Abstract
Exposure to certain arsenic (As) species has been associated with increased cancer risk and a wide range of other health concerns, even at low levels. Here we used urine as a biomarker of As internal dose in a well-characterized cohort to relate diet, demographics and geography to exposure. As speciation in spot urine samples was determined for 89 participants aged ≥ 50 years from the Northern Ireland Cohort for the Longitudinal Study of Ageing (NICOLA), stratified to cover the country. Principal component analysis showed that all As species clustered together, suggesting that arsenobetaine, inorganic As (iAs) and the methylated species monomethylarsonic acid and dimethylarsinic acid forms have a common source. Seafood and alcohol consumption were positively correlated with As species, while dairy products (i.e. milk) and tap water were negatively correlated. Multiple regression analysis showed that diet explained approximately 30% of the variability in urinary iAs concentrations. Geography was not found to be a predictor of As exposure. Dairy consumption was negatively correlated and the best predictor of iAs in urine, explaining 15.9% of the variability. The majority of the variation in As biomarkers was not explained, suggesting the contribution of other sources and other non-predicted variables on As metabolism and elimination.

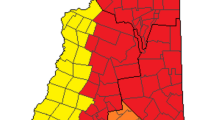
copyright and database rights 2016. Compiled using QGIS, version 3.2.3


Similar content being viewed by others
References
C.E.U. Council Directive 98/83/EC of November 1998 on the quality of water intended for human consumption. Official Journal European Community, May 12, 1998, pp L330/32–L330/52. https://eur-lex.europa.eu/legal-content/EN/TXT/PDF/?uri=CELEX:01998L0083-20151027&from=EN. Accessed 20 May 2019
Chappell WR, Abernathy CO, Calderon RL, Thomas DJ (2003) In: Chappell WR, Abernathy CO, Calderon RL, Thomas DJ (eds) Arsenic exposure and health effects V, 1st edn. Elsevier, Amsterdam, pp 3–103
Davis MA, Gilbert-Diamond D, Karagas MR, Li Z, Moore JH, Williams SM, Frost HR (2014) A dietary-wide association study (DWAS) of environmental metal exposure in US children and adults. PLoS ONE 9:e104768. https://doi.org/10.1371/journal.pone.0104768
Davis MA, Signes-Pastor AJ, Argos M, Slaughter F, Pendergrast C, Punshon T, Gossai A, Ahsan H, Karagas MR (2017) Assessment of human dietary exposure to arsenic through rice. Sci Total Environ 586:1237–1244. https://doi.org/10.1016/j.scitotenv.2017.02.119
Diaz OP, Arcos R, Tapia Y, Pastene R, Velez D, Devesa V, Montoro R, Aguilera V, Becerra M (2015) Estimation of arsenic intake from drinking water and food (raw and cooked) in a rural village of northern Chile. Urine as a biomarker of recent exposure. Int J Environ Res Public Health 12:5614–5633. https://doi.org/10.3390/ijerph120505614
Gamble MV, Liu X, Ahsan H, Pilsner JR, Ilievski V, Slavkovich V, Parvez F, Chen Y, Levy D, Factor-Litvak P, Graziano JH (2006) Folate and arsenic metabolism: a double-blind, placebo-controlled folic acid-supplementation trial in Bangladesh. Am J Clin Nutr 84:1093–1101. https://doi.org/10.1093/ajcn/84.5.1093
Geological Survey Northern Ireland, GSNI (2007) Tellus project overview. https://www.bgs.ac.uk/data/home.html?src=topNav. Accessed on 25 Sep 2018
Gribble MO, Voruganti VS, Cole SA, Haack K, Balakrishnan P, Laston SL, Tellez-Plaza M, Francesconi KA, Goessler W, Thomas DC, Gilliland F, North KE, Franceschini N, Navas-Acien A, (2015) Linkage analysis of urine arsenic species patterns in the strong heart family study. Toxicol Sci 148:89–100. https://doi.org/10.1093/toxsci/kfv164
Harrington KE, McGowan MJ, Kiely M, Robson PJ, Livingstone MB, Morrissey PA, Gibney MJ (2001) Macronutrient intakes and food sources in Irish adults: findings of the North/South Ireland Food Consumption Survey. Public Health Nutr 5A:1051–1060
Hilmer SN (2008) ADME-tox issues for the elderly. Expert Opin Drug Metab Toxicol 4:1321–1331. https://doi.org/10.1517/17425255.4.10.1321
Hopenhayn-Rich C, Biggs ML, Smith AH, Kalman DA, Moore LE (1996) Methylation study of a population environmentally exposed to arsenic in drinking water. Environ Health Perspect 104:620–628. https://doi.org/10.1289/ehp.96104620
Huang YK, Huang YL, Hsueh YM, Yang MH, Wu MM, Chen SY, Hsu LI, Chen CJ (2008) Arsenic exposure, urinary arsenic speciation, and the incidence of urothelial carcinoma: a twelve-year follow-up study. Cancer Causes Control 19:829–839. https://doi.org/10.1007/s10552-008-9146-5
Hudgens EE, Drobna Z, He B, Le XC, Styblo M, Rogers J, Thomas DJ (2016) Biological and behavioral factors modify urinary arsenic metabolic profiles in a U.S. population. Environ Health 15:62. https://doi.org/10.1186/s12940-016-0144-x.
IARC (2004) Monographs on the evaluation of carcinogenic risk to humans. Some drinking-water disinfectants and contaminants, including arsenic, vol 84. World Health Organization, Lyon
IARC (2012) Arsenic, metals, fibres and dust. Volume 100C. A review of human carcinogens. IARC monographs on the evaluation of carcinogenic risk to humans. World Health Organization, Lyon
Jackson BP, Taylor VF, Punshon T, Cottingham KL (2012) Arsenic concentration and speciation in infant formulas and first foods. Pure Appl Chem 84:215–223. https://doi.org/10.1351/PAC-CON-11-09-17
Jackson CE, McKinley JM, Ofterdinger U, Fogarty D, Atkinson PM, Palmer S (2016) Investigating relations between environmental toxins in Northern Irish soils and streams and Chronic Kidney Disease prevalence. Appl Geochem 75:236–246. https://doi.org/10.1016/j.apgeochem.2016.10.016
Jones MR, Tellez-Plaza M, Vaidya D, Grau M, Francesconi KA, Goessler W, Guallar E, Post WS, Kaufman JD, Navas-Acien A (2016) Estimation of inorganic arsenic exposure in populations with frequent seafood intake: evidence from MESA and NHANES. Am J Epidemiol 184:590–602. https://doi.org/10.1093/aje/kww097
Kordas K, Queirolo EI, Mañay N, Peregalli F, Hsiao PY, Lu Y, Vahter M (2016) Low-level arsenic exposure: nutritional and dietary predictors in first-grade Uruguayan children. Environ Res 147:16–23. https://doi.org/10.1016/j.envres.2016.01.022
Kurzius-Spencer M, da Silva V, Thomson CA, Hartz V, Hsu CH, Burgess JL, O’Rourke MK, Harris RB (2017) Nutrients in one-carbon metabolism and urinary arsenic methylation in the National Health and Nutrition Examination Survey (NHANES) 2003–2004. Sci Total Environ 607–608:381–390. https://doi.org/10.1016/j.scitotenv.2017.07.019
Lindberg AL, Ekström EC, Nermell B, Rahman M, Lönnerdal B, Persson LA, Vahter M (2008) Gender and age differences in the metabolism of inorganic arsenic in a highly exposed population in Bangladesh. Environ Res 106:110–120. https://doi.org/10.1016/j.envres.2007.08.011
McKinley JM, Ofterdinger U, Young M, Barsby A, Gavin A (2013) Investigating local relationships between trace elements in soils and cancer data. Spat Stat 5:25–41. https://doi.org/10.1016/j.spasta.2013.05.001
Meharg AA, Raab A (2010) Getting to the bottom of arsenic standards and guidelines. Environ Sci Technol 44:4395–4399. https://doi.org/10.1021/es9034304
Middleton DR, Watts MJ, Lark RM, Milne CJ, Polya DA (2016) Assessing urinary flow rate, creatinine, osmolality and other hydration adjustment methods for urinary biomonitoring using NHANES arsenic, iodine, lead and cadmium data. Environ Health 15:68. https://doi.org/10.1186/s12940-016-0152-x
Mori M, Sato T, Yoshida HY, Ohira Y, Itou Y, Shimizu S (2016) Association of beer consumption with arsenic concentration in urine: a result from a cross-sectional study of the general Japanese population. Environ Health Prev Med 21:327–333. https://doi.org/10.1007/s12199-016-0533-3
Navas-Acien A, Francesconi KA, Silbergeld EK, Guallar E (2011) Seafood intake and urine concentrations of total arsenic, dimethylarsinate and arsenobetaine in the US population. Environ Res 111:110–118. https://doi.org/10.1016/j.envres.2010.10.009
Navoni JA, De Pietri D, Olmos V, Gimenez C, Bovi Mitre G, de Titto E, Villaamil Lepori EC (2014) Human health risk assessment with spatial analysis: study of a population chronically exposed to arsenic through drinking water from Argentina. Sci Total Environ 499:166–174. https://doi.org/10.1016/j.scitotenv.2014.08.058
Neville CE, Cruise SM, Burns F (2019) The Northern Ireland Cohort for the Longitudinal Study of Ageing (NICOLA). In: Encyclopedia of gerontology and geriatrics. Springer, Cham. https://doi.org/10.1007/978-3-319-69892-2_346-1
Nutritics (2018) Research Edition (v5.02) (computer software). Nutritics, Dublin. www.nutritics.com. Accessed 4 Feb 2019
Ouypornkochagorn S, Feldmann J (2010) Dermal uptake of arsenic through human skin depends strongly on its speciation. Environ Sci Technol 44:3972–3978. https://doi.org/10.1021/es903667y
Pang Y, Peng RD, Jones MR, Francesconi KA, Goessler W, Howard BV, Umans JG, Best LG, Guallar E, Post WS, Kaufman JD, Vaidya D, Navas-Acien A (2016) Metal mixtures in urban and rural populations in the US: the Multi-Ethnic Study of Atherosclerosis and the Strong Heart Study. Environ Res 147:356–364. https://doi.org/10.1016/j.envres.2016.02.032
Popowich A, Zhang Q, Le XC (2016) Arsenobetaine: the ongoing mystery. Natl Sci Rev 3:451–458. https://doi.org/10.1093/nsr/nww061
Punshon T, Carey AM, Ricachenevsky FK, Meharg AA (2018) Elemental distribution in developing rice grains and the effect of flag-leaf arsenate exposure. Environ Exp Bot 149:51–58. https://doi.org/10.1016/j.envexpbot.2018.02.007
Saoudi A, Zeghnoun A, Bidondo ML, Garnier R, Cirimele V, Persoons R, Fréry N (2012) Urinary arsenic levels in the French adult population: the French National Nutrition and Health Study, 2006–2007. Sci Total Environ 433:206–215. https://doi.org/10.1016/j.scitotenv.2012.06.053
Shen H, Niu Q, Xu M, Rui D, Xu S, Feng G, Ding Y, Li S, Jing M (2016) Factors affecting arsenic methylation in arsenic-exposed humans: a systematic review and meta-analysis. Int J Environ Res Public Health 13:205. https://doi.org/10.3390/ijerph13020205
Shi G, Chen Z, Teng J, Bi C, Zhou D, Sun C, Li Y, Xu S (2012) Fluxes, variability and sources of cadmium, lead, arsenic and mercury in dry atmospheric depositions in urban, suburban and rural areas. Environ Res 113:28–32. https://doi.org/10.1016/j.envres.2012.01.001
Signes-Pastor AJ, Carey M, Vioque J, Navarrete-Muñoz EM, Rodríguez-Dehli C, Tardón A, Begoña-Zubero M, Santa-Marina L, Vrijheid M, Casas M, Llop S, Gonzalez-Palacios S, Meharg AA (2017a) Urinary arsenic speciation in children and pregnant women from Spain. Expo Health 9:105–111. https://doi.org/10.1007/s12403-016-0225-7
Signes-Pastor AJ, Vioque J, Navarrete-Muñoz EM, Carey M, García de la Hera MG, Sunyer J, Casas M, Riaño-Galán I, Tardón A, Llop S, Amorós R, Amiano P, Bilbao JR, Karagas MR, Meharg AA (2017b) Concentrations of urinary arsenic species in relation to rice and seafood consumption among children living in Spain. Environ Res 159:69–75. https://doi.org/10.1016/j.envres.2017.07.046
Signes-Pastor AJ, Woodside JV, McMullan P, Mullan K, Carey M, Karagas MR, Meharg AA (2017c) Levels of infants’ urinary arsenic metabolites related to formula feeding and weaning with rice products exceeding the EU inorganic arsenic standard. PLoS ONE 12:e0176923. https://doi.org/10.1371/journal.pone.0176923
Strosnider H, Kennedy C, Monti M, Yip F (2017) Rural and urban differences in air quality, 2008–2012, and community drinking water quality, 2010–2015: United States. MMWR Surveill Summ 66:1–10. https://doi.org/10.15585/mmwr.ss6613a1
Subhani M, Mustafa I, Alamdar A, Katsoyiannis IA, Ali N, Huang Q, Peng S, Shen H, Eqani SA (2015) Arsenic levels from different land-use settings in Pakistan: bio-accumulation and estimation of potential human health risk via dust exposure. Ecotoxicol Environ Saf 115:187–194. https://doi.org/10.1016/j.ecoenv.2015.02.019
Sugár E, Tatár E, Záray G, Mihucz VG (2013) Relationship between arsenic content of food and water applied for food processing. Food Chem Toxicol 62:601–608. https://doi.org/10.1016/j.fct.2013.09.028
Tseng CH, Huang YK, Huang YL, Chung CJ, Yang MH, Chen CJ, Hsueh YM (2005) Arsenic exposure, urinary arsenic speciation, and peripheral vascular disease in blackfoot disease-hyperendemic villages in Taiwan. Toxicol Appl Pharmacol 206:299–308. https://doi.org/10.1016/j.taap.2004.11.022
Wardrop NA, Le Blond JS (2015) Assessing correlations between geological hazards and health outcomes: addressing complexity in medical geology. Environ Int 84:90–93. https://doi.org/10.1016/j.envint.2015.07.016
Wei Y, Zhu J, Nguyen A (2014) Rice consumption and urinary concentrations of arsenic in US adults. Int J Environ Health Res 24:459–470. https://doi.org/10.1080/09603123.2013.857393
WHO (2001) Environmental Health Criteria 224—arsenic and arsenic compounds. International Program on Chemical Safety, Geneva
Wilding S, Martin D, Moon G (2018) Place and preference effects on the association between mental health and internal migration within Great Britain. Health Place 52:180–187. https://doi.org/10.1016/j.healthplace.2018.06.008
Williams PN, Islam MR, Adomako EE, Raab A, Hossain SA, Zhu YG, Feldmann J, Meharg AA (2006) Increase in rice grain arsenic for regions of Bangladesh irrigating paddies with elevated arsenic in groundwaters. Environ Sci Technol 40:4903–4908. https://doi.org/10.1021/es060222i
Wu F, Chi L, Ru H, Parvez F, Slavkovich V, Eunus M, Ahmed A, Islam T, Rakibuz-Zaman M, Hasan R, Sarwar G, Graziano JH, Ahsan H, Lu K, Chen Y (2018) Arsenic exposure from drinking water and urinary metabolomics: associations and long-term reproducibility in Bangladesh adults. Environ Health Perspect 126:017005. https://doi.org/10.1289/EHP1992
Xu S, Zheng N, Liu J, Wang Y, Chang S (2013) Geochemistry and health risk assessment of arsenic exposure to street dust in the zinc smelting district, Northeast China. Environ Geochem Health 35:89–99. https://doi.org/10.1007/s10653-012-9463-1
Zailina H, Najibah H, Aiezzati AN, Praveena SM, Patimah I (2014) Comparison of the health implications on the use of As and Cd contaminated water supply between urban and rural communities. Biomed Res Int 2014:797603. https://doi.org/10.1155/2014/797603
Zhang X, Wang B, Cui X, Lin C, Liu X, Ma J (2018) Total arsenic concentrations in Chinese children’s urine by different geographic locations, ages, and genders. Environ Geochem Health 40:1027–1036. https://doi.org/10.1007/s10653-017-9963-0
Acknowledgements
We are grateful to all the participants of the NICOLA, and the whole NICOLA Team, which includes nursing staff, research scientists, clerical staff, computer and laboratory technicians, managers and receptionists. The Atlantic Philanthropies, the Economic and Social Research Council, the UKCRC Centre of Excellence for Public Health Northern Ireland, the Centre for Ageing Research and Development in Ireland, the Office of the First Minister and Deputy First Minister, the Health and Social Care Research and Development Division of the Public Health Agency, the Wellcome Trust/Wolfson Foundation and Queen’s University Belfast provide core financial support for NICOLA. The authors alone are responsible for the interpretation of the data and any views or opinions presented are solely those of the authors and do not necessarily represent those of the NICOLA Study Team.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
All authors declare that there is no conflict of interest.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
de Moraes, N.V., Carey, M., Neville, C.E. et al. Water Dilutes and Alcohol Concentrates Urinary Arsenic Species When Food is the Dominant Source of Exposure. Expo Health 12, 699–710 (2020). https://doi.org/10.1007/s12403-019-00329-5
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12403-019-00329-5