Abstract
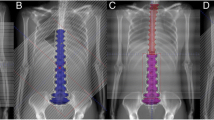
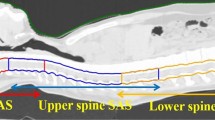
In radiotherapy involving craniospinal irradiation (CSI), field junctions of therapeutic beams are necessary, because a CSI target is generally several times larger than the maximum field size of the beams. The purpose of this study was to develop a simplified method for estimating dose uniformity around the field junctions in proton CSI. We estimated the dose profiles around the field junctions of proton beams using a simplified field-junction model, in which partial lateral dose distributions around the field edge were assumed to be approximated using the error function. We measured the lateral dose distributions of the proton beams planned for the CSI treatment using a two-dimensional (2D) ionization chamber array. Although dose hot spots and cold spots tend to be underestimated by a chamber array because of the partial volume effect of the sensitive volume and discrete chamber positions, the model estimation results were fairly consistent with the measurements obtained using a 2D chamber array subjected to CSI-simulated serial irradiation. The simplified junction model enabled us to estimate the dose distributions and dependence of the setup position gap on the dose uniformity around the field junctions on the basis of the field-by-field dose profiles measured using the 2D chamber array.








Similar content being viewed by others
References
Wilson RR. Radiological use of fast protons. Radiology. 1946;47:487–91.
International Commission on Radiation Units and Measurements (ICRU). Prescribing, Recording, and Reporting Proton-Beam Therapy. ICRU Report 78. Bethesda: MD; 2007. p. 17–20.
Yuh GE, Loredo LN, Yonemoto LT, Bush DA, Shahnazi K, Preston W, Slater JM, Slater JD. Reducing toxicity from craniospinal irradiation: using proton beams to treat medulloblastoma in young children. Cancer J. 2004;10:386–90.
Howell RM, Giebeler A, Koontz-Raisig W, Mahajan A, Etzel CJ, D’Amelio AM, Homann KL, Newhauser WD. Comparison of therapeutic dosimetric data from passively scattered proton and photon craniospinal irradiations for medulloblastoma. Radiat Oncol. 2012;7:116.
Brown AP, Barney CL, Grosshans DR, McAleer MF, De Groot JF, Puduvalli VK, Tucker SL, Crawford CN, Khan M, Khatua S, Gilbert MR, Brown PD, Mahajan A. Proton beam craniospinal irradiation reduces acute toxicity for adults with medulloblastoma. Int J Radiat Oncol Biol Phys. 2013;86:277–84.
Cheng CW, Das IJ, Srivastava SP, Zhao L, Wolanski M, Simmons J, Johnstone PA, Buchsbaum JC. Dosimetric comparison between proton and photon beams in the moving gap region in cranio-spinal irradiation (CSI). Acta Oncol. 2013;52:553–60.
Titt U, Zheng Y, Vassiliev ON, Newhauser WD. Monte Carlo investigation of collimator scatter of proton-therapy beams produced using the passive scattering method. Phys Med Biol. 2008;53:487–504.
Kase Y, Yamashita H, Sakama M, Mizota M, Maeda Y, Tameshige Y, Murayama S. Semi-analytical model for output factor calculations in proton beam therapy with consideration for the collimator aperture edge. Phys Med Biol. 2015;60:5833–52.
Renner T, Chu WT. Wobbler facility for biomedical experiments. Med Phys. 1987;14:825–34.
Hong L, Goitein M, Bucciolini M, Comiskey R, Gottschalk B, Rosenthal S, Serago C, Urie M. A pencil beam algorithm for proton dose calculations. Phys Med Biol. 1996;41:1305–30.
Kanematsu N, Akagi T, Futami Y, Higashi A, Kanai T, Matsufuji N, Tomura H, Yamashita H. A proton dose calculation code for treatment planning based on the pencil beam algorithm. Japan J Med Phys. 1998;18:88–103.
Kanematsu N, Matsufuji N, Kohno R, Minohara S, Kanai T. A CT calibration method based on the polybinary tissue model for radiotherapy treatment planning. Phys Med Biol. 2003;48:1053–64.
Yom SS, Frija EK, Mahajan A, Chang E, Klein K, Shiu A, Ohrt J, Woo S. Field-in-field technique with intrafractionally modulated junction shifts for craniospinal irradiation. Int J Radiat Oncol Biol Phys. 2007;69:1193–8.
Stoker JB, Grant J, Zhu XR, Pidikiti R, Mahajan A, Grosshans DR. Intensity modulated proton therapy for craniospinal irradiation: organ-at-risk exposure and a low-gradient junctioning technique. Int J Radiat Oncol Biol Phys. 2014;90:637–44.
Hadley A, Ding GX. A single-gradient junction technique to replace multiple-junction shifts for craniospinal irradiation treatment. Med Dosim. 2015;39:314–9.
Okonogi N, Hashimoto T, Ishida M, Ohno T, Terunuma T, Okumura T, Sakae T, Sakurai H. Designed-seamless irradiation technique for extended whole mediastinal proton-beam irradiation for esophageal cancer. Radiat Oncol. 2012;7:173.
Lin H, Ding X, Kirk M, Liu H, Zhai H, Hill-Kayser CE, Lustig RA, Tochner Z, Both S, McDonough J. Supine craniospinal irradiation using a proton pencil beam scanning technique without match line changes for field junctions. Int J Radiat Oncol Biol Phys. 2014;90:71–8.
Acknowledgments
We thank all the staff of the Radiation and Proton Therapy Center in the Shizuoka Cancer Center, and we thank the Mitsubishi Electric Corporation for their expert support with the proton beam irradiation.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflicts of interest.
About this article
Cite this article
Yamashita, H., Kase, Y. & Murayama, S. Simplified estimation method for dose distributions around field junctions in proton craniospinal irradiation. Radiol Phys Technol 10, 95–105 (2017). https://doi.org/10.1007/s12194-016-0373-2
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12194-016-0373-2