Abstract
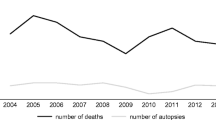
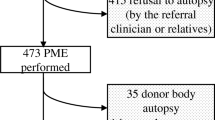
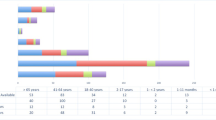
Medical autopsies have been in considerable decline for several decades, in France and worldwide. We aimed to determine whether a medical autopsy still currently has a role to play in diagnosis, by analyzing its performance and diagnostic limitations. This dual-centre retrospective descriptive study included all medical autopsies performed in the university hospitals of Lille and Marseille, France, between January 2007 and December 2012. Autopsies of fetuses or stillborn infants, or those related to sudden infant deaths and research protocols were excluded. 412 medical autopsies were included. The male:female ratio was 1.5:1 and mean age was 27.3 years. Half of all autopsies were pediatric. Regarding anatomical region and/or injury mechanism, a clinical diagnosis was suggested in 52.2% of cases, an autopsy diagnosis in 55.6% and a microscopic diagnosis in 81.8%. There was very low agreement between the clinician’s suggested diagnosis and the final diagnosis, both for organ specific diseases and cause of death. Agreement was moderate between autopsy diagnoses and microscopic diagnoses for organ specific diseases and low for cause of death. From our findings we concluded that an autopsy associated with microscopic examination was still valuable in diagnosing cause of death. Microscopic examination was indispensable to determine certain causes of death.
Similar content being viewed by others
References
Loi de bioéthique de 1994. n°94–654 juillet, 1994. http://www.legifrance.gouv.fr/affichTexte.do?cidTexte=JORFTEXT000000549618. Accessed 26 March 2019.
Loi de bioéthique de 2004. n°2004–800 août, 2004. https://www.legifrance.gouv.fr/affichTexte.do?cidTexte=JORFTEXT000000441469. Accessed 26 March 2019.
Groß D, Wilhelmy S. Clinical autopsies from a medical ethics perspective. Pathologe. 2017;38:396.
van den Tweel JG, Wittekind C. The medical autopsy as quality assurance tool in clinical medicine: dreams and realities. Virchows Arch. 2016;468:75–81.
Gosselin B, Gaillard D, Rambaud C. Les autopsies à l’aube de l’an 2000. Ann Pathol. 1999;19S:56–63.
Hauw JJ. L’Académie nationale de médecine appelle au don post-mortem de cerveau. Acad Nat Méd 2014. http://www.academie-medecine.fr/lacademie-nationale-de-medecine-appelle-au-don-post-mortem-de-cerveau-2/. Accessed 26 March 2019.
Hoyert DL. The changing profile of autopsied deaths in the United States, 1972-2007. NCHS Data Brief. 2011;67:1–8.
Royal College of Pathologists of Australasia Autopsy Working Party. The decline of the hospital autopsy: a safety and quality issue for healthcare in Australia. Med J Aust. 2004;180:281–5.
Burton JL. Necropsy practice after the “organ retention scandal”: requests, performance, and tissue retention. J Clin Pathol. 2003;56:537–41.
Chariot P, Witt K, Pautot V, et al. Declining autopsy rate in a French hospital: physician’s attitudes to the autopsy and use of autopsy material in research publications. Arch Pathol Lab Med. 2000;124:739–45.
Chatelain D, Brevet M, Guernou M, et al. Adult autopsies in a French university hospital (CHU Amiens) for the period 1975-2005. Ann Pathol. 2007;27:269–83.
Duband S, Forest F, Dumollard JM, Chambonnière-Simon ML, Clémenson A, Péoc’h M. Les autopsies médicales : analyse rétrospective des demandes et apport de leurs résultats à la communauté hospitalo-universitaire. Ann Pathol. 2009;29:4–19.
Sington JD, Cottrell BJ. Analysis of the sensitivity of death certificates in 440 hospital deaths: a comparison with necropsy findings. J Clin Pathol. 2002;55:499–502.
Sonderegger-Iseli K, Burger S, Muntwyler J, Salomon F. Diagnostic errors in three medical eras: a necropsy study. Lancet. 2000;355:2027–31.
Ornelas-Aguirre JM, Vázquez-Camacho G, Gonzalez-Lopez L, Garcia-Gonzalez A, Gamez-Nava JI. Concordance between premortem and postmortem diagnosis in the autopsy: results of a 10-year study in a tertiary care center. Ann Diagn Pathol. 2003;7:223–30.
Bernardi FDC. Histological examination has a major impact on macroscopic necropsy diagnoses. J Clin Pathol. 2005;58:1261–4.
Harris MD, Blundell JW. Audit of necropsies in a British district general hospital. J Clin Pathol. 1991;44:862–5.
Loughrey MB, McCluggage WG, Toner PG. The declining autopsy rate and clinicians’ attitudes. Ulster Med J. 2000;69:83–9.
Goldman L, Sayson R, Robbins S, Cohn LH, Bettmann M, Weisberg M. The value of the autopsy in three medical eras. N Engl J Med. 1983;308:1000–5.
Capuani C, Guilbeau-Frugier C, Dedouit F, Rougé D, Delisle MB, Telmon N. Implication des médecins légistes dans l’autopsie médicale : l’expérience toulousaine. Ann Pathol. 2013;33:87–92.
Zaitoun AM, Fernandez C. The value of histological examination in the audit of hospital autopsies: a quantitative approach. Pathology (Phila). 1998;30:100–4.
Roulson J, Benbow EW, Hasleton PS. Discrepancies between clinical and autopsy diagnosis and the value of post mortem histology; a meta-analysis and review. Histopathol. 2005;47:551–9.
Cameron HM, McGoogan E, Watson H. Necropsy: a yardstick for clinical diagnoses. Br Med J. 1980;281:985–8.
Mosquera DA, Goldman MD. Surgical audit without autopsy: tales of the unexpected. Ann R Coll Surg Engl. 1993;75:115–7.
Shanks JH, McCluggage G, Anderson NH, Toner PG. Value of the necropsy in perioperative deaths. J Clin Pathol. 1990;43:193–5.
Hunt CR, Benbow EW, Knox WF, McMahon RF, McWilliam LJ. Can histopathologists diagnose bronchopneumonia? Clin Pathol. 1995;48:120–3.
Reid WA. Cost effectiveness of routine postmortem histology. J Clin Pathol. 1987;40:459–61.
Hutchins GM. Practice guidelines for autopsy pathology. Autopsy performance. Autopsy Committee of the College of American pathologists. Arch Pathol Lab Med. 1994;118:19–25.
The Royal College of Pathologists, London. Guidelines on autopsy practice. 2002. www.rcpath.org. Accessed 26 March 2019.
Blokker BM, Wagensveld IM, Weustink AC, Oosterhuis JW, Hunink MG. Non-invasive or minimally invasive autopsy compared to conventional autopsy of suspected natural deaths in adults: a systematic review. Eur Radiol. 2016;26:1159–79.
Lewis C, Hutchinson J, Riddington M, Hill M, Arthurs O, Fisher J, et al. Feasibility study of minimally invasive autopsy for fetuses and children. Health Technol Assess. 2019;23:1–104.
Latten BGH, Bakers FCH, Hofman PAM, Zur Hausen A, Kubat B. The needle in the haystack: histology of post-mortem computed tomography guided biopsies versus autopsy derived tissue. Forensic Sci Int. 2019;302:109882.
Role of author
• Sarah Humez performed the research.
• Marie-Dominique Piercecchi and Claude Alain Maurage designed the research study.
• Julia Torrents, Caroline Capuani, Lucile Tuchtan contributed essential reagents or tools.
• Sarah Humez analysed the data.
• Clémence Delteil wrote the paper.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Research involving human participants and/or animals
No.
Ethical approval
The approval of the ethics committee was therefore not necessary.
Informed consent
The informed consent was therefore not necessary.
This research study was however notified to the representative of the Commission on Data Processing and Freedom (CNIL in French).
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Humez, S., Delteil, C., Maurage, C.A. et al. Does the medical autopsy still have a place in the current diagnostic process? A 6-year retrospective study in two French University hospitals. Forensic Sci Med Pathol 15, 564–569 (2019). https://doi.org/10.1007/s12024-019-00170-x
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12024-019-00170-x