Abstract
Objectives
To determine the incidence of readmission in pediatric patients in a tertiary care hospital in a developing nation and to ascertain factors precipitating readmissions.
Methods
A prospective study was conducted from February 2016 through January 2017 at a tertiary care hospital. Children between 1 mo to 15 y of age were included if they were readmitted within 60 d of discharge. The risk factors for readmission were determined on the basis of medical record review and a structured questionnaire and the ascribed cause of readmission was grouped into three categories: Patient specific factors, Hospital specific factors and Unrelated/ New illness.
Results
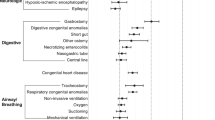
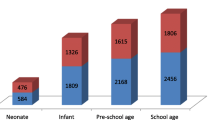
The readmission rate was 3%, out of which 80.66% were found to be causally related to the index admission. Several sociodemographic characteristics i.e. lack of health information like television, lower socioeconomic status, absence of adequate breastfeeding, lower age, migrants were found to be significantly associated with readmission along with other patient specific factors like presence of cardiac disease, presence of comorbid conditions like anemia, malnutrition, and global developmental delay. The most important cause for readmission was determined as patient specific (48.66%) followed by hospital specific (38%) and unknown/unrelated factors (13.33%).
Conclusions
The progression of the primary illness and social determinants of pediatric readmissions are important contributing risk factors for readmission in developing countries in pediatric patients. Multicentric studies are needed from this region of the world to include different hospital readmissions rate and to address the issue of potential preventability of pediatric readmissions.

Similar content being viewed by others
References
Bardach NS, Vittinghoff E, Asteria-Penaloza R, et al. Measuring hospital quality using pediatric readmission and revisit rates. Pediatrics. 2013;132:429–36.
Auger KA, Teufel RJ 2nd, Harris JM 2nd, et al. Children's hospital characteristics and readmission metrics. Pediatrics. 2017;139:e20161720.
Berry JG, Toomey SL, Zaslavsky AM, et al. Pediatric readmission prevalence and variability across hospitals. JAMA. 2013;309:372–80.
Khan A, Nakamura MM, Zaslavsky AM, et al. Same-hospital readmission rates as a measure of pediatric quality of care. JAMA Pediatr. 2015;169:905–12.
Nakamura MM, Toomey SL, Zaslavsky AM, et al. Measuring pediatric hospital readmission rates to drive quality improvement. Acad Pediatr. 2014;14:S39–46.
Toomey SL, Peltz A, Loren S, et al. Potentially preventable 30-day hospital readmissions at a children's hospital. Pediatrics. 2016;138:pii:e20154182.
Gay JC, Agrawal R, Auger KA, et al. Rates and impact of potentially preventable readmissions at children's hospitals. J Pediatr. 2015;166:613–9.e5.
Wijlaars LP, Hardelid P, Woodman J, Allister J, Cheung R, Gilbert R. Who comes back with what: a retrospective database study on reasons for emergency readmission to hospital in children and young people in England. Arch Dis Child. 2016;101:714–8.
Feudtner C, Levin JE, Srivastava R, et al. How well can hospital readmission be predicted in a cohort of hospitalized children? A retrospective, multicenter study. Pediatrics. 2009;123:286–93.
Berry JG, Hall DE, Kuo DZ, et al. Hospital utilization and characteristics of patients experiencing recurrent readmissions within children's hospitals. JAMA. 2011;305:682–90.
Brittan M, Albright K, Cifuentes M, Jimenez-Zambrano A, Kempe A. Parent and provider perspectives on pediatric readmissions: what can we learn about readiness for discharge? Hosp Pediatr. 2015;5:559–65.
Flores G, Abreu M, Chaisson CE, Sun D. Keeping children out of hospitals: parents’ and physicians’ perspectives on how pediatric hospitalizations for ambulatory care-sensitive conditions can be avoided. Pediatrics. 2003;112:1021–30.
Wallace SS, Keller SL, Falco CN, et al. An examination of physician-, caregiver-, and disease-related factors associated with readmission from a pediatric hospital medicine service. Hosp Pediatr. 2015;5:566–73.
Jonas JA, Devon EP, Ronan JC, et al. Determining preventability of pediatric readmissions using fault tree analysis. J Hosp Med. 2016;11:329–35.
Blunt I, Bardsley M, Grove A, Clarke A. Classifying emergency 30-day readmissions in England using routine hospital data 2004–2010: what is the scope for reduction? Emerg Med J. 2015;32:44–50.
Dharmarajan K, Hsieh AF, Lin Z, et al. Hospital readmission performance and patterns of readmission: retrospective cohort study of medicare admissions. BMJ. 2013;347:f6571.
Auger KA, Mueller EL, Weinberg SH, et al. A validated method for identifying unplanned pediatric readmission. J Pediatr. 2016;170:105-12.e1-2.
Gay JC, Hain PD, Grantham JA, Saville BR. Epidemiology of 15-day readmissions to a children's hospital. Pediatrics. 2011;127:e1505–12.
Nakamura MM, Zaslavsky AM, Toomey SL, et al. Pediatric readmissions after hospitalizations for lower respiratory infections. Pediatrics. 2017;140:pii:e20160938.
Kaur A, Singh K, Pannu MS, Singh P, Sehgal N, Kaur R. The effect of exclusive breastfeeding on hospital stay and morbidity due to various diseases in infants under 6 months of age: a prospective observational study. Int J Pediatr. 2016;2016:7647054.
Lohiya A, Nongkynrih B, Gupta SK. Migrants to urban India: need for public health action. Indian J Community Med. 2014;39:73–5.
Stephenson R, Matthews Z, McDonald J. The impact of rural–urban migration on under-two mortality in India. J Biosoc Sci. 2003;35:15–31.
Choudhary N, Parthasarathy D. Is migration status a determinant of urban nutrition insecurity? Empirical evidence from Mumbai city, India. J Biosoc Sci. 2009;41:583–605.
Coller RJ, Klitzner TS, Lerner CF, Chung PJ. Predictors of 30-day readmission and association with primary care follow-up plans. J Pediatr. 2013;163:1027–33.
Auger KA, Simon TD, Cooperberg D, et al. Summary of STARNet: seamless transitions and (re)admissions network. Pediatrics. 2015;135:164–75.
Lax Y, Martinez M, Brown NM. Social determinants of health and hospital readmission. Pediatrics. 2017;140:e20171427.
Bajpai V. The challenges confronting public hospitals in india, their origins, and possible solutions. Adv Public Health. 2014;2014:898502.
Rao M, Rao KD, Kumar AK, Chatterjee M, Sundararaman T. Human resources for health in India. Lancet. 2011;377:587–98.
Acknowledgements
The authors thank Dr. Anusha Ramesh, Dr. Neha Bidhuri, Dr. Preeti Kukreja, Dr. Praveen, Dr. Navjot Saini for helping with the data collection. They would also like to thank Kirti Ranjan and Bhawna Garg for helping with data analysis and Ms. Reena Mehta for the technical support.
Author information
Authors and Affiliations
Contributions
DK: Conception and design of the study, drafting the article and revising it critically for important intellectual content and final approval of the version to be submitted; SS: Acquisition of data and analysis and interpretation of data, drafting the article or revising it critically for important intellectual content and final approval of the version to be submitted; GS: Conception and design of the study, acquisition of data and drafting the article; SA: Conception and design of the study, drafting the article and final approval of the version to be submitted; AS, PJ, NS: Acquisition of data and analysis and interpretation of data, drafting the article. DK will act as guarantor for this paper.
Corresponding author
Ethics declarations
Conflict of Interest
None.
Informed Consent
Informed written consent was obtained from the parents for reporting the case.
Rights and permissions
About this article
Cite this article
Kumar, D., Swarnim, S., Sikka, G. et al. Factors Associated with Readmission of Pediatric Patients in a Developing Nation. Indian J Pediatr 86, 267–275 (2019). https://doi.org/10.1007/s12098-018-2767-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12098-018-2767-0