Abstract
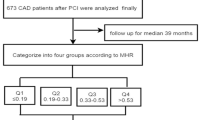
Lower level of low-density lipoprotein cholesterol (LDL-C) is paradoxically associated with increased mortality in ST elevation myocardial infarction (STEMI) patients. The underlying mechanism remains unclear. In a cohort of 220 de novo STEMI patients receiving timely primary percutaneous coronary intervention, admission LDL-C was negatively associated with circulating CD14++CD16+ monocyte counts. Moreover, admission LDL-C < 85 mg/dL was associated with increased risk for major adverse cardiovascular events (MACE) during a median follow-up of 2.7 years. After categorizing the patients according to the cutoff values of 85 mg/dL for LDL-C and the median for CD14++CD16+ monocytes, low LDL-C-associated MACE risk was only observed in those with high CD14++CD16+ monocyte counts (low LDL-C/high CD14++CD16+ monocytes vs. low LDL-C/low CD14++CD16+ monocytes: hazard ratio 5.38, 95% confidence interval 1.52 to 19.06, P = 0.009). This work provided the proof-of-principle evidence indicating a role of CD14++CD16+ monocytes in risk stratification of STEMI patients presenting with low LDL-C level.

Graphical abstract






Similar content being viewed by others
Abbreviations
- ACS:
-
Acute coronary syndrome
- ASCVD:
-
Atherosclerotic cardiovascular disease
- CANTOS:
-
Canakinumab anti-inflammatory thrombosis outcomes study
- COLCOT:
-
Colchicine cardiovascular outcomes trial
- ELISA:
-
Enzyme-linked immunosorbent assay
- FITC:
-
Fluorescein isothiocyanate
- hsCRP:
-
High sensitivity C-reactive protein
- LDL-C:
-
Low-density lipoprotein cholesterol
- LVEF:
-
Left ventricular ejection fraction
- MACE:
-
Major adverse cardiovascular events
- MI:
-
Myocardial infarction
- NSTEMI:
-
Non-ST elevation myocardial infarction
- PCI:
-
Percutaneous coronary intervention
- PE:
-
Phycoerythrin
- STEMI:
-
ST elevation myocardial infarction
References
Cholesterol Treatment Trialists Collaboration, Baigent, C., Blackwell, L., Emberson, J., Holland, L. E., Reith, C., et al. (2010). Efficacy and safety of more intensive lowering of LDL cholesterol: a meta-analysis of data from 170,000 participants in 26 randomised trials. Lancet, 376(9753), 1670–1681.
Cholesterol Treatment Trialists Collaboration, Fulcher, J., O'Connell, R., Voysey, M., Emberson, J., Blackwell, L., et al. (2015). Efficacy and safety of LDL-lowering therapy among men and women: meta-analysis of individual data from 174,000 participants in 27 randomised trials. Lancet, 385(9976), 1397–1405.
Heeschen, C., Hamm, C. W., Laufs, U., Snapinn, S., Bohm, M., White, H. D., et al. (2002). Withdrawal of statins increases event rates in patients with acute coronary syndromes. Circulation, 105(12), 1446–1452.
Spencer, F. A., Allegrone, J., Goldberg, R. J., Gore, J. M., Fox, K. A., Granger, C. B., et al. (2004). Association of statin therapy with outcomes of acute coronary syndromes: the grace study. Annals of Internal Medicine, 140(11), 857–866.
Cho, K. H., Jeong, M. H., Ahn, Y., Kim, Y. J., Chae, S. C., Hong, T. J., et al. (2010). Low-density lipoprotein cholesterol level in patients with acute myocardial infarction having percutaneous coronary intervention (the cholesterol paradox). The American Journal of Cardiology, 106(8), 1061–1068.
Nozue, T. (2016). Low-density lipoprotein cholesterol level and statin therapy in patients with acute myocardial infarction (cholesterol paradox). Circulation Journal, 80(2), 323–324.
Wang, T. Y., Newby, L. K., Chen, A. Y., Mulgund, J., Roe, M. T., Sonel, A. F., et al. (2009). Hypercholesterolemia paradox in relation to mortality in acute coronary syndrome. Clinical Cardiology, 32(9), E22–E28.
Reddy, V. S., Bui, Q. T., Jacobs, J. R., Begelman, S. M., Miller, D. P., French, W. J., et al. (2015). Relationship between serum low-density lipoprotein cholesterol and in-hospital mortality following acute myocardial infarction (the lipid paradox). The American Journal of Cardiology, 115(5), 557–562.
Weber, C., Shantsila, E., Hristov, M., Caligiuri, G., Guzik, T., Heine, G. H., et al. (2016). Role and analysis of monocyte subsets in cardiovascular disease. Joint consensus document of the European Society of Cardiology (ESC) working groups “atherosclerosis & vascular biology” and “thrombosis”. Thrombosis and Haemostasis, 116(4), 626–637.
Maekawa, Y., Anzai, T., Yoshikawa, T., Asakura, Y., Takahashi, T., Ishikawa, S., et al. (2002). Prognostic significance of peripheral monocytosis after reperfused acute myocardial infarction: a possible role for left ventricular remodeling. Journal of the American College of Cardiology, 39(2), 241–246.
Tapp, L. D., Shantsila, E., Wrigley, B. J., Pamukcu, B., & Lip, G. Y. (2012). The CD14++CD16+ monocyte subset and monocyte-platelet interactions in patients with ST-elevation myocardial infarction. Journal of Thrombosis and Haemostasis, 10(7), 1231–1241.
Shantsila, E., Ghattas, A., Griffiths, H. R., & Lip, G. Y. H. (2019). Mon2 predicts poor outcome in ST-elevation myocardial infarction. Journal of Internal Medicine, 285(3), 301–316.
Zhou, X., Liu, X. L., Ji, W. J., Liu, J. X., Guo, Z. Z., Ren, D., et al. (2016). The kinetics of circulating monocyte subsets and monocyte-platelet aggregates in the acute phase of ST-elevation myocardial infarction: associations with 2-year cardiovascular events. Medicine, 95(18), e3466.
Zeng, S., Yan, L. F., Luo, Y. W., Liu, X. L., Liu, J. X., Guo, Z. Z., et al. (2018). Trajectories of circulating monocyte subsets after ST-elevation myocardial infarction during hospitalization: latent class growth modeling for high-risk patient identification. Journal of Cardiovascular Translational Research, 11(1), 22–32.
Zhou, X., Li, J., Guo, J., Geng, B., Ji, W., Zhao, Q., et al. (2018). Gut-dependent microbial translocation induces inflammation and cardiovascular events after ST-elevation myocardial infarction. Microbiome, 6(1), 66.
Ridker, P. M., Everett, B. M., Thuren, T., MacFadyen, J. G., Chang, W. H., Ballantyne, C., et al. (2017). Antiinflammatory therapy with canakinumab for atherosclerotic disease. The New England Journal of Medicine, 377(12), 1119–1131.
Tardif, J. C., Kouz, S., Waters, D. D., Bertrand, O. F., Diaz, R., Maggioni, A. P., et al. (2019). Efficacy and safety of low-dose colchicine after myocardial infarction. The New England Journal of Medicine, 381(26), 2497–2505.
Zuurbier, C. J., Abbate, A., Cabrera-Fuentes, H. A., Cohen, M. V., Collino, M., De Kleijn, D. P. V., et al. (2019). Innate immunity as a target for acute cardioprotection. Cardiovascular Research, 115(7), 1131–1142.
Azzam, K. M., & Fessler, M. B. (2012). Crosstalk between reverse cholesterol transport and innate immunity. Trends in Endocrinology and Metabolism, 23(4), 169–178.
Task Force on the management of ST segment elevation acute myocardial infarction of the European Society of Cardiology, Steg, P. G., James, S. K., Atar, D., Badano, L. P., Blomstrom-Lundqvist, C., et al. (2012). ESC guidelines for the management of acute myocardial infarction in patients presenting with ST-segment elevation. European Heart Journal, 33(20), 2569–2619.
Chinese Society of Cardiology. (2012). Guidelines for the management of acute coronary syndromes in patients presenting without persistent ST-segment elevation. Chinese Journal of Cardiology, 40(5), 353–367.
Zhou, X., Zhang, L., Ji, W. J., Yuan, F., Guo, Z. Z., Pang, B., et al. (2013). Variation in dietary salt intake induces coordinated dynamics of monocyte subsets and monocyte-platelet aggregates in humans: implications in end organ inflammation. PLoS One, 8(4), e60332.
Ma, Y. C., Zuo, L., Chen, J. H., Luo, Q., Yu, X. Q., Li, Y., et al. (2006). Modified glomerular filtration rate estimating equation for Chinese patients with chronic kidney disease. Journal of the American Society of Nephrology, 17(10), 2937–2944.
Lu, Y. W., Lu, S. F., Chou, R. H., Wu, P. S., Ku, Y. C., Kuo, C. S., et al. (2019). Lipid paradox in patients with acute myocardial infarction: potential impact of malnutrition. Clinical Nutrition, 38(5), 2311–2318.
Ravnskov, U., Diamond, D. M., Hama, R., Hamazaki, T., Hammarskjold, B., Hynes, N., et al. (2016). Lack of an association or an inverse association between low-density-lipoprotein cholesterol and mortality in the elderly: a systematic review. BMJ Open, 6(6), e010401.
Myasoedova, E., Crowson, C. S., Kremers, H. M., Roger, V. L., Fitz-Gibbon, P. D., Therneau, T. M., et al. (2011). Lipid paradox in rheumatoid arthritis: the impact of serum lipid measures and systemic inflammation on the risk of cardiovascular disease. Annals of the Rheumatic Diseases, 70(3), 482–487.
Robertson, J., Peters, M. J., McInnes, I. B., & Sattar, N. (2013). Changes in lipid levels with inflammation and therapy in RA: a maturing paradigm. Nature Reviews Rheumatology, 9(9), 513–523.
Avina-Zubieta, J. A., Thomas, J., Sadatsafavi, M., Lehman, A. J., & Lacaille, D. (2012). Risk of incident cardiovascular events in patients with rheumatoid arthritis: a meta-analysis of observational studies. Annals of the Rheumatic Diseases, 71(9), 1524–1529.
Oduncu, V., Erkol, A., Kurt, M., Tanboga, I. H., Karabay, C. Y., Sengul, C., et al. (2013). The prognostic value of very low admission LDL-cholesterol levels in ST-segment elevation myocardial infarction compared in statin-pretreated and statin-naive patients undergoing primary percutaneous coronary intervention. International Journal of Cardiology, 167(2), 458–463.
Ridker, P. M. (2017). How common is residual inflammatory risk? Circulation Research, 120(4), 617–619.
Guedeney, P., Claessen, B. E., Kalkman, D. N., Aquino, M., Sorrentino, S., Giustino, G., et al. (2019). Residual inflammatory risk in patients with low LDL cholesterol levels undergoing percutaneous coronary intervention. Journal of the American College of Cardiology, 73(19), 2401–2409.
Penson, P. E., Long, D. L., Howard, G., Toth, P. P., Muntner, P., Howard, V. J., et al. (2018). Associations between very low concentrations of low density lipoprotein cholesterol, high sensitivity c-reactive protein, and health outcomes in the reasons for geographical and racial differences in stroke (REGARDS) study. European Heart Journal, 39(40), 3641–3653.
Bohula, E. A., Giugliano, R. P., Leiter, L. A., Verma, S., Park, J. G., Sever, P. S., et al. (2018). Inflammatory and cholesterol risk in the FOURIER trial. Circulation, 138(2), 131–140.
Vreugdenhil, A. C., Rousseau, C. H., Hartung, T., Greve, J. W., van ‘t Veer, C., & Buurman, W. A. (2003). Lipopolysaccharide (LPS)-binding protein mediates LPS detoxification by chylomicrons. Journal of Immunology, 170(3), 1399–1405.
Feng, Q., Wei, W. Q., Chaugai, S., Leon, B. G. C., Mosley, J. D., Leon, D. A. C., et al. (2019). Association between low-density lipoprotein cholesterol levels and risk for sepsis among patients admitted to the hospital with infection. JAMA Network Open, 2(1), e187223.
Kaysen, G. A., Ye, X., Raimann, J. G., Wang, Y., Topping, A., Usvyat, L. A., et al. (2018). Lipid levels are inversely associated with infectious and all-cause mortality: international mondo study results. Journal of Lipid Research, 59(8), 1519–1528.
Baartscheer, A., Schumacher, C. A., Wekker, V., Verkerk, A. O., Veldkamp, M. W., van Oort, R. J., et al. (2015). Dyscholesterolemia protects against ischemia-induced ventricular arrhythmias. Circulation. Arrhythmia and Electrophysiology, 8(6), 1481–1490.
Dekker, L. R., Bezzina, C. R., Henriques, J. P., Tanck, M. W., Koch, K. T., Alings, M. W., et al. (2006). Familial sudden death is an important risk factor for primary ventricular fibrillation: a case-control study in acute myocardial infarction patients. Circulation, 114(11), 1140–1145.
Li, M., Huang, Y., Du, X., Li, S., Ji, J., Patel, A., et al. (2016). Impact of prior use of four preventive medications on outcomes in patients hospitalized for acute coronary syndrome--results from CPACS-2 study. PLoS One, 11(9), e0163068.
Imanishi, T., Ikejima, H., Tsujioka, H., Kuroi, A., Ishibashi, K., Komukai, K., et al. (2010). Association of monocyte subset counts with coronary fibrous cap thickness in patients with unstable angina pectoris. Atherosclerosis, 212(2), 628–635.
Ammirati, E., Cannistraci, C. V., Cristell, N. A., Vecchio, V., Palini, A. G., Tornvall, P., et al. (2012). Identification and predictive value of interleukin-6+ interleukin-10+ and interleukin-6- interleukin-10+ cytokine patterns in ST-elevation acute myocardial infarction. Circulation Research, 111(10), 1336–1348.
Foster, G. A., Gower, R. M., Stanhope, K. L., Havel, P. J., Simon, S. I., & Armstrong, E. J. (2013). On-chip phenotypic analysis of inflammatory monocytes in atherogenesis and myocardial infarction. Proceedings of the National Academy of Sciences of the United States of America, 110(34), 13944–13949.
Funding
This work was supported by the National Natural Science Foundation of China (81970304) and Tianjin Municipal Science and Technology Commission (18ZXZNSY00290).
Author information
Authors and Affiliations
Corresponding authors
Ethics declarations
Conflict of Interest
The authors declare that they have no conflict of interest.
Research Involving Human Subjects
All procedures followed were in accordance with the ethical standards of the Ethical Committee of Pingjin Hospital on human experimentation and with the Helsinki Declaration of 1975, as revised in 2000.
Informed Consent
Informed consent was obtained from all patients for being included in the study.
Additional information
Associate Editor Junjie Xiao oversaw the review of this article
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Dong, S., Ji, W., Zeng, S. et al. Admission Low-Density Lipoprotein Cholesterol Stratified by Circulating CD14++CD16+ Monocytes and Risk for Recurrent Cardiovascular Events Following ST Elevation Myocardial Infarction: Lipid Paradox Revised. J. of Cardiovasc. Trans. Res. 13, 916–927 (2020). https://doi.org/10.1007/s12265-020-10015-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12265-020-10015-6