Abstract
Background
Recurrence occurs in up to 20% of patients with stage II colon cancer operated on for cure. Although postoperative intra-abdominal infection has been linked with an increased risk of recurrence, the association is controversial. The aim was to investigate the impact of postoperative intra-abdominal infection on disease-free survival and disease-specific survival in patients with stage II colon cancer.
Methods
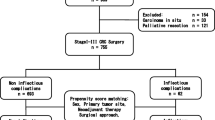
Patients undergoing elective surgery for colon cancer stage II, between 2003 and 2014, were included. Patients with anastomotic leak or intra-abdominal abscess were included in the infection group. We used the Kaplan–Meier method to represent the distribution of survival and the Cox proportional hazards model to estimate the contribution of relevant clinicopathological factors with prognosis.
Results
Postoperative intra-abdominal infection was diagnosed in 37 of 363 (10.2%) patients. Perioperative blood transfusion was more frequent in patients with infection (p = 0.008). Overall 5-year disease-free survival rate was 85.1%. Disease-free survival at 5 years was lower in patients with postoperative intra-abdominal infection (52.8 vs 88.7%; p < 0.001), perineural invasion (p = 0.001), lymphovascular invasion (p = 0.001), pT4 (p = 0.013), and in patients with adjuvant chemotherapy (p = 0.013). Multivariate analysis showed that postoperative intra-abdominal infection (HR 4.275; p < 0.001), perineural invasion (HR 2.230; p = 0.007), and lymphovascular invasion (HR 2.052; p = 0.016) were all significant independent predictors of reduced disease-free survival. Regarding specific survival, independent significant prognostic factors were the number of lymph nodes, lymphovascular invasion, and postoperative intra-abdominal infection.
Conclusion
In this series of patients with stage II colon cancer, postoperative intra-abdominal infection has an independent negative impact on disease-free survival and disease-specific survival.


Similar content being viewed by others
References
Chang GJ, Kaiser AM, Mills S, Rafferty JS, Buie WD, on behalf of the Standards Practice Task Force of the American Society of Colon and Rectal Surgeons. Practice parameters for the management of colon cancer. Dis Colon Rectum. 2012;55:831–43.
Bockelman C, Engelmann BE, Kaprio T, Hansen TF, Glimelius B. Risk of recurrence in patients with colon cancer stage II and III: a systematic review and meta-analysis of recent literature. Acta Oncol. 2015;54:5–16.
Kumar A, Kennecke HF, Renouf DJ, Lim HJ, Gill S, Woods R, et al. Adjuvant chemotherapy use and outcomes of patients with high-risk versus low-risk stage II colon cancer. Cancer. 2015;121:527–34.
O’Connor ES, Greenblatt DY, LoConte NK, Gangnon RE, Liou JI, Heise CP, et al. Adjuvant chemotherapy for stage II colon cancer with poor prognostic features. J Clin Oncol. 2011;29:3381–8.
Bruce J, Krukowski ZH, Al-Khairy G, Russell EM, Park KG. Systematic review of the definition and measurement of anastomotic leak after gastrointestinal surgery. Br J Surg. 2001;88:1157–68.
Serra-Aracil X, García-Domingo MI, Parés D, Espín E, Biondo S, Guirao X, et al. Surgical site infection in elective operations for colorectal cancer after de application of preventive measures. Arch Surg. 2011;146:606–12.
Rullier E, Laurent C, Garrelon JL, Michel P, Saric J, Parneix M. Risk factors for anastomotic leakage after resection of rectal cancer. Br J Surg. 1998;85:355–8.
Bell SW, Walker KG, Rickard MJ, Sinclair G, Dent OF, Chapuis PH, et al. Anastomotic leakage after curative anterior resection results in a higher prevalence of local recurrence. Br J Surg. 2003;90(10):1261–6.
Walker KG, Bell SW, Rickard MJ, Mehanna D, Dent OF, Chapuis PH, et al. Anastomotic leakage is predictive of diminished survival after potentially curative resection for colorectal cancer. Ann Surg. 2004;240:255–9.
McArdle CS, McMillan DC, Hole DJ. Impact of anastomotic leakage on long-term survival of patients undergoing curative resection for colorectal cancer. Br J Surg. 2005;92:1150–4.
Law WL, Choi H, Lee Y, Ho JW, Seto CL. Anastomotic leakage is associated with poor long-term outcome in patients after curative colorectal resection for malignancy. J Gastrointest Surg. 2007;11:8–15.
Ptok H, Marusch F, Meyer F, Schubert D, Gastinger I, Lippert H. Impact of anastomotic leakage on oncological outcome after rectal cancer resection. Br J Surg. 2007;94:1548–54.
Varty P, Linehan I, Boulos P. Intra-abdominal sepsis and survival after surgery for colorectal cancer. Br J Surg. 1994;81:915–8.
Eriksen MT, Wibe A, Norstein J, Haffner J, Wiig JN, Norwegian Rectal Cancer Group. Anastomotic leakage following routine mesorectal excision for rectal cancer in a national cohort of patients. Colorectal Dis. 2005;7:51–7.
Smith JD, Paty PB, Guillem JG, Temple LK, Wiser MR, Nash GM. Anastomotic leak is not associated with oncologic outcome in patients undergoing low anterior resection for rectal cancer. Ann Surg. 2012;256:1034–8.
Katoh H, Yamashita K, Wang G, Sato T, Nakamura T, Watanabe M. Anastomotic leakage contributes to the risk for systemic recurrence in stage II colorectal cancer. J Gastrointest Surg. 2011;15:120–9.
Eberhardt JM, Kiran RP, Lavery IC. The impact of anastomotic leak and intra-abdominal abscess on cancer-related outcomes after resection for colorectal cancer: a case control study. Dis Colon Rectum. 2009;52:380–6.
Bohle B, Pera M, Pascual M, Alonso S, Mayol X, Salvado M, et al. Postoperative intra-abdominal infection increases angiogenesis and tumor recurrence after surgical excision of colon cancer in mice. Surgery. 2010;147:120–6.
Artinyan A, Orcutt ST, Anaya DA, Richardson P, Chen GJ, Berger DH. Infectious postoperative complications decrease long-term survival in patients undergoing curative surgery for colorectal cancer. A study of 12.075 patients. Ann Surg. 2015;261:497–505.
Krarup PM, Nordhol-Carstensen A, Jorgensen LN, Harling H. Anastomotic leak increases distant recurrence and long-term mortality after curative resection for colonic cancer. A nationwide cohort study. Ann Surg. 2014;259:930–8.
Bertelsen CA, Andreasen AH, Jørgensen T, Harling H, Danish Colorectal Cancer Group. Anastomotic leakage after curative anterior resection for rectal cancer: short and long-term outcome. Colorectal Dis. 2010;12:e76–81.
Jörgren F, Johansson R, Damber L, Lindmark G. Anastomotic leakage after surgery for rectal cancer: a risk factor for local recurrence. Distant metastasis and reduced cancer-specific survival? Colorectal Dis. 2011;13:272–83.
Espín E, Ciga MA, Pera M, Ortiz H. Anastomotic leak is not associated with oncologic outcome in patients undergoing sphincter-saving surgery for rectal cancer. Br J Surg. 2015;102:416–22.
Richards CH, Platt JJ, Anderson JH, McKee RF, Horgan PG, McMillan DC. The impact of perioperative risk. Tumor pathology and surgical complications on disease recurrence following potentially curative resection of colorectal cancer. Ann Surg. 2011;254:83–9.
Mirnezami A, Mirnezami R, Chandrakumaran K, Sasapu K, Sagar P, Finan P. Increased local recurrence and reduced survival from colorectal cancer following anastomotic leak: systematic review and meta-analysis. Ann Surg. 2011;253:890–9.
Alonso S, Pascual M, Salvans S, Mayol X, Mojal S, Gil MJ, et al. Postoperative intra-abdominal infection and colorectal cancer recurrence: a prospective matched cohort study of inflammatory and angiogenic responses as mechanisms involved in this association. Eur J Surg Oncol. 2015;41:208–14.
Salvans S, Mayol X, Alonso S, Messeguer R, Pascual M, Mojal S, et al. Postoperative peritoneal infection enhances migration and invasion capacities of tumor cells in vitro: an insight into the association between anastomotic leak and recurrence after surgery for colorectal cancer. Ann Surg. 2014;260:939–43.
Alonso S, Mayol X, Nonell L, Salvans S, Pascual M, Pera M, Colorectal Cancer Research Group (Hospital del Mar Medical Research Institute). Peripheral blood leucocytes show differential expression of tumour progression-related genes in colorectal cancer patients who have a postoperative intra-abdominal infection: a prospective matched cohort study. Colorectal Dis. 2017;19(5):O115–25.
Funding
Supported by research Grant from Instituto de Salud Carlos III (FIS Grant PI11/01093).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The author declares that there is no competing interest.
Research involving human participants
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards.
Informed consent
The Hospital del Mar Institutional Review Board does not require formal informed consent for retrospective studies including only chart review. Complete patient anonymity is guaranteed.
Rights and permissions
About this article
Cite this article
Sánchez-Velázquez, P., Pera, M., Jiménez-Toscano, M. et al. Postoperative intra-abdominal infection is an independent prognostic factor of disease-free survival and disease-specific survival in patients with stage II colon cancer. Clin Transl Oncol 20, 1321–1328 (2018). https://doi.org/10.1007/s12094-018-1866-8
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12094-018-1866-8