Abstract
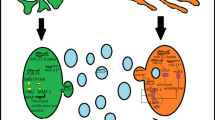
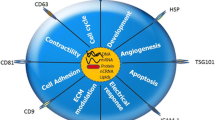
Cardiac exosomes mediate cell-to-cell communication, stimulate or inhibit the activities of target cells, and affect myocardial hypertrophy, injury and infarction, ventricular remodeling, angiogenesis, and atherosclerosis. The exosomes that are released in the heart from cardiomyocytes, vascular cells, fibroblasts, and resident stem cells are hypoimmunogenic, are physiologically more stable than cardiac cells, can circulate in the body, and are able to cross the blood–brain barrier. Exosomes utilize three mechanisms for cellular communication: (1) internalization by cells, (2) direct fusion to the cell membrane, and (3) receptor-ligand interactions. Cardiac exosomes transmit proteins, mRNA, and microRNAs to other cells during both physiological and pathological process. Cardiac-specific exosome miRNAs can regulate the expression of sarcomeric genes, ion channel genes, autophagy, anti-apoptotic and anti-fibrotic activity, and angiogenesis. This review discusses the role of exosomes and microRNAs in normal myocardium, myocardial injury and infarction, atherosclerosis, and the importance of circulating microRNAs as biomarkers of cardiac disease.

Graphical Abstract


Similar content being viewed by others
References
Due to space limitations, not all excellent papers on cardiac exosomes could be listed in the bibliography
Colombo, M., Raposo, G., & Thery, C. (2014). Biogenesics, secretion, and intercellular interactions of exosomes and other extracellular vesicles. Annual Review of Cell and Developmental Biology, 30, 255–289. https://doi.org/10.1146/annurev-cellbio-101512-122326.
Yanez-Mo M, Siljander P, Andreu Z, Bedina A et al. (2015) Biological properties of extracellular vesicles and their physiological functions. Journal of Extracell Vesicles 4: 27066 – doi:https://doi.org/10.3402/jev.v4.27066.
Barile, L., & Vassalli, G. (2017). Exosomes: therapy delivery tools and biomarkers of diseases. Pharmacology & Therapeutics, 174, 63–78.
Raposo, G., & Stoorvogel, W. (2013). Extracellular vesicles: exosomes, microvesicles, and friends. The Journal of Cell Biology, 200(4), 373–383. https://doi.org/10.1083/jcb.201211138.
Poe, A., & Knowlton, A. (2017). Exosomes as agents of change in the cardiovascular system. Journal of Molecular and Cellular Cardiology, 111, 40–50. https://doi.org/10.1016/j.yjmcc.2017.08.002.
Record, M., Subra, C., Silvente-Poirot, S., & Poirot, M. (2011). Exosomes as intercellular signalosomes and pharmacological effectors. Biochemical Pharmacology, 81, 1171–1182.
Malik, Z., Kott, K., Poe, A., Kuo, T., Chen, L., Ferrara, K., & Knowlton, A. (2013). Cardiac myocyte exosomes: stability, HSP60, and proteomics. American Journal of Physiology. Heart and Circulatory Physiology, 304, H954–H965. https://doi.org/10.1152/ajpheart.00835.2012.
Caby, M., Lankar, D., Vincendeau-Scherrer, C., Raposo, G., & Bonnerot, C. (2005). Exosomal-like vesicles are present in human blood plasma. International Immunology, 17, 879–887. https://doi.org/10.1093/intimm/dxh267.
Keller, S., Ridinger, J., Rupp, A., Janssen, J., & Altevogt, P. (2011). Body fluid derived exosomes as a novel template for clinical diagnostics. Journal of Translational Medicine, 9, 86–95. https://doi.org/10.1186/1479-5876-9-86.
Sluijter, J., Verhage, V., Deddens, J., van den Akker, F., & Doevendans, P. (2014). Microvesicles and exosomes for intracardiac communication. Cardiovascular Research, 102, 302–311.
Sahoo, S., & Losordo, D. W. (2014). Exosomes and cardiac repair after myocardial infarction. Circulation Research, 114, 333–344.
Pironti, G., Strachan, R. T., Abraham, D., Mon-Wei, Y. U. S., Chen, M., Chen, W., Hanada, K., Mao, L., Watson, L. J., & Rockman, H. A. (2015). Circulating exosomes induced by cardiac pressure overload contain functional angiotensin II type 1 receptors. Circ., 24, 2120–2130.
Kowal, J., Tkach, M., & Théry, C. (2014). Biogenesis and secretion of exosomes. Current Opinion in Cell Biology, 29, 116–125. https://doi.org/10.1016/j.ceb.2014.05.004.
Hanson, P. I., & Cashikar, A. (2012). Multivesicular body morphogenesis. Annual Review of Cell and Developmental Biology, 28, 337–362.
Villarroya-Beltri, C., Baixauli, F., Gutierrez-Vazquez, C., Sanchez-Madrid, F., & Mittelbrunn, M. (2014). Sorting it out: regulation of exosome loading. Seminars in Cancer Biology, 28, 3–13.
Colombo, M., Moita, C., van Niel, G., Kowal, J., Vigneron, J., Benaroch, P., Manel, N., Moita, L. F., Thery, C., & Raposo, G. (2013). Analysis of ESCRT functions in exosome biogenesis, composition and secretion highlights the heterogeneity of extracellular vesicles. Journal of Cell Science, 126(24), 5553–5565.
Henne, W., Buchkovich, N., & Emr, S. (2011). The ESCRT pathway. Developmental Cell, 21(1), 77–91.
Raiborg, C., & Stenmark, H. (2009). The ESCRT machinery in endosomal sorting of ubiquitylated membrane proteins. Nature, 458(7237), 445–452. https://doi.org/10.1038/nature07961.
Hurley, J., Boura, E., Carlson, L., & Różycki. (2010). Membrane budding. Cell., 143(6), 875–887. https://doi.org/10.1016/j.cell.2010.11.030.
Stoorvogel, W., Kleijmeer, M., Geuze, H., & Raposo, G. (2002). The biogenesis and functions of exosomes. Traffic, 3, 321–330.
Stoorvogel, W. (2015). Resolving sorting mechanisms into exosomes. Cell Research, 25, 531–532.
Kowal, J., Tkach, M., & Thery, C. (2014). Biogenesis and secretion of exosomes. Current Opinion in Cell Biology, 29, 116–125.
Hsu, C., Chiantia, S., Rajendran, L., Wenzel, D., Wieland, F., Schwille, P., Brugger, B., & Trajkovic, K. (2008). Ceramide triggers budding of exosome vesicles into multivesicular endosomes. Science, 319(5867), 1244–1247. https://doi.org/10.1126/science.1153124.
Maas, S., Breakefeld, X., & Weaver, A. (2017). Extracellular vesicles: unique intercellular delivery vehicles. Trends in Cell Biology, 27(3), 172–188. https://doi.org/10.1016/j.tcb.2016.11.003.
Hsu, C., Morohashi, Y., Yoshimura, S., Manrique-Hoyos, N., Jung, S., Lauterbach, M. A., Bakhti, M., Gronborg, M., Mobius, W., Rhee, J., Barr, F. A., & Simons, M. (2010). Regulation of exosome secretion by Rab35 and its GTPase-activating proteins TBC1D10A-C. The Journal of Cell Biology, 189(2), 223–232.
Seabra, M. C., Mules, E. H., & Hume, A. N. (2002). Rab GTPases, intracellular traffic and disease. Trends in Molecular Medicine, 8, 23–30.
Savina, A., Vidal, M., & Colombo, M. (2002). The exosome pathway in K562 cells is regulated by Rab11. Journal of Cell Science, 115(Pt 12), 2505–2515.
Pfeffer, S. (2010). Two Rabs for exosome release. Nature Cell Biology, 12, 3–4. https://doi.org/10.1038/ncb0110-3.
Ostrowski, M., Carmo, N., Krumeich, S., Fanget, I., Raposo, G., Savina, A., Moita, C. F., Schauer, K., Hume, A., Freitas, R., Goud, B., Benaroch, P., Hacohen, N., Fukuda, M., Desnos, C., Seabra, M., Darchen, F., Amigorena, S., Moita, L., & Thery, C. (2010). Rab27a and Rab27b control different steps of the exosome secretion pathway. Nature Cell Biology, 12(1), 19–30 sup pp 1–13.
Ali, B., & Seabra, M. (2005). Targeting of Rab GTPases to cellular membranes. Biochemical Society Transactions, 33, 652–656.
Jahn, R., & Scheller, R. H. (2006). SNAREs--engines for membrane fusion. Nature Reviews. Molecular Cell Biology, 7(9), 631–643.
Fader, C., Sanchez, D., Mestre, M., & Colombo, M. (2009). v-SNARE proteins involved in specific steps of the autophagy/multivesicular body pathways. Biochim Et Biophys Acta-Mol Cell Res., 1793(12), 1901–1916.
French, K., Antonyak, M., & Cerione, R. (2017). Extracellular vesicle docking at the cellular port: extracellular vesicle binding and uptake. Seminars in Cell & Developmental Biology, 67, 48–55. https://doi.org/10.1016/j.semcdb.2017.01.002.
Qui, G., Zheng, G., Ge, M., Wang, J., Huang, R., Shu, Q., & Xu, J. (2018). Mesenchymal stem cell-derived extracellular vesicles affect disease outcomes via transfer of microRNAs. Stem Cell Research & Therapy, 9, 320–329. https://doi.org/10.1186/s13287-018-1069.
Rana, S., Yue, S., Stadel, D., & Zöller, M. (2012). Toward tailored exosomes: the exosomal tetraspanin web contributes to target cell selection. The International Journal of Biochemistry & Cell Biology, 44(9), 1574–1584.
Yoshioka, Y., Konishi, Y., Kosaka, N., Nobuyoshi, K., Takeshi, K., Takashi, K., & Takahiro, O. (2013). Comparative marker analysis of extracellular vesicles in different human cancer types. J Extracell Vesicles., 2, 10.3402. https://doi.org/10.3402/jev.v2i0.20424.
Gurunathan, S., Kang, M.-H., Jeyaraj, M., Qasim, M., & Kim, J.-H. (2019). Review of the isolation, characterization, biological function and multifarious therapeutic approaches of exosomes. Cells, 8, 307–343. https://doi.org/10.3390/cells804030737.
Takov, K., Yellon, D., & Davidson, S. (2017). Confounding factors in vesicle uptake studies using fluorescent lipophilic membrane dyes. J Extracell Vesicles., 6, 1388731. https://doi.org/10.1080/20013078.2017.1388731.
Zeringer, E., Barta, T., Li, M., & Vlassov, A. (2015). Strategies for isolation of exosomes. Cold Spring Harbor Protocols. https://doi.org/10.1101/pdb.top074476.
Wu, M., Ouyang, Y., Wang, Z. R., Huang, P.-H., Chen, C., Li, H., Li, P., Quinn, D., Dao, M., Suresh, S., Sadovsky, Y., & Huang, T. (2017). Acoustofluidic exosome isolation from whole blood. Pro Nat Acad Sci, 114(40), 10584–10589. https://doi.org/10.1073/pnas.1709210114.
Gennebäck, N., Hellman, U., Malm, L., Larsson, G., Ronquist, G., Waldenström, A., & Mörner, S. (2013). Growth factor stimulation of cardiomyocytes induces changes in the transcriptional contents of secreted exosomes. J Extracell Vesicles, 2. https://doi.org/10.3402/jev.v2i0.20167.
Szatanek, R., Baj-Krzyworzeka, M., Zimoch, J., Lekka, M., Siedlar, M., & Baran, J. (2017). The methods of choice for extracellular vesicles (EVs) characterization. International Journal of Molecular Sciences, 18, 1153.
Erdbrügger, U., & Lannigan, J. (2015). Analytical challenges of extracellular vesicle detection: a comparison of different techniques. Cytometry. Part A, 89, 123–134.
Hessvik, N., Liorente, A. (2018). Current knowledge on exosome biogenesis and release. Cell and Moll Life Sci, 75(2), 193–208. https://doi.org/10.1007/s00018-017-2595-9.
Li, P., Kaslan, M., Lee, S. H., Yao, J., & Gao, Z. (2017). (2017) Progress in exosome isolation techniques. Theranost., 7(3), 789–804. https://doi.org/10.7150/thno.18133.
Thery, C., Witwer, K., Aikawa, E., et al. Minimal information for studies of extracellular vesicles 2018 (MISEV2018): a position statement of the International Society for Extracellular Vesicles and update of the MISEV2014 guidelines. Journal of Extracellular Vesicles, 7(1), 1535750. https://doi.org/10.1080/20013078.2018.1535750.
Garikipati, V., Shoja-Taheri, F., Davis, M., & Kishore, R. (2018). Extracellular vesicles and the application of system biology and computational modeling in cardiac repair. Circulation Research, 123, 188–204. https://doi.org/10.1161/CIRCRESAHA.117.311215.
Waldenstrom, A., Genneback, N., Hellman, U., & Ronquist, G. (2012). Cardiomyocyte microvesicles contain DNA/RNA and convey biological messages to target cells. PLoS One, 7, e34653.
Malik, Z., Kott, K., Poe, A., Kuo, T., Chen, L., Ferrara, K., & Knowlton, A. (2013). Cardiac myocyte exosomes: stability, HSP60, and proteomics. American Journal of Physiology. Heart and Circulatory Physiology, 304(7), H954–H965. https://doi.org/10.1152/ajpheart.00835.2012.
Ribeiro, M., Zhu, H., Millard, R., & Fan, G. (2013). Exosomes function in pro- and anti-angiogenesis. Curr. Angiogenes, 2, 54–59. https://doi.org/10.2174/22115528113020020001.
Stastna, M., Chimenti, I., Marban, E., & Van Eyk, J. (2010). Identification and functionality of proteomes secreted by rat cardiac stem cells and neonatal cardiomyocytes. Proteom., 10, 245–253.
Bei Y, Chen T, Banciu D, Cretoiu D, Xiao J. (2017) Circulating exosomes in cardiovascular diseases. In: Xiao J., Cretoiu S. (eds) Exosomes in Cardiovascular Diseases. Advan Exper Med and Bio, Springer, Singapore, vol 998.
Garcia, N., Moncay-Arlandi, J., Sepulveda, P., & Diez-Juan, A. (2016). Cardiomyocyte exosomes regulate glycolytic flux in endothelium by direct transfer of GLUT transporters and glycolytic enzymes. Cardiovascular Research, 109, 397–408. https://doi.org/10.1093/cvr/cvv260.
Garcia, N., Ontoria-Oviedo, I., González-King, H., Diez-Juan, A., & Sepúlveda, P. (2015). Glucose starvation in cardiomyocytes enhances exosome secretion and promotes angiogenesis in endothelial cells. PLoS One, 10, e0138849. https://doi.org/10.1371/journal.pone.0138849.
Gupta, S., & Knowlton, A. (2007). HSP60 trafficking in adult cardiac myocytes: role of the exosomal pathway. American Journal of Physiology. Heart and Circulatory Physiology, 292, H3052–H3056.
Yu, X., Deng, L., Wang, D., Li, N., Chen, X., Cheng, X., Yuan, J., Gao, X., Liao, M., Wang, M., & Liao, Y. (2012). Mechanism of TNF-α autocrine effects in hypoxic cardiomyocytes: initiated by hypoxia inducible factor 1α, presented by exosomes. J Mol Cell Cardiol, 53, 848–857. https://doi.org/10.1016/j.yjmcc.2012.10.002.
Wang, X., Gu, H., Huang, W., Peng, J., Li, Y., Yang, L., Qin, D., Essandoh, K., Wang, Y., Peng, T., & Fan, G. (2016). Hsp20-mediated activation of exosome biogenesis in cardiomyocytes improves cardiac function and angiogenesis in diabetic mice. Diabet., 65(10), 3111–3128.
Louapre, P., Grongnet, J., Tanguay, R., & David, J. (2005). Effects of hypoxia on stress proteins in the piglet heart at birth. Cell Stress & Chaperones, 10, 17–23.
Yu, H., & Wang, Z. (2019). Cardiomyocyte-derived exosomes: biological functions and potential therapeutic implications. Frontiers in Physiology, 10, 1049–1058. https://doi.org/10.3389/fphys.2019.01049.
Wang, X., Gu, H., Huang, W., Peng, J., Li, Y., Yang, L., Qin, D., Essandoh, K., Wang, Y., Peng, T., & Fan, G. (2016). Hsp20-mediated activation of exosome biogenesis in cardiomyocytes improves cardiac function and angiogenesis in diabetic mice. Diabetes, 65(10), 3111–3128. https://doi.org/10.2337/db15-1563.
Zhang, X., Wang, X., Zhu, H., Kranias, E., Tang, Y., Peng, T., Chang, J., & G-Cl, F. (2012). Hsp20 functions as a novel cardiokine in promoting angiogenesis via activation of VEGFR2. PLoS One, 7, e32765. https://doi.org/10.1371/journal.pone.0032765.
Feng, Y., Huang, W., Meng, W., Jegga, A., Wang, Y., Cai, W., Kim, H., Pasha, Z., Wen, Z., Rao, F., Modi, R., Yu, X., & Ashraf, M. (2014). Heat shock improves Sca-1+ stem cell survival and directs ischemic cardiomyocytes toward a prosurvival phenotype via exosomal transfer: a critical role for HSF1/miR-34a/HSP70 pathway. Stem Cells, 32, 462–472. https://doi.org/10.1002/stem.1571.
Yu, X., Deng, L., Wang, D., Li, N., Chen, X., Cheng, X., Yuan, J., Gao, X., Liao, M., Wang, M., & Liao, Y. (2012). Mechanism of TNF-a autocrine effects in hypoxic cardiomyocytes: initiated by hypoxia inducible factor 1a, presented by exosomes. Journal of Molecular and Cellular Cardiology, 53, 848–857. https://doi.org/10.1016/j.yjmcc.2012.10.002.
Datta, R., Bansal, T., Rana, S., Datta, K., Datta Chaudhur, R., Chawla-Sarkar, M., & Sarar, S. (2017). Myocyte-derived Hsp90 modulates collagen upregulation via biphasic activation of STAT-3 in fibroblasts during cardiac hypertrophy. Molecular and Cellular Biology, 37, e00611–e00616. https://doi.org/10.1128/MCB.00611-16.
Yates, L., Norbury, C., & Gilbert, R. (2013). The long and short of MicroRNA. Cell, 153(3), 516–519. https://doi.org/10.1016/j.cell.2013.04.003.
Friedman, R. C., Farh, K. K., Burge, C. B., & Bartel, D. P. (2009). Most mammalian mRNAs are conserved targets of microRNAs. Genome Research, 19, 92–105.
Bollini, S., Smits, A., Balbi, C., Lazzarini, E., & Amer, P. (2018). Triggering endogenous cardiac repair and regeneration via extracellular vesicle-mediated communication. Frontiers in Physiology, 9, 1497. https://doi.org/10.3389/fphys.2018.01497.
Deng, F., Xu, X., & Chen, Y. (2014). The role of miR-1 in the heart: from cardiac morphogenesis to physiological function. Human Genet Embryol., 4, 1. https://doi.org/10.4172/2161-0436.1000119.
Xu, C., Lu, Y., Pan, Z., Chu, W., Luo, X., Lin, H., Xiao, J., Shan, H., Wang, Z., & Yang, B. (2007). The muscle-specific microRNAs miR-1 and miR-133 produce opposing effects on apoptosis by targeting HSP60, HSP70 and caspase-9 in cardiomyocytes. Journal of Cell Science, 120, 3045–3052.
Castoldi, G., di Gioia, C., Bombardi, C., Catalucc, D., Corradi, B., Gualazzi, M., Leopizzi, M., Mancini, M., Zerbini, G., Condorell, G., & Stella, A. (2012). MiR-133a regulates collagen 1A1: potential role of miR-133a in myocardial fibrosis in angiotensin II-dependent hypertension. Journal of Cellular Physiology, 227, 850–856.
Kozakowska, M., Ciesla, M., Stefanska, A., Skrzypek, K., Was, H., Jazwa, A., Grochot-Przeczek, A., Kotlinowski, J., Szymula, A., Bartelik, A., Mazan, M., Yagensky, O., Florczyk, U., Lemke, K., Zebzda, A., Dyduch, G., Nowak, W., Szade, K., Stepniewski, J., Majka, M., Derlacz, R., Loboda, A., Dulak, J., & Jozkowicz, A. (2012). Heme oxygenase-1 inhibits myoblast differentiation by targeting myomirs. Antioxidants & Redox Signaling, 16(2), 113–127. https://doi.org/10.1089/ars.2011.3964.
Li, X., Wang, J., Jia, Z., Cui, Q., Zhang, C., Wang, W., Chen, P., Ma, K., & Zhou, C. (2013). MiR-499 regulates cell proliferation and apoptosis during late-stage cardiac differentiation via Sox6 and cyclin D1. PLoS One, 8(9), e74504. https://doi.org/10.1371/journal.pone.0074504.
Izarra, A., Moscoso, I., Levent, E., Cañón, S., Cerrada, I., Díez-Juan, A., Blanca, V., Núñez-Gil, I., Valiente, I., Ruíz-Sauri, A., Sepulveda, P., Tiburcy, M., Zimmermann, W., & Berna, A. (2014). miR-133a enhances the protective capacity of cardiac progenitors cells after myocardial infarction. Stem Cell Reports, 3, 1029–1042.
Wang, J., Jia, Z., Zhang, C., Sun, M., Wang, W., Chen, P., Ma, K., Zhang, Y., Li, X., & Zhou, C. (2014). miR-499 protects cardiomyocytes from H2O2-induced apoptosis via its effects on Pdcd4 and Pacs2. RNA Biology, 11, 339–350.
Li, S., Xiao, F., Shan, P., Su, L., Chen, D., Ding, J., & Wang, Q. (2015). Overexpression of microRNA-133a inhibits ischemia-reperfusion-induced cardiomyocyte apoptosis by targeting DAPK2. Journal of Human Genetics, 60(11), 709–716. https://doi.org/10.1038/jhg.2015.96.
Matsui, Y., Takagi, H., Qu, X., Abdellatif, M., Sakoda, H., Asano, T., Levine, B., & Sadoshima, J. (2007). Distinct roles of autophagy in the heart during ischemia and reperfusion: roles of AMP-activated protein kinase and Beclin 1 in mediating autophagy. Circulation Research, 100(6), 914–922.
Yang, J., Yu, X., Xue, F., Li, Y., Liu, W., & Zhang, S. (2018). Exosomes derived from cardiomyocytes promote cardiac fibrosis via myocyte-fibroblast crosstalk. American Journal of Translational Research, 10, 4350–4366.
Vanhaverbeke, M., Gal, D., & Holvoet, P. (2017). Functional role of cardiovascular exosomes in myocardial injury and atherosclerosis. In J. Xiao & S. Cretoiu (Eds.), Exosomes in cardiovascular diseases. Advances in Experimental Medicine and Biology (Vol. 998, pp. 45–58). Singapore: Springer.
Kuo, H., Hsieh, C., Wang, S., Chang, C., Hung, C., Kuo, L., Liu, Y.-R., Li, C.-Y., & Liu, P.-L. (2019). Simvastatin attenuates cardiac fibrosis via regulation of cardiomyocyte derived exosome secretion. Journal of Clinical Medicine, 8, E794. https://doi.org/10.3390/jcm8060794.
Wang, X., Huang, W., Liu, G., Cai, W., Millard, R. W., Wang, Y., Chang, J., Peng, T., & Fan, G. (2014). Cardiomyocytes mediate anti-angiogenesis in type 2 diabetic rats through the exosomal transfer of miR-320 into endothelial cells. Journal of Molecular and Cellular Cardiology, 74, 139–150. https://doi.org/10.1016/j.yjmcc.2014.05.001.
Davidson, S., Riquelme, J., Takov, K., Vicencio, J., Boi-Doku, C., Khoo, V., Doreth, C., Radenkovic, D., Lavandero, S., & Yellon, D. (2018). Cardioprotection mediated by exosomes is impaired in the setting of type II diabetes but can be rescued by the use of non-diabetic exosomes in vitro. Journal of Cellular and Molecular Medicine, 22, 141–151.
van Balkom, B., de Jong, O., Smits, M., Brummelman, J., den Ouden, K., de Bree, P., van Eijndhoven, M., Pegtel, D., Stoorvogel, W., Würdinger, T., & Verhaar, M. (2013). Endothelial cells require miR-214 to secrete exosomes that suppress senescence and induce angiogenesis in human and mouse endothelial cells. Blood., 121(3997–4006), S1–S15. https://doi.org/10.1182/blood-2013-02-478925.
Njock, M., Cheng, H., Dang, L., Nazari-Jahantigh, M., Lau, A., Boudreau, E., Roufaiel, M., Cybulsky, M. I., Schober, A., & Fish, J. (2015). Endothelial cells suppress monocyte activation through secretion of extracellular vesicles containing antiinflammatory microRNAs. Blood., 125(20), 3202–3212.
Vasa-Nicoteraa, M., Chena, H., Tuccia, P., Yanga, A., Saintignyc, G., Menghinid, R., Mahec, C., Agostinia, M., Knight, R., Melino, G., & Federic, M. (2011). miR-146a is modulated in human endothelial cell with aging. Athero., 217(2), 326–330. https://doi.org/10.1016/j.atherosclerosis.2011.03.034.
Lyu, L., Wang, H., Li, B., Qin, Q., Qi, L., Nagarkatti, M., Nagarkatti, P., Janicki, J., Wang, X., & Cui, T. (2015). A critical role of cardiac fibroblast-derived exosomes in activating renin angiotensin system in cardiomyocytes. Journal of Molecular and Cellular Cardiology, 89, 268–279. https://doi.org/10.1016/j.yjmcc.2015.10.022.
Zhao, Y., Ransom, J. F., Li, A., Vedantham, V., von Drehle, M., Muth, A., Tsuchihashi, T., McManus, M. T., Schwartz, R. J., & Srivastava, D. (2007). Dysregulation of cardiogenesis, cardiac conduction, and cell cycle in mice lacking miRNA-1-2. Cell, 129, 303–317. https://doi.org/10.1016/j.cell.2007.03.030.
Tian, C., Gao, L., Zimmerman, M., & Zucker, I. (2018). Myocardial infarction-induced microRNA-enriched exosomes contribute to cardiac Nrf2 dysregulation in chronic heart failure. American Journal of Physiology. Heart and Circulatory Physiology, 314, H928–H939. https://doi.org/10.1152/ajpheart.00602.2017.
Yang, Y., Li, Y., Chen, X., Cheng, X., Liao, Y., & Yu, X. (2016). Exosomal transfer of miR-30a between cardiomyocytes regulates autophagy after hypoxia. Journal of Molecular Medicine, 94, 711–724. https://doi.org/10.1007/s00109-016-1387-287.
Oliveira-Carvalho, V., da Silva, M., Guimarães, G., Bacal, F., & Bocchi, E. (2013). MicroRNAs: new players in heart failure. Molecular Biology Reports, 40(3), 2663–2670. https://doi.org/10.1007/s11033-012-2352-y.
He, B., Xiao, J., Ren, A., Zhang, Y.-F., Zhang, H., Chen, M., Xie, B., Gao, X.-G., & Wang, Y.-W. (2011). Role of miR-1 and miR-133a in myocardial ischemic postconditioning. Journal of Biomedical Science, 18, 22. https://doi.org/10.1186/1423-0127-18-22.
Puthanveetila, P., Benga, B., Matkovichb, S., Dorn, G., & Chakrabarti, S. (2014). Cardiac miR-133a overexpression preventsearly cardiac fibrosis in diabetes. Journal of Cellular and Molecular Medicine, 18(3), 415–421.
Oliveira-Carvalho, V., Carvalho, V., & Bocchi, E. (2013). (2013) The emerging role of miR-208a in the heart. DNA and Cell Biology, 32(1), 8–12. https://doi.org/10.1089/dna.2012.1787.
Nie, X., Fan, J., Li, H., Yin, Z., Zhao, Y., Dai, B., Dong, N., Chen, C., & Wang, D. W. (2018). MiR-217 promotes cardiac hypertrophy and dysfunction by targeting PTEN. Molecular Therapy--Nucleic Acids, 12, 254–266.
Fish, J., Santoro, M., Morton, S., Yu, S., Yeh, R., Wythe, J., Ivey, K., Bruneau, B., Stainier, D., & Srivastava, D. (2008). miR-126 regulates angiogenic signaling and vascular integrity. Developmental Cell, 5(2), 272–284.
Wang, S., Aurora, A., Johnson, B., Qi, X., McAnally, J., Hill, J., Richardson, J., Bassel-Duby, R., & Olson, E. (2008). The endothelial-specific microRNA miR-126 governs vascular integrity and angiogenesis. Developmental Cell, 15(2), 261–271.
Chen, Y., & Gorski, D. (2008). Regulation of angiogenesis through a microRNA (miR-130a) that down-regulates antiangiogenic homeobox genes GAX and HOXA5. Blood, 111(3), 1217–1226.
Halkein, J., Tabruyn, S., Ricke-Hoch, M., Haghikia, A., Nguyen, N., Scherr, M., Castermans, K., Malvaux, L., Lambert, V., Thiry, M., Sliwa, K., Noel, A., Martial, J., Hilfiker-Kleiner, D., & Struman, I. (2013). MicroRNA-146a is a therapeutic target and biomarker for peripartum cardiomyopathy. The Journal of Clinical Investigation, 123, 2143–2154. https://doi.org/10.1172/JCI64365.
Teng, X., Chen, L., Chen, W., Yang, J., Yang, Z., & Shen, Z. (2015). Mesenchymal stem cell-derived exosomes improve the microenvironment of infarcted myocardium contributing to angiogenesis and anti-inflammation. Cellular Physiology and Biochemistry, 37, 2415–2424.
Yu, B., Kim, H., Gong, M., Wang, J., Millard, R., Wang, Y., Ashraf, M., & Xu, M. (2015). Exosomes secreted from GATA-4 overexpressing mesenchymal stem cells serve as a reservoir of anti-apoptotic microRNAs for cardioprotection. International Journal of Cardiology, 182, 349–360.
Vrijsen, K., Maring, J., Chamuleau, S., Verhage, V., Mol, E., Deddens, J., Metz, C., Lodder, K., van Eeuwijk, E., van Dommelen, S., Doevendans, P., Smits, A., Goumans, M., & Sluijter, J. (2016). Exosomes from cardiomyocyte progenitor cells and mesenchymal stem cells stimulate angiogenesis via EMMPRIN. Advanced Healthcare Materials, 5, 2555–2565.
Lai, R., Tan, S., Teh, B., Sze, S., Arslan, F., de Kleijn, D., Choo, A., & Lim, S. (92012). Proteolytic potential of the MSC exosome proteome: implications for an exosome-mediated delivery of therapeutic proteasome. Int J Proteom, 2012, 971907. https://doi.org/10.1155/2012/971907.
Chen T, Lai R, Lee M, Choo A, Lee C, Lim S. (2010) Mesenchymal stem cell secretes microparticles enriched in premicroRNAs. Nuc Acids Res.38:215–224.
Chen, L., Wang, Y., Pan, Y., Zhang, L., Shen, C., Qin, G., Ashraf, M., Weintraub, N., Ma, G., & Tang, Y. (2013). Cardiac progenitor-derived exosomes protect ischemic myocardium from acute ischemia/reperfusion injury. Biochemical and Biophysical Research Communications, 431, 566–571. https://doi.org/10.1016/j.bbrc.2013.01.015.
Barile, L., Lionetti, V., Cervio, E., Matteucci, M., Gherghiceanu, M., Popescu, L. M., Torre, T., Siclari, F., Moccetti, T., & Vassalli, G. (2014). Extracellular vesicles from human cardiac progenitor cells inhibit cardiomyocyte apoptosis and improve cardiac function after myocardial infarction. Cardiovascular Research, 103(4), 530–541. https://doi.org/10.1093/cvr/cvu167.
Ibrahim, A., Cheng, K., & Marb#an E. (2014). Exosomes as critical agents of cardiac regeneration triggered by cell therapy. Stem Cell Reports, 5, 606–619.
Chen, L., Wang, Y., Pan, Y., Zhang, L., Shen, C., Qin, G., Ashraf, M., Weintraub, N., Ma, G., & Tang, Y. (2013). Cardiac progenitor-derived exosomes protect ischemic myocardium from acute ischemia/reperfusion injury. Biochemical and Biophysical Research Communications, 431(3), 566–571.
Xiao, J., Pan, Y., Li, X., Yang, X., Feng, Y., Tan, H., Jiang, L., Feng, J., & Yu, X. (2016). Cardiac progenitor cell-derived exosomes prevent cardiomyocytes apoptosis through exosomal miR-21 by targeting PDCD4. Cell Death & Disease, 7, e2277.
Agarwal, U., George, A., Bhutani, S., Ghosh-Choudhary, S., Maxwell, J., Brown, M., Mehta, Y., Platt, M., Liang, Y., Sahoo, S., & Davis, M. (2017). Experimental, systems, and computational approaches to understanding the MicroRNA-mediated reparative potential of cardiac progenitor cell-derived exosomes from pediatric patients. Circulation Research, 120(4), 701–712.
Sharma, S., Mishra, R., Bigham, G. E., Wehman, B., Khan, M. M., Xu, H., Saha, P., Goo, Y., Datla, S., Chen, L., Tulapurkar, M., Taylor, B., Yang, P., Karathanasis, S., Goodlett, D., & Kaushal, S. (2017). A deep proteome analysis identifies the complete secretome as the functional unit of human cardiac progenitor cells. Circulation Research, 120(5), 816–834.
Lin, C., Li, S., Deng, S., Fu, X., Qin, A., & Yu, X. (2019). The role of stem cell-derived exosomes in repairing myocardial injury. Sheng Li Xue Bao, 71(2), 205–215. https://doi.org/10.13294/j.aps.2019.0010.
Duan, P., Tan, J., Miao, Y., & Zhang, Q. (2019). Potential role of exosomes in the pathophysiology, diagnosis, and treatment of hypoxic diseases. American Journal of Translational Research, 11(3), 1184–1201.
Moghaddama, A., Afsharia, J., Esmaeilib, S.-A., Saburid, E., Joneidif, Z., & Momtazi-Borojenig, A. (2019). Cardioprotective microRNAs: lessons from stem cell-derived exosomal microRNAs to treat cardiovascular disease. Athero., 285, 1–9.
Mol, E., Goumans, M., & Sluijter, J. (2017). Cardiac progenitor-cell derived exosomes as cell-free therapeutic for cardiac repair. Exosomes in cardiovascular diseases: biomarkers, pathological and therapeutic effects. Advances in Experimental Medicine and Biology, 98, 207–219.
Srivastava, D., & Ivey, K. (2006). Potential of stem-cell-based therapies for heart disease. Nature, 441, 1097–1099. https://doi.org/10.1038/nature04961.
Khan, M., Nickoloff, E., Abramova, T., Johnson, J., Verma, S., Krishnamurthy, P., Mackie, A., Vaughan, E., Garikipati, V., Benedict, C., Ramirez, V., Lambers, E., Ito, A., Gao, E., Misener, S., Luongo, T., Elrod, J., Qin, G., Houser, S., Koch, W., & Kishore, R. (2015). Embryonic stem cell-derived exosomes promote endogenous repair mechanisms and enhance cardiac function following myocardial infarction. Circulation Research, 117(1), 52–64.
Xiao, J., Pan, Y., Li, X., Yang, X., Feng, Y., Tan, H., Jiang, L., Feng, J., & Yu, X. Y. (2016). Cardiac progenitor cell-derived exosomes prevent cardiomyocytes apoptosis through exosomal miR-21 by targeting PDCD4. Cell Death & Disease, 7(6), e2277.
Gray, W., French, K., Ghosh-Choudhary, S., Maxwell, J., Brown, M., Platt, M., Searles, C., & Davis, M. (2015). Identification of therapeutic covariant microRNA clusters in hypoxia-treated cardiac progenitor cell exosomes using systems biology. Circulation Research, 116(2), 255–263. https://doi.org/10.1161/CIRCRESAHA.116.304360.
Luthera, K., Haara, L., McGuinessa, M., Wanga, Y., Lynch, T., Phana, A., Songa, Y., Shenb, Z., Gardnerb, G., Kuffeia, G., Rena Xm Zilloxa, M., & Jonesa, W. (2018). Exosomal miR-21a-5p mediates cardioprotection by mesenchymal stem cell. Journal of Molecular and Cellular Cardiology, 119, 125–137.
Feng Y, Huang W, Wani M, Yu X, Ashraf M. (2014) Ischemic preconditioning potentiates the protective effect of stem cells through secretion of exosomes by targeting Mecp2 via miR-22 PLoS One 9(2): e88685.
Ottaviani, L., Sansonetti, M., & da Costa Martins, P. A. (2018). Myocardial cell-to-cell communication via microRNAs. Noncoding RNA Res., 3(3), 144–153. https://doi.org/10.1016/j.ncrna.2018.05.004.
Wang, B., Komers, R., Carew, R., Winbanks, C., Xu, B., Herman-Edelstein, M., Koh, P., Thomas, M., Jandeleit-Dahm, K., Gregorevic, P., Cooper, M., & Kantharidis, P. (2012). Suppression of microRNA-29 expression by TGF-β1 promotes collagen expression and renal fibrosis. J Am Soc Nephrol., 23(2), 252–265. https://doi.org/10.1681/ASN.201101005521.
Wang, K., Jiang, Z., Webster, K. A., Chen, J. H., Hu, H. X., Zhou, Y., Zhao, J., Wang, L. H., Wang, Y. C., Zhong, Z. W., Ni, C., Li, Q. J., Xiang, C., Zhang, L., Wu, R., Zhu, W., Yu, H., Hu, X., & Wang, J. (2017). Enhanced cardioprotection by human endometrium mesenchymal stem cells driven by exosomal microRNA-21. Stem Cells Translational Medicine, 6(1), 209–222.
Park, H., Park, H., Mun, D., Kang, J., Kim, H., Kim, M., Cui, S., Lee, S., & Joung, B. (2018). Extracellular vesicles derived from hypoxic human mesenchymal stem cells attenuate gsk3β expression via mirna-26a in an ischemia-reperfusion injury model. Yonsei Medical Journal, 59, 736–745. https://doi.org/10.3349/ymj.2018.59.6.736.
Wang, N., Chen, C., Yang, D., Liao, Q., Luo, H., Wang, X., Zhou, F., Yang, X., Yang, J., Zeng, C., & Wang, W. (2017). Mesenchymal stem cells-derived extracellular vesicles, via miR-210, improve infarcted cardiac function by promotion of angiogenesis. Biochimica et Biophysica Acta - Molecular Basis of Disease, 1863(8), 2085–2092.
Xiao, C., Wang, K., Xu, Y., Hu, H., Zhang, N., Wang, Y., Zhong, Z., Zhao, J., Li, Q., Zhu, D., Ke, C., Zhong, S., Wu, X., Yu, H., Zhu, W., Chen, J., Zhang, J., Wang, J., & Hu, X. (2018). Transplanted mesenchymal stem cells reduce autophagic flux in infarcted hearts via the exosomal transfer of miR-125b. Circulation Research, 123(5), 564–578. https://doi.org/10.1161/CIRCRESAHA.118.312758.
Namazi, H., Mohit, E., Namazi, I., Rajabi, S., Samadian, A., Hajizadeh-Saffar, E., Aghdami, N., & Baharvand, H. (2018). Exosomes secreted by hypoxic cardiosphere-derived cells enhance tube formation and increase pro-angiogenic miRNA. Journal of Cellular Biochemistry, 119(5), 4150–4160.
de Couto, G., Gallet, R., Cambier, L., Jaghatspanyan, E., Makkar, N., Dawkins, J., Berman, B., & Marban, E. (2017). Exosomal MicroRNA transfer into macrophages mediates cellular postconditioning. Circ., 136(2), 200–214.
Li J, Wan W, Chen T, Tong S, Jiang X, Liu W. (2019) miR-451 silencing inhibited doxorubicin exposure-induced cardiotoxicity in mice. BioMed Research International Article ID 1528278, 11 pages. doi:https://doi.org/10.1155/2019/1528278.
Shi, B., Wang, Y., Zhao, R., Long, X., Deng, W., & Wang, Z. (2018). Bone marrow mesenchymal stem cell-derived exosomal miR-21 protects C-kit(+) cardiac stem cells from oxidative injury through the PTEN/PI3K/Akt axis. PLoS One, 13(2), e0191616.
Luo, Q., Guo, D., Liu, G., Chen, G., Hang, M., & Jin, M. (2017). Overexpressing ADscs are therapeutic in relieving acute myocardial ischaemic injury. Cellular Physiology and Biochemistry, 44, 2105–2116. https://doi.org/10.1159/000485949.
Kwak, J., Choi, S., Oh, W., Yang, Y., Jeon, H., & Jeon, E. (2018). Cobalt chloride enhances the anti-inflammatory potency of human umbilical cord blood-derived mesenchymal stem cells through the erk-hif-1α-microrna-146a-mediated signaling pathway. Stem Cells Internat, 2018:Article ID 4978763. https://doi.org/10.1155/2018/4978763.29.
Emanueli, C., Shearn, A., Angelini, G., & Sahoo, S. (2015). Exosomes and exosomal miRNAs in cardiovascular protection and repair. Vascular Pharmacology, 71, 24–30.
Kuwabara, Y., Ono, K., Horie, T., Nishi, H., Nagao, K., Kinoshita, M., Watanabe, S., Baba, O., Kojima, Y., Shizuta, S., Imai, M., Tamura, T., Kita, T., & Kimura, T. (2011). Increased microRNA-1 and microRNA-133a levels in serum of patients with cardiovascular disease indicate myocardial damage. Circulation. Cardiovascular Genetics, 4, 446–454.
Cheng, Y., Wang, X., Yang, J., Duan, X., Yao, Y., Shi, X., Chen, Z., Fan, Z., Liu, X., Qin, S., Tang, X., & Zhang, C. (2012). A translational study of urine miRNAs in acute myocardial infarction. Journal of Molecular and Cellular Cardiology, 53, 668–676.
D’Alessandra, Y., Devanna, P., Limana, F., Straino, S., Di Carlo, A., Brambilla, P. G., Rubino, M., Carena, M. C., Spazzafumo, L., De Simone, M., Micheli, B., Biglioli, P., Achilli, F., Martelli, F., Maggiolini, S., Marenzi, G., Pompilio, G., & Capogrossi, M. C. (2010). Circulating microRNAs are new and sensitive biomarkers of myocardial infarction. European Heart Journal, 31, 2765–2773.
Olivieri, F., Antonicelli, R., Lorenzi, M., D’Alessandra, Y., Lazzarini, R., Santini, G., Spazzafumo, L., Lisa, R., La, S., Galeazzi, R., Recchioni, R., Testa, R., Pompilio, G., Capogrossi, M., & Procopio, A. (2013). Diagnostic potential of circulating miR-499-5p in elderly patients with acute non ST-elevation myocardial infarction. International Journal of Cardiology, 167, 531–536.
Wang, G. K., Zhu, J. Q., Zhang, J. T., Li, Q., Li, Y., He, J., Qin, Y. W., & Jing, Q. (2010). Circulating microRNA: a novel potential biomarker for early diagnosis of acute myocardial infarction in humans. European Heart Journal, 31, 659–666.
Bi, S., Wang, C., Jin, Y., Lv, Z., Xing, X., & Lu, Q. (2015). Correlation between serum exosome derived miR-208a and acute coronary syndrome. International Journal of Clinical and Experimental Medicine, 8, 4275–4280.
Matsumoto, S., Sakata, Y., Suna, S., Nakatani, D., Usami, M., Hara, M., Kitamura, T., Hamasaki, T., Nanto, S., Kawahara, Y., & Komuro, I. (2013). Circulating p53-responsive microRNAs are predictive indicators of heart failure after acute myocardial infarction. Circulation Research, 113(3), 322–326.
Jakob, P., Doerries, C., Briand, S., Mocharla, P., Krankel, N., Besler, C., Mueller, M., Manes, C., Templin, C., Baltes, C., Rudin, M., Adams, H., Wolfrum, M., Noll, G., Ruschitzka, F., Luscher, T., & Landmesser, U. (2012). Loss of angiomiR-126 and 130a in angiogenic early outgrowth cells from patients with chronic heart failure: role for impaired in vivo neovascularization and cardiac repair capacity. Circulation, 126(25), 2962–2975.
Jansen, F., Yang, X., Proebsting, S., Hoelscher, M., Przybilla, D., Baumann, K., Schmitz, T., Dolf, A., Endl, E., Franklin, B., Sinning, J., Vasa-Nicotera, M., Nickenig, G., & Werner, N. (2014). MicroRNA expression in circulating microvesicles predicts cardiovascular events in patients with coronary artery disease. Journal of the American Heart Association, 3(6), e001249. https://doi.org/10.1161/JAHA.114.001249.
Luo, H., Li, X., Li, T., Zhao, L., He, J., Zha, L., Qi, Q., & Yu, Z. (2019). microRNA-423-3p exosomes derived from cardiac fibroblasts mediates the cardioprotective effects of ischaemic post-conditioning. Cardiovascular Research, 115(7), 1189–1204. https://doi.org/10.1093/cvr/cvy231.
Cheng, M., Zhao, X., Wu, B., Mao, X., Yi, G., Zeng, Q., & Qin, G. (2014). Circulating exosomal miR-1a is markedly induced by myocardial infarction and downregulates CXCR4 expression in the bone marrow mononuclear cells. Circ., 130, A18383.
Yang, Y., Li, Y., Chen, X., Cheng, X., Liao, Y., & Yu, X. (2016). Exosomal transfer of miR-30a between cardiomyocytes regulates autophagy after hypoxia. Journal of Molecular Medicine (Berlin, Germany), 94, 711–724.
Li, J., Gelber, R., Rutka, J., Sabah, N., Gladstone, R., Wei, C., Hu, P., Kharbanda, R., & Redington, A. (2014). MicroRNA-144 is a circulating effector of remote ischemic preconditioning. Basic Research in Cardiology, 109, 423. https://doi.org/10.1007/s00395-014-0423-z.
Aurora, A., Mahmoud, A., Luo, X., Johnson, B., van Rooij, E., Matsuzaki, S., Humphries, K., Hill, J., Bassel-Duby, R., Sadek, H., & Olson, E. (2012). MicroRNA-214 protects the mouse heart from ischemic injury by controlling Ca2+ overload and cell death. The Journal of Clinical Investigation, 122(4), 1222–1232. https://doi.org/10.1172/JCI59327.
Chaturvedi, P., Kalani, A., Medina, I., Familtseva, A., & Tyagi, S. (2015). Cardiosome-mediated regulation of MMP9 in diabetic heart: role of mir29b and mir455 in exercise. Journal of Cellular and Molecular Medicine, 19, 2153–2161.
Vicencio, J., Yellon, D., Sivaraman, V., Das, D., Boi-Doku, C., Arjun, S., Zheng, Y., Riquelme, J., Kearney, J., Sharma, V., Multhoff, G., Hall, A., & Davidson, S. (2015). Plasma exosomes protect the myocardium from ischemia-reperfusion injury. Journal of the American College of Cardiology, 65, 1525–1536. https://doi.org/10.1016/j.jacc.2015.02.026.
Zhang, X., Wang, X., Zhu, H., Kranias, E. G., Tang, Y., Peng, T., et al. (2012). Hsp20 functions as a novel cardiokine in promoting angiogenesis via activation of VEGFR2. PLoS One, 7, e32765. https://doi.org/10.1371/journal.pone.0032765.
Zhang, C., Wu, J., Xu, X., Potter, B., & Gao, X. (2010). Direct relationship between levels of TNF-alpha expression and endothelial dysfunction in reperfusion injury. Basic Research in Cardiology, 105, 453–464.
Tian, J., Guo, X., Liu, X., Liu, L., Weng, Q., Dong, S., Knowlton, A., Yuan, W., & Lin, L. (2013). Extracellular HSP60 induces inflammation through activating and up-regulating TLRs in cardiomyocytes. Cardiovascular Research, 98, 391–401.
Loyer, X., Zlatanova, I., Devue, C., Yin, M., Howangyin, K., Klaihmon Pzannis, K., Fleischmann, B., Hwang, D., Park, J., Lee, H., Menasche, P., Silvestre, J.-S., & Bourlanger, C. (2018). Intra-cardiac release of extracellular vesicles shapes inflammation following myocardial infarction. Circulation Research, 123, 100–106. https://doi.org/10.1161/CIRCRESAHA.117.311326.
Belevych, A., Sansom, S., Terentyeva, R., Ho, H., Nishijima, Y., Martin, M., Jindal, H., Rochira, J., Kunitomo, Y., Abdellatif, M., Carnes, C., Elton, T., Gyorke, S., & Terenhyev, D. (2011). MicroRNA-1 and -133 increase arrhythmogenesis in heart failure by dissociating phosphatase activity from RyR2 complex. PLoS One, 6(12), e28324. https://doi.org/10.1371/journal.pone.0028324.
Lu, Y., Zhang, Y., Wang, N., Pan, Z., Gao, X., et al. (2010). MicroRNA-328 contributes to adverse electrical remodeling in atrial fibrillation. Circulation, 122, 2378–2387.
Arslan, F., Lai, R., Smeets, M., Akeroyd, L., Choo, A., Aguor, E., Timmers, L., van Rijen, H., Doevendans, P., Pasterkamp, G., Lim, S., & de Kleijn, D. (2013). Mesenchymal stem cell-derived exosomes increase ATP levels, decrease oxidative stress and activate PI3K/Akt pathway to enhance myocardial viability and prevent adverse remodeling after myocardial ischemia/reperfusion injury. Stem Cell Research, 10(3), 301–312. https://doi.org/10.1016/j.scr.2013.01.002.
Vandergriff, A., De Andrade, J., Tang, J., Hensley, M., Piedrahita, J., Caranasos, T., & Cheng, K. (2015). Intravenous cardiac stem cell-derived exosomes ameliorate cardiac dysfunction in doxorubicin induced dilated cardiomyopathy. Stem Cells Int, 960926. https://doi.org/10.1155/2015/960926.
Tseliou, E., Fouad, J., Reich, H., Slipczuk, L., de Couto, G., Aminzadeh, M., Middleton, R., Valle, J., Weixin, L., & Marbán, E. (2015). Fibroblasts rendered antifibrotic, antiapoptotic, and angiogenic by priming with cardiosphere-derived extracellular membrane vesicles. Journal of the American College of Cardiology, 66(6), 599–611. https://doi.org/10.1016/j.jacc.2015.05.068.
Kumar, S., Kim, C., & Simmons, R. (2014). Role of flow-sensitive microRNAs in endothelial dysfunction and atherosclerosis – “Mechanosensitive Athero-miRs”. Arterioscler Thromb Vasc Biol, 34(10), 2206–2216. https://doi.org/10.1161/ATVBAHA.114.303425.
Zhan, R., Leng, X., Liu, X., Wang, X., Gong, J., Yan, L., Yang, W., Wang, W., & Qian, L.-J. (2009). Heat shock protein 70 is secreted from endothelial cells by a non-classical pathway involving exosomes. Biochemical and Biophysical Research Communications, 387, 229–223. https://doi.org/10.1016/j.bbrc.2009.06.095.
Zhang, Y., Hu, Y.-W., Zheng, L., & Wang, Q. (2017). Characteristics and roles of exosomes in cardiovascular disease. DNA and Cell Biology, 36(3), 202–211. https://doi.org/10.1089/dna.2016.3496.
Gao, W., Liu, H., Yuan, J., Wu, C., Huang, D., Ma, Y., Zhu, J., Ma, L., Guo, J., Shi, H., Zou, Y., & Ge, J. (2016). Exosomes derived from mature dendritic cells increase endothelial inflammation and atherosclerosis via membrane TNF-alpha mediated NF-kappaB pathway. Journal of Cellular and Molecular Medicine, 20(12), 2318–2327. https://doi.org/10.1111/jcmm.12923.
Zakharova, L., Svetlova, M., & Fomina, A. (2007). T cell exosomes induce cholesterol accumulation in human monocytes via phosphatidylserine receptor. Journal of Cellular Physiology, 212, 174–181.
Wei, Y., Nazari-Jahantigh, M., Chan, L., Zhu, M., Heyll, K., Corbalan-Campos, J., Hartmann, P., Thiemann, A., Weber, C., & Schober, A. (2013). The microrna-342-5p fosters inflammatory macrophage activation through an akt1- and microrna-155-dependent pathway during atherosclerosis. Circ., 127, 1609–1619.
Srikanthan, S., Li, W., Silverstein, R., & McIntyre, T. (2014). Exosome poly-ubiquitin inhibits platelet activation, downregulates CD36 and inhibits pro-atherothombotic cellular functions. Journal of Thrombosis and Haemostasis, 12, 1906–1917.
Wang, Y., Xie, Y., Zhang, A., Wang, M., Fang, Z., & Zhang, J. (2019). Exosomes: an emerging factor in atherosclerosis. Biomedicine & Pharmacotherapy, 118, 109119.
Zernecke, A., Bidzhekov, K., Noels, H., Shagdarsuren, E., Gan, L., Denecke, B., Hristov, M., Köppel, T., Jahantigh, M., Lutgens, E., Wang, S., Olson, E., Schober, A., & Weber, C. (2009). Delivery of microRNA-126 by apoptotic bodies induces CXCL12-dependent vascular protection. Sci Signal, 2(100), ra81. https://doi.org/10.1126/scisignal.2000610.
Hergenreider, E., Heydt, S., Tréguer, K., Boettger, T., Horrevoets, A., Zeiher, A., Scheffer, M., Frangakis, A., Yin, X., Mayr, M., Braun, T., Urbich, C., Boon, R., & Dimmeler, S. (2012). Atheroprotective communication between endothelial cells and smooth muscle cells through miRNAs. Nature Cell Biology, 14(3), 249–256. https://doi.org/10.1038/ncb2441.
Wang, K., Garmire, L., Young, A., Nguyen, P., Trinh, A., Subramaniam, S., Wang, N., Shyy, J., Li, Y., & Chien, S. (2010). Role of microrna-23b in flow-regulation of rb phosphorylation and endothelial cell growth. Pro Nat Acad Sci USA., 107, 3234–3239.
Fang, Y., & Davies, P. F. (2012). Site-specific microrna-92a regulation of kruppel-like factors 4 and 2 in atherosusceptible endothelium. Arteriosclerosis, Thrombosis, and Vascular Biology, 32, 979–987.
Kim, C., Kumar, S., Son, D., Jang, I., Griendling, K., & Jo, H. (2014). Prevention of abdominal aortic aneurysm by anti-microrna-712 or anti-microrna-205 in angiotensin ii-infused mice. Arteriosclerosis, Thrombosis, and Vascular Biology, 34(7), 1412–1421. https://doi.org/10.1161/ATVBAHA.113.303134.
Ni, C., Qiu, H., & Jo, H. (2011). Microrna-663 upregulated by oscillatory shear stress plays a role ininflammatory response of endothelial cells. The American Journal of Physiology, 300, H1762–H1769.
Son, D., Kumar, S., Takabe, W., Kim, C., Ni, C., Alberts-Grill, N., Jang, I., Kim, S., Kim, W., Won Kang, S., Baker, A., Woong Seo, J., Ferrara, K., & Jo, H. (2013). The atypical mechanosensitive microrna-712 derived from pre-ribosomal rna induces endothelial inflammation and atherosclerosis. Nature Communications, 4, 3000. https://doi.org/10.1038/ncomms4000.
Rotllan, N., Ramirez, C. M., Aryal, B., Esau, C., & Fernandez-Hernando, C. (2013). Therapeutic silencing of microrna-33 inhibits the progression of atherosclerosis in ldlr−/− mice--brief report. Arteriosclerosis, Thrombosis, and Vascular Biology, 33, 1973–1977.
Rayner, K., Esau, C., Hussain, F., McDaniel, A., Marshall, S., van Gils, J., Ray, T., Sheedy, F., Goedeke, L., Liu, X., Khatsenko, O., Kaimal, V., Lees, C., Fernandez-Hernando, C., Fisher, E., Temel, R., & Moore, K. (2011). Inhibition of mir-33a/b in non-human primates raises plasma hdl and lowers vldl triglycerides. Nature., 478, 404–407.
Sun, H.-X., Zeng, D.-Y., Li, R.-T., Pang, R.-P., Yang, H., Hu, Y.-L., Zhang, W., Jiang, Y., Huang, L.-Y., Tang, Y.-B., Yan, G.-J., & Zhou, J.-G. (2012). Essential role of microrna-155 in regulating endothelium-dependent vasorelaxation by targeting endothelial nitric oxide synthase. Hypertension, 60, 1407–1414.
Chistiakov, D., Sobenin, I., Orekhov, A., & Bobryshev, Y. (2015). Human miR-221/222 in physiological and atherosclerotic vascular remodeling. BioMed Research International, 2015, 354517. https://doi.org/10.1155/2015/354517.
Wei, Y., Nazari-Jahantigh, M., Chan, L., Zhu, M., Heyll, K., Corbalan-Campos, J., Hartmann, P., Thiemann, A., Weber, C., & Schober, A. (2013). The microrna-342-5p fosters inflammatory macrophage activation through an akt1- and microrna-155-dependent pathway during atherosclerosis. Circ., 127, 1609–1619.
Fang, Y., Shi, C., Manduchi, E., Civelek, M., & Davies, P. (2010). Microrna-10a regulation of proinflammatory phenotype in athero-susceptible endothelium in vivo and in vitro. Proceedings of the National Academy of Sciences of the United States of America, 107, 13450–13455.
Qin, X., Wang, X., Wang, Y., Tang, Z., Cui, Q., Xi, J., Li, Y., Chien, S., & Wang, N. (2010). Microrna-19a mediates the suppressive effect of laminar flow on cyclin d1 expression in human umbilical vein endothelial cells. Proceedings of the National Academy of Sciences of the United States of America, 107, 3240–3244.
Wang, K., Garmire, L., Young, A., Nguyen, P., Trinh, A., Subramaniam, S., Wang, N., Shyy, J., Li, Y., & Chien, S. (2010). Role of microrna-23b in flow-regulation of rb phosphorylation and endothelial cell growth. Proceedings of the National Academy of Sciences of the United States of America, 107, 3234–3239.
Chen, K., Fan, W., Wang, X., Ke, X., Wu, G., & Hu, C. (2012). Microrna-101 mediates the suppressive effect of laminar shear stress on mtor expression in vascular endothelial cells. Biochem Biophys Com., 427, 138–142.
Hergenreider, E., Heydt, S., Treguer, K., Boettger, T., Horrevoets, A. J., Zeiher, A., Scheffer, M., Frangakis, A., Yin, X., Mayr, M., Braun, T., Urbich, C., Boon, R. A., & Dimmeler, S. (2012). Atheroprotective communication between endothelial cells and smooth muscle cells through mirnas. Nature Cell Biology, 14, 249–256.
Lovren, F., Pan, Y., Quan, A., Singh, K., Shukla, P., Gupta, N., Steer, B., Ingram, A. J., Gupta, M., Alomran, M., Teoh, H., Marsden, P., & Verma, S. (2012). Microrna-145 targeted therapy reduces atherosclerosis. Circ., 126, S81–S90.
Tian, G., Tang, Y., He, P., Lv, Y., Ouyang, X., Zhao, G., Tang, S., Wu, J., Wang, J., Peng, J., Zhang, M., Li, Y., Cayabyab, F., Zheng, X., Zhang, D., Yin, W., & Tang, C. (2014). The effects of mir-467b on lipoprotein lipase (lpl) expression, pro-inflammatory cytokine, lipid levels and atherosclerotic lesions in apolipoprotein e knockout mice. Biochemical and Biophysical Research Communications, 443, 428–434.
Wang, H., Zhu, H. Q., Wang, F., Zhou, Q., Gui, S. Y., & Wang, Y. (2013). Microrna-1 prevents high-fat diet-induced endothelial permeability in apoe knock-out mice. Molecular and Cellular Biochemistry, 378, 153–159.
Soh, J., Iqbal, J., Queiroz, J., Fernandez-Hernando, C., & Hussain, M. (2013). Microrna-30c reduces hyperlipidemia and atherosclerosis in mice by decreasing lipid synthesis and lipoprotein secretion. Nature Medicine, 19, 892–900.
Hao, X., & Fan, H. (2017). Identification of miRNAs as atherosclerosis biomarkers and functional role of miR-126 in atherosclerosis progression through MAPK signalling pathway. European Review for Medical and Pharmacological Sciences, 21, 2725–2733.
de Aguiar, V. T., Tarling, E., Kim, T., Civelek, M., Baldan, A., Esau, C., & Edwards, P. (2013). Microrna-144 regulates hepatic atp binding cassette transporter a1 and plasma high-density lipoprotein after activation of the nuclear receptor farnesoid × receptor. Circulation Research, 112, 1602–1612.
Cheng, H., Sivachandran, N., Lau, A., Boudreau, E., Zhao, J., Baltimore, D., Delgado-Olguin, P., Cybulsky, M., & Fish, J. (2013). Microrna-146 represses endothelial activation by inhibiting proinflammatory pathways. EMBO Molecular Medicine, 5, 949–966.
Zhao, Y., Li, Y., Luo, P., Gao, Y., Yang, J., Lao, K.-H., Wang, G., Cockerill, G., Hu, Y., Xu, Q., Li, T., & Zeng, L. I. (2016). XBP1 splicing triggers miR-150 transfer from smooth muscle cells to endothelial cells via extracellular vesicles. Scientific Reports, 6, 28627. https://doi.org/10.1038/srep28627.
Sun, X., He, S., Wara, A., Icli, B., Shvartz, E., Tesmenitsky, Y., Belkin, N., Li, D., Blackwell, T., Sukhova, G., Croce, K., & Feinberg, M. (2014). Systemic delivery of microrna-181b inhibits nuclear factor-kappab activation, vascular inflammation, and atherosclerosis in apolipoprotein e-deficient mice. Circulation Research, 114, 32–40.
Wang, Y., Wang, H., Liao, Y., Tsai, P., Chen, K., Cheng, H., Lin, R., & Juo, S. (2012). Microrna-195 regulates vascular smooth muscle cell phenotype and prevents neointimal formation. Cardiovascular Research, 95, 517–526.
Ong, S.-G., Lee, W., Huang, M., Dey, D., Kodo, K., Sachez-Freire, V., Gold, J., & Wu, J. (2014). Cross talk of combined gene and cell therapy in ischemic heart disease role of exosomal microRNA transfer. Circ., 130, S60–S69. https://doi.org/10.1161/CIRCULATIONAHA.113.007917.
Wang, S., Liao, J., Huang, H., Yin, H., Yang, W., & Hu, M. (2018). miR-214 and miR-126 were associated with restoration of endothelial function in obesity after exercise and dietary intervention. Journal of Applied Biomedicine, 16, 34–39. https://doi.org/10.1016/j.jab.2017.10.003.
Zhuang, G., Meng, C., Guo, X., Cheruku, P. S., Shi, L., Xu, H., Li, H., Wang, G., Evans, A. R., Safe, S., Wu, C., & Zhou, B. (2012). A novel regulator of macrophage activation: miR-223 in obesity-associated adipose tissue inflammation. Circ., 125(23), 2892–2903. https://doi.org/10.1161/CIRCULATIONAHA.111.087817.
Gidlof, O., van der Brug, M., Ohman, J., Gilje, P., Olde, B., Wahlestedt, C., & Erlinge, D. (2013). Platelets activated during myocardial infarction release functional miRNA, which can be taken up by endothelial cells and regulate ICAM1 expression. Blood, 121(19), 3908–3917, S1-26. https://doi.org/10.1182/blood-2012-10-461798.
Acknowledgments
The author thanks the librarians of the James A. Haley Hospital/University of South Florida for their assistance in providing many of the articles cited in this manuscript.
Funding
This study was supported in part by a grant from the Children’s Cardiomyopathy Foundation (002016).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of Interest
The author has received research grants from the Children’s Cardiomyopathy Foundation (002016).
Ethical Approval
This is a review article and does not contain studies by the author on either humans or animals.
Declaration
The author has no any actual or potential conflict of interest including any financial, personal, or other relationships with other people or organizations that could inappropriately influence (bias) this work.
Additional information
Associate Editor Junjie Xiao oversaw the review of this article
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Henning, R.J. Cardiovascular Exosomes and MicroRNAs in Cardiovascular Physiology and Pathophysiology. J. of Cardiovasc. Trans. Res. 14, 195–212 (2021). https://doi.org/10.1007/s12265-020-10040-5
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12265-020-10040-5