Abstract
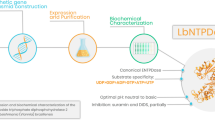
Leishmaniasis is one of the most important neglected tropical diseases, with a broad spectrum of clinical manifestations. Among the clinical manifestations of the disease, cutaneous leishmaniasis, caused by species of Leishmania braziliensis, presents wide distribution in Brazil. In this work, we performed the cloning, expression, and purification of the enzyme superoxide dismutase of Leishmania braziliensis (LbSOD-B2) considered a promising target for the search of new compounds against leishmaniasis. In vitro assays based on pyrogallol oxidation showed that LbSOD-B2 is most active around pH 8 and hydrogen peroxide is a LbSOD-B2 inhibitor at low millimolar range (IC50 = 1 mM).





Similar content being viewed by others
References
de Menezes, J. P. B., Guedes, C. E. S., Petersen, A. L. D. O. A., Fraga, D. B. M., & Veras, P. S. T. (2015). Advances in development of new treatment for Leishmaniasis. BioMed Research International, 2015, 1–12. https://doi.org/10.1155/2015/815023.
Gutierrez, F. R. S., Mineo, T. W. P., Pavanelli, W. R., Guedes, P. M. M., & Silva, J. S. (2009). The effects of nitric oxide on the immune system during Trypanosoma cruzi infection. Memórias do Instituto Oswaldo Cruz, 104 Suppl(Gilroy 2005), 236–245.
Tessarollo, N. G., Andrade, J. M., Moreira, D. S., & Murta, S. M. F. (2015). Functional analysis of iron superoxide dismutase-A in wild-type and antimony-resistant Leishmania braziliensis and Leishmania infantum lines. Parasitology International, 64(2), 125–129. https://doi.org/10.1016/j.parint.2014.11.001.
NASSIF, P.W., De Mello, T. F. P., Navasconi, T. R., Mota, C. A., Demarchi, I. G., Aristides, S. M. A., Lonardoni, M. V. C. (2017). Safety and efficacy of current alternatives in the topical treatment of cutaneous leishmaniasis: A systematic review. Parasitology. https://doi.org/10.1017/S0031182017000385.
WHO. (2015). Investing to overcome the global impact of neglected tropical diseases: third WHO report on neglected diseases 2015. Investing to overcome the global impact of neglected tropical diseases: Third WHO report on neglected diseases. ISBN 978 92 4 156486 1.
Torres-Guerrero, E., Quintanilla-Cedillo, M. R., Ruiz-Esmenjaud, J., & Arenas, R. (2017). Leishmaniasis: A review. F1000Research. https://doi.org/10.12688/f1000research.11120.1.
Longoni, S. S., Marín, C., & Sánchez-Moreno, M. (2014). Excreted Leishmania peruviana and Leishmania amazonensis iron-superoxide dismutase purification: Specific antibody detection in Colombian patients with cutaneous leishmaniasis. Free Radical Biology and Medicine, 69, 26–34. https://doi.org/10.1016/j.freeradbiomed.2014.01.012.
Sanchez-Moreno, M., Gomez-Contreras, F., Navarro, P., Marin, C., Ramirez-Macias, I., Rosales, M. J., et al. (2015). Imidazole-containing phthalazine derivatives inhibit Fe-SOD performance in Leishmania species and are active in vitro against visceral and mucosal leishmaniasis. Parasitology, 142(10), 1115–1129. https://doi.org/10.1017/S0031182015000657.
PAHO/WHO. (2015). Informe Epidemiológico das Américas. Report Leishmaniases No, 3, 3–7. https://doi.org/10.1017/CBO9781107415324.004.
Yasinzai, M., Khan, M., Nadhman, A., & Shahnaz, G. (2013). Drug resistance in leishmaniasis: Current drug-delivery systems and future perspectives. Future Medicinal Chemistry, 5(15), 1877–1888. https://doi.org/10.4155/fmc.13.143.
Mouttaki, T., Morales-Yuste, M., Merino-Espinosa, G., Chiheb, S., Fellah, H., Martin-Sanchez, J., & Riyad, M. (2014). Molecular diagnosis of cutaneous leishmaniasis and identification of the causative Leishmania species in Morocco by using three PCR-based assays. Parasites & Vectors, 7, 420. https://doi.org/10.1186/1756-3305-7-420.
Borborema, S. E. T., Osso Junior, J. A., de Andrade Junior, H. F., & do Nascimento, N. D. (2013). Biodistribution of meglumine antimoniate in healthy and Leishmania (Leishmania) infantum chagasi-infected BALB/c mice. Memorias do Instituto Oswaldo Cruz, 108(5), 623–630. https://doi.org/10.1590/0074-0276108052013014.
Mar Castro del M., Cossio, A., Velasco, C., Osorio, L., Saravia, N., & Cloetens, L. (2017). Risk factors for therapeutic failure to meglumine antimoniate and miltefosine in adults and children with cutaneous leishmaniasis in Colombia: A cohort study. PLoS Neglected Tropical Diseases, 11(4), e0005515. https://doi.org/10.1371/journal.pntd.0005515.
de Vries, H. J. C., Reedijk, S. H., & Schallig, H. D. F. H. (2015). Cutaneous Leishmaniasis: Recent developments in diagnosis and management. American Journal of Clinical Dermatology, 16(2), 99–109. https://doi.org/10.1007/s40257-015-0114-z.
Haldar, A. K., Sen, P., & Roy, S. (2011). Use of antimony in the treatment of Leishmaniasis: Current status and future directions. Molecular Biology International, 2011, 1–23. https://doi.org/10.4061/2011/571242.
Vanaerschot, M., de Doncker, S., Rijal, S., Maes, L., Dujardin, J. C., & Decuypere, S. (2011). Antimonial resistance in Leishmania donovani is associated with increased in vivo parasite burden. PLoS ONE, 6(8), 1–5. https://doi.org/10.1371/journal.pone.0023120.
Van Assche, T., Deschacht, M., da Luz, RaI., Maes, L., & Cos, P. (2011). Leishmania-macrophage interactions: Insights into the redox biology. Free Radical Biology & Medicine, 51(2), 337–351. https://doi.org/10.1016/j.freeradbiomed.2011.05.011.
Turrens, J. F. (2004). Oxidative stress and antioxidant defenses: A target for the treatment of diseases caused by parasitic protozoa. Molecular Aspects of Medicine, 25(1–2), 211–220. https://doi.org/10.1016/j.mam.2004.02.021.
Sheng, Y., Abreu, I. A., Cabelli, D. E., Maroney, M. J., Miller, A. F., Teixeira, M., & Valentine, J. S. (2014). Superoxide dismutases and superoxide reductases. Chemical Reviews, 114(7), 3854–3918. https://doi.org/10.1021/cr4005296.
Plewes, K. A., Barr, S. D., & Gedamu, L. (2003). Iron superoxide dismutases targeted to the glycosomes of Leishmania chagasi are important for survival. Infection and Immunity, 71(10), 5910–5920. https://doi.org/10.1128/IAI.71.10.5910.
Romero, A. H., Medina, R., Alcala, A., García-Marchan, Y., Núñez-Duran, J., Leañez, J., et al. (2017). Design, synthesis, structure-activity relationship and mechanism of action studies of a series of 4-chloro-1-phthalazinyl hydrazones as a potent agent against Leishmania braziliensis. European Journal of Medicinal Chemistry, 127, 606–620. https://doi.org/10.1016/j.ejmech.2017.01.022.
O’Shea, I. P., Shahed, M., Aguilera-Venegas, B., & Wilkinson, S. R. (2016). Evaluating 5-nitrothiazoles as trypanocidal agents. Antimicrobial Agents and Chemotherapy, 60(2), 1137–1140. https://doi.org/10.1128/AAC.02006-15.
Papadopoulou, M. V., Bloomer, W. D., Rosenzweig, H. S., Wilkinson, S. R., Szular, J., & Kaiser, M. (2016). Antitrypanosomal activity of 5-nitro-2-aminothiazole-based compounds. European Journal of Medicinal Chemistry, 117, 179–186. https://doi.org/10.1016/j.ejmech.2016.04.010.
Sánchez-moreno, M., Gómez-Contreras, F., Navarro, P., Marín, C., Ramírez-macías, I., Olmo, F., et al. (2012). In vitro leishmanicidal activity of imidazole- or pyrazole-based benzo [g] phthalazine derivatives against leishmania infantum and leishmania braziliensis species. Journal of Antimicrobial Chemotherapy, 67(2), 387–397. https://doi.org/10.1093/jac/dkr480.
Froger, A., & Hall, J. E. (2007). Transformation of plasmid DNA into E. coli using the heat shock method. Journal of Visualized Experiments. https://doi.org/10.3791/253.
Aslanidis, C., & Dejong, P. J. (1990). Ligation-independent cloning of PCR products (LIC-PCR). Nucleic Acids Research, 18(20), 6069–6074. https://doi.org/10.1093/nar/18.20.6069.
Marklund, S., & Marklund, G. (1974). Involvement of the superoxide anion radical in the autoxidation of pyrogallol and a convenient assay for superoxide dismutase. European Journal of Biochemistry, 47, 469–474. https://doi.org/10.1111/j.1432-1033.1974.tb03714.x.
Stols, L., Gu, M., Dieckman, L., Raffen, R., Collart, F. R., & Donnelly, M. I. (2002). A new vector for high-throughput, ligation-independent cloning encoding a tobacco etch virus protease cleavage site. Protein Expression and Purification, 25(1), 8–15. https://doi.org/10.1006/prep.2001.1603.
Weeks, S. D., Drinker, M., & Loll, P. J. (2007). Ligation independent cloning vectors for expression of SUMO fusions. Protein Expression and Purification, 53(1), 40–50. https://doi.org/10.1016/j.pep.2006.12.006.
Fang, J., Chen, L., Cheng, B., & Fan, J. (2013). Engineering soluble tobacco etch virus protease accompanies the loss of stability. Protein Expression and Purification, 92(1), 29–35. https://doi.org/10.1016/j.pep.2013.08.015.
Sun, C., Liang, J., Shi, R., Gao, X., Zhang, R., Hong, F., et al. (2012). Tobacco etch virus protease retains its activity in various buffers and in the presence of diverse additives. Protein Expression and Purification, 82(1), 226–231. https://doi.org/10.1016/j.pep.2012.01.005.
Faúndez, M., Rojas, M., Bohle, P., Reyes, C., Letelier, M. E., Aliaga, M. E., et al. (2011). Pyrogallol red oxidation induced by superoxide radicals: Application to evaluate redox cycling of nitro compounds. Analytical Biochemistry, 419(2), 284–291. https://doi.org/10.1016/j.ab.2011.08.048.
Roth, E. F., & Gilbert, H. S. (1984). The pyrogallol assay for superoxide dismutase: Absence of a glutathione artifact. Analytical Biochemistry, 137(1), 50–53.
Meier, B., Michel, C., Saran, M., Parak, F., Rotilioii, G., & Oberschleissheim, D. (1995). Kinetic and spectroscopic studies on a superoxide dismutase from Propionibacterium shermanha that is active with iron or manganese: pH-dependence. Biochemical Journal, 310, 945–950.
Jr, W. B., & Fridovich, I. (1987). Effect of hydrogen peroxide on the iron-containing superoxide dismutase of Escherichia coli. Biochemistry, 26(5), 1251–1257.
Gratepanche, S., Ménage, S., Touati, D., Wintjens, R., Delplace, P., Fontecave, M., et al. (2002). Biochemical and electron paramagnetic resonance study of the iron superoxide dismutase from Plasmodium falciparum. Molecular and Biochemical Parasitology, 120(2), 237–246. https://doi.org/10.1016/S0166-6851(02)00004-X.
Acknowledgements
The authors are grateful for the academic support of PPGBiotec-UEFS and the Grants from CNPq 306277/2014-0, FAPESB BOL0688/2014, and FAPESP 2013/07600-3.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors confirm that this article content has no conflicts of interest.
Rights and permissions
About this article
Cite this article
Brito, C.C.B., Maluf, F.V., de Lima, G.M.A. et al. Molecular Cloning and Biochemical Characterization of Iron Superoxide Dismutase from Leishmania braziliensis. Mol Biotechnol 60, 595–600 (2018). https://doi.org/10.1007/s12033-018-0095-2
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12033-018-0095-2