Abstract
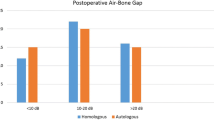
Ossicular discontinuity is the most common cause of conductive hearing loss. The use of ossicular graft material in ossicular chain reconstruction significantly improves the result in hearing. This study was conducted to compare and analyze the outcome of ossicular reconstruction using allogenic septal spur cartilage and autologous cortical bone in terms of hearing results and graft uptake rates. Study design: randomized clinical trial. Study included 112 patients visiting our ENT department. Patients between 16 and 50 years of age with history of chronic ear discharge and air–bone–gap (ABG) of > 35 dB and ossicular involvement were included in the study. The patients underwent detailed ENT examination, audiological and radiological assessment of temporal bone and those patients with evidence of ossicular erosion were subjected to ossiculoplasty with allogenic septal spur cartilage (group I) and autologous cortical bone (group II) randomly. The patients were followed up to 6 months to analyze functional and anatomical results. 50 patients out of 56 patients (90%) from group I who underwent allogenic septal cartilage ossicular reconstruction showed significant improvement in hearing as assessed by pure tone audiogram after 3 months and 6 months. Remaining 10% of patients who did not show hearing improvement on PTA were reopened after 6 months. It was observed that the stapes head got necrosed in them. 40 patients (72%) out of 56 patients (50%) from group II who underwent autologous cortical bone reconstruction showed hearing improvement. Remaining 16 patients (28%) showed no hearing improvement. They were reopened and ankylosis, dislocation of ossicle and extrusion were noted. In our study, graft uptake rates, formation of retraction pockets, and hearing improvements were analyzed. Complications like ankylosis formation, dislocation of ossicle and extrusion rates were more in the group II compared to group I. Hearing results of group I are better compared to group II and the allogenic septal cartilage being readily available is a good option for ossicular reconstruction.





Similar content being viewed by others
References
Yung M, Vowler SL (2006) Long-term results in ossiculoplasty: an analysis of prognostic factors. Otol Neurotol 27(6):874–881
Dornhoffer JL, Gardner E (2001) Prognostic factors in ossiculoplasty: a statistical staging system. Otol Neurotol 22(3):299–304
Gleeson M, Clarke R (2008) Scott-Brown’s otorhinolaryngology: head and neck surgery, vol 3, 7th edn. CRC Press, Cleveland
Amith N, Rs M (2017) Autologous incus versus titanium partial ossicular replacement prosthesis in reconstruction of austin type an ossicular defects: a prospective randomised clinical trial. J Laryngol Otol 131:391–398
Chaudhary N, Anand N, Taperwal A, Rai AK (2003) Role of autografts in the reconstruction of ossicular chain in intact canal wall procedures. Indian J Otolaryngol Head Neck Surg 55(3):157–159
Jha S, Mehta K, Prajapati V, Patel D, Kharadi P (2011) A comparative study of ossiculoplasty by using various graft materials. NJIRM 2(4):53–55
Athanasiadis-Sismanis A, Poe DS (2010) Ossicular chain reconstruction. In: Gulya AJ, Minor LB, Poe DS (eds) Glasscock-Shambaugh surgery of the ear, chap 29, 6th edn. Peoples Medical Publishing House, Connecticut, pp 489–501
Iurato S, Marioni G, Onofri M (2001) Hearing results of ossiculoplasty in Austin-Kartush group A patients. Otol Neurotol 22(2):140–144
Martin TP, Weller MD, Kim DS, Smith MC (2009) Results of primary ossiculoplasty in ears with an intact stapes superstructure and malleus handle: inflammation in the middle ear at the time of surgery does not affect hearing outcomes. Clin Otolaryngol 34(3):218–224
Harvey SA, Lin SY (1999) Double cartilage block ossiculoplasty in chronic ear surgery. The Laryngoscope 109(6):911–914
Acknowledgements
We are thankful to Dr S.M Azeem Mohiyuddin Department of ENT and Head and Neck Surgery, Sri Devaraj Urs Medical College, Tamaka, Kolar for his helpful discussion and technical expertise. We express our gratitude to Dr. Sekhar for supporting me and constant encouragement and Dr Indhu Department of ENT and HNS, Sri Devraj Urs Medical College and Research Centre, Tamaka, Kolar helping in editing the article.
Funding
Nil.
Author information
Authors and Affiliations
Contributions
KP Contributed to the design of study, collected samples, did data analysis and drafted the manuscript. Corresponding author of the manuscript. KCP Contributed to the design of study, data analysis, helped to frame the manuscript. MBS Contributed to the design of study, data analysis and reviewed the manuscript and helping me in editing the article. PKA Contributed to the design of study, data analysis and reviewed the manuscript. IG Contributed to the design of study, data analysis and reviewed the manuscript and helping me in editing the article. All authors read and approved the final manuscript.
Corresponding author
Ethics declarations
Conflict of interest
Authors declare no conflict of interest
Ethical Approval
Taken from the Sridevaraj medical college ethical committee.
Human and Animal Rights
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional committee, Institutional ethical committee approved it.
Informed Consent
Approval for the study was obtained from the Institutional Ethics Committee. Informed consent was required for this study.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Prasad, K.C., Koneru, P., Swapanthi, M.B. et al. Comparision of Allogenic Cartilage and Autologous Cortical Bone in Ossicular Reconstruction: A Comparative Study. Indian J Otolaryngol Head Neck Surg 74 (Suppl 1), 148–152 (2022). https://doi.org/10.1007/s12070-020-01924-8
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12070-020-01924-8