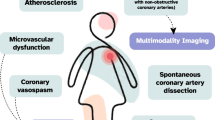
Abstract
Cardiovascular disease remains the leading cause of death for women in the USA. While it is clear that gender-specific differences in presentation, pathophysiology, and outcomes exist among men and women presenting with acute coronary syndromes (ACS), efforts to better understand and to improve recognition and outcomes for women with ACS continue. Past studies have shown differences in age, presentation, comorbidities, extent of disease, management, and outcomes for women presenting with ACS compared with men. This review will highlight these differences and provide current knowledge regarding potential mechanisms underlying the observed differences.
Similar content being viewed by others
References
Papers of particular interest, published recently, have been highlighted as: • Of importance •• Of major importance
Murphy SL, Xu J, Kochanek KD. Deaths: final data for 2010. Natl Vital Stat Rep. 2013;61(4):1–117.
Kennedy JW et al. The clinical spectrum of coronary artery disease and its surgical and medical management, 1974–1979. The Coronary Artery Surgery Study. Circulation. 1982;66(5 Pt 2):III16–23.
Bairey Merz N et al. Women’s ischemic syndrome evaluation: current status and future research directions: report of the national heart, lung and blood institute workshop: October 2–4, 2002: executive summary. Circulation. 2004;109(6):805–7.
Reynolds HR et al. Mechanisms of myocardial infarction in women without angiographically obstructive coronary artery disease. Circulation. 2011;124(13):1414–25.
Lee BK et al. Invasive evaluation of patients with angina in the absence of obstructive coronary artery disease. Circulation. 2015;131(12):1054–60. This study revealed that a substantial number of patients presenting with angina without evidence of obstructive coronary disease still have evidence of occult coronary abnormalities including atherosclerosis by IVUS, endothelial dysfunction, microvascular impairment, or abnormal fractional flow reserve on invasive evaluation.
De Ferrari GM et al. Outcomes among non-ST-segment elevation acute coronary syndromes patients with no angiographically obstructive coronary artery disease: observations from 37,101 patients. Eur Heart J Acute Cardiovasc Care. 2014;3(1):37–45. This study examined outcomes in patients presenting with NSTEMI found to have non-obstructive CAD. They found that the population was younger, more likely to be female, and less likely to have a history of previous MI or revascularization. However, they found that rates of 30-day death or MI, although lower than those with obstructive CAD, were not insignificant at 2.2%, highlighting the need for a better understanding of this unique patient population and specific management strategies for this group.
Gulati M et al. Adverse cardiovascular outcomes in women with nonobstructive coronary artery disease: a report from the Women’s Ischemia Syndrome Evaluation Study and the St James Women Take Heart Project. Arch Intern Med. 2009;169(9):843–50.
Go AS et al. Heart disease and stroke statistics–2014 update: a report from the American Heart Association. Circulation. 2014;129(3):e28–292.
Duvernoy CS. Coronary heart disease in women: what do we know now? Future Cardiol. 2005;1(5):617–28.
Lin CF et al. Sex differences in the treatment and outcome of patients with acute coronary syndrome after percutaneous coronary intervention: a population-based study. J Womens Health (Larchmt). 2014;23(3):238–45.
Hochman JS et al. Sex, clinical presentation, and outcome in patients with acute coronary syndromes. Global Use of Strategies to Open Occluded Coronary Arteries in Acute Coronary Syndromes IIb Investigators. N Engl J Med. 1999;341(4):226–32.
Egan BM, Zhao Y, Axon RN. US trends in prevalence, awareness, treatment, and control of hypertension, 1988–2008. JAMA. 2010;303(20):2043–50.
Lansky AJ et al. Gender and the extent of coronary atherosclerosis, plaque composition, and clinical outcomes in acute coronary syndromes. JACC Cardiovasc Imaging. 2012;5(3 Suppl):S62–72.
Cowie CC et al. Full accounting of diabetes and pre-diabetes in the U.S. population in 1988–1994 and 2005–2006. Diabetes Care. 2009;32(2):287–94.
Duvernoy CS et al. Gender differences in adverse outcomes after contemporary percutaneous coronary intervention: an analysis from the Blue Cross Blue Shield of Michigan Cardiovascular Consortium (BMC2) percutaneous coronary intervention registry. Am Heart J. 2010;159(4):677–83. e1.
Gupta A et al. Trends in acute myocardial infarction in young patients and differences by sex and race, 2001 to 2010. J Am Coll Cardiol. 2014;64(4):337–45. This study revealed that younger women presenting with ACS may represent a particularly high risk group with more comorbidities, longer hospitalizations, and higher in-hospital mortality compared to young men.
Towfighi A, Markovic D, Ovbiagele B. National gender-specific trends in myocardial infarction hospitalization rates among patients aged 35 to 64 years. Am J Cardiol. 2011;108(8):1102–7.
Davis M et al. Acute coronary syndrome in young women under 55 years of age: clinical characteristics, treatment, and outcomes. Clin Res Cardiol. 2015. doi: 10.1007/s00392-015-0827-2 .This study showed that young women, <55 years of age, presenting with ACS had more comorbidities than older women, underwent less invasive evaluation, and were less likely to receive evidence based medical therapy. This study highlights the need to aggressively screen for and treat modifiable risk factors in this population.
Davis MB et al. Characteristics and outcomes of women veterans undergoing cardiac catheterization in the Veterans Affairs Healthcare System: insights from the VA CART Program. Circ Cardiovasc Qual Outcomes. 2015;8(2 Suppl 1):S39–47. This study revealed a unique subset of women, veterans, presenting with angina who are more likely to have non-traditional cardiac risk factors including obesity, depression, and PTSD. These women had less obstructive CAD at catheterization and lower 1-year mortality as well as re-hospitalization rates, suggesting a potential alternate etiology for their angina.
Kubzansky LD et al. Prospective study of posttraumatic stress disorder symptoms and coronary heart disease in the normative aging study. Arch Gen Psychiatry. 2007;64(1):109–16.
Tan G et al. Associations among pain, PTSD, mTBI, and heart rate variability in veterans of operation enduring and Iraqi freedom: a pilot study. Pain Med. 2009;10(7):1237–45.
Ho KY et al. Non-cardiac, non-oesophageal chest pain: the relevance of psychological factors. Gut. 1998;43(1):105–10.
Rasul F et al. Common mental disorder and physical illness in the Renfrew and Paisley (MIDSPAN) study. J Psychosom Res. 2002;53(6):1163–70.
Christoph M et al. Mental symptoms in patients with cardiac symptoms and normal coronary arteries. Open Heart. 2014;1(1):e000093. This study revealed that in patients with cardiac symptoms and normal coronary arteries at catheterization, there is a much higher prevalence of mental health symptoms.
Arslanian-Engoren C et al. Symptoms of men and women presenting with acute coronary syndromes. Am J Cardiol. 2006;98(9):1177–81.
Milner KA et al. Gender and age differences in chief complaints of acute myocardial infarction (Worcester Heart Attack Study). Am J Cardiol. 2004;93(5):606–8.
Meshack AF et al. Comparison of reported symptoms of acute myocardial infarction in Mexican Americans versus non-Hispanic whites (the Corpus Christi Heart Project). Am J Cardiol. 1998;82(11):1329–32.
Kreatsoulas C et al. Reconstructing angina: cardiac symptoms are the same in women and men. JAMA Intern Med. 2013;173(9):829–31. This study looked at symptom descriptors of patients with cardiac symptoms undergoing their first catheterization, and found no significant difference in symptom descriptions between women and men, with the most common descriptors for both sexes being chest pain, pressure, or tightness.
Gibler WB et al. Persistence of delays in presentation and treatment for patients with acute myocardial infarction: the GUSTO-I and GUSTO-III experience. Ann Emerg Med. 2002;39(2):123–30.
Dracup K, Moser DK. Beyond sociodemographics: factors influencing the decision to seek treatment for symptoms of acute myocardial infarction. Heart Lung. 1997;26(4):253–62.
Yarzebski J et al. Gender differences and factors associated with the receipt of thrombolytic therapy in patients with acute myocardial infarction: a community-wide perspective. Am Heart J. 1996;131(1):43–50.
O’Donoghue M et al. Early invasive vs conservative treatment strategies in women and men with unstable angina and non-ST-segment elevation myocardial infarction: a meta-analysis. JAMA. 2008;300(1):71–80.
Kornowski R et al. A comparative analysis of major clinical outcomes with drug-eluting stents versus bare metal stents in male versus female patients. EuroIntervention. 2012;7(9):1051–9.
Stefanini GG et al. Safety and efficacy of drug-eluting stents in women: a patient-level pooled analysis of randomised trials. Lancet. 2013;382(9908):1879–88. This meta-analysis looked at 11,557 women undergoing percutaneous intervention to determine the safety and efficacy of DES. They found that the use of DES resulted in lower rate of death or MI as well as a better safety profile and lower rates of target lesion revascularization compared to older generation DES or BMS.
Malenka DJ et al. Differences in outcomes between women and men associated with percutaneous transluminal coronary angioplasty. A regional prospective study of 13,061 procedures. Northern New England Cardiovascular Disease Study Group. Circulation. 1996;94(9 Suppl):II99–104.
Mehilli J et al. Differences in prognostic factors and outcomes between women and men undergoing coronary artery stenting. JAMA. 2000;284(14):1799–805.
Daly C et al. Gender differences in the management and clinical outcome of stable angina. Circulation. 2006;113(4):490–8.
Hvelplund A et al. Women with acute coronary syndrome are less invasively examined and subsequently less treated than men. Eur Heart J. 2010;31(6):684–90.
Pancholy SB et al. Sex differences in short-term and long-term all-cause mortality among patients with ST-segment elevation myocardial infarction treated by primary percutaneous intervention: a meta-analysis. JAMA Intern Med. 2014;174(11):1822–30. This meta-analysis examined differences in mortality by sex of patients presenting with STEMI. They found that after adjustment for baseline cardiovascular risk factors, there was no significant difference in 1-year mortality between men and women, arguing against the previously held thought that women have higher mortality than men.
Iakovou I et al. Gender differences in clinical outcome after coronary artery stenting with use of glycoprotein IIb/IIIa inhibitors. Am J Cardiol. 2002;89(8):976–9.
Ashby DT et al. Comparison of outcomes in men versus women having percutaneous coronary interventions in small coronary arteries. Am J Cardiol. 2003;91(8):979.
Peterson ED et al. Effect of gender on the outcomes of contemporary percutaneous coronary intervention. Am J Cardiol. 2001;88(4):359–64.
Latif F et al. In-hospital and 1-year outcomes among percutaneous coronary intervention patients with chronic kidney disease in the era of drug-eluting stents: a report from the EVENT (Evaluation of Drug Eluting Stents and Ischemic Events) registry. JACC Cardiovasc Interv. 2009;2(1):37–45.
Rubenstein MH et al. Are patients with renal failure good candidates for percutaneous coronary revascularization in the new device era? Circulation. 2000;102(24):2966–72.
Best PJ et al. The impact of renal insufficiency on clinical outcomes in patients undergoing percutaneous coronary interventions. J Am Coll Cardiol. 2002;39(7):1113–9.
Kahn JK et al. Short- and long-term outcome of percutaneous transluminal coronary angioplasty in chronic dialysis patients. Am Heart J. 1990;119(3 Pt 1):484–9.
Lansky AJ et al. Gender differences in outcomes after primary angioplasty versus primary stenting with and without abciximab for acute myocardial infarction: results of the Controlled Abciximab and Device Investigation to Lower Late Angioplasty Complications (CADILLAC) trial. Circulation. 2005;111(13):1611–8.
Lansky AJ et al. Percutaneous coronary intervention and adjunctive pharmacotherapy in women: a statement for healthcare professionals from the American Heart Association. Circulation. 2005;111(7):940–53.
Antman EM et al. ACC/AHA guidelines for the management of patients with ST-elevation myocardial infarction; a report of the American college of cardiology/American Heart Association Task Force on Practice Guidelines (Committee to Revise the 1999 Guidelines for the Management of Patients with Acute Myocardial Infarction). J Am Coll Cardiol. 2004;44(3):E1–211.
Amsterdam EA et al. 2014 AHA/ACC Guideline for the management of patients with non-ST-elevation acute coronary syndromes: a report of the American College of Cardiology/American Heart Association Task Force on Practice Guidelines. J Am Coll Cardiol. 2014;64(24):e139–228.
Shaw LJ et al. Gender differences in the noninvasive evaluation and management of patients with suspected coronary artery disease. Ann Intern Med. 1994;120(7):559–66.
Mark DB et al. Absence of sex bias in the referral of patients for cardiac catheterization. N Engl J Med. 1994;330(16):1101–6.
Roeters van Lennep JE et al. Gender differences in diagnosis and treatment of coronary artery disease from 1981 to 1997. No evidence for the Yentl syndrome. Eur Heart J. 2000;21(11):911–8.
Bowker TJ et al. A national Survey of Acute Myocardial Infarction and Ischaemia (SAMII) in the U.K.: characteristics, management and in-hospital outcome in women compared to men in patients under 70 years. Eur Heart J. 2000;21(17):1458–63.
Blomkalns AL et al. Gender disparities in the diagnosis and treatment of non-ST-segment elevation acute coronary syndromes: large-scale observations from the CRUSADE (Can Rapid Risk Stratification of Unstable Angina Patients Suppress Adverse Outcomes With Early Implementation of the American College of Cardiology/American Heart Association Guidelines) National Quality Improvement Initiative. J Am Coll Cardiol. 2005;45(6):832–7.
Alfredsson J et al. Gender differences in management and outcome in non-ST-elevation acute coronary syndrome. Heart. 2007;93(11):1357–62.
Shehab A et al. Gender disparities in the presentation, management and outcomes of acute coronary syndrome patients: data from the 2nd Gulf Registry of Acute Coronary Events (Gulf RACE-2). PLoS One. 2013;8(2):e55508.
Shehab A et al. Gender differences in acute coronary syndrome in Arab Emirati women–implications for clinical management. Angiology. 2013;64(1):9–14.
Song XT et al. Gender based differences in patients with acute coronary syndrome: findings from Chinese Registry of Acute Coronary Events (CRACE). Chin Med J (Engl). 2007;120(12):1063–7.
Witt BJ et al. Cardiac rehabilitation after myocardial infarction in the community. J Am Coll Cardiol. 2004;44(5):988–96.
Suaya JA et al. Use of cardiac rehabilitation by Medicare beneficiaries after myocardial infarction or coronary bypass surgery. Circulation. 2007;116(15):1653–62.
Jespersen L et al. Stable angina pectoris with no obstructive coronary artery disease is associated with increased risks of major adverse cardiovascular events. Eur Heart J. 2012;33(6):734–44.
Bugiardini R, Bairey Merz CN. Angina with “normal” coronary arteries: a changing philosophy. JAMA. 2005;293(4):477–84.
Berger JS et al. Sex differences in mortality following acute coronary syndromes. JAMA. 2009;302(8):874–82.
Dey S et al. Treatment bias against women with acute coronary syndrome: fact or fantasy? J Am Coll Cardiol. 2004;43(5):276A–7.
dos Santos RL et al. Sex hormones in the cardiovascular system. Horm Mol Biol Clin Investig. 2014;18(2):89–103.
Orshal JM, Khalil RA. Gender, sex hormones, and vascular tone. Am J Physiol Regul Integr Comp Physiol. 2004;286(2):R233–49.
Hulley S et al. Randomized trial of estrogen plus progestin for secondary prevention of coronary heart disease in postmenopausal women. Heart and Estrogen/progestin Replacement Study (HERS) Research Group. JAMA. 1998;280(7):605–13.
Manson JE et al. Estrogen plus progestin and the risk of coronary heart disease. N Engl J Med. 2003;349(6):523–34.
Barrett-Connor E et al. Effects of raloxifene on cardiovascular events and breast cancer in postmenopausal women. N Engl J Med. 2006;355(2):125–37.
Reynolds HR. Myocardial infarction without obstructive coronary artery disease. Curr Opin Cardiol. 2012;27(6):655–60.
Mortensen KH et al. Spontaneous coronary artery dissection: a Western Denmark Heart Registry study. Catheter Cardiovasc Interv. 2009;74(5):710–7.
Pepine CJ et al. Coronary microvascular reactivity to adenosine predicts adverse outcome in women evaluated for suspected ischemia results from the National Heart, Lung and Blood Institute WISE (Women’s Ischemia Syndrome Evaluation) study. J Am Coll Cardiol. 2010;55(25):2825–32.
Murthy VL et al. Improved cardiac risk assessment with noninvasive measures of coronary flow reserve. Circulation. 2011;124(20):2215–24.
Britten MB, Zeiher AM, Schachinger V. Microvascular dysfunction in angiographically normal or mildly diseased coronary arteries predicts adverse cardiovascular long-term outcome. Coron Artery Dis. 2004;15(5):259–64.
Herzog BA et al. Long-term prognostic value of 13N-ammonia myocardial perfusion positron emission tomography added value of coronary flow reserve. J Am Coll Cardiol. 2009;54(2):150–6.
Fukushima K et al. Prediction of short-term cardiovascular events using quantification of global myocardial flow reserve in patients referred for clinical 82Rb PET perfusion imaging. J Nucl Med. 2011;52(5):726–32.
Johnson BD et al. Prognosis in women with myocardial ischemia in the absence of obstructive coronary disease: results from the National Institutes of Health-National Heart, Lung, and Blood Institute-Sponsored Women’s Ischemia Syndrome Evaluation (WISE). Circulation. 2004;109(24):2993–9.
Shaw LJ et al. The economic burden of angina in women with suspected ischemic heart disease: results from the National Institutes of Health–National Heart, Lung, and Blood Institute–sponsored Women’s Ischemia Syndrome Evaluation. Circulation. 2006;114(9):894–904.
Ong P et al. High prevalence of a pathological response to acetylcholine testing in patients with stable angina pectoris and unobstructed coronary arteries. The ACOVA Study (Abnormal COronary VAsomotion in patients with stable angina and unobstructed coronary arteries). J Am Coll Cardiol. 2012;59(7):655–62.
Humphries KH et al. Angina with “normal” coronary arteries: sex differences in outcomes. Am Heart J. 2008;155(2):375–81.
Suwaidi JA et al. Long-term follow-up of patients with mild coronary artery disease and endothelial dysfunction. Circulation. 2000;101(9):948–54.
Prescott E et al. Improving diagnosis and treatment of women with angina pectoris and microvascular disease: the iPOWER study design and rationale. Am Heart J. 2014;167(4):452–8. This study revealed that routine non-invasive assessment of coronary flow reserve with TTE is feasible and could lead to better identification and treatment of patients with microvascular ischemia.
Bugiardini R et al. Comparison of verapamil versus propranolol therapy in syndrome X. Am J Cardiol. 1989;63(5):286–90.
Lanza GA et al. Atenolol versus amlodipine versus isosorbide-5-mononitrate on anginal symptoms in syndrome X. Am J Cardiol. 1999;84(7):854–6.
Pauly DF et al. In women with symptoms of cardiac ischemia, nonobstructive coronary arteries, and microvascular dysfunction, angiotensin-converting enzyme inhibition is associated with improved microvascular function: a double-blind randomized study from the National Heart, Lung and Blood Institute Women’s Ischemia Syndrome Evaluation (WISE). Am Heart J. 2011;162(4):678–84.
Treasure CB et al. Beneficial effects of cholesterol-lowering therapy on the coronary endothelium in patients with coronary artery disease. N Engl J Med. 1995;332(8):481–7.
Kayikcioglu M et al. Benefits of statin treatment in cardiac syndrome-X1. Eur Heart J. 2003;24(22):1999–2005.
Eriksson BE et al. Physical training in syndrome X: physical training counteracts deconditioning and pain in syndrome X. J Am Coll Cardiol. 2000;36(5):1619–25.
Duvernoy CS. Evolving strategies for the treatment of microvascular angina in women. Expert Rev Cardiovasc Ther. 2012;10(11):1413–9.
Compliance with Ethics and Guidelines
Conflicts of Interest
Ashley M. Funk and Claire S. Duvernoy declare that they have no conflict of interest.
Human and Animal Rights and Informed Consent
This article does not contain any studies with human or animal subjects performed by any of the authors.
Author information
Authors and Affiliations
Corresponding author
Additional information
This article is part of the Topical Collection on Women + Heart Disease
Rights and permissions
About this article
Cite this article
Funk, A.M., Duvernoy, C.S. Acute Coronary Syndrome: Current Diagnosis and Management in Women. Curr Cardiovasc Risk Rep 9, 39 (2015). https://doi.org/10.1007/s12170-015-0468-z
Published:
DOI: https://doi.org/10.1007/s12170-015-0468-z