Abstract
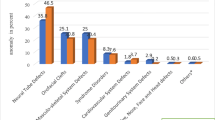
Monitoring newborns for adverse outcomes like stillbirth and major congenital anomalies (MCA) is being carried out in government hospitals since 1995 in and around high-level natural radiation areas, a narrow strip of land on the southwest coast of Kerala, India. Natural deposits of monazite sand containing thorium and its daughter products account for elevated levels of natural radiation. Among 141,540 newborns [140,558 deliveries: 139,589 singleton, 957 twins (6.81 ‰), 11 triplets (0.078 ‰), and one quadruplet] screened, 615 (4.35 ‰) were stillbirth and MCA were seen in 1,370 (9.68 ‰) newborns. Clubfoot (404, 2.85 ‰) was the most frequent MCA followed by hypospadias (152, 2.10 ‰ among male newborns), congenital heart disease (168, 1.19 ‰), cleft lip/palate (149, 1.05 ‰), Down syndrome (104, 0.73 ‰), and neural tube defects (72, 0.51 ‰). Newborns with MCA among stillbirths were about 20-fold higher at 190.24 ‰ (117/615) compared to 8.89 ‰ (1,253/140,925) among live births (P < .001). Logistic regression was carried out to compare stillbirth, overall, and specific MCA among newborns from areas with dose levels of ≤1.5, 1.51–3.0, 3.01–6.0 and >6 mGy/year after controlling for maternal age at birth, gravida, consanguinity, ethnicity, and gender of the baby. Clubfoot showed higher prevalence of 3.26 ‰ at dose level of 1.51–3.0 mGy/year compared to 2.33 ‰ at ≤1.5 mGy/year (OR = 1.39; 95 % CI, 1.12–1.72), without indication of any clear dose–response. Prevalences of stillbirth, overall MCA, and other specific MCA were similar across different dose levels and were relatively lower than that reported elsewhere in India, probably due to better literacy, health awareness, and practices in the study population.

Similar content being viewed by others
References
Ahman E, Zupan J (2007) Neonatal and perinatal mortality—country, regional and global estimates 2004. World Health Organisation, Geneva
Ayengar ARG, Sundaram K, Mistry KB, Suntha CM, Nambi CSV, Kaithuria SP et al (1972) Evaluation of the long term effects of high background radiation on selected population groups of Kerala coasts. In: Proceedings of 4th UN International Conference on Peaceful Uses of Atomic Energy. United Nations, New York, pp 31–51
Bharatwal DS, Vaze GH (1959) Radiation dose measurements in the monazite areas of Kerala State in India. In: Proceedings of the 2nd UN International Conference on Peaceful Uses of Atomic Energy. United Nations, New York, p 156
Bharucha BA (1998) Study of malformation and Down syndrome in India (SOMDI): Bombay region. Indian J Hum Genet 4:88–92
Breslow NE, Day NE (1987) Statistical methods in cancer research, vol II: The design and analysis of cohort studies. Oxford University Press, Oxford
Carothers AD, Boyd E, Lowther G, Ellis PM, Couzin DA, Faed MJ et al (1999) Trends in prenatal diagnosis of Down syndrome and other autosomal trisomies in Scotland 1990 to 1994, with associated cytogenetic and epidemiological findings. Genet Epidemiol 16(2):179–190
Chaturvedi P, Banerjee KS (1989) Spectrum of congenital malformations in newborns from rural Maharashtra. Indian J Pediatr 56(4):501–507
Cherian A, Seena S, Bullock RK, Antony AC (2005) Incidence of neural tube defects in the least-developed area of India: a population-based study. Lancet 366:930–931
Cheriyan VD, Kurien CJ, Das B, Ramachandran EN, Karuppasamy CV, Thampi MV et al (1999) Genetic monitoring of the human population from high level natural radiation areas of Kerala on the southwest coast of India. II. Incidence of numerical and structural chromosomal aberrations in the lymphocytes of newborns. Radiat Res 152((Suppl)):S154–S158
Choudhury AR, Mukherjee M, Sharma A, Talukder G, Goash PK (1989) Study of 1,26,266 consecutive births for major congenital defects. Ind J Pediatr 56(4):493–499
Coggle JE (1983) Biological effects of radiation, 2nd edn. Taylor and Francis Inc, New York
Das B, Karuppasamy CV (2009) Spontaneous frequency of micronuclei among the newborns from high level natural radiation areas of Kerala in the southwest coast of India. Int J Radiat Biol 85(3):272–280. doi:10.1080/09553000902751462
Das B, Saini D, Seshadri M (2009) Telomere length in human adults and high level natural background radiation. PLoS One 4(12):e8440
Forster L, Forster P, Lutz-Bonengel S, Willkomm H, Brinkmann B (2002) Natural radioactivity and human mitochondrial DNA mutations. Proc Natl Acad Sci USA 99:13950–13954
Gaulden ME (1992) Maternal age effect: the enigma of Down syndrome and other trisomic conditions. Mutat Res 296(1–2):69–88
Ghirri P, Scaramuzzo RT, Bertelloni S, Pardi D, Celandroni A, Cocchi G et al (2009) Prevalence of hypospadias in Italy according to severity, gestational age and birthweight: an epidemiological study. Ital J Pediatr 35:18. doi:10.1186/1824-7288-35-18
Gruneberg H (1964) Genetic research in an area of high natural radioactivity in South India. Nature 204:222–224
Gruneberg H, Bains GS, Berry RJ, Riles LL, Smith CAB, Weiss RA (1966) A search for genetic effects of high natural radioactivity in South India. Report No. SRS 307. London: Medical Research Council, Her Majesty's Stationary Office
Gupta RK, Gupta CR, Singh D (2003) Incidence of congenital malformations of the musculoskeletal system in new live borns in Jammu. JK Sci 5(4):157–160
Hecht CA, Hook EB (1996) Rates of Down syndrome at live birth by one-year maternal age intervals in studies with apparent close to complete ascertainment in populations of European origin: a proposed revised rate schedule for use in genetic and prenatal screening. Am J Med Genet 62(4):376–385
Jaikrishan G, Andrews VJ, Thampi MV, Koya PKM, Chauhan PS (1999) Genetic monitoring of the human population from high level natural radiation areas of Kerala on the Southwest Coast of India. I. Prevalence of congenital malformations in newborns. Radiat Res 152(Sppl):S149–S153
Khalil A, Aggarwal R, Thirupuram S, Arora R (1994) Incidence of congenital heart disease among hospital live births in India. Indian Pediatr 31(5):519–527
Khan HA, Sempos CT (1989) Statiscal methods in epidemiology. Oxford University Press, Oxford
Kochupillai N, Verma IC, Grewal MS, Ramalingaswamy V (1976) Down syndrome and related abnormalities in an area of high background radiation in coastal Kerala. Nature 262:60–61
Koya PKM, Chougaonkar MP, Predeep P, Jojo PJ, Cheriyan VD, Mayya YS et al (2012) Effect of low and chronic radiation exposure: a case-control study of mental retardation and cleft lip/palate in the monazite bearing coastal areas of Southern Kerala. Radiat Res 177:109–116
Modi UJ, Nayak U, Aiyer S, Bharani S (1998) Study of malformation and Down syndrome in India (SOMDI): Baroda region. Indian J Hum Genet 4:93–98
Nair MK, Nambi KSV, Amma SN, Gangadharan P, Jayalekshmi P, Jayadevan S et al (1999) Population study in the high natural background radiation area in Kerala, India. Radiat Res 152(Suppl):S145–S148
Nair RRK, Rajan B, Akiba S, Jayalekshmi P, Nair MK, Gangadharan P et al (2009) Background radiation and cancer incidence in Kerala, India-Karunagapally cohort study. Health Phys 96(1):55–66
Neel JV, Schull WJ, Awa AA, Satoh C, Kato H, Otake M et al (1990) The children of parents exposed to atomic bombs: estimates of the genetic doubling dose of radiation for humans. Am J Hum Genet 46:1053–1072
Radhakrishna U, Ratnamala U, Gaines M, Beiraghi S, Hutchings D, Golla J et al (2006) Genomewide scan for nonsyndromic cleft lip and palate in multigenerational Indian families reveals significant evidence of Linkage at 13q33.1–34. Am J Hum Genet 79:580–585
Reddy SG, Reddy RR, Bronkhorst EM, Prasad R, Ettema AM, Sailer HF et al (2010) Incidence of cleft lip and palate in the state of Andhra Pradesh, South India. Indian J Plast Surg 43(2):184–189
Ronya R, Gupta D, Ghosh SK, Narang R, Jain KB (2002) Spectrum of congenital surgical malformations in newborns. J Indian Med Assoc 100(9):565–566
Seller MJ, Opitz JM (1987) Neural tube defects and sex ratios. Am J Med Genet 26(3):699–707
Singh M (1985) Early diagnosis of congenital malformations. In: Care of newborn. 3rd edn. Sagar Publications, New Delhi
StatSoft, Inc. (2010). STATISTICA (data analysis software system), version 9.1. www.statsoft.com.
Stoltenberg C, Magnus P, Lie RT, Daltveit AK, Irgens LM (1998) Influence of consanguinity and maternal education on risk of stillbirth and infant death in Norway, 1967–1993. Am J Epidemiol 148:452–459
Sundaram K (1977) Down's syndrome in Kerala [letter]. Nature 267:728
Sunta CM (1993) A review of the studies of high background areas of the S–W coast of India. In: Sohrabi M, Ahmed JU, Durani SA (eds) Proceedings of the international conference on high levels of natural radiation. Atomic Energy Organization of Iran, Tehran, p 71
Talukder G, Sharma A (2006) Genetic causes of congenital malformation in India. Int J Hum Genet 6(1):15–25
Thampi MV, Cheriyan VD, Kurien CJ, Ramachandran EN, Karuppasamy CV, Koya PKM et al (2002) Cytogenetic studies in the high level natural radiation areas of Kerala. Int Congress Ser 1225:207–211
Thampi MV, Cheriyan VD, Jaikrishan G, Das B, Kurien CJ, Ramachandran EN et al (2005) Investigations on the health effects of human population residing in the high-level natural radiation areas in Kerala in the southwest coast of India. Int Congr Ser 1276:8–12
United Nations Scientific Committee on the Effects of Atomic Radiation (1993) Report to the general assembly. I. Sources, effects and risks of ionizing radiation. United Nations, New York
United Nations Scientific Committee on the Effects of Atomic Radiation (2000) Report to the general assembly with scientific annexes. Vol I. Annex B: exposures from natural radiation sources. United Nations, New York
Verma IC, Anand NK, Kabra M, Menon PSN, Sharma N (1998) Study of malformation and Down syndrome in India (SOMDI): Delhi region. Indian J Hum Genet 4:84–87
Vogel F, Motulsky AG (1997) Human genetics—problems and approaches, 3rd edn. Springer, New York
World Health Organization (1959) Effects of radiation on human heredity: investigations of areas of high natural radiation. WHO Technical Report Series No. 166, Geneva
Acknowledgments
The co-operation and unfailing support of the medical, nursing, and paramedical staff of the Directorate of Health Services, Government of Kerala and the staff of the Ministry of Social Welfare is gratefully acknowledged. Without their dedication and hard work, these investigations would not have been possible. The contribution of Dr. PS Chauhan and Mr. MV Thampi at different stages of the study is also gratefully acknowledged. The authors also acknowledge the services of the cytogeneticists of the laboratory who did the karyotyping for cytological confirmation of suspected chromosomal anomalies including Down syndrome.
Conflict of interest
The authors declare that they have no conflict of interest.
Author information
Authors and Affiliations
Corresponding author
Appendix
Appendix
Rights and permissions
About this article
Cite this article
Jaikrishan, G., Sudheer, K.R., Andrews, V.J. et al. Study of stillbirth and major congenital anomaly among newborns in the high-level natural radiation areas of Kerala, India. J Community Genet 4, 21–31 (2013). https://doi.org/10.1007/s12687-012-0113-1
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12687-012-0113-1