2008;67:56–60.
Zipp F. Apoptosis in multiple sclerosis. Cell Tissue Res 2000;301:163–171.
Pender MP Treating autoimmune demyelination by augmenting lymphocyte apoptosis in the central nervous system. J Neuroimmunol 2007;191:26–38.
Trapp BD, Nave KA. Multiple sclerosis: an immune or neurodegenerative disorder? Annu Rev Neurosci 2008;31:247–269.
Lassmann H. [Clinical and pathological topics of multiple sclerosis]. Rinsho Shinkeigaku 2009;49:715–718 (in Japanese).
Lassmann H. Axonal and neuronal pathology in multiple sclerosis: what have we learnt from animal models. Exp Neurol 2010;225:2-8.
Lucchinetti C, BrückW, Parisi J, Scheithauer B, Rodriguez M, Lassmann H. Heterogeneity of multiple sclerosis lesions: implications for the pathogenesis of demyelination. Ann Neurol 2000;47:707–717.
Lassmann H, Bruck W, Lucchinetti C. Heterogeneity of multiple sclerosis pathogenesis: implications for diagnosis and therapy. Trends Mol Med 2001;7:115–121.
Lassmann H, Bruck W, Lucchinetti CF. The immunopathology of multiple sclerosis: an overview. Brain Pathol 2007;17:210–218.
Kuhle J, Disanto G, Dobson, R, et al. Conversion from clinically isolated syndrome to multiple sclerosis: a large multicentre study. Mult Scler 2015; 21:1013–1024.
Wingerchuk D, Banwell B, Bennett J, et al. International consensus diagnostic criteria for neuromyelitis optica spectrum disorders. Neurology 2015;85:177–189.
McGuigan C, Craner M, Guadagno J, et al. Stratification and monitoring of Natalizumab-associated progressive multifocal leukoencephalopathy risk: recommendations from an expert group. J Neurol Neurosurg Psychiatry 2016;87:117–125.
Biomarkers Definitions Working Group. Biomarkers and surrogate endpoints: preferred definitions and conceptual framework. Clin Pharmacol Ther 2001;69:89–95.
Bielekova B, Martin R. Development of biomarkers in multiple sclerosis. Brain 2004;127:1463–1478.
Tumani H, Hartung HP, Hemmer B, et al. Cerebrospinal fluid biomarkers in multiple sclerosis. Neurobiol Dis 2009;35:117–127.
Harris VK, Sadiq SA. Disease biomarkers in multiple sclerosis: potential for use in therapeutic decision making. Mol Diagn Ther 2009;13:225–244.
Polman CH, Reingold SC, Edan G, et al. Diagnostic criteria for multiple sclerosis: 2005 revisions to the “McDonald Criteria”. Ann Neurol 2005;58:840–846.
Tejera-Alhambra M, Casrouge A, De Andrés C, et al. Plasma biomarkers discriminate clinical forms of multiple sclerosis. PLOS ONE 2015;10:e0128952.
Fenoglio C, Ridolfi E, Cantoni C, et al. Decreased circulating miRNA levels in patients with primary progressive multiple sclerosis. Mult Scler 2013;19:1938–1942.
Bauernfeind F, Rieger A, Schildberg FA, Knolle PA, Schmid-Burgk JL, Hornung V. NLRP3 inflammasome activity is negatively controlled by miR-223. J Immunol 2012;189:4175–4181.
Lv X, Jiang H, Liu Y, Lei X, Jiao J. MicroRNA-15b promotes neurogenesis and inhibits neural progenitor proliferation by directly repressing TET3 during early neocortical development. EMBO Rep 2014;15:1305–1314.
Cox MB, Cairns MJ, Gandhi KS, et al. MicroRNAs miR-17 and miR-20a inhibit T cell activation genes and are under-expressed in MS whole blood. PLOS ONE 2010;5:e12132.
Keller A, Leidinger P, Steinmeyer F, et al. Comprehensive analysis of microRNA profiles in multiple sclerosis including next-generation sequencing. Mult Scler 2014;20:295–303.
Siegel SR, Mackenzie J, Chaplin G, Jablonski NG, Griffiths L. Circulating microRNAs involved in multiple sclerosis. Mol Biol Rep 2012;39:6219–6225.
O'Connor KC, McLaughlin KA, De Jager PL, et al. Self-antigen tetramers discriminate between myelin autoantibodies to native or denatured protein. Nat Med 2007;13:211–217.
Kim S, Woodhall M, Kim J, et al. Antibodies to MOG in adults with inflammatory demyelinating disease of the CNS. Neurol Neuroimmunol Neuroinflamm 2015;2:e163.
Tanaka M, Tanaka K. Anti-MOG antibodies in adult patients with demyelinating disorders of the central nervous system. J Neuroimmunol 2014;270:98–99.
Höftberger R, Sepulveda M, Armangue T, et al. Antibodies to MOG and AQP4 in adults with neuromyelitis optica and suspected limited forms of the disease. Mult Scler 2014;21:866–874.
Kitley J, Woodhall M, Waters P, et al. Myelin-oligodendrocyte glycoprotein antibodies in adults with a neuromyelitis optica phenotype. Neurology 2012;79:1273–1277.
Quintana FJ, Farez MF, Viglietta V, et al. Antigen microarrays identify unique serum autoantibody signatures in clinical and pathologic subtypes of multiple sclerosis. Proc Natl Acad Sci U S A 2008;105:18889–18894.
Quintana FJ, Patel B, Yeste A, et al. Epitope spreading as an early pathogenic event in pediatric multiple sclerosis. Neurology 2014;83:2219–2226.
Lycke JN, Karlsson JE, Andersen O, Rosengren LE. Neurofilament protein in cerebrospinal fluid: a potential marker of activity in multiple sclerosis. J Neurol Neurosurg Psychiatry 1998;64:402–404.
Malmestrom C, Haghighi S, Rosengren L, Andersen O, Lycke J. Neurofilament light protein and glial fibrillary acidic protein as biological markers in MS. Neurology 2003;61:1720–1725.
Rejdak K, Petzold A, Stelmasiak Z, Giovannoni G. Cerebrospinal fluid brain specific proteins in relation to nitric oxide metabolites during relapse of multiple sclerosis. Mult Scler 2008;14:59–66.
Disanto G, Adiutori R, Dobson R, et al. Serum neurofilament light chain levels are increased in patients with a clinically isolated syndrome. J Neurol Neurosurg Psychiatry 2016;87:126–129.
Kapaki E, Paraskevas GP, Michalopoulou M, Kilidireas K. Increased cerebrospinal fluid tau protein in multiple sclerosis. Eur Neurol 2000;43:228–232.
Bartosik-Psujek H, Archelos JJ. Tau protein and 14-3-3 are elevated in the cerebrospinal fluid of patients with multiple sclerosis and correlate with intrathecal synthesis of IgG. J Neurol 2004;251:414–420.
Martinez-Yelamos A, Saiz A, Bas J, Hernandez JJ, Graus F, Arbizu T. Tau protein in cerebrospinal fluid: a possible marker of poor outcome in patients with early relapsing-remitting multiple sclerosis. Neurosci Lett 2004;363:14–17.
Bartosik-Psujek H, Stelmasiak Z. The CSF levels of total-tau and phosphotau in patients with relapsing-remitting multiple sclerosis. J Neural Transm 2006;113:339–345.
Guimaraes I, Cardoso MI, Sa MJ. Tau protein seems not to be a useful routine clinical marker of axonal damage in multiple sclerosis. Mult Scler 2006;12:354–356.
Terzi M, Birinci A, Cetinkaya E, Onar MK. Cerebrospinal fluid total tau protein levels in patients with multiple sclerosis. Acta Neurol Scand 2007;115:325–330.
Brettschneider J, Maier M, Arda S, et al. Tau protein level in cerebrospinal fluid is increased in patients with early multiple sclerosis. Mult Scler 2005;11:261–265.
Srivastava R, Aslam M, Kalluri SR, et al. Potassium channel KIR4.1 as an immune target in multiple sclerosis. N Engl J Med 2012;367:115–123.
Kraus V, Srivastava R, Kalluri SR, et al. Potassium channel KIR4.1- specific antibodies in children with acquired demyelinating CNS disease. Neurology 2014;82:470–473.
Nerrant E, Salsac C, Charif M, et al. Lack of confirmation of antiinward rectifying potassium channel 4.1 antibodies as reliable markers of multiple sclerosis. Mult Scler 2014;20:1699–1703.
Brickshawana A, Hinson SR, Romero MF, et al. Investigation of the KIR4.1 potassium channel as a putative antigen in patients with multiple sclerosis: a comparative study. Lancet Neurol 2013;13:795–806.
Brill L, Goldberg L, Karni A, et al. Increased anti-KIR4.1 antibodies in multiple sclerosis: could it be a marker of disease relapse? Mult Scler 2015;21:572–579.
Leoni V, Masterman T, Diczfalusy U, et al. Changes in human plasma levels of the brain specific oxysterol 24S-hydroxycholesterol during progression of multiple sclerosis. Neurosci Lett 2002;331:163–166.
Teunissen CE, Dijkstra CD, Polman CH, et al. Decreased levels of the brain specific 24S-hydroxycholesterol and cholesterol precursors in serum of multiple sclerosis patients. Neurosci Lett 2003;347:159–162.
Van de Kraats C, Killestein J, Popescu V, et al. Oxysterols and cholesterol precursors correlate to magnetic resonance imaging measures of neurodegeneration in multiple sclerosis. Mult Scler 2014;20:412–417.
Berger T, Rubner P, Schautzer F, et al. Antimyelin antibodies as a predictor of clinically definite multiple sclerosis after a first demyelinating event. N Engl J Med 2003;349:139–145.
Ketelslegers IA, Van Pelt DE, Bryde S, et al. MOG cell-based assay detects Non-MS Patients with inflammatory neurologic disease. Anti-MOG antibodies plead against MS diagnosis in an Acquired Demyelinating Syndromes cohort. Mult Scler 2015;21:1513–1520.
Cantó E, Tintoré M, Villar LM, et al. Chitinase 3-like 1: prognostic biomarker in clinically isolated syndromes. Brain 2015;138:918-931.
Hinsinger G, Galéotti N, Nabholz N, et al. Chitinase 3-like proteins as diagnostic and prognostic biomarkers of multiple sclerosis. Mult Scler 2015;21:1251–1261.
Szczucinski A, Losy J. Chemokines and chemokine receptors in multiple sclerosis. Potential targets for new therapies. Acta Neurol Scand 2007;115:137–146.
Festa ED, Hankiewicz K, Kim S, et al. Serum levels of CXCL13 are elevated in active multiple sclerosis. Mult. Scler 2009;15:1271–1279.
Sellebjerg F, Bornsen L, Khademi M, et al. Increased cerebrospinal fluid concentrations of the chemokine CXCL13 in active MS. Neurology 2009;73:2003–2010.
Brettschneider J, Czerwoniak A, Senel M, et al. The chemokine CXCL13 is a prognostic marker in clinically isolated syndrome (CIS). PLOS ONE 2010;5:e11986.
Khademi M, Kockum I, Andersson ML, et al. Cerebrospinal fluid CXCL13 in multiple sclerosis: a suggestive prognostic marker for the disease course. Mult Scler 2011;17:335–343.
Ragheb S, Li Y, Simon K, et al. Multiple sclerosis: BAFF and CXCL13 in cerebrospinal fluid. Mult Scler 2011;17:819–829.
Martinelli V, Dalla CG, Colombo B, et al. Vitamin D levels and risk of multiple sclerosis in patients with clinically isolated syndromes. Mult Scler 2014; 20:147–155.
Hagman S, Raunio M, Rossi M, Dastidar P, Elovaara I. Disease-associated inflammatory biomarker profiles in blood in different subtypes of multiple sclerosis: prospective clinical and mri follow-up study. J Neuroimmunol 2011;234:141–147.
Semra YK, Seidi OA, Sharief MK. Heightened intrathecal release of axonal cytoskeletal proteins in multiple sclerosis is associated with progressive disease and clinical disability. J Neuroimmunol 2002;122:132–139.
Silber E, Sharief M.K. Axonal degeneration in the pathogenesis of multiple sclerosis. J Neurol Sci 1999;170:11–18.
Eikelenboom MJ, Petzold A, Lazeron RH, et al. Multiple sclerosis: neurofilament light chain antibodies are correlated to cerebral atrophy. Neurology 2003;60:219–223.
Ehling R, Lutterotti A, Wanschitz J, et al. Increased frequencies of serum antibodies to neurofilament light in patients with primary chronic progressive multiple sclerosis. Mult Scler 2004;10:601–606.
Gaiottino J, Norgren N, Dobson R, et al. Increased neurofilament light chain blood levels in neurodegenerative neurological diseases. PLOS ONE 2013;8:e75091.
Khalil M, Enzinger C, Langkammer C, et al. CSF neurofilament and N-acetylaspartate related brain changes in clinically isolated syndrome. Mult Scler 2013;19:436–442.
Salzer J, Svenningsson A, Sundström P. Neurofilament light as a prognostic marker in multiple sclerosis. Mult Scler 2010;16:287–292.
Trentini A, Comabella M, Tintoré M, et al. N-Acetylaspartate and neurofilaments as biomarkers of axonal damage in patients with progressive forms of multiple sclerosis. J Neurol 2014;261:2338–2343.
Kuhle J, Barro C, Andreasson U, et al. Comparison of three analytical platforms for quantification of the neurofilament light chain in blood samples: ELISA, electrochemiluminescence immunoassay and Simoa. Clin Chem Lab Med 2016;54:1655–1661.
Kuhle J, Gaiottino J, Leppert D, et al. Serum neurofilament light chain is a biomarker of human spinal cord injury severity and outcome. J Neurol Neurosurg Psychiatry 2015;86:273–279.
Comabella M, Fernández M, Martin R, et al. Cerebrospinal fluid chitinase 3-like 1 levels are associated with conversion to multiple sclerosis. Brain 2010;133:1082–1093.
Sharief MK. Increased cellular expression of the caspase inhibitor FLIP in intrathecal lymphocytes from patients with multiple sclerosis. J Neuroimmunol 2000;111:203–209.
Semra YK, Seidi OA, Sharief M.K. Overexpression of the apoptosis inhibitor FLIP in T cells correlates with disease activity in multiple sclerosis. J Neuroimmunol 2001;113:268–274.
Sharief MK, Noori MA, Douglas MR, Semra K. Upregulated surviving expression in activated T lymphocytes correlates with disease activity in multiple sclerosis. Eur J Neurol 2002;9:503–510.
Inoue A, Koh CS, Sakai T, et al. Detection of the soluble form of the Fas molecule in patients with multiple sclerosis and human T-lymphotropic virus type I-associated myelopathy. J Neuroimmunol 1997;75:141–146.
Huang W, Huang MP, Gomes MA, Hillert J. Apoptosis mediators fasL and TRAIL are upregulated in peripheral blood mononuclear cells in MS. Neurology 2000;55:928–934.
Bilinska M, Frydecka I, Podemski R, Gruszka E. Fas expression on T cells and sFas in relapsing-remitting multiple sclerosis. Acta Neurol Scand 2003;107:387–393.
Gomes AC, Jonsson G, Mjornheim S, Olsson T, Hillert J, Grandien A. Upregulation of the apoptosis regulators cFLIP, CD95 and CD95 ligand in peripheral blood mononuclear cells in relapsing-remitting multiple sclerosis. J Neuroimmunol 2003;135:126–134.
Mahovic D, Petravic D, Petelin Z, Zurak N, Horvat G, Hajnsek S. Level of sFas/APO 1 in serum and cerebrospinal fluid in multiple sclerosis. Clin Neurol Neurosurg 2004;106:230–232.
Holman DW, Klein RS, Ransohoff RM. The Blood–brain barrier, chemokines and multiple sclerosis. Biochim Biophys Acta 2011;1812:220–230.
Kuenz B, Lutterotti A, Khalil M, et al. Plasma levels of soluble adhesion molecules sPECAM-1, sP-selectin and sE-selectin are associated with relapsing-remitting disease course of multiple sclerosis. J Neuroimmunol 2005;167:143–149.
Lee MA, Palace J, Stabler G, Ford J, Gearing A, Miller K. Serum gelatinase B, TIMP-1 and TIMP-2 levels in multiple sclerosis. A longitudinal clinical and MRI study. Brain 1999;122:191–197.
Waubant E, Goodkin D, Bostrom A, et al. IFN beta lowers MMP-9/TIMP-1 ratio, which predicts new enhancing lesions in patients with SPMS. Neurology 2003;60:52–57.
Acar G, Idiman F, Idiman E, Kirkali G, Cakmakci H, Ozakbas S. Nitric oxide as an activity marker in multiple sclerosis. J Neurol 2003;250:588–592.
Rejdak K, Eikelenboom MJ, Petzold A, et al. CSF nitric oxide metabolites are associated with activity and progression of multiple sclerosis. Neurology 2004;63:1439–1445.
Calabrese V, Scapagnini G, Ravagna A, et al. Nitric oxide synthase is present in the cerebrospinal fluid of patients with active multiple sclerosis and is associated with increases in cerebrospinal fluid protein nitrotyrosine and S-nitrosothiols and with changes in glutathione levels. J Neurosci Res 2002;70:580–587.
Hohlfeld R. Neurotrophic cross-talk between the nervous and immune systems: relevance for repair strategies in multiple sclerosis? J Neurol Sci 2008;265:93–96.
Azoulay D, Vachapova V, Shihman B, Miler A, Karni A. Lower brain derived neurotrophic factor in serum of relapsing remitting MS: reversal by glatiramer acetate. J Neuroimmunol 2005;167:215–218.
Frota ER, Rodrigues DH, Donadi EA, Brum DG, Maciel DR, Teixeira AL. Increased plasma levels of brain derived neurotrophic factor (BDNF) after multiple sclerosis relapse. Neurosci Lett 2009;460:130–132.
Weinstock-Guttman B, Zivadinov R, Tamaño-Blanco M, et al. Immune cell BDNF secretion is associated with white matter volume in multiple sclerosis. J Neuroimmunol 2007;188:167–174.
Ottoboni L, Keenan BT, Tamayo P, et al. An RNA profile identifies two subsets of multiple sclerosis patients differing in disease activity. Sci Transl Med 2012;4:153ra131.
Gandhi R, Healy B, Gholipour T, et al. Circulating microRNAs as biomarkers for disease staging in multiple sclerosis. Ann Neurol 2013;73:729–740.
Kacperska MJ, Jastrzebski K, Tomasik B, Walenczak J, Konarska-Krol M, Glabinski A. Selected extracellular microRNA as potential biomarkers of multiple sclerosis activity--preliminary study. J Mol Neurosci 2015;56:154–163.
Weinstock-Guttman B, Zivadinov R, Mahfooz N, et al. Serum lipid profiles are associated with disability and MRI outcomes in multiple sclerosis. J Neuroinflamm 2011;8:127.
Giubilei F, Antonini G, Di Legge S, et al. Blood cholesterol and MRI activity in first clinical episode suggestive of multiple sclerosis. Acta Neurol Scand 2002;106:109–112.
Itay R, Webb J, Stuve O, et al. Body fluid biomarkers in multiple sclerosis: how far we have come and how they could affect the clinic now and in the future. Expert Rev Clin Immunol 2015;11:69–91.
Lovelace, M.D., et al. Recent evidence for an expanded role of the kynurenine pathway of tryptophan metabolism in neurological diseases, Neuropharmacology 2016 Mar 16 [Epub ahead of print].
Lovelace MD, Varney B, Sundaram G, et al. current evidence for a role of the kynurenine pathway of tryptophan metabolism in multiple sclerosis. Front Immunol 2016;7:246.
Mancuso R, Hernis A, Agostini S, et al. Indoleamine 2,3 dioxygenase (IDO) expression and activity in relapsing- remitting multiple sclerosis. PLOS ONE 2015;10:e0130715.
Ascherio A, Munger K, White R, et al. Vitamin D as an early predictor of multiple sclerosis activity and progression. JAMA Neurol 2014;71:306–314.
Mowry E, Pelletier D, Gao Z, Howell M, Zamvil S, Waubant E. Vitamin D in clinically isolated syndrome: evidence for possible neuroprotection. Eur J Neurol 2016;23:327–332.
Polman CH, Bertolotto A, Deisenhammer F, et al. Recommendations for clinical use of data on neutralising antibodies to interferon-beta therapy in multiple sclerosis. Lancet Neurol 2010;9:740–750.
Buck D, Cepok S, Hoffmann S, et al. Influence of the HLA-DRB1 genotype on antibody development to interferon beta in multiple sclerosis. Arch Neurol 2011;68:480–487.
Hoffmann S, Cepok S, Grummel V, et al. HLA-DRB1*0401 and HLA-DRB1*0408 are strongly associated with the development of antibodies against interferon-β therapy in multiple sclerosis. Am J Hum Genet 2008;83:219–227.
Hegen H, Millonig A, Bertolotto A, et al. Early detection of neutralizing antibodies to interferon-beta in multiple sclerosis patients: binding antibodies predict neutralizing antibody development. Mult Scler 2014;20:577–587.
Gibbs E, Karim M E, Oger J. Antibody dissociation rates are predictive of neutralizing antibody (NAb) course: a comparison of interferon beta-1b-treated patients with transient versus sustained NAbs. Clin Immunol 2014;157:91–101.
Graber JJ, Allie SR, Mullen KM, et al. Interleukin-17 in transverse myelitis and multiple sclerosis. J Neuroimmunol 2008;196:124–132.
Matusevicius D, Kivisäkk P, He B, et al. Interleukin-17 mRNA expression in blood and CSF mononuclear cells is augmented in multiple sclerosis. Mult Scler 1999;5:101–104.
Axtell RC, de Jong BA, Boniface K, et al. T helper type 1 and 17 cells determine efficacy of interferon-beta in multiple sclerosis and experimental encephalomyelitis. Nat Med 2010;16:406–412.
Hartung HP, Steinman L, Goodin DS, et al. Interleukin 17F level and interferon β response in patients with multiple sclerosis. JAMA Neurol 2013;70:1017–1021.
Hecker M, Thamilarasan M, Koczan D, et al. MicroRNA expression changes during interferon-beta treatment in the peripheral blood of multiple sclerosis patients. Int J Mol Sci 2013;14:16087–16110.
Liu X, Luo Y, Luo Z, Yang H. Biomarker studies in multiple sclerosis: from proteins to noncoding RNAs. Neurochem Res 2014;39:1661–1674.
De Felice B, Mondola P, Sasso A, et al. Small non-coding RNA signature in multiple sclerosis patients after treatment with interferon-β. BMC Med Genomics 2014;7:26.
Vennegoor A, Rispens T, Strijbis EM, et al. Clinical relevance of serum natalizumab concentration and anti-natalizumab antibodies in multiple sclerosis. Mult Scler 2013;19:593–600.
Lundkvist M, Engdahl E, Holmén C, et al. Characterization of anti-natalizumab antibodies in multiple sclerosis patients. Mult Scler 2013;19:757–764.
Teunissen C, Malekzadeh A, Leurs C, Bridel C, Killestein J. Body fluid biomarkers for multiple sclerosis-the long road to clinical application. Nat Rev Neurol 2015;11:585–596.
Ehrlich S, Infante-Duarte C, Seeger B, Zipp F. Regulation of soluble and surface-bound TRAIL in human T cells, B cells, and monocytes. Cytokine 2003;24:244–253.
Diehl GE, Yue HH, Hsieh K, et al. TRAIL-R as a negative regulator of innate immune cell responses. Immunity 2004;21:877–889.
Lunemann JD, Waiczies S, Ehrlich S, et al. Death ligand TRAIL induces no apoptosis but inhibits activation of human (auto)antigen-specific T cells. J Immunol 2002;168:4881–4888.
Hilliard B, Wilmen A, Seidel C, Liu TS, Goke R, Chen Y. Roles of TNF-related apoptosis-inducing ligand in experimental autoimmune encephalomyelitis. J Immunol 2001;166:1314–1319.
Wandinger KP, Lunemann JD, Wengert O, et al. TNF-related apoptosis inducing ligand (TRAIL) as a potential response marker for interferon-beta treatment in multiple sclerosis. Lancet 2003;361:2036–2043.
Bartosik-Psujek H, Stelmasiak Z. Correlations between IL-4, IL-12 levels and CCL2, CCL5 levels in serum and cerebrospinal fluid of multiple sclerosis patients. J Neural Transm 2005;112:797-803.
Kannel K, Alnek K, Vahter L, Gross-Paju K, Uibo R, Kisand KV. Changes in blood B cell activating factor (BAFF) levels in multiple sclerosis: a sign of treatment outcome. PLOS ONE 2015;10:e0143393.
Krumbholz M, Faber H, Steinmeyer F, et al. Interferon-b increases BAFF levels in multiple sclerosis: implications for B cell autoimmunity. Brain 2008;131:1455–1463.
Bloomgren G, Richman S, Hotermans C, et al. Risk of natalizumab associated progressive multifocal leukoencephalopathy. N Engl J Med 2012;366:1870-1880.
Calabresi PA, Giovannoni G, Confavreux C, et al. The incidence and significance of anti-natalizumab antibodies. Neurology 2007;69:1391–1403.
Plavina T, Subramanyam M, Bloomgren G, et al. Anti-JC virus antibody levels in serum or plasma further define risk of natalizumab-associated progressive multifocal leukoencephalopathy. Ann Neurol 2014;76:802–812.
Schwab N, Schneider-Hohendorf T, Posevitz V, et al. L-selectin is a possible biomarker for individual PML risk in Natalizumab-treated MS patients. Neurology 2013;81:865–871.
Lieberman L, Zeng W, Singh C, et al. CD62L is not a reliable biomarker for predicting PML risk in Natalizumab-treated R-MS patients. Neurology 2016;86:375–381.
Schwab N, Schneider-Hohendorf T, Pignolet B, et al. PML risk stratification using anti-JCV antibody index and L-selectin. Mult Scler 2016;22:1048–1060.
Teunissen C, Menge T, Altintas A, et al. Consensus definitions and application guidelines for control groups in cerebrospinal fluid biomarker studies in multiple sclerosis. Mult Scler 2013;19:1802–1809.
Gnanapavan S, Hegen H, Khalil M, et al. Guidelines for uniform reporting of body fluid biomarker studies in neurologic disorders. Neurology 2014;83:1210–1216.
Teunissen CE, Tumani H, Engelborghs S, Mollenhauer B. Biobanking of CSF: international standardization to optimize biomarker development. Clin Biochem 2014;47:288–292.
Required Author Forms
Disclosure forms provided by the authors are available with the online version of this article.
Author information
Authors and Affiliations
Corresponding author
Electronic supplementary material
Below is the link to the electronic supplementary material.
ESM 1
(PDF 1224 kb)
Rights and permissions
About this article
Cite this article
El Ayoubi, N.K., Khoury, S.J. Blood Biomarkers as Outcome Measures in Inflammatory Neurologic Diseases. Neurotherapeutics 14, 135–147 (2017). https://doi.org/10.1007/s13311-016-0486-7
Published:
Issue Date:
DOI: https://doi.org/10.1007/s13311-016-0486-7