Abstract
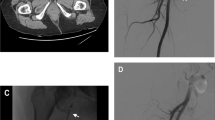
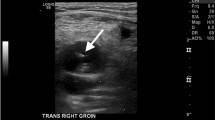
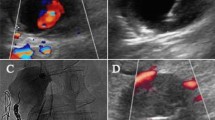
The increasing number of percutaneous endovascular procedures in highly anticoagulated patients has increased the possibility of iatrogenic femoral artery pseudoaneurysm (IFAP). Ultrasound (US)-guided percutaneous thrombin injection is one of the feasible treatments; however, there are concerns about complications such as peripheral embolization. This study was performed to examine the efficacy and safety of treatment of IFAPs using a combination of percutaneous thrombin injection and intravascular balloon inflation. In this retrospective, single-center study, we analyzed 11 patients who developed and were treated for IFAPs from January 2017 through April 2020. The patients were treated with endovascular therapy (EVT) with percutaneous thrombin injection. The technique utilized fluoroscopic guidance to place a balloon at the neck of the IFAP, and the balloon was then inflated to prevent the inflow of blood to the aneurysm. We then performed US-guided thrombin injection. The mean age was 72.36 ± 10.43 years; mean body mass index (BMI) was 25.25 ± 3.18. All patients had hypertension, 72.7% were undergoing hemodialysis, and 54.5% used oral anticoagulant drugs. The mean aneurysm size was 24.34 ± 13.54 mm. The approach was transfemoral in ten patients and transradial in one patient. All procedures were successful, and there were no complications. The mean thrombin dose was 677.3 ± 410.7 IU; the total hemostatic time was 45.4 ± 24.9 min. In conclusion, the combination of percutaneous thrombin injection and endovascular balloon inflation was feasible and safe for the treatment of IFAPs. This technique may contribute to the treatment of IFAPs.



Similar content being viewed by others
References
Stone PA, Campbell JE, AbuRahma AF. Femoral pseudoaneurysm after percutaneous access. J Vasc Surg. 2014;60:1359–66.
Otsuka M, Shiode N, Nakao Y, Ikegami Y, Kobayashi Y, Takeuchi A, et al. Comparison of radial, brachial, and femoral accesses using hemostatic devices for percutaneous coronary intervention. Cardiovasc Interv Ther. 2018;33:62–9.
Schneider C, Malisius R, Kuchler R, Lampe F, Krause K, Bahlmann E, et al. A prospective study on ultrasound-guided percutaneous thrombin injection for treatment of iatrogenic post-catheterisation femoral pseudoaneurysms. Int J Cardiol. 2009;131:356–61.
Webber GW, Jang J, Gustavson S, Olin JW. Contemporary management of postcatheterization pseudoaneurysms. Circulation. 2007;115:2666–74.
Castillo-Sang M, Tsang AW, Almaroof B, Cireddu J, Sferra J, Zelenock GB, et al. Femoral artery complications after cardiac catheterization: a study of patient profile. Ann Vasc Surg. 2010;24:328–35.
Fellmeth BD, Roberts AC, Bookstein JJ, Freischlag JA, Forsythe JR, Buckner NK, et al. Postangiographic femoral artery injuries:nonsurgical repair with US-guided compression. Radiology. 1991;178:671–5.
Stone P, Lohan JA, Copeland SE, Hamrick RE Jr, Tiley EH 3rd, Flaherty SK. Iatrogenic pseudoaneurysms: comparison of treatment modalities, including duplex-guided thrombin injection. W V Med J. 2003;99:230–2.
Ugurluoglu A, Katzenschlager R, Ahmadi R, Atteneder M, Koppensteiner R, Lang G, et al. Ultrasound guided compression therapy in 134 patients with iatrogenic pseudo-aneurysms: advantage of routine duplex ultrasound control of the puncture site following transfemoral catheterization. Vasa. 1997;26:110–6.
Cope CZR. Coagulation of aneurysms by direct percutaneous thrombin injection. AJR Am J Roentgenol. 1986;147:383–7.
Chen DH, Sammel AM, Jain P, Jepson NS. Cardiologist operated ultrasound guided thrombin injection as asafe and efficacious first line treatment for iatrogenic femoral artery pseudoaneurysms. Heart Lung Circ. 2015;24:165–72.
Kurzawski J, Sadowski M, Sadowska AJ. Complications of percutaneous thrombin injection inpatients with postcatheterization femoral pseudoaneurysm. J Clin Ultrasound. 2016;44:188–95.
Stolt M, Dullaeus RB, Herold J. Do not underestimate the femoral pseudoaneurysm. Vasa. 2018;47:177–85.
Toursarkissian B, Allen BT, Petrinec D, Thompson RW, Rubin BG, Reilly JM, et al. Spontaneous closure of selected iatrogenic pseudoaneourysms and arteriovenous fistulae. J Vasc Surg. 1997;25:803–8.
Eisenberg L, Paulson EK, Kliewer MA, Hudson MP, DeLong DM, Carroll BA. Sonographically guided compression repair of pseudoaneurysms: future experience from a single institution. AJR Am J Roentgenol. 1999;173:1567–73.
Kang SS, Labropoulos N, Mansour MA, Michelini M, Filliung D, Baubly MP, et al. Expanded indications for ultrasound-guided thrombin injection of pseudoaneurysms. J Vasc Surg. 2000;31:289–98.
Hofmann I, Wunderlich N, Robertson G, Kieback A, Haller C, Pfeil W, et al. Percutaneous injection of thrombin for the treatment of pseudoaneurysm: the German multicentre registry. Eurointervention. 2007;3:321.
Kodama A, Yamamoto M, Shimura T, Kagase A, Koyama Y, Tada N, et al. Comparative data of single versus double ProGlide vascular preclose technique after percutaneous transfemoral transcatheter aortic valve implantation from the Optimized CathEter vAlvular iNtervention (OCEAN-TAVI) Japanese Multicenter Registry. Catheter Cardiovasc Interv. 2017;90:55–62.
Mogi S, Endo A, Kawamura A. Left main trunk perforation sealed by 90 second perfusion balloon inflation. J Invasive Cardio. 2012;24:115–8.
Nakabayashi K, Kaneko N, Sunaga D, Matsui A, Tanaka K, Ando H, et al. Utility of a 0.035′′ compatible rapid-exchange balloon (Metacross RX) as a perfusion balloon in endovascular therapy compared with conventional percutaneous coronary intervention: a mini-review. Cardiovasc Revasc Med. 2017;18:619–22.
Shinozaki N, Ikari Y. Superficial femoral artery stenting via radial access using R2P® Misago® stents: first-in-human report of the new R2P® system. SAGE Open Med Case Rep. 2019;7:1–4.
Parodi JC, Schonholz C, Ferreira LM, Bergan J. Endovascular stent-graft treatment of traumatic arterial lesions. Ann Vasc Surg. 1999;13:121–9.
Moulakakis KG, Sfyroeras GS, Alexiou VG, Kakisis J, Lazaris A, Vasdekis SN, et al. Endovascular management of infected illiofemoral pseudoaneurysms: a case series. Vasc Endovascular Surg. 2016;50:421–6.
Hadziomerovic A, Jetty P, Gupta A. Angioseal-assisted closure of iatrogenic refractory femoral arterial pseudoaneurysm: a novel technique. JACC Cardiovasc Interv. 2016;9:e55–7.
Ibrahim K, Christoph M, Wunderlich C, Jellinghaus S, Loehn T, Youssef A, et al. A novel interventional method for trating femoral pseudoaneurysms:results from a monocentric experience. Eurointervention. 2017;13:366–70.
Ergun O, Çeltikçi P, Güneş Tatar İ, Yılmaz M, Hekimoğlu B. Percutaneous thrombin injection treatment of a femoral artery pseudoaneurysm with simultaneous arterial balloon occlusion: Case report and review of the literature. Turk Kardiyol Dern Ars. 2016;44:684–9.
Vowels TJ, Zubair MM, Bismuth J, Le L. Balloon-assisted ultrasound-guided percutaneous thrombin injection of iatrogenic femoral artery pseudoaneurysms: a case report and description of the technique. Vasc Endovascular Surg. 2020;54:532–5.
Acknowledgements
We thank Andrea Baird, MD, from Edanz Group (https://en-author-services.edanzgroup.com/ac) for editing a draft of this manuscript.
Funding
This research received no specific grants from any funding agency in the public, commercial, or not-for-profit sectors.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interests
The authors declare no potential conflicts of interest regarding the research, authorship, and/or publication of this article.
Ethical approval
All procedures were performed in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Declaration of Helsinki and its later amendments or comparable ethical standards. The study was approved by the Institutional Review Board of Asahi General Hospital.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Hayakawa, N., Kodera, S., Miyauchi, A. et al. Effective treatment of iatrogenic femoral pseudoaneurysms by combined endovascular balloon inflation and percutaneous thrombin injection. Cardiovasc Interv and Ther 37, 158–166 (2022). https://doi.org/10.1007/s12928-021-00764-9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12928-021-00764-9