Abstract
Background
Behavioral treatment strategies improve adherence to lifestyle intervention for adults with obesity, but can be time and resource intensive when delivered via traditional face-to-face care. This study aimed to investigate the efficacy and optimal timing of using telephone calls and text message as adjunctive tools to support a community-based obesity management program.
Method
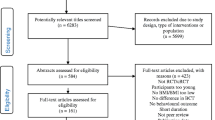
This 8-month randomized controlled crossover trial recruited 61 adults with class III obesity (BMI > 40 kg/m2) enrolled in a publicly funded obesity management service (OMS). Participants were randomly assigned to receive telephone and text message support in addition to standard OMS care, or standard OMS care alone. After 4 months, participants crossed over to the alternative sequence. The technological support was based on self-determination theory. Outcome measures included diet, physical activity, anthropometry, self-efficacy, and treatment self-regulation.
Results
Telephone and text message support improved lifestyle intervention adherence and clinical outcomes when compared with standard care. Participants who received the intervention in the first 4-month period lost 4.87 kg, compared with no weight loss (+ 0.38 kg) in the standard care only group. There was no evidence to indicate an optimal timing of the intervention, with both groups achieving significant results by the end of the intervention.
Conclusion
These results suggest a high degree of promise for the incorporation of telephone and text message support into community-based obesity management services. The findings have the potential to improve existing practices and reduce the burden on the health care system by demonstrating a resource-effective improvement to obesity management service delivery.




Similar content being viewed by others
References
Diabetes Prevention Program (DPP) Research Group. The Diabetes Prevention Program (DPP): description of lifestyle intervention. Diab Care. 2002;25(12):2165–71.
Look AHEAD Research Group. Reduction in weight and cardiovascular disease risk factors in individuals with type 2 diabetes. One-year results of the Look AHEAD trial. Diab Care. 2007;30(6):1374–83.
Gudzune KA, Doshi RS, Mehta AK, Chaudhry ZW, Jacobs DK, Vakil RM, et al. Efficacy of commercial weight loss programs: an updated systematic review. Ann Intern Med. 2015;162(7):501–12.
Eddy DM, Schlessinger L, Kahn R. Clinical outcomes and cost-effectiveness of strategies for managing people at high risk for diabetes. Ann Intern Med. 2005;143(4):251–64.
Pellegrini CA, Duncan JM, Moller AC, Buscemi J, Sularz A, DeMott A, et al. A smartphone-supported weight loss program: design of the ENGAGED randomized controlled trial. BMC Public Health. 2012;12(1):1041.
Markowitz JT, Harrington KR, Laffel LMB. Technology to optimize pediatric diabetes management and outcomes. Curr Diab Rep. 2013;13(6):877–85.
Ostojic V, Cvoriscec B, Ostojic SB, Reznikoff D, Stipic-Markovic A, Tudjman Z. Improving asthma control through telemedicine: a study of short-message service. Telemed J E Health. 2005;11(1):28–35.
Marquez CE, de la Figueroa von Wichmann M, Gil GV, Ella-Catala A, Figueras M, Balana M. Effectiveness of an intervention to provide information to patients with hypertension as short text messages and reminders sent to their mobile phone. Aten Primaria. 2004;15(34):399–405.
Fjeldsoe BS, Marshall AL, Miller YD. Behavior change interventions delivered by mobile telephone short-message service. Am J Prev Med. 2009;36(2):165–73.
Cole-Lewis H, Kershaw T. Text messaging as a tool for behavior change in disease prevention and management. Epidemiol Rev. 2010;32(1):56–69.
Reynolds NR, Testa MA, Su M, Chesney MA, Neidig JL, Frank I, et al. Telephone support to improve antiretroviral medication adherence: a multisite, randomized controlled trial. J Acquir Immune Defic Syndr. 2008;1(47):62–8.
Rodgers A, Corbett T, Bramley D, Riddell T, Wills M, Lin R-B, et al. Do u smoke after txt? Results of a randomised trial of smoking cessation using mobile phone text messaging. Tob Control. 2005;14(4):255–61.
Fischer HH, Fischer IP, Pereira RI, Furniss AL, Rozwadowski JM, Moore SL, et al. Text message support for weight loss in patients with prediabetes: a randomized clinical trial. Diabetes Care. 2016;39(8):1364–70.
Chow CK, Redfern J, Hillis GS, Thakkar J, Santo K, Hackett ML, et al. Effect of lifestyle-focused text messaging on risk factor modification in patients with coronary heart disease. A randomized clinical trial. J Am Med Assoc. 2015;314(12):1255–63.
Tang J, Abraham C, Greaves C, Yates T. Self-directed interventions to promote weight loss: a systematic review of reviews. J Med Internet Res. 2014;16(2):e58.
Butryn ML, Webb V, Wadden TA. Behavioral treatment of obesity. Psychiatr Clin North Am. 2011;34(4):841–59.
Fry JP, Neff RA. Periodic prompts and reminders in health promotion and health behavior interventions: systematic review. J Med Internet Res. 2009;11(2):e16.
Donaldson EL, Fallows S, Morris M. A text message based weight management intervention for overweight adults. J Hum Nutr Diet. 2014;27(Suppl 2):90–7.
Joo N, Kim BT. Mobile phone short message service messaging for behaviour modification in a community-based weight control programme in Korea. J Telemed Telecare. 2007;13(8):416–20.
Svetkey LP, Stevens VJ, Brantley PJ, Appel LJ, Hollis JF, Loria CM, et al. Weight loss maintenance collaborative research group. Comparison of strategies for sustaining weight loss. The weight loss maintenance randomized controlled trial. JAMA. 2008;299(10):1139–48.
Haapala I, Barengo NC, Biggs S, Surakka L, Manninen P. Weight loss by mobile phone: a 1-year effectiveness study. Public Health Nutr. 2009;12(12):2382–91.
Lombard DN, Lombard TN, Winett RA. Walking to meet health guidelines: the effect of prompting frequency and prompt structure. Health Psychol. 1995;14(2):164–70.
Hurling R, Catt M, De Boni M. Using internet and mobile phone technology to deliver an automated physical activity program: randomized controlled trial. J Med Internet Res. 2007;9(2):e7.
Boutelle KN, Kirschenbaum DS, Baker RC, Mitchell ME. How can obese weight controllers minimize weight gain during the high risk holiday season? By self-monitoring very consistently. Health Psychol. 1999;18(4):364–8.
Appel LJ, Clark JM, Yeh H-C, Wang N-Y, Coughlin JW, Daumit G, et al. Comparative effectiveness of weight-loss interventions in clinical practice. N Engl J Med. 2011;365(21):1959–68.
Patrick K, Raab F, Adams MA, Dillon L, Zabinski M, Rock CL, et al. A text message-based intervention for weight loss: randomized controlled trial. J Med Internet Res. 2009;11(1):e1.
Donnelly JE, Smith BK, Dunn L, Mayo MM, Jacobsen DJ, Stewart EE, et al. Comparison of a phone vs clinic approach to achieve 10% weight loss. Int J Obes. 2007;31(8):1270–6.
Digenio AG, Mancuso JP, Gerber RA, Dvorak RV. Comparison of methods for delivering a lifestyle modification program for obese patients: a randomized trial. Ann Intern Med. 2009;150(4):255–62.
Perri MG, Limacher MC, Durning PE, Janicke DM, Lutes LD, Bobroff LB, et al. Extended-care programs for weight management in rural communities. The treatment of obesity in underserved rural settings (TOURS) randomized trial. Arch Intern Med. 2008;168(21):2347–54.
Kodama S, Saito K, Tanaka S, Horikawa C, Fujiwara K, Hirasawa R, et al. Effect of web-based lifestyle modification on weight control: a meta-analysis. Int J Obes. 2012;36(5):675–85.
Siopis G, Chey T, Allman-Farinelli M. A systematic review and meta-analysis of interventions for weight management using text messaging. J Hum Nutr Diet. 2015;28(Suppl. 2):1–15.
Zwickert K, Rieger E, Swinbourne J, Manns C, McAulay C, Gibson A, et al. High or low intensity text-messaging combined with group treatment equally promote weight loss maintenance in obese adults. Obes Res Clin Pract. 2016;10(6):680–91.
Silva MN, Vieira PN, Coutinho SR, Minderico CS, Matos MG, Sardinha LB, et al. Using self-determination theory to promote physical activity and weight control: a randomized controlled trial in women. J Behav Med. 2010;33(2):110–22.
Burgess E, Hassmen P, Walvaert M, Pumpa KL. Behavioural treatment strategies improve adherence to lifestyle intervention programmes in adults with obesity: a systematic review and meta-analysis. Clin Obes. 2017;7(2):105–14.
Dijkstra A, De Vries H. The development of computer-generated tailored interventions. Patient Educ Couns. 1999;36(2):193–203.
Ryan P, Lauver DR. The efficacy of tailored interventions. J Nurs Scholarsh. 2002;34(4):331–7.
Fjeldsoe BS, Miller YD, Marshall AL. MobileMums: a randomized controlled trial of an SMS-based physical activity intervention. Ann Behav Med. 2010;39(2):101–11.
Park S-H, Hwang J, Choi Y-K. Effect of mobile health on obese adults: a systematic review and meta-analyis. Healthc Inform Res. 2019;25(1):12–26.
Antoine Parker C, Ellis C. Effect of electronic messaging on physical activity participation among older adults. J Aging Res. 2016; 6171028.
Rieger E, Dean HY, Steinbeck KS, Caterson ID, Manson E. The use of motivational enhancement strategies for the maintenance of weightloss among obese individuals: a preliminary investigation. Diabetes Obes Metab. 2009;11:637–40.
Reeves MM, Winkler EAH, Eakin EG. Fat and fibre behaviour questionnaire: reliability, relative validity and responsiveness to change in Australian adults with type 2 diabetes and/or hypertension. Nutr Diet. 2015;72(4):368–76.
Whelan ME, Winkler EAH, Eakin EG, Reeves MM. Relative validity of a brief Fat and Fibre Behaviour Questionnaire in a population of overweight and obese breast cancer survivors: a note of caution. Nutr Diet. 2017;74(1):18–28.
Brazeau AS, Karelis AD, Mignault D, Lacroix MJ, Prud'homme D, Rabasa-Lhoret R. Test-retest reliability of a portable monitor to assess energy expenditure. Appl Physiol Nutr Metab. 2011;3(36):339–43.
World Health Organization (WHO). Physical status: the use and interpretation of anthropometry. Report of a WHO Expert Committee. Technical Report Series No. 854. Geneva, Switzerland; 1995.
Ames GE, Heckman MG, Diehl NN, Grothe KB, Clark MM. Further statistical and clinical validity for the Weight Efficacy Lifestyle Questionnaire-Short Form. Eat Behav. 2015;18:115–9.
Ames GE, Heckman MG, Grothe KB, Clark MM. Eating self-efficacy: development of a short-form WEL. Eat Behav. 2012;13(4):375–8.
Haas BK, Norham S. Measuring self efficacy: Development of the physical activity assessment inventory. South Online J Nurs Res. 2010;10(4).
Deci EL, Ryan RM. Intrinsic motivation and self-determination in human behavior. New York: NY: Plenum Publishing Co; 1985.
Williams GC, Ryan RM, Deci EL. Health-care, self-determination theory packet 2017 [cited 29 March 2017]. Available from: http://selfdeterminationtheory.org/questionnaires/.
R Core Team. R: A language and environment for statistical computing. R foundation for statistical computing Vienna, Austria2016 [cited 2nd October 2018]. Available from: https://www.R-project.org/.
Bates D, Maechler M, Bolker B, Walker S. Fitting linear mixed-effects models using lme4. J Stat Softw. 2015;67(1):1–48.
Wang T, Malone J, Fu H, Heilmann C, Qu Y, Huster WJ. Crossover design and its application in late-phase diabetes studies. J Diabetes. 2016;8(5):610–8.
Fox J, Weisberg S. An R companion to applied regression, second edition. Thousand Oaks, California: SAGE; 2011.
Burgess E, Hassmen P, Pumpa KL. Determinants of adherence to lifestyle intervention in adults with obesity: a systematic review. Clin Obes. 2017;7(3):123–35.
World Health Organization. Controlling the global obesity epidemic 2018 [cited 24 October 2018]. Available from: http://www.who.int/nutrition/topics/obesity/en/.
Australian Government. Australian Institute for Health and Welfare (AIHW). An interactive insight into overweight and obesity in Australia. Cat. no. WEB 236 2017 [cited 24 October 2018]. Available from: https://www.aihw.gov.au/reports/overweight-obesity/interactive-insight-into-overweight-and-obesity/contents/how-many-people-are-overweight-or-obese.
Naslund JA, Aschbrenner KA, Scherer EA, Pratt SI, Wolfe RS, Bartels SJ. Lifestyle intervention for people with severe obesity and serious mental illness. Am J Prev Med. 2016;50(2):145–53.
Annesi JJ, Whitaker A. Psychological factors associated with weight loss in obese and severely obese women in a behavioral physical activity intervention. Health Educ Behav. 2009;37(4):593–606.
Hofso D, Jenssen T, Bollerslev J, Ueland T, Godang K, Stumvoll M, et al. Beta cell function after weight loss: a clinical trial comparing gastric bypass surgery and intensive lifestyle intervention. Eur J Endocrinol. 2011;164(2):231–8.
Annesi JJ, Gorjala S. Changes in theory-based psychological factors predict weight loss in women with class III obesity initiating supported exercise. J Obes. 2010; 171957.
Annesi JJ. Relations of mood with body mass index changes in severely obese women enrolled in a supported physical activity treatment. Obes Facts. 2008;1:88–92.
Malone M, Alger-Mayer S, Lindstrom J. Use of orlistat 60 mg in the management of weight loss before bariatric surgery. Ann Pharmacother. 2012;46(6):779–84.
Neve M, Morgan PJ, Jones PR, Collins CE. Effectiveness of web-based interventions in achieving weight loss and weight loss maintenance in overweight and obese adults: a systematic review with meta-analysis. Obes Rev. 2010;11(4):306–21.
Rothman AJ, Salovey P, Antone C, Keough K, Martin CD. The influence of message framing on intentions to perform health behaviors. J Exp Soc Psychol. 1993;29(5):408–33.
Acknowledgments
Thank you to all of the participants who gave up their time to participate in this study; your support of this important research is greatly appreciated.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of Interest
The authors declare that they have no conflict of interest.
Ethical Approval
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Lewis, E., Huang, HC.C., Hassmén, P. et al. Adding Telephone and Text Support to an Obesity Management Program Improves Behavioral Adherence and Clinical Outcomes. A Randomized Controlled Crossover Trial. Int.J. Behav. Med. 26, 580–590 (2019). https://doi.org/10.1007/s12529-019-09815-1
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12529-019-09815-1