Abstract
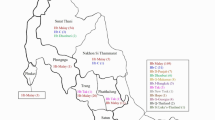
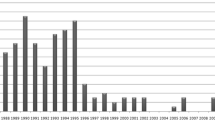
Genotypes of 260 individuals with hemoglobin H (Hb H) disease originating from various provinces in southern Thailand were characterized by multiplex PCR (M-PCR) and reverse dot blot hybridization (RDB). M-PCR was used to amplify target fragments and then hybridized with allele-specific oligonucleotide (ASO) probes which were bound on a nylon membrane. A total of eight α-thalassemia (α-thal) mutations, which produced eight Hb H disease genotypes (α0-thal/α+-thal), were detected. The most common form of α0-thal was −SEA with a frequency of 99.23%. The other form (0.77%) of α0-thal mutation was a THAI deletion (−THAI). The deletional α+-thal mutations comprised 3.7 kb (-α3.7) and 4.2 kb (-α4.2) deletions which were found in 172 (66.15%) and 5 (1.92%) alleles, respectively. The incidence of non-deletional α+-thal in decreasing order was Hb Constant Spring (Hb CS, αCS) 28.85%, Hb Quong Sze (Hb QS, αQS) 1.54%, and Hb Paksé (Hb PS, αPS) 0.77%. The genotype characterization of Hb H disease and the development of the RDB technic for detection of α-thal mutations presented in this study enable the prenatal diagnosis of Hb Bart’s hydrops fetalis syndrome.


Similar content being viewed by others
References
Origa R, Moi P. (2016) Alpha-Thalassemia. GeneReviews® [Internet]. https://www.ncbi.nlm.nih.gov/books/NBK1435/ (cited 2017 Oct 20).
Chui DHK. Thalassemia. Hb H disease and Hb Bart’s hydrops fetalis. Ann N Y Acad Sci. 2005;1054:25–32.
Xu XM, Zhou YQ, Luo GX, Liao C, Zhou M, Chen PY, et al. The prevalence and spectrum of alpha and beta thalassaemia in Guangdong province: implications for the future health burden and population screening. J Clin Pathol. 2004;57:517–22.
Fucharoen S, Winichagoon P. Haemoglobinopathies in Southeast Asia. Indian J Med Res. 2011;134:498–506.
Chui DHK, Fucharoen S, Chan V. Hemoglobin H disease: not necessarily a benign disorder. Blood. 2003;101:791–800.
Pharephan S, Sirivatanapa P, Makonkawkeyoon S, Tuntiwechapikul W, Makonkawkeyoon L. Prevalence of α-thalassaemia genotypes in pregnant women in northern Thailand. Indian J Med Res. 2016;143:315–22.
Giardine B, van Baal S, Kaimakis P, Riemer C, Miller W, Samara M, et al. HbVar database of human hemoglobin variants and thalassemia mutations: 2007 update. Hum Mutat. 2007;28:206.
Lin M, Zhu JJ, Wang Q, Xie LX, Lu M, Wang JL, et al. Development and evaluation of a reverse dot blot assay for the simultaneous detection of common alpha and beta thalassemia in Chinese. Blood Cells Mol Dis. 2012;48:86–90.
Chan V, Yam I, Chen FE, Chan TK. A reverse dot-blot method for rapid detection of non-deletion alpha thalassaemia. Br J Haematol. 1999;104:513–5.
Ye BC1, Zhang Z, Lei Z. Oligonucleotide array for detection of common severe determinants of alpha thalassemia. J Biotechnol. 2005;115:1–9.
Zesong L, Ruijun G, Wen Z. Rapid detection of deletional alpha-thalassemia by an oligonucleotide microarray. Am J Hematol. 2005;80:306–8.
Baysal E, Huisman THJ. Detection of common deletional α-thalassaemia-2 determinants by PCR. Am J Hematol. 1994;46:208–13.
Chong SS, Boehm CD, Higgs DR, Cutting GR. Single-tube multiplex-PCR screen for common deletional determinants of α-thalassemia. Blood. 2000;95:360–2.
Liu YT, Old JM, Fisher CA, Weatherall DJ, Clegg JB. Rapid detection of α-thalassaemia deletions andα-globin gene triplication by multiplex polymerase chain reactions. Br J Haematol. 2000;108:295–9.
Chen TP, Liu TC, Chang CS, Chang JG, Tsai HJ, Lin SF. PCR-based analysis of alpha-thalassemia in Southern Taiwan. Int J Hematol. 2002;75:277–80.
Foglietta E, Bianco I, Maggio A, Giambona A. Rapid detection of six common Mediterranean and three non-Mediterranean α-thalassemia point mutations by reverse dot blot. Am J Hematol. 2003;74:191–5.
Puehringer H, Najmabadi H, Law HY, Krugluger W, Viprakasit V, Pissard S, et al. Validation of a reverse-hybridization StripAssay for the simultaneous analysis of common alpha-thalassemia point mutations and deletions. Clin Chem Lab Med. 2007;45:605–10.
Winichagoon P, Fucharoen S, Wasi P. The molecular basis of alpha-thalassemia in Thailand. Southeast Asian J Trop Med Public Health. 1992;23(Suppl 2):7–13.
Lithanatudom P, Khampan P, Duncan RS, Svasti S, Fucharoen S, Kangwanpong D, et al. The prevalence of alpha-thalassemia amongst Tai and Mon-Khmer ethnic groups residing in northern Thailand: a population-based study. Hematology. 2016;21:480–5.
Laosombat V, Viprakasit V, Chotsampancharoen T, Wongchanchailert M, Khodchawan S, Chinchang W, et al. Clinical features and molecular analysis in Thai patients with Hb H disease. Ann Hematol. 2009;88:1185–92.
Pornprasert S, Punyamung M. Detection of compound heterozygous of Hb constant spring and Hb Q-Thailand by capillary electrophoresis and high performance liquid chromatography. Indian J Hematol Blood Transfus. 2015;31:229–32.
Charoenkwan P, Taweephon R, Sae-Tung R, Thanarattanakorn P, Sanguansermsri T. Molecular and clinical features of Hb H disease in northern Thailand. Hemoglobin. 2005;29:133–40.
Yang Y, Lou JW, Liu YH, He Y, Li DZ. Screening and diagnosis of Hb Quong Sze [HBA2: c.377T> C (or HBA1)] in a prenatal control program for thalassemia. Hemoglobin. 2014;38:158–60.
Sanguansermsri T, Matragoon S, Changloah L, Flatz G. Hemoglobin Suan-Dok (α2 109(G16)LEU-ARGβ2). an unstable variant associated with α-thalassemia. Hemoglobin. 1979;3:161.
Bang-Ce Y, Hongqiong L, Zhuanfong Z, et al. Simultaneous detection of alpha-thalassemia and beta-thalassemia by oligonucleotide microarray. Haematologica. 2004;89:1010–2.
Old J, Henderson S. Molecular diagnostics for haemoglobinopathies. Expert Opin Med Diagn. 2010;4:225–40.
Harteveld CL, Kleanthous M, Traeger-Synodinos J. Prenatal diagnosis of hemoglobin disorders: present and future strategies. Clin Biochem. 2009;42:1767–79.
Acknowledgements
The authors thank the staff of the Hematology and Thalassemia Laboratory of the Department of Pathology, Faculty of Medicine, Prince of Songkla University for the technical support. This work was supported by a Grant (REC 57-005-04-6-2) from the Faculty of Medicine, Prince of Songkla University. The sponsors of this study are public or nonprofit organizations that support science in general.
Author information
Authors and Affiliations
Contributions
KN performed the research, analyzed the data, and wrote the manuscript. CN designed the research study, interpreted the data, and edited the manuscript. Final version of the article was read and approved by all of the authors.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interests regarding the publication of this paper.
About this article
Cite this article
Nittayaboon, K., Nopparatana, C. Molecular characterization of Hb H disease in southern Thailand. Int J Hematol 108, 384–389 (2018). https://doi.org/10.1007/s12185-018-2494-3
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12185-018-2494-3