Purpose
Abstract
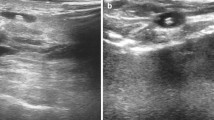
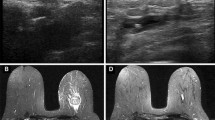
To evaluate the usefulness of the HydroMARK, a hydrogel-based breast biopsy site marker for ultrasound localization of breast lesions, we investigated the tendency for dislocation and sonographic detectability of the marker placed in patients.
Materials and methods
The marker was placed in lesions that were expected to become obscured after biopsy for a suspicious breast lesion or after neoadjuvant chemotherapy for breast cancer. The patients consented to return for a repeat ultrasound ± mammography examination, and the degree of displacement of the marker was measured as the marker-to-residual lesion distance.
Results
The marker was placed after stereotactic biopsy, ultrasound-guided biopsy, and before/during neoadjuvant chemotherapy, in 11, 22, and 7 lesions, respectively. Surgical resection was performed for 22 of the 40 lesions, while remaining 18 benign lesions were followed. The marker was sonographically detectable in 89.7% (35/39), 100% (35/35), and 100% (18/18) of the cases, respectively, at a median of 8 days, 13 weeks, and 11 months after the deployment. The degree of displacement was lower in the ultrasound-guided placement group than in the stereotactic placement group (median displacement: 0 vs. 4.3 mm; p = 0.001), it was also lower in the core-needle biopsy and neoadjuvent therapy cases than in the vacuum-assisted biopsy cases (p = 0.003). At a median interval of 2.5 months after deployment, the marker remained unchanged in location in all cases (n = 18, p = NS).
Conclusions
The HydroMARK appears to be a safe and effective marker with the advantageous characteristics of a low tendency for dislocation with time and long-term sonographic detectability.



Similar content being viewed by others
References
Nurco J, Mancino AT, Whitacre E, Edwards MJ. Surgical benefits conveyed by biopsy site marking system using ultrasound localization. Am J Surg. 2005;190:618–22.
Gittleman MA. Single-step ultrasound localization of breast lesions and lumpectomy procedure. Am J Surg. 2003;186(4):386–90.
Klein RL, Mook JA, Euhus DM, Rao R, Wynn RT, Eastman AB, et al. Evaluation of a hydrogel based breast biopsy marker (HydroMARK®) as an alternative to wire andradio active seed localization for non-palpable breast lesions. J Surg Oncol. 2012;105(6):591–4.
Blumencranz PW, Ellis D, Barlowe K. Use of hydrogel breast biopsy tissue markers reduces the need for wire localization. Ann Surg Oncol. 2014;21(10):3273–7.
Gentile LF, Himmler A, Shaw CM, Bouton A, Vorhis E, Marshall J, et al. Ultrasound-guided segmental mastectomy and excisional biopsy using hydrogel-encapsulated clip localization as an alternative to wire localization. Ann Surg Oncol. 2016;23(10):3284–9.
Rosen EL, Baker JA, Soo MS. Accuracy of a collagen-plug biopsy site marking device deployed after stereotactic core needle breast biopsy. AJR. 2003;181:1295–9.
Eby PR, Calhoun KE, Kurland BF, Demartini WB, Gutierrez RL, Peacock S, et al. Preoperative and intraoperative sonographic visibility of collagen-based breast biopsy marker clips. Acad Radiol. 2010;17(3):340–7.
Pinkney D, Shah A. Prospective comparative study to evaluate the sonographic visibility of five commercially available breast biopsy markers. J Diagn Med Sonography. 2013;29(4):151–8.
Sakamoto N, Ogawa Y, Tsunoda Y, Fukuma E. Evaluation of the sonographic visibility and sonographic appearance of the breast biopsy marker (UltraClip®) placed in phantoms and patients. Breast Cancer. 2017;24(4):585–92.
Ahmed M, Douek M. Intra-operative ultrasound versus wire-guided localization in the surgical management of non-palpable breast cancers: systematic review and meta-analysis. Breast Cancer Res Treat. 2013;140(3):435–46.
Ahmed M, van Hemelrijck M, Douek M. Systematic review of radioguided versus wire-guided localization in the treatment of non-palpable breast cancers. Breast Cancer Res Treat. 2013;140(2):241–52.
Pinkney DM, Mychajlowycz M, Shah BA. A prospective comparative study to evaluate the displacement of four commercially available breast biopsy markers. Br J Radiol. 1065;2016(89):20160149. https://doi.org/10.1259/bjr.20160149.
Rosen EL, Vo TT. Metallic clip deployment during stereotactic breast biopsy: retrospective analysis. Radiology. 2001;218(2):510–6.
Liberman L, Dershaw DD, Morris EA, Abramson AF, Thornton CM, Rosen PP. Clip placement after stereotactic vacuumassisted breast biopsy. Radiology. 1997;205:417–22.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflicts of interest.
About this article
Cite this article
Sakamoto, N., Fukuma, E., Tsunoda, Y. et al. Evaluation of the dislocation and long-term sonographic detectability of a hydrogel-based breast biopsy site marker. Breast Cancer 25, 575–582 (2018). https://doi.org/10.1007/s12282-018-0854-8
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12282-018-0854-8