Abstract
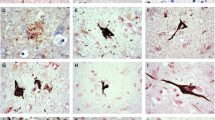
Tau is a microtubule-associated protein highly expressed in neurons with a chief role in microtubule dynamics and axonal maintenance. Adrenomedullin gene (ADM) codifies for various peptides that exert broad range of actions in the body. Previous works in our groups have shown that increased ADM products are positively correlated to microtubule disruption and tau pathology in Alzheimer’s disease brains. In the present study, we explore the involvement of ADM in the neuropathology of frontotemporal lobar degeneration that presents with primary tauopathy (FTLD-tau). Proteins from frontal cortices of FTLD-tau patients and age- and sex-matched non-demented controls were analyzed with antibodies against different microtubule components, including adrenomedullin, and synaptic markers. Tau pathology in frontal cortex from FTLD patients was confirmed. Levels of total βIII-tubulin as well as acetylated and detyrosinated tubulins, two markers of stabilized and aged microtubules, were significantly reduced and directly correlated with PSD95 and proBDNF in FTLD-tau patients when compared to non-demented controls. In contrast, no change in actin cytoskeleton was found. Interestingly, changes in microtubule elements, indicators of disturbed axonal preservation, were accompanied by decreased levels of free adrenomedullin, although no association was found. Altogether, reduced levels of adrenomedullin might not be directly linked to the microtubule pathology of FTLD-tau, but based on previous works, it is suggested that downregulation of ADM might be an adaptive attempt of neurons to mitigate microtubule disruption.




Similar content being viewed by others
References
Mann DMA, Snowden JS (2017) Frontotemporal lobar degeneration: pathogenesis, pathology and pathways to phenotype. Brain Pathol 27:723–736. https://doi.org/10.1111/bpa.12486
Kovacs GG (2015) Invited review: neuropathology of tauopathies: principles and practice. Neuropathol Appl Neurobiol 41:3–23. https://doi.org/10.1111/nan.12208
Revesz T, Holton JL (2003) Anatamopathological spectrum of tauopathies. Mov Disord 18:13–20. https://doi.org/10.1002/mds.10558
Mackenzie IRA, Neumann M, Bigio EH, Cairns NJ, Alafuzoff I, Kril J, Kovacs GG, Ghetti B et al (2010) Nomenclature and nosology for neuropathologic subtypes of frontotemporal lobar degeneration: an update. Acta Neuropathol 119:1–4. https://doi.org/10.1007/s00401-009-0612-2
Rademakers R, Cruts M, van Broeckhoven C (2004) The role of tau (MAPT) in frontotemporal dementia and related tauopathies. Hum Mutat 24:277–295. https://doi.org/10.1002/humu.20086
Iqbal K, Liu F, Gong C-X, Alonso Adel C, Grundke-Iqbal I (2009) Mechanisms of tau-induced neurodegeneration. Acta Neuropathol 118:53–69. https://doi.org/10.1007/s00401-009-0486-3
Goedert M, Spillantini MG, Cairns NJ, Crowther RA (1992) Tau proteins of Alzheimer paired helical filaments: abnormal phosphorylation of all six brain isoforms. Neuron 8:159–168
Rossi G, Tagliavini F (2015) Frontotemporal lobar degeneration: old knowledge and new insight into the pathogenetic mechanisms of tau mutations. Front Aging Neurosci 7:192. https://doi.org/10.3389/fnagi.2015.00192
Sackett DL, Ozbun L, Zudaire E, Wessner L, Chirgwin JM, Cuttitta F, Martínez A (2008) Intracellular proadrenomedullin-derived peptides decorate the microtubules and contribute to cytoskeleton function. Endocrinology 149:2888–2898. https://doi.org/10.1210/en.2007-1763
Larráyoz IM, Martínez A (2012) Proadrenomedullin N-terminal 20 peptide increases kinesin’s velocity both in vitro and in vivo. Endocrinology 153:1734–1742. https://doi.org/10.1210/en.2011-1685
Ferrero H, Larrayoz IM, Martisova E, Solas M, Howlett DR, Francis PT, Gil-Bea FJ, Martínez A et al (2017) Increased levels of brain adrenomedullin in the neuropathology of Alzheimer’s disease. Mol Neurobiol:1–7. https://doi.org/10.1007/s12035-017-0700-6
Fernandez AP, Masa JS, Guedan MA, Futch HS, Martínez-Murillo R (2016) Adrenomedullin expression in Alzheimer’s brain. Curr Alzheimer Res 13:428–438
Larrayoz IM, Ferrero H, Martisova E, Gil-Bea FJ, Ramírez MJ, Martínez A (2017) Adrenomedullin contributes to age-related memory loss in mice and is elevated in aging human brains. Front Mol Neurosci 10:384. https://doi.org/10.3389/fnmol.2017.00384
Mackenzie IRA, Neumann M, Baborie A, Sampathu DM, du Plessis D, Jaros E, Perry RH, Trojanowski JQ et al (2011) A harmonized classification system for FTLD-TDP pathology. Acta Neuropathol 122:111–113. https://doi.org/10.1007/s00401-011-0845-8
Forman MS, Zhukareva V, Bergeron C, Chin SS, Grossman M, Clark C, Lee VM, Trojanowski JQ (2002) Signature tau neuropathology in gray and white matter of corticobasal degeneration. Am J Pathol 160:2045–2053. https://doi.org/10.1016/S0002-9440(10)61154-6
Pollak D, Cairns N, Lubec G (2003) Cytoskeleton derangement in brain of patients with Down syndrome, Alzheimer’s disease and Pick’s disease. J Neural Transm Suppl:149–158
Ma Q-L, Zuo X, Yang F, Ubeda OJ, Gant DJ, Alaverdyan M, Kiosea NC, Nazari S et al (2014) Loss of MAP function leads to hippocampal synapse loss and deficits in the Morris water maze with aging. J Neurosci 34:7124–7136. https://doi.org/10.1523/JNEUROSCI.3439-13.2014
Rapoport M, Dawson HN, Binder LI, Vitek MP, Ferreira A (2002) Tau is essential to beta-amyloid-induced neurotoxicity. Proc Natl Acad Sci 99:6364–6369. https://doi.org/10.1073/pnas.092136199
Hempen B, Brion JP (1996) Reduction of acetylated alpha-tubulin immunoreactivity in neurofibrillary tangle-bearing neurons in Alzheimer’s disease. J Neuropathol Exp Neurol 55:964–972
Yuesong Gong Y, Lippa CF (2010) Review: disruption of the postsynaptic density in Alzheimer’s disease and other neurodegenerative dementias. Am J Alzheimer’s Dis Other Dementiasr 25:547–555. https://doi.org/10.1177/1533317510382893
Guo T, Noble W, Hanger DP (2017) Roles of tau protein in health and disease. Acta Neuropathol 133:665–704. https://doi.org/10.1007/s00401-017-1707-9
Brunden KR, Trojanowski JQ, Smith AB et al (2014) Microtubule-stabilizing agents as potential therapeutics for neurodegenerative disease. Bioorg Med Chem 22:5040–5049. https://doi.org/10.1016/j.bmc.2013.12.046
Ishikawa T, Chen J, Wang J, Okada F, Sugiyama T, Kobayashi T, Shindo M, Higashino F et al (2003) Adrenomedullin antagonist suppresses in vivo growth of human pancreatic cancer cells in SCID mice by suppressing angiogenesis. Oncogene 22:1238–1242. https://doi.org/10.1038/sj.onc.1206207
Robinson SD, Aitken JF, Bailey RJ, Poyner DR, Hay DL (2009) Novel peptide antagonists of adrenomedullin and calcitonin gene-related peptide receptors: identification, pharmacological characterization, and interactions with position 74 in receptor activity-modifying protein 1/3. J Pharmacol Exp Ther 331:513–521. https://doi.org/10.1124/jpet.109.156448
Acknowledgments
We thank the Brains for Dementia Research (BDR) program for the provision of human brain samples.
Funding Information
H.F. is a recipient of a fellowship from the Ministerio de Educación, Cultura y Deporte (FPU). I.M.L. is supported by a Miguel Servet contract (CP15/00198) from the “Instituto de Salud Carlos III-FEDER” (Fondo Europeo de Desarrollo Regional, a way to build Europe) and A.M. is funded by the Fundación Rioja Salud (FRS).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Informed consent was obtained from the patients’ next of kin before collection of brains, and the study was approved by the UK National Research Ethics Service.
Electronic supplementary material
ESM 1
(DOCX 1380 kb)
Rights and permissions
About this article
Cite this article
Ferrero, H., Larrayoz, I.M., Solas, M. et al. Reduced Adrenomedullin Parallels Microtubule Dismantlement in Frontotemporal Lobar Degeneration. Mol Neurobiol 55, 9328–9333 (2018). https://doi.org/10.1007/s12035-018-1079-8
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12035-018-1079-8