Abstract
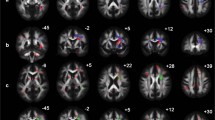
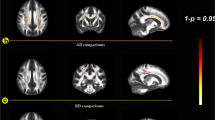
The purpose of this study is to investigate chemotherapy-related cognitive impairment (CRCI) in breast cancer patients, analyze absolute concentration and structural changes of metabolites in different brain regions by multimodal neuroimaging technology, and explore correlation between them. Breast cancer patients with chemotherapy treatment group (Ctx+, N = 24) and control group without treatment (Ctx–, N = 20) underwent neuropsychological tests, multivoxel magnetic resonance spectroscopy (MRS), and diffusion tensor imaging (DTI) before and after chemotherapy. Regions of interest (ROls) in magnetic resonance scan include bilateral posterior cingulate gyrus (PCG), bilateral dorsal thalamus (DT), bilateral lenticular nucleus (LN), bilateral posterior horn of the lateral ventricle paratrigonal white matter (PWM). In MRS, absolute concentrations of N-acetylaspartate (NAA), myo-inositol (MI), choline-containing compounds (Cho), total creatine (tCr), glutamine + glutamate (Glx) were quantified using LC Model and SAGE software. In DTI, we used fractional anisotropy (FA) and mean diffusivity (MD) to reflect white matter integrity. In Ctx+ patients, scores of functional assessment of cancer treatment cognition test (FACT-Cog), perceived cognitive impairments (PCI), impact of perceived impairments on quality of life (QOL), perceived cognitive abilities (PCA), auditory-verbal learning test (AVLT) recognition and clock drawing test (CDT) were lower than those before chemotherapy (p < 0.05). In MRS, Ctx+ patients had significantly lower NAA values in bilateral PCG, DT, respectively. The concentrations of tCr were observed to decline in bilateral PCG and right DT. Glx values decreased in right DT. Cho values decreased significantly in bilateral DT. In DTI, Ctx+ patients had lower FA values in bilateral PCG compared with patients before chemotherapy. Among imaging metrics and cognitive scores, positive correlations were observed between changes in AVLT recognition scores and changes in NAA values in bilateral PCG (left PCG: r = 0.470, p < 0.01; right PCG: r = 0.500, p < 0.01). Positive correlations were also found between changes in AVLT recognition and changes in FA values in bilateral PCG (left PCG: r = 0.513, p < 0.01; right PCG: r = 0.563, p < 0.01). Chemotherapy can lead to a decrease in memory function, accompanied by changes in brain metabolite concentration and white matter integrity in some parts of brain.



Similar content being viewed by others
References
Anderson-Hanley C, Sherman ML, Riggs R, Agocha VB, Compas BE. Neuropsychological effects of treatments for adults with cancer: a meta-analysis and review of the literature. J Int Neuropsychol Soc. 2003;9:967–82.
Stewart A, Bielajew C, Collins B, Parkinson M, Tomiak E. A meta-analysis of the neuropsychological effects of adjuvant chemotherapy treatment in women treated for breast cancer. Clin Neuropsychol. 2006;20:76–89.
Correa DD, Ahles TA. Neurocognitive changes in cancer survivors. Cancer J. 2008;14:396–400.
Aas M, Djurovic S, Ueland T, Morch RH, Laskemoen JF, Reponen EJ, et al. The relationship between physical activity, clinical and cognitive characteristics and BDNF mRNA levels in patients with severe mental disorders. World J Biol Psychiatry. 2019;20(7):567–76.
Lawrence JA, Griffin L, Balcueva EP, Groteluschen DL, Samuel TA, Lesser GJ, Naughton MJ, et al. A study of donepezil in female breast cancer survivors with self-reported cognitive dysfunction 1 to 5 years following adjuvant chemotherapy. J Cancer Surviv. 2016;10:176–84.
Ahles TA, Saykin AJ. Candidate mechanisms for chemotherapy-induced cognitive changes. Nat Rev Cancer. 2007;7:192–201.
Cascella M, Di Napoli R, Carbone D, Cuomo GF, Bimonte S, Muzio MR. Chemotherapy-related cognitive impairment: mechanisms, clinical features and research perspectives. Recenti Prog Med. 2018;109:523–30.
Billiet T, Emsell L, Vandenbulcke M, Peeters R, Christiaens D, Leemans A, et al. Recovery from chemotherapy-induced white matter changes in young breast cancer survivors? Brain Imaging Behav. 2018;12:64–77.
Menning S, de Ruiter MB, Veltman DJ, Boogerd W, Oldenburg H, Reneman L, et al. Changes in brain white matter integrity after systemic treatment for breast cancer: a prospective longitudinal study. Brain Imaging Behav. 2018;12:324–34.
Perrier J, Viard A, Levy C, Morel N, Allouache D, Noal S, et al. Longitudinal investigation of cognitive deficits in breast cancer patients and their gray matter correlates: impact of education level. Brain Imaging Behav. 2020;14(1):226–41.
Kesler SR, Rao A, Blayney DW, Oakley-Girvan IA, Karuturi M, Palesh O. Predicting long-term cognitive outcome following breast cancer with pre-treatment resting state fMRI and random forest machine learning. Front Hum Neurosci. 2017;11:555.
Slowik AJ, Jablonski MJ, Michalowska-Kaczmarczyk AM, Jach R. Evaluation of quality of life in women with breast cancer, with particular emphasis on sexual satisfaction, future perspectives and body image, depending on the method of surgery. Psychiatr Pol. 2017;51:871–88.
Xuan H, Gan C, Li W, Huang Z, Wang L, Jia Q, et al. Altered network efficiency of functional brain networks in patients with breast cancer after chemotherapy. Oncotarget. 2017;8:105648–61.
Dumas JA, Makarewicz J, Schaubhut GJ, Devins R, Albert K, Dittus K, et al. Chemotherapy altered brain functional connectivity in women with breast cancer: a pilot study. Brain Imaging Behav. 2013;7:524–32.
Kesler SR, Watson C, Koovakkattu D, Lee C, O'Hara R, Mahaffey ML, et al. Elevated prefrontal myo-inositol and choline following breast cancer chemotherapy. Brain Imaging Behav. 2013;7:501–10.
Kesler S, Janelsins M, Koovakkattu D, Palesh O, Mustian K, Morrow G, et al. Reduced hippocampal volume and verbal memory performance associated with interleukin-6 and tumor necrosis factor-alpha levels in chemotherapy-treated breast cancer survivors. Brain Behav Immun. 2013;30(Suppl):S109–S116116.
McDonald BC, Conroy SK, Smith DJ, West JD, Saykin AJ. Frontal gray matter reduction after breast cancer chemotherapy and association with executive symptoms: a replication and extension study. Brain Behav Immun. 2013;30(Suppl):S117–S12525.
Brown MS, Stemmer SM, Simon JH, Stears JC, Jones RB, Cagnoni PJ, et al. White matter disease induced by high-dose chemotherapy: longitudinal study with MR imaging and proton spectroscopy. AJNR Am J Neuroradiol. 1998;19:217–21.
de Ruiter MB, Reneman L, Boogerd W, Veltman DJ, Caan M, Douaud G, Lavini C, et al. Late effects of high-dose adjuvant chemotherapy on white and gray matter in breast cancer survivors: converging results from multimodal magnetic resonance imaging. Hum Brain Mapp. 2012;33:2971–83.
Deprez S, Amant F, Smeets A, Peeters R, Leemans A, Van Hecke W, et al. Longitudinal assessment of chemotherapy-induced structural changes in cerebral white matter and its correlation with impaired cognitive functioning. J Clin Oncol. 2012;30:274–81.
Abraham J, Haut MW, Moran MT, Filburn S, Lemiuex S, Kuwabara H. Adjuvant chemotherapy for breast cancer: effects on cerebral white matter seen in diffusion tensor imaging. Clin Breast Cancer. 2008;8:88–91.
Deprez S, Amant F, Yigit R, Porke K, Verhoeven J, Van den Stock J, et al. Chemotherapy-induced structural changes in cerebral white matter and its correlation with impaired cognitive functioning in breast cancer patients. Hum Brain Mapp. 2011;32:480–93.
Koppelmans V, Vernooij MW, Boogerd W, Seynaeve C, Ikram MA, Breteler MM, et al. Prevalence of cerebral small-vessel disease in long-term breast cancer survivors exposed to both adjuvant radiotherapy and chemotherapy. J Clin Oncol. 2015;33:588–93.
Cerulla N, Arcusa A, Navarro JB, de la Osa N, Garolera M, Enero C, Chico G, et al. Cognitive impairment following chemotherapy for breast cancer: the impact of practice effect on results. J Clin Exp Neuropsychol. 2019;41(3):290–99.
Pendergrass JC, Targum SD, Harrison JE. Cognitive impairment associated with cancer: a brief review. Innov Clin Neurosci. 2018;15:36–44.
Ren X, Boriero D, Chaiswing L, Bondada S, St Clair DK, Butterfield DA. Plausible biochemical mechanisms of chemotherapy-induced cognitive impairment (“chemobrain”), a condition that significantly impairs the quality of life of many cancer survivors. Biochim Biophys Acta Mol Basis Dis. 2019;1865(6):1088–97.
Khan OF, Cusano E, Raissouni S, Pabia M, Haeseker J, Bosma N, et al. Immediate-term cognitive impairment following intravenous (IV) chemotherapy: a prospective pre-post design study. BMC Cancer. 2019;19:150.
Wagner LI, Berg SR, Gandhi M, Hlubocky FJ, Webster K, Aneja M, et al. The development of a functional assessment of cancer therapy (FACT) questionnaire to assess dermatologic symptoms associated with epidermal growth factor receptor inhibitors (FACT-EGFRI-18). Support Care Cancer. 2013;21:1033–41.
Cheung YT, Lim SR, Shwe M, Tan YP, Chan A. Psychometric properties and measurement equivalence of the English and Chinese versions of the functional assessment of cancer therapy-cognitive in Asian patients with breast cancer. Value Health. 2013;16:1001–133.
van der Willik KD, Koppelmans V, Hauptmann M, Compter A, Ikram MA, Schagen SB. Inflammation markers and cognitive performance in breast cancer survivors 20 years after completion of chemotherapy: a cohort study. Breast Cancer Res. 2018;20:135.
Vardy JL, Dhillon HM, Pond GR, Renton C, Clarke SJ, Tannock IF. Prognostic indices of inflammatory markers, cognitive function and fatigue for survival in patients with localised colorectal cancer. ESMO Open. 2018;3:e000302.
Vega JN, Dumas J, Newhouse PA. Self-reported chemotherapy-related cognitive impairment compared with cognitive complaints following menopause. Psychooncology. 2018;27:2198–205.
Stanley JA, Raz N. Functional magnetic resonance spectroscopy: the "New" MRS for cognitive neuroscience and psychiatry research. Front Psychiatry. 2018;9:76.
Henigsberg N, Sarac H, Rados M, Rados M, Ozretic D, Foro T, et al. Lower choline-containing metabolites/creatine (Cr) rise and failure to sustain NAA/Cr levels in the dorsolateral prefrontal cortex are associated with depressive episode recurrence under maintenance therapy: a proton magnetic resonance spectroscopy retrospective cohort study. Front Psychiatry. 2017;8:277.
Huber RS, Kondo DG, Shi XF, Prescot AP, Clark E, Renshaw PF, et al. Relationship of executive functioning deficits to N-acetyl aspartate (NAA) and gamma-aminobutyric acid (GABA) in youth with bipolar disorder. J Affect Disord. 2018;225:71–8.
Khomenko YG, Kataeva GV, Bogdan AA, Chernysheva EM, Susin DS. Cerebral metabolism in patients with cognitive disorders: a combined MRS and PET study. Zh Nevrol Psikhiatr Im S S Korsakova. 2019;119:51–8.
Li H, Lu Q, Xiao E, Li Q, He Z, Mei X. Methamphetamine enhances the development of schizophrenia in first-degree relatives of patients with schizophrenia. Can J Psychiatry. 2014;59:107–13.
Gasparovic C, Prestopnik J, Thompson J, Taheri S, Huisa B, Schrader R, et al. 1H-MR spectroscopy metabolite levels correlate with executive function in vascular cognitive impairment. J Neurol Neurosurg Psychiatry. 2013;84:715–21.
Brooks WM, Sibbitt WJ, Kornfeld M, Jung RE, Bankhurst AD, Roldan CA. The histopathologic associates of neurometabolite abnormalities in fatal neuropsychiatric systemic lupus erythematosus. Arthritis Rheum. 2010;62:2055–63.
Zieminska E, Toczylowska B, Diamandakis D, Hilgier W, Filipkowski RK, Polowy R, et al. Glutamate glutamine and GABA levels in rat brain measured using MRS, HPLC and NMR methods in study of two models of autism. Front Mol Neurosci. 2018;11:418.
Keeney J, Ren X, Warrier G, Noel T, Powell DK, Brelsfoard JM, et al. Doxorubicin-induced elevated oxidative stress and neurochemical alterations in brain and cognitive decline: protection by MESNA and insights into mechanisms of chemotherapy-induced cognitive impairment ("chemobrain"). Oncotarget. 2018;9:30324–39.
Marjanska M, McCarten JR, Hodges JS, Hemmy LS, Terpstra M. Distinctive neurochemistry in Alzheimer’s disease via 7 T in vivo magnetic resonance spectroscopy. J Alzheimers Dis. 2019;68(2):559–69.
Joe E, Medina LD, Ringman JM, O'Neill J. 1H MRS spectroscopy in preclinical autosomal dominant Alzheimer disease. Brain Imaging Behav. 2019;13(4):925–32.
Rutman AM, Peterson DJ, Cohen WA, Mossa-Basha M. Diffusion tensor imaging of the spinal cord: clinical value, investigational applications, and technical limitations. Curr Probl Diagn Radiol. 2018;47:257–69.
Warbrick T, Rosenberg J, Shah NJ. The relationship between BOLD fMRI response and the underlying white matter as measured by fractional anisotropy (FA): a systematic review. Neuroimage. 2017;153:369–81.
Saykin AJ, de Ruiter MB, McDonald BC, Deprez S, Silverman DH. Neuroimaging biomarkers and cognitive function in non-CNS cancer and its treatment: current status and recommendations for future research. Brain Imaging Behav. 2013;7:363–73.
Yue Y, Yuan Y, Hou Z, Jiang W, Bai F, Zhang Z. Abnormal functional connectivity of amygdala in late-onset depression was associated with cognitive deficits. PLoS ONE. 2013;8:e75058.
Funding
This research received no specific grant from any funding agency in the public, commercial, or not-for-profit sectors.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
All authors have disclosed no conflicts of interest.
Ethical approval
All procedures performed in studies were in accordance with the ethical standards of the institutional research committee.
Informed consent
Informed consent was obtained from all individual participants included in the study.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
About this article
Cite this article
Tong, T., Lu, H., Zong, J. et al. Chemotherapy-related cognitive impairment in patients with breast cancer based on MRS and DTI analysis. Breast Cancer 27, 893–902 (2020). https://doi.org/10.1007/s12282-020-01094-z
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12282-020-01094-z