Abstract
Background
Patients with cortisol secreting adrenal adenomas present with Cushing’s syndrome (CS), while 5–15% of subjects with adrenal incidentalomas have subclinical hypercortisolism (SH) as they have biochemical abnormalities suggesting autonomous cortisol secretion without associated clinical features of CS.
Goals
Examine HPA function immediately after resection of either of these adenomas and utilize the data to decide on initiating glucocorticoid replacement.
Methods
ACTH, cortisol, and DHEA-S levels were measured frequently for 8 h after adrenalectomy in 14 patients with CS and 19 others with incidentalomas + SH. Glucocorticoids were withheld before/during surgery and administered 6–8 h postoperatively to those who had cortisol levels of <3 ug/dL (83 nmol/L).
Results
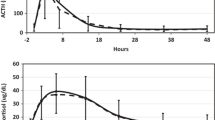
Preoperatively, incidentalomas + SH patients had larger tumors, higher ACTH, and DHEA-S but lower dexamethasone-suppressed serum cortisol levels than those with CS. Postoperatively, ACTH levels increased in both groups: (90.1 ± 31.6; 24.1 ± 14.4 ng/L, respectively; P < 0.001). Postoperative ACTH levels correlated negatively with preoperative Dexamethasone-suppressed cortisol concentrations in both groups. Patients with CS had steeper decline in cortisol concentrations than those with incidentalomas + SH. All patients with CS had hypocortisolemia requiring glucocorticoid therapy for several months, while only 5/19 with incidentalomas + SH had cortisol levels <3 ug/dL;(83 nmol/L) 6–8 h after adrenalectomy and received hydrocortisone replacement therapy for ≤4 weeks.
Conclusions
Surgical stress stimulates HPA function even in patients with hypercortisolemia. Patients with incidentalomas + SH have incomplete HPA suppression that allows more robust response to surgical stress than that observed in patients with CS. HPA assessment immediately after surgical resection of adrenal incidentalomas identified those requiring glucocorticoid replacement before discharge.




Similar content being viewed by others
References
M. Reincke, Subclinical Cushing’s syndrome. Endocrinol. Metab. Clin. North Am. 29(1), 43–56 (2000)
M. Terzolo, G. Reimondo, S. Bovio, A. Angeli, Subclinical Cushing’s syndrome. Pituitary 7(4), 217–223 (2004)
V. Morelli, B. Masserini, A.S. Salcuni, C. Eller-Vainicher, C. Savoca, R. Viti, F. Coletti, G. Guglielmi, C. Battista, L. Lorio, P. Beck-Peccoz, B. Ambrosi, M. Arosio, A. Scillitani, I. Chiodini, Subclinical hypercortisolism: correlation between biochemical diagnostic criteria and clinical aspects. Clin. Endocrinol. 73(2), 161–166 (2010)
I. Chiodini, Clinical review: diagnosis and treatment of subclinical hypercortisolism. J. Clin. Endocrinol. Metab. 96(5), 1223–1236 (2011)
M. Terzolo, A. Pia, G. Reimondo, Subclinical Cushing’s syndrome: definition and management. Clin. Endocrinol. 76(1), 12–18 (2012)
L.K. Neiman, Update on subclinical Cushing’s syndrome. Curr. Opin. Endocrinol. Diabetes Obese 22(3), 180–184 (2015)
M. Terzolo, A. Pia, A. Alì, G. Osella, G. Reimondo, S. Bovio, F. Daffara, M. Procopio, P. Paccotti, G. Borretta, A. Angeli, Adrenal incidentaloma: a new cause of the metabolic syndrome? J. Clin. Endocrinol. Metab. 87(3), 998–1003 (2002)
I. Chiodini, V. Morelli, B. Masserini, A.S. Salcuni, C. Eller-Vainicher, R. Viti, F. Coletti, G. Guglielmi, C. Battista, V. Carnevale, L. Iorio, P. Beck-Peccoz, M. Arosio, B. Ambrosi, A. Scillitani, Bone mineral density, prevalence of vertebral fractures and bone quality in patients with adrenal incidentalomas with and without subclinical hypercortisolism: an Italian Multicenter Study. J. Clin. Endocrinol. Metab. 94(9), 3207–3214 (2009)
C. Eller-Vainicher, V. Morelli, F.M. Uliveri, S. Palmieri, V.V. Zhukouskaya, E. Cairoli, R. Pino, A. Naccarato, A. Scillitani, P. Beck-Peccoz, I. Chiodini, Bone quality, as measured by trabecular bone score in patients with adrenal incidentalomas with and without subclinical hypercortisolism. J. Bone Miner. Res. 27(10), 2223–2230 (2012)
V. Morelli, C. Eller-Vainicher, A.S. Salcuni, F. Coletti, L. Iorio, G. Muscogiuri, S. Della Casa, M. Arosio, B. Ambrosi, P. Beck-peccoz, I. Chiodini, Risk of new vertebral fractures in patients with adrenal incidentaloma with and without subclinical hypercortisolism: a multicenter longitudinal study. J. Bone Miner. Res. 26(8), 1816–1821 (2011)
L. Tauchmanovà, R. Rossi, B. Biondi, M. Pulcrano, V. Nuzzo, E.A. Palmieri, S. Fazio, G. Lombardi, Patients with subclinical Cushing’s syndrome due to adrenal adenoma have increased cardiovascular risk. J. Clin. Endocrinol. Metab. 87(11), 4872–4878 (2002)
V. Morelli, G. Reimondo, Giordano, S. Della Casa, C. Policola, S. Palmieri, A.S. Salcuni, A. Dolci, M. Mendola, M. Arosio, B. Ambrosi, A. Scillitani, E. Ghigo, P. Beck-Peccoz, M. Terzolo, I. Chiodini, Long-term follow-up in adrenal incidentalomas: an Italian multicenter study. J. Clin. Endocrinol. Metab. 99(3), 827–834 (2014)
I. Chiodini, V. Morelli, A.S. Salcuni, C. Eller-Vainicher, M. Torlontano, F. Coletti, L. Iorio, A. Cuttitta, A. Ambrosio, L. Vicentini, F. Pellegrini, M. Copetti, P. Beck-Peccoz, M. Arosio, B. Ambrosi, V. Trischitta, A. Scillitani, Beneficial metabolic effects of prompt surgical treatment in patients with an adrenal incidentaloma causing biochemical hypercortisolism. J. Clin. Endocrinol. Metab. 95(6), 2736–2745 (2010)
M. Iacobone, M. Citton, M. Scarpa, G. Viel, M. Boscaro, D. Nitti, Systematic review of surgical treatment of subclinical Cushing’s syndrome. Br. J. Surg. 102(4), 318–330 (2015)
I. Akaza, T. Yoshimoto, F. Iwashima, C. Nakayama, M. Doi, H. Izumiyama, Y. Hirata, Clinical outcome of subclinical Cushing’s syndrome after surgical and conservative treatment. Hypertens. Res. 34(1), 1111–1115 (2011)
I. Bancos, F. Alahdab, R.K. Crowley, V. Chortis, D.A. Delivanis, D. Erickson, N. Natt, M. Terzolo, W. Arlt, W.F.J.R. Young, M.H. Murad, Improvement of cardiovascular risk factors after adrenalectomy in patients with adrenal tumors and subclinical Cushing’s syndrome: A systematic review and meta-Analysis. Eur. J. Endocrinol. 175(6), R283–R295 (2016)
M. Iacobone, M. Citton, G. Viel, R. Boetto, I. Bonadio, I. Mondi, S. Tropea, D. Nitti, G. Favia, Adrenalectomy may improve cardiovascular and metabolic impairment and ameliorate quality of life in patients with adrenal incidentalomas and subclinical Cushing’s syndrome. Surgery 152(6), 991–997 (2012)
M.C. Dennedy, A.K. Annmalai, O. Prankerd-Smith, N. Freeman, K. Vengopal, J. Graggaber, O. Koulouri, A.S. Powlson, A. Shaw, D.J. Halsall, M. Gunnell, Low DHEA-S: A sensitive and specific test for the detection of subclinical hypercortisolism in adrenal incidentalomas. J. Clin. Endocrinol. Metab. 102, 786–792 (2017)
C. Eller-Vainicher, V. Morelli, A.S. Salcuni, M. Torlontano, F. Coletti, L. Iorio, A. Cuttitta, A. Ambrosio, L. Vicentini, V. Carnevale, P. Beck-Peccoz, M. Arosio, B. Ambrosi, A. Scillitani, I. Chiodini, Post-surgical hypocortisolism after removal of an adrenal incidentaloma: is it predictable by an accurate endocrinological work-up before surgery? Eur. J. Endocrinol. 162(1), 91–99 (2010)
G. Di Dalmazi, C.M. Berr, M. Fassnacht, F. Beuschlein, M. Reincke, Adrenal function after adrenalectomy for subclinical hypercortisolism and Cushing’s syndrome: A systematic review of the literature. J. Clin. Endocrinol. Metab. 99, 2637–2645 (2014)
C.M. Berr, G. Di Dalmazi, A. Osswald, K. Ritzel, M. Bidlingmaier, L.L. Geyer, M. Treitl, K. Hallfeldt, W. Rachinger, N. Reisch, R. Blaser, J. Schopohl, F. Beuschlein, M. Reincke, Time to recovery of adrenal function after curative surgery for Cushing’s syndrome depends on etiology. J. Clin. Endocrinol. Metab. 100(4), 1300–1308 (2015)
M. Fassnacht, W. Arlt, I. Bancos, H. Dralle, J. Newell-Price, A. Sahdev, A. Tabarin, M. Terzolo, S. Tsagarakis, O.M. Dekkers, Management of adrenal incidentalomas: European Society of Endocrinology Clinical Practice Guideline in collaboration with the European Network for the Study of Adrenal Tumors. Eur. J. Endocrinol. 175(2), G1–G34 (2016)
S.H. Lee, K.H. Song, J. Kim, S. Park, S.H. Ahn, H. Kim, Y.Y. Cho, S. Suh, B.J. Kin, J.H. Kim, J.M. Koh, New diagnostic criteria for subclinical hypercortisolism using postsurgical hypocortisolism: the co-work of adrenal research study. Clin. Endocrinol. 86(1), 10–18 (2017)
V. Morelli, L. Minelli, C. Eller-Vainicher, S. Palmieri, E. Cairoli, A. Spada, M. Arosio, I. Chiodini, Predictability of hypoadrenalism occurrence and duration after adrenalectomy for ACTH independent hypercortisolism. J. Endocrinol. Invest. 41(4), 485–493 (2018)
D. Ortiz, J.W. Finding, T.B. Carroll, B.R. Javorsky, A.A. Carr, D.B. Evans, T.W. Yen, T.S. Wang, Cosyntropin stimulation testing on postoperative day 1 allows for selective glucocorticoid replacement therapy after adrenalectomy for hypercortisolism: Results of a novel, multidisciplinary institutional protocol. Surgery 159(1), 259–265 (2016)
B.M. Arafah, O.H. Pearson. in Cushing’s syndrome. ed. by R.E. Rakel. Conn’s Current Therapy, 36th edn., (WB Saunders Co, Philadelphia, 1984), p. 472–477
A. Krikorian, D. Abdelmannan, W.R. Selman, B.M. Arafah, Cushing disease: use of perioperative serum cortisol measurements in early determination of success following pituitary surgery. Neurosurg. Focus 23(3), E6–E11 (2007)
D. Abdelmannan, W.R. Selman, B.M. Arafah, Perioperative management of Cushing’s disease. Rev. Endocr. Metab. Disord. 11, 127–134 (2010)
D. Abdelmannan, J. Chaiban, W.R. Selman, B.M. Arafah, Recurrences of ACTH-secreting adenomas after pituitary adenomectomy can be accurately predicted by perioperative measurements of plasma ACTH levels. J. Clin. Endocrinol. Metab. 98(4), 1458–1465 (2013)
N. El Asmar, A. Rajpal, W.R. Selman, B.M. Arafah, The value of perioperative levels of ACTH, DHEA, and DHEAS and tumor size in predicting recurrence of Cushing disease. J. Clin. Endocrinol. Metab. 103(2), 477–485 (2018)
V. Bansal, N. El Asmar, W.R. Selman, B.M. Arafah, Pitfalls in the diagnosis and management of Cushing’s syndrome. Neurological. Focus 38, 1–11 (2015)
H. Derendorf, H. Mollmann, J. Barth, C. Mollmann, S. Tunn, M. Kreig, Pharmacokinetics and oral bioavailability of hydrocortisone. J. Clin. Pharmacol. 31, 473–476 (1991)
B. Chernow, R. Alexander, R.C. Smallridge, E.R. Thompson, D. Cook, D. Beardsley, M.P. Fink, C.R. Lake, J.R. Fletcher, Hormonal responses to graded surgical stress. Arch. Intern. Med. 147, 1273–1278 (1987)
R. Udelsman, J.A. Norton, S.E. Jelenich, D.S. Goldstein, W.M. Linehan, D.L. Loriaux, G.P. Chrousos, Responses of the hypothalamic-pituitary-adrenal and renin-angiotensin axes and the sympathetic system during controlled surgical and anesthetic stress. J. Clin. Endocrinol. Metab. 64, 986–994 (1987)
K. El-Sibai, A. Rajpal, W.R. Selman, B.M. Arafah, The impact peri-operative dexamethasone administration on the normal hypothalamic pituitary adrenal response to major surgical procedures. Endocrine 58, 134–142 (2017)
A.F. Cheres, N. ElAsmar, A. Rajpal, W.R. Selman, B.M. Arafah, Perioperative hypothalamic pituitary adrenal function in patients with silent corticotroph adenomas. Pituitary 20(4), 471–476 (2017)
V. Morelli, L. Minelli, C. Eller-Vainicher, S. Palmieri, E. Cairoli, A. Spada, M. Arosio, I. Chiodini, Predictability of hypoadrenalism occurrence and duration after adrenalectomy for ACTH-independent hypercortisolism. J. Endocrinol. Investig. 41, 485–493 (2018)
A. Prete, R.M. Paragliola, F. Bottiglieri, C.A. Rota, A. Pontecorvi, R. Salvatori, S.M. Corsello, Factors predicting the duration of adrenal insufficiency in patients successfully treated for Cushing’s disease an nonmalignant primary adrenal Cushing’s syndrome. Endocrine 55, 969–980 (2017)
M. Reincke, J. Nieke, G.P. Krestin, W. Saeger, B. Allolio, W. Winkelmann, Precrinical Cushing’s syndrome in adrenal incidentalomas: comparison with adrenal Cushing’s syndrome. J. Clin. Endocrinol. Metab. 75, 826–832 (1992)
Funding
Local/departmental
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Ethical approval
All procedures performed in studies involving human participants were in accordance with the ethical standards of the Institutional Review Board and with the 1964 Helsinki declaration and later amendments or comparable ethical standards.
Informed consent
An informed consent was obtained from all participants in the study.
Rights and permissions
About this article
Cite this article
Khawandanah, D., ElAsmar, N. & Arafah, B.M. Alterations in hypothalamic-pituitary-adrenal function immediately after resection of adrenal adenomas in patients with Cushing’s syndrome and others with incidentalomas and subclinical hypercortisolism. Endocrine 63, 140–148 (2019). https://doi.org/10.1007/s12020-018-1769-z
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12020-018-1769-z