Abstract
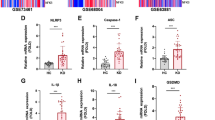
Tumor necrosis factor-α (TNF-α), a pro-apoptotic cytokine, is involved in vascular hyperpermeability, tissue edema, and inflammation. We hypothesized that TNF-α induces microvascular hyperpermeability through the mitochondria-mediated intrinsic apoptotic signaling pathway. Rat lung microvascular endothelial cells grown on Transwell inserts, chamber slides, or dishes were treated with recombinant TNF-α (10 ng/ml) in the presence or absence of a caspase-3 inhibitor, Z-DEVD-FMK (100 μM). Fluorescein isothiocyanate (FITC)-albumin (5 mg/ml) was used as a marker of monolayer permeability. Mitochondrial reactive oxygen species (ROS) was determined using dihydrorhodamine 123 and mitochondrial transmembrane potential using JC-1. The adherens junction integrity and actin cytoskeletal organization were studied using β-catenin immunofluorescence and rhodamine phalloidin, respectively. Caspase-3 activity was measured fluorometrically. The pretreatment with Z-DEVD-FMK (100 μM) attenuated TNF-α-induced (10 ng/ml) disruption of the adherens junctions, actin stress fiber formation, increased caspase-3 activity, and monolayer hyperpermeability (p < 0.05). TNF-α (10 ng/ml) treatment resulted in increased mitochondrial ROS formation and decreased mitochondrial transmembrane potential. Intrinsic apoptotic signaling-mediated caspase-3 activation plays an important role in regulating TNF-α-induced endothelial cell hyperpermeability.





Similar content being viewed by others
References
Bubici C, Papa S, Dean K, Franzoso G (2006) Mutual cross-talk between reactive oxygen species and nuclear factor-kappa B: molecular basis and biological significance. Oncogene 25:6731–6748
Campbell MT, Dagher P, Hile KL, Zhang H, Meldrum DR, Rink RC, Meldrum KK (2008) Tumor necrosis factor-α induces intrinsic apoptotic signaling during renal obstruction through truncated Bid activation. J Urol 180:2694–2700
Childs EW, Tharakan B, Hunter FA, Isong M, Liggins ND (2008) Mitochondrial complex III is involved in proapoptotic BAK-induced microvascular endothelial cell hyperpermeability. Shock 29:636–641
Childs EW, Tharakan B, Hunter FA, Tinsley JH, Cao X (2007) Apoptotic signaling induces hyperpermeability following hemorrhagic shock. Am J Physiol Heart Circ Physiol 292:H3179–3189
Childs EW, Udobi KF, Hunter FA, Dhevan V (2005) Evidence of transcellular albumin transport after hemorrhagic shock. Shock 23:565–570
Childs EW, Udobi KF, Wood JG, Hunter FA, Smalley DM, Cheung LY (2002) In vivo visualization of reactive oxidants and leukocyte-endothelial adherence following hemorrhagic shock. Shock 18:423–427
Dada LA, Sznajder JI (2011) Mitochondrial Ca2+ and ROS take center stage to orchestrate TNF-α-mediated inflammatory responses. J Clin Invest 121:1683–1685
Dewar D, Moore FA, Moore EE, Balogh Z (2009) Postinjury multiple organ failure. Injury 40:912–918
Fulda S, Debatin KM (2006) Extrinsic versus intrinsic apoptosis pathways in anticancer chemotherapy. Oncogene 25:4798–4811
Galluzzi L, Blomgren K, Kroemer G (2009) Mitochondrial membrane permeabilization in neuronal injury. Nat Rev Neurosci 10:481–494
Groeneveld AB (2002) Vascular pharmacology of acute lung injury and acute respiratory distress syndrome. Vasc Pharmacol 39:247–256
Goldblum SE, Hennig B, Jay M, Yoneda K, McClain CJ (1989) Tumor necrosis factor alpha-induced pulmonary vascular endothelial injury. Infect Immun 57:1218–1226
Hartsock A, Nelson WJ (2008) Adherens and tight junctions: structure, function and connections to the actin cytoskeleton. Biochim Biophys Acta 1778:660–669
Heller R, Unbehaun A, Schellenberg B, Mayer B, Werner-Felmayer G, Werner ER (2001) L-ascorbic acid potentiates endothelial nitric oxide synthesis via a chemical stabilization of tetrahydrobiopterin. J Biol Chem 276:40–47
Hotchkiss RS, Strasser A, McDunn JE, Swanson PE (2009) Cell death. N Engl J Med 361:1570–1583
Jia L, Liu Z, Sun L, Miller SS, Ames BN, Cotman CW, Liu J (2007) Acrolein, a toxicant in cigarette smoke, causes oxidative damage and mitochondrial dysfunction in RPE cells: protection by (R)-alpha-lipoic acid. Invest Ophthalmol Vis Sci 48:339–348
Johansen JS, Harris AK, Rychly DJ, Ergul A (2005) Oxidative stress and the use of antioxidants in diabetes: linking basic science to clinical practice. Cardiovasc Diabetol 4:5
Li AE, Ito H, Rovira II, Kim KS, Takeda K, Yu ZY, Ferrans VJ, Finkel T (1999) A role for reactive oxygen species in endothelial cell anoikis. Circ Res 85:304–310
Liu J, Ames BN (2005) Reducing mitochondrial decay with mitochondrial nutrients to delay and treat cognitive dysfunction, Alzheimer’s disease, and Parkinson’s disease. Nutr Neurosci 8:67–89
Moffitt KL, Martin SL, Walker B (2010) From sentencing to execution—the processes of apoptosis. J Pharm Pharmacol 62:547–562
Packer L, Roy S, Sen CK (1997) Alpha-lipoic acid: a metabolic antioxidant and potential redox modulator of transcription. Adv Pharmacol 38:79–101
Perocchi F, Gohil VM, Girgis HS, Huertas A, Quadri SK, Horiuchi K, Inamdar N, Emin MT, Lindert J, Ten VS, Bhattacharya S, Bhattacharya J (2010) MICU1 encodes a mitochondrial EF hand protein required for Ca(2+) uptake. Nature 467:291–296
Petrache I, Birukova A, Ramirez SI, Garcia JG, Verin AD (2003) The role of the microtubules in tumor necrosis factor-alpha-induced endothelial cell permeability. Am J Respir Cell Mol Biol 28:574–581
Petrache I, Verin AD, Crow MT, Birukova A, Liu F, Garcia JG (2001) Differential effect of MLC kinase in TNF-alpha-induced endothelial cell apoptosis and barrier dysfunction. Am J Physiol Lung Cell Mol Physiol 280:L1168–L1178
Prasain N, Stevens T (2009) The actin cytoskeleton in endothelial cell phenotypes. Microvasc Res 77:53–63
Rowlands DJ, Islam MN, Das SR et al (2011) Activation of TNFR1 ectodomain shedding by mitochondrial Ca2+ determines the severity of inflammation in mouse lung microvessels. J Clin Invest 121:1986–1999
Sawant DA, Tharakan B, Adekanbi A, Hunter FA, Smythe WR, Childs EW (2011) Inhibition of VE-cadherin proteasomal degradation attenuates microvascular hyperpermeability. Microcirculation 18:46–55
Sawant DA, Tharakan B, Hunter FA, Smythe WR, Childs EW (2011) Role of β-catenin in regulating microvascular endothelial cell hyperpermeability. J Trauma 70:481–487
Sawant DA, Tharakan B, Tobin RP, Reilly J, Hunter FA, Newell MK, Smythe WR, Childs EW (2013) Microvascular endothelial cell hyperpermeability induced by endogenous caspase 3 activator staurosporine. J Trauma Acute Care Surg 74:516–523
Shankar R, Melstrom KA Jr, Gamelli RL (2007) Inflammation and sepsis: past, present, and the future. J Burn Care Res 28:566–571
Tharakan B, Hellman J, Sawant DA, Tinsley JH, Parrish AR, Hunter FA, Smythe WR, Childs EW (2012) β-Catenin dynamics in the regulation of microvascular endothelial cell hyperpermeability. Shock 37:306–311
Tharakan B, Holder-Haynes JG, Hunter FA, Childs EW (2008) Alpha lipoic acid attenuates microvascular endothelial cell hyperpermeability by inhibiting the intrinsic apoptotic signaling. Am J Surg 195:174–178
Tharakan B, Hunter FA, Smythe WR, Childs EW (2008) Alpha-lipoic acid attenuates hemorrhagic shock-induced apoptotic signaling and vascular hyperpermeability. Shock 30:571–577
Vandenbroucke E, Mehta D, Minshall R, Malik AB (2008) Regulation of endothelial junctional permeability. Ann NY Acad Sci 1123:134–145
van Nieuw Amerongen GP, van Hinsbergh VW (2002) Targets for pharmacological intervention of endothelial hyperpermeability and barrier function. Vasc Pharmacol 39:257–272
Acknowledgments
We acknowledge the Texas A&M Health Science Center College of Medicine Integrated Microscopy and Imaging Laboratory.
Funding
This work was supported by a grant (1K01HL07815-01A1) from National Heart, Lung and Blood Institute, National Institutes of Health, USA.
Conflict of interest
The authors have no conflict of interest.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Sawant, D.A., Wilson, R.L., Tharakan, B. et al. Tumor necrosis factor-α-induced microvascular endothelial cell hyperpermeability: role of intrinsic apoptotic signaling. J Physiol Biochem 70, 971–980 (2014). https://doi.org/10.1007/s13105-014-0366-8
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s13105-014-0366-8