Abstract
Background
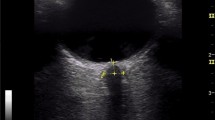
Intracranial pressure (ICP) monitoring is essential after subarachnoid hemorrhage (SAH) to prevent secondary brain insults and to tailor individualized treatments. Optic nerve sheath diameter (ONSD), measured using ultrasound (US), could serve as a noninvasive bedside tool to estimate ICP, avoiding the risks of hemorrhage or infection related to intracranial catheters. The aims of this study were twofold: first, to explore the reliability of US for measuring ONSD; second, to establish whether the US-ONSD can be considered a proxy for ICP in SAH patients early after bleeding. For the first aim, we compared the ONSD measurements given by magnetic resonance imaging (MRI-ONSD) with the US-ONSD findings. For the second aim, we analyzed the relationship between US-ONSD measurements and ICP values.
Methods
Adult patients with diagnosis of aneurysmal SAH and external ventricular drainage system (EVD) were included. Ten patients were examined by MRI to assess ONSD, and the results were compared to the diameter given by US. In 20 patients, the US-ONSD values were related to ICP measured simultaneously through EVD. In ten of these patients, we explored the changes in the US-ONSD at the time of controlled and fairly rapid changes in ICP after cerebrospinal fluid (CSF) drainage.
Results
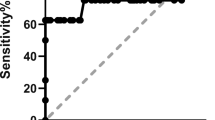
US-ONSD measurements at the bedside were accurate, very similar to the diameters measured by MRI (the mean difference in the Bland–Altman plot was 0.08 mm, 95% limits of agreement: − 1.13; + 1.23 mm). No clear relationship was detectable between the ICP and US-ONSD, and a linear regression model showed an angular coefficient very close to 0 (p > 0.05). US-ONSD and ICP values were in agreement after CSF drainage and shifts in ICP in a limited number of patients.
Conclusions
US-ONSD measurement does not accurately estimate ICP in SAH patients in the intensive care unit.





Similar content being viewed by others
References
Chen S, Feng H, Sherchan P, Klebe D, Zhao G, Sun X, et al. Controversies and evolving new mechanisms in subarachnoid hemorrhage. Prog Neurobiol. 2014;115:64–91. https://doi.org/10.1016/j.pneurobio.2013.09.002.
Voldby B, Enevoldsen EM. Intracranial pressure changes following aneurysm rupture. Part 3: recurrent hemorrhage. J Neurosurg. 1982;56(6):784–9.
Prunell GF, Mathiesen T, Diemer NH, Svendgaard NA. Experimental subarachnoid hemorrhage: subarachnoid blood volume, mortality rate, neuronal death, cerebral blood flow, and perfusion pressure in three different rat models. Neurosurgery. 2003;52(1):165–75 (discussion 175-6).
Magni F, Pozzi M, Rota M, Vargiolu A, Citerio G. High-resolution intracranial pressure burden and outcome in subarachnoid hemorrhage. Stroke. 2015;46(9):2464–9. https://doi.org/10.1161/STROKEAHA.115.010219.
Heuer GG, Smith MJ, Elliott JP, Winn HR, LeRoux PD. Relationship between intracranial pressure and other clinical variables in patients with aneurysmal subarachnoid hemorrhage. J Neurosurg. 2004;101(3):408–16.
Zoerle T, Lombardo A, Colombo A, Longhi L, Zanier ER, Rampini P, et al. Intracranial pressure after subarachnoid hemorrhage. Crit Care Med. 2015;43(1):168–76. https://doi.org/10.1097/CCM.0000000000000670.
Le Roux P, Menon DK, Citerio G, Vespa P, Bader MK, Brophy GM, et al. Consensus summary statement of the international multidisciplinary consensus conference on multimodality monitoring in neurocritical care: a statement for healthcare professionals from the Neurocritical Care Society and the European Society of Intensive Care Medicine. Neurocrit Care. 2014;21(Suppl 2):S1–26. https://doi.org/10.1007/s12028-014-0041-5.
Heldt T, Zoerle T, Teichmann D, Stocchetti N. Intracranial pressure and intracranial elastance monitoring in neurocritical care. Annu Rev Biomed Eng. 2019;4(21):523–49. https://doi.org/10.1146/annurev-bioeng-060418-052257.
Ortolano F, Carbonara M, Stanco A, Civelli V, Carrabba G, Zoerle T, et al. External ventricular drain causes brain tissue damage: an imaging study. Acta Neurochir (Wien). 2017;159(10):1981–9. https://doi.org/10.1007/s00701-017-3291-0.
Jamjoom AAB, Joannides AJ, Poon MT, Chari A, Zaben M, Abdulla MAH, Roach J, et al. Prospective, multicentre study of external ventricular drainage-related infections in the UK and Ireland. J Neurol Neurosurg Psychiatry. 2018;89(2):120–6. https://doi.org/10.1136/jnnp-2017-316415.
Robba C, Santori G, Czosnyka M, Corradi F, Bragazzi N, Padayachy L, et al. Optic nerve sheath diameter measured sonographically as non-invasive estimator of intracranial pressure: a systematic review and meta-analysis. Intensive Care Med. 2018;44(8):1284–94. https://doi.org/10.1007/s00134-018-5305-7.
Fernando SM, Tran A, Cheng W, Rochwerg B, Taljaard M, Kyeremanteng K, et al. Diagnosis of elevated intracranial pressure in critically ill adults: systematic review and meta-analysis. BMJ. 2019;24(366):l4225. https://doi.org/10.1136/bmj.l4225.
Robba C, Bacigaluppi S, Cardim D, Donnelly J, Bertuccio A, Czosnyka M. Non-invasive assessment of intracranial pressure. Acta Neurol Scand. 2016;134(1):4–21. https://doi.org/10.1111/ane.12527.
Lee S, Kim YO, Baek JS, Ryu JA. The prognostic value of optic nerve sheath diameter in patients with subarachnoid hemorrhage. Crit Care. 2019;23(1):65. https://doi.org/10.1186/s13054-019-2360-6.
Sekhon MS, Griesdale DE, Robba C, McGlashan N, Needham E, Walland K, et al. Optic nerve sheath diameter on computed tomography is correlated with simultaneously measured intracranial pressure in patients with severe traumatic brain injury. Intensive Care Med. 2014;40(9):1267–74. https://doi.org/10.1007/s00134-014-3392-7.
Morgan WH, Balaratnasingam C, Lind CR, Colley S, Kang MH, House PH, et al. Cerebrospinal fluid pressure and the eye. Br J Ophthalmol. 2016;100(1):71–7. https://doi.org/10.1136/bjophthalmol-2015-306705.
Connolly ES Jr, Rabinstein AA, Carhuapoma JR, Derdeyn CP, Dion J, Higashida RT, et al. Guidelines for the management of aneurysmal subarachnoid hemorrhage: a guideline for healthcare professionals from the American Heart Association/american Stroke Association. Stroke. 2012;43(6):1711–37. https://doi.org/10.1161/STR.0b013e3182587839.
Geeraerts T, Merceron S, Benhamou D, Vigué B, Duranteau J. Non-invasive assessment of intracranial pressure using ocular sonography in neurocritical care patients. Intensive Care Med. 2008;34(11):2062–7. https://doi.org/10.1007/s00134-008-1149-x.
Geeraerts T, Launey Y, Martin L, Pottecher J, Vigué B, Duranteau J, et al. Ultrasonography of the optic nerve sheath may be useful for detecting raised intracranial pressure after severe brain injury. Intensive Care Med. 2007;33(10):1704–11.
Neri L, Storti E, Lichtenstein D. Toward an ultrasound curriculum for critical care medicine. Crit Care Med. 2007;35(5 Suppl):S290–304.
Hansen HC, Lagrèze W, Krueger O, Helmke K. Dependence of the optic nerve sheath diameter on acutely applied subarachnoidal pressure - an experimental ultrasound study. Acta Ophthalmol. 2011;89(6):e528–32. https://doi.org/10.1111/j.1755-3768.2011.02159.x.
Bäuerle J, Niesen WD, Egger K, Buttler KJ, Reinhard M. Enlarged optic nerve sheath in aneurysmal subarachnoid hemorrhage despite normal intracranial pressure. J Neuroimaging. 2016;26(2):194–6. https://doi.org/10.1111/jon.12287.
Tayal VS, Neulander M, Norton HJ, Foster T, Saunders T, Blaivas M. Emergency department sonographic measurement of optic nerve sheath diameter to detect findings of increased intracranial pressure in adult head injury patients. Ann Emerg Med. 2007;49(4):508–14.
Moretti R, Pizzi B. Optic nerve ultrasound for detection of intracranial hypertension in intracranial hemorrhage patients confirmation of previous findings in a different patient population. J Neurosurg Anesthesiol. 2009;21(1):16–20. https://doi.org/10.1097/ANA.0b013e318185996a.
Rajajee V, Vanaman M, Fletcher JJ, Jacobs TL. Optic nerve ultrasound for the detection of raised intracranial pressure. Neurocrit Care. 2011;15(3):506–15. https://doi.org/10.1007/s12028-011-9606-8.
del Saz-Saucedo P, Redondo-González O, Mateu-Mateu Á, Huertas-Arroyo R, García-Ruiz R, Botia-Paniagua E. J Sonographic assessment of the optic nerve sheath diameter in the diagnosis of idiopathic intracranial hypertension. Neurol Sci. 2016;15(361):122–7. https://doi.org/10.1016/j.jns.2015.12.032.
Rajajee V, Williamson CA, Fontana RJ, Courey AJ, Patil PG. Noninvasive intracranial pressure assessment in acute liver failure. Neurocrit Care. 2018;29(2):280–90. https://doi.org/10.1007/s12028-018-0540-x.
Acknowledgements
The authors appreciate the support of Dr. Luca Neri and Dr. Carmela Graci who offered their help for ultrasound training. The authors are grateful for the cooperation of Dr. Alessandra Merrino who helped in the acquisition of data and for the support of Dr. EJA Wiegers who helped in data analysis.
Funding
Support was provided by funds from Ricerca Corrente of Fondazione IRCCS Ca’ Granda Ospedale Maggiore Policlinico.
Author information
Authors and Affiliations
Contributions
NS, AC, TZ, and MC conceived and designed the study. AC, TZ, NS, ED, GC, SA, FT, and TB contributed to data analysis and interpretation. TZ, NS, AC, MC, FO, and ERZ critically revised the manuscript.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest in relation to this manuscript.
Ethical approval/informed consent
The institutional review board of the hospital (Ethics Committee Milan, Zone 1) approved the study, and written consent was obtained according to the regulations applied in our Institution. Number: ATTI 774/2016 - 24.05.2016
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
This work was performed at the Neuroscience Intensive Care Unit, Department of Anesthesia and Critical Care, Fondazione IRCCS Ca’ Granda Ospedale Maggiore Policlinico, Milan, Italy.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Zoerle, T., Caccioppola, A., D’Angelo, E. et al. Optic Nerve Sheath Diameter is not Related to Intracranial Pressure in Subarachnoid Hemorrhage Patients. Neurocrit Care 33, 491–498 (2020). https://doi.org/10.1007/s12028-020-00970-y
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12028-020-00970-y