Abstract
Background
Celiac disease (CD) is a lifelong condition with significant morbidity and requires an accurate diagnosis. Guidelines for pediatric CD were revised by the European and British Societies of Paediatric Gastroenterology Hepatology and Nutrition in 2012 and 2013, respectively. New recommendations introduced non-biopsy pathway (NBP) of diagnosis for a selective group of symptomatic children whose anti-tissue transglutaminase (anti-tTG) antibody titer is greater than ten times upper limit of normal. A clear understanding of the guidelines amongst consultant pediatricians will ensure all children with suspected CD receive a prompt and secure diagnosis. The aim of this study was to establish the interpretation and implementation of the revised guideline for CD amongst consultant general pediatricians in Southwest England (SWE) during the study period.
Methods
Telephone/email survey was conducted amongst consultant general pediatricians (n ≈ 140) working in 12 secondary care hospitals across SWE. The survey included eight questions incorporating three main themes: understanding of diagnostic pathway particularly for non-biopsy diagnosis, awareness of laboratory tests involved, and variations in practice in relation to the revised guidelines.
Results
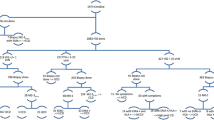
Responses were available from 101/140 (72%). One hundred respondents were aware of the revised guidelines for diagnosing CD. However, only 17 respondents stated all the criteria of the guideline required for diagnosis by NBP, with further 17 seeking immediate advice from a specialist. Forty-four listed both the criteria for HLA-DQ2/DQ8 testing applicable to pediatricians. Forty-nine out of 100 pediatricians would commence gluten-free diet only after all the results were available. Thirty-three pediatricians also considered asymptomatic children with high anti-tTG titer eligible for diagnosis of CD by NBP.
Conclusions
There is a need for improved understanding of revised CD guidelines amongst consultant general pediatricians especially while using the NBP and requesting HLA-DQ2/DQ8 testing.



Similar content being viewed by others
References
Husby S, Koletzko S, Korponay-Szabó IR, et al. European Society for Pediatric Gastroenterology, Hepatology, and Nutrition guidelines for the diagnosis of coeliac disease. J Pediatr Gastroenterol Nutr. 2012;54:136–60.
Bingley PJ, Williams AJ, Norcross AJ, et al. Undiagnosed coeliac disease at age seven: population based prospective birth cohort study. BMJ. 2004;328:322–3.
Mustalahti K, Catassi C, Reunanen A, et al. The prevalence of celiac disease in Europe: results of a centralized, international mass screening project. Ann Med. 2010;42:587–95.
Paul SP, Hoghton M, Sandhu B. Limited role of HLA DQ2/8 genotyping in diagnosing coeliac disease. Scott Med J. 2017;62:25–7.
Paul SP, Harries SL, Basude D. Barriers to implementing the revised ESPGHAN guidelines for coeliac disease in children: a cross sectional survey of coeliac screen reporting in laboratories in England. Arch Dis Child. 2017;102:942–6.
Murch S, Jenkins H, Auth M, et al. Joint BSPGHAN and Coeliac UK guidelines for the diagnosis and management of coeliac disease in children. Arch Dis Child. 2013;98:806–11.
Trovato CM, Montuori M, Anania C, et al. Are ESPGHAN “biopsy-sparing” guidelines for celiac disease also suitable for asymptomatic patients? Am J Gastroenterol. 2015;110:1485–9.
Paul SP, Sandhu BK, Spray CH, Basude D, Ramani P. Evidence supporting serology based pathway for diagnosing coeliac disease in asymptomatic children from high-risk groups. J Pediatr Gastroenterol Nutr. 2018;66:641–4.
Paul SP, Mazhar H, Spray CH. Applicability of the new ESPGHAN guidelines for diagnosing coeliac disease in children from resource limited countries. J Coll Physicians Surg Pak. 2015;25:455–7.
Al-Musawi ZM. Is high tissue transglutaminase antibody titers enough to diagnose coeliac disease in children? Karbala J Med. 2010;3:860–6.
Bhattacharya M, Lomash A, Sakhuja P, Dubey AP, Kapoor S. Clinical and histopathological correlation of duodenal biopsy with IgA anti-tissue transglutaminase titers in children with coeliac disease. Indian J Gastroenterol. 2014;33:350–4.
Paul SP, Kirkham EN. Celiac disease - a case series from North India: correspondence. Indian J Pediatr. 2016;83:760–1.
National Institute for Health and Care Excellence. Coeliac disease: recognition, assessment and management. NICE guidelines 20. London: NICE; 2015. Available at https://www.nice.org.uk/guidance/ng20. Accessed 21 Feb 2019.
Author information
Authors and Affiliations
Consortia
Contributions
All the authors have contributed equally to the manuscript.
Corresponding author
Ethics declarations
Competing interests
SPP, HLA, DB, and Collaborators declare that they have no competing interests.
Disclaimer
The authors are solely responsible for the data and the content of the paper. In no way, the Honorary Editor-in-Chief, Editorial Board Members, or the printer/publishers are responsible for the results/ findings and content of this article.
Collaborators
Alison Rushforth - Gloucestershire Royal Hospital, Gloucester
Christopher Knight - Musgrove Park Hospital, Taunton
Camelia Vaina - Yeovil District Hospital, Yeovil
Girish Gowda - Great Western Hospital, Swindon
James Hart - Royal Devon and Exeter Hospital, Exeter
Loh Ne-Ron - Royal United Hospital, Bath
Matthew Thorpe - Royal Cornwall Hospital, Truro
Rebecca Cordingley - North Devon District Hospital, Barnstaple
Samuel Broad - Derriford Hospital, Plymouth
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Paul, S.P., Adams, H.L., Basude, D. et al. Interpretation and implementation of the revised European Society for Paediatric Gastroenterology Hepatology and Nutrition (ESPGHAN) guidelines on pediatric celiac disease amongst consultant general pediatricians in Southwest of England. Indian J Gastroenterol 38, 203–210 (2019). https://doi.org/10.1007/s12664-019-00952-9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12664-019-00952-9