Abstract
Background and aim
Impaired cortisol rhythm is a characteristic feature of Cushing’s Syndrome, nevertheless late night salivary cortisol (LNSC) is not suitable to detect subclinical hypercortisolism in patients with adrenal incidentaloma (AI). We studied daily salivary cortisol (F) and cortisone (E) rhythm in patients with AI.
Materials and methods
Six saliva samples were collected from awakening to night in 106 patients with AI and 40 controls. F and E were measured with LC-MS/MS and daily F exposure was calculated with the area under the curve (AUC).
Results
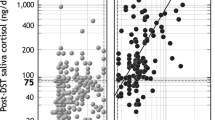
Patients with serum cortisol after dexamethasone suppression test (DST) > 50 nmol/L showed higher morning F (15.5 ± 14.5 vs. 8.6 ± 5.5 nmol/L, p = 0.001), suppressed corticotropin levels (76 vs. 35%, p < 0.001) and increased daily F exposure (3795 ± 1716 vs. 2898 ± 1478, p = 0.012), especially in the morning (2035 ± 1267 vs. 1365 ± 777, p = 0.003), otherwise LNSC levels were similar. Salivary E and AUC levels were higher in patients with DST > 50 nmol/L. AUC was not correlated with urinary cortisol levels or adenoma size. F and E levels were similar among patients with unilateral or bilateral adenoma, or considering the presence of hypertension, dyslipidemia, diabetes, or cardiovascular events.
Conclusion
Daily cortisol exposure, evaluated with AUC from multiple saliva collections, is increased in AI patients with serum cortisol > 50 nmol/L after DST, especially in the morning, leading to reduced corticotropin levels. Cortisol rhythm is preserved in patients with AI, remarking that LNSC is not a screening test for subclinical hypercortisolism.


Similar content being viewed by others
References
M. Terzolo, A. Stigliano, I. Chiodini, P. Loli, L. Furlani, G. Arnaldi, G. Reimondo, A. Pia, V. Toscano, M. Zini, G. Borretta, E. Papini, P. Garofalo, B. Allolio, B. Dupas, F. Mantero, A. Tabarin, Italian association of clinical endocrinologists. AME position statement on adrenal incidentaloma. Eur. J. Endocrinol. 6, 851–870 (2011). https://doi.org/https://doi.org/10.1530/EJE-10-1147
M. Fassnacht, W. Arlt, I. Bancos, H. Dralle, J. Newell-Price, A. Sahdev, A. Tabarin, M. Terzolo, S. Tsagarakis, O.M. Dekkers, Management of adrenal incidentalomas: European society of endocrinology clinical practice guideline in collaboration with the European network for the study of Adrenal Tumors. Eur. J. Endocrinol. 175, G1–G34 (2016). https://doi.org/10.1530/EJE-16-0467
F. Ceccato, G. Antonelli, A.C. Frigo, D. Regazzo, M. Plebani, M. Boscaro, C. Scaroni, First-line screening tests for Cushing’s syndrome in patients with adrenal incidentaloma: the role of urinary free cortisol measured by LC-MS/MS. J. Endocrinol. Invest. 40, 753–760 (2017). https://doi.org/10.1007/s40618-017-0644-8.
M. Debono, M. Bradburn, M. Bull, B. Harrison, R.J. Ross, J. Newell-Price, Cortisol as a marker for increased mortality in patients with incidental adrenocortical adenomas. J. Clin. Endocrinol. Metab. 99, 4462–4470 (2014). https://doi.org/10.1210/jc.2014-3007
G. Di Dalmazi, V. Vicennati, S. Garelli, E. Casadio, E. Rinaldi, E. Giampalma, C. Mosconi, R. Golfieri, A. Paccapelo, U. Pagotto, R. Pasquali, Cardiovascular events and mortality in patients with adrenal incidentalomas that are either non-secreting or associated with intermediate phenotype or subclinical Cushing’s syndrome: a 15-year retrospective study. Lancet Diabetes Endocrinol. 2, 396–405 (2014). https://doi.org/10.1016/S2213-8587(13)70211-0
L.K. Nieman, B.M. Biller, J.W. Findling, J. Newell-Price, M.O. Savage, P.M. Stewart, V.M. Montori, The diagnosis of Cushing’s syndrome: an Endocrine society clinical practice guideline. J. Clin. Endocrinol. Metab. 93, 1526–1540 (2008). https://doi.org/10.1210/jc.2008-0125
M. Boscaro, G. Arnaldi, Approach to the patient with possible Cushing’s syndrome. J. Clin. Endocrinol. Metab. 94, 3121–3131 (2009). https://doi.org/10.1210/jc.2009-0612
L. Plat, R. Leproult, M. L’Hermite-Baleriaux, F. Fery, J. Mockel, K.S. Polonsky, E. Van Cauter, Metabolic effects of short-term elevations of plasma cortisol are more pronounced in the evening than in the morning. J. Clin. Endocrinol. Metab. 84, 3082–3092 (1999)
B. Masserini, V. Morelli, S. Bergamaschi, F. Ermetici, C. Eller-Vainicher, A.M. Barbieri, M.A. Maffini, A. Scillitani, B. Ambrosi, P. Beck-Peccoz, I. Chiodini, The limited role of midnight salivary cortisol levels in the diagnosis of subclinical hypercortisolism in patients with adrenal incidentaloma. Eur. J. Endocrinol. 160, 87–92 (2009). https://doi.org/10.1530/EJE-08-0485
S. Palmieri, V. Morelli, E. Polledri, S. Fustinoni, R. Mercadante, L. Olgiati, C. Eller Vainicher, E. Cairoli, V.V. Zhukouskaya, P. Beck-Peccoz, I. Chiodini, The role of salivary cortisol measured by liquid chromatography-tandem mass spectrometry in the diagnosis of subclinical hypercortisolism. Eur. J. Endocrinol. 168, 289–296 (2013). https://doi.org/10.1530/EJE-12-0803
H. Raff, Measurement of Salivary Cortisone to assess the adequacy of hydrocortisone replacement. J. Clin. Endocrinol. Metab. 101, 1350–1352 (2016). https://doi.org/10.1210/jc.2016-1228
F. Ceccato, G. Antonelli, M. Barbot, M. Zilio, L. Mazzai, R. Gatti, M. Zaninotto, F. Mantero, M. Boscaro, M. Plebani, C. Scaroni, The diagnostic performance of urinary free cortisol is better than the cortisol:cortisone ratio in detecting de novo Cushing’s syndrome: the use of a LC-MS/MS method in routine clinical practice. Eur. J. Endocrinol. 171, 1–7 (2014). https://doi.org/10.1530/EJE-14-0061
J.W. Funder, R.M. Carey, F. Mantero, M.H. Murad, M. Reincke, H. Shibata, M. Stowasser, W.F. Young Jr., The management of primary aldosteronism: Case detection, diagnosis, and treatment: An endocrine society clinical practice guideline. J. Clin. Endocrinol. Metab. 101, 1889–1916 (2016). https://doi.org/10.1210/jc.2015-4061
J.W. Lenders, Q.Y. Duh, G. Eisenhofer, A.P. Gimenez-Roqueplo, S.K. Grebe, M.H. Murad, M. Naruse, K. Pacak, W.F. Young Jr, Endocrine Society. Pheochromocytoma and paraganglioma: an endocrine society clinical practice guideline. J. Clin. Endocrinol. Metab. 99, 1915–1942 (2014). https://doi.org/10.1210/jc.2014-1498
G. Antonelli, C. Artusi, M. Marinova, L. Brugnolo, M. Zaninotto, C. Scaroni, R. Gatti, F. Mantero, M. Plebani, Cortisol and cortisone ratio in urine: LC-MS/MS method validation and preliminary clinical application. Clin. Chem. Lab. Med. 52, 213–220 (2014). https://doi.org/10.1515/cclm-2013-0471
F. Ceccato, M. Barbot, M. Zilio, A.C. Frigo, N. Albiger, V. Camozzi, G. Antonelli, M. Plebani, F. Mantero, M. Boscaro, C. Scaroni, Screening tests for cushing’s syndrome: Urinary free cortisol role measured by LC-MS/MS. J. Clin. Endocrinol. Metab. 100, 3856–3861 (2015). https://doi.org/10.1210/jc.2015-2507
G. Antonelli, A. Padoan, C. Artusi, M. Marinova, M. Zaninotto, M. Plebani, Automated saliva processing for LC-MS/MS: Improving laboratory efficiency in cortisol and cortisone testing. Clin Biochem. 49, 518–520 (2016). https://doi.org/10.1016/j.clinbiochem.2015.12.006
J.C. Pruessner, C. Kirschbaum, G. Meinlschmid, D.H. Hellhammer, Two formulas for computation of the area under the curve represent measures of total hormone concentration versus time-dependent change. Psychoneuroendocrinology 28, 916–931 (2003)
H. Raff, Cushing’s syndrome: diagnosis and surveillance using salivary cortisol. Pituitary 15, 64–70 (2012). https://doi.org/10.1007/s11102-011-0333-0
F. Ceccato, M. Barbot, M. Zilio, S. Ferasin, G. Occhi, A. Daniele, S. Mazzocut, M. Iacobone, C. Betterle, F. Mantero, C. Scaroni, Performance of salivary cortisol in the diagnosis of Cushing’s syndrome, adrenal incidentaloma, and adrenal insufficiency. Eur. J. Endocrinol. 169, 31–36 (2013). https://doi.org/10.1530/EJE-13-0159
R. Bou Khalil, C. Baudry, L. Guignat, C. Carrasco, J. Guibourdenche, S. Gaillard, X. Bertagna, J. Bertherat, Sequential hormonal changes in 21 patients with recurrent Cushing’s disease after successful pituitary surgery. Eur. J. Endocrinol. 165, 729–737 (2011). https://doi.org/10.1530/EJE-11-0424
I.I. Androulakis, G.A. Kaltsas, G.E. Kollias, A.C. Markou, A.K. Gouli, D.A. Thomas, K.I. Alexandraki, C.M. Papamichael, D.J. Hadjidakis, G.P. Piaditis, Patients with apparently nonfunctioning adrenal incidentalomas may be at increased cardiovascular risk due to excessive cortisol secretion. J. Clin. Endocrinol. Metab. 99, 2754–2762 (2014). https://doi.org/10.1210/jc.2013-4064
D.A. Vassiliadi, G. Ntali, E. Vicha, S. Tsagarakis, High prevalence of subclinical hypercortisolism in patients with bilateral adrenal incidentalomas: a challenge to management. Clin. Endocrinol. 74, 438–444 (2011). https://doi.org/10.1111/j.1365-2265.2010.03963.x
E. Vassilatou, A. Vryonidou, D. Ioannidis, S.A. Paschou, M. Panagou, I. Tzavara, Bilateral adrenal incidentalomas differ from unilateral adrenal incidentalomas in subclinical cortisol hypersecretion but not in potential clinical implications. Eur. J. Endocrinol. 171, 37–45 (2014). https://doi.org/10.1530/EJE-13-0848
V. Morelli, S. Palmieri, A.S. Salcuni, C. Eller-Vainicher, E. Cairoli, V. Zhukouskaya, A. Scillitani, P. Beck-Peccoz, I. Chiodini, Bilateral and unilateral adrenal incidentalomas: biochemical and clinical characteristics. Eur. J. Endocrinol. 168, 235–241 (2013). https://doi.org/10.1530/EJE-12-0777
L. Petramala, G. Cavallaro, M. Galassi, C. Marinelli, G. Tonnarini, A. Concistrè, U. Costi, M. Bufi, P. Lucia, G. De Vincentis, G. Iannucci, G. De Toma, C. Letizia, Clinical benefits of unilateral adrenalectomy in patients with subclinical hypercortisolism due to adrenal incidentaloma: Results from a single center. High Blood Press Cardiovasc. Prev. 24, 69–75 (2017). https://doi.org/10.1007/s40292-017-0182-7
S.A. Paschou, E. Kandaraki, F. Dimitropoulou, D.G. Goulis, A. Vryonidou, Subclinical Cushing’s syndrome in patients with bilateral compared to unilateral adrenal incidentalomas: a systematic review and meta-analysis. Endocrine 51, 225–235 (2016). https://doi.org/10.1007/s12020-015-0776-6
A. Toniato, I. Merante-Boschin, G. Opocher, M.R. Pelizzo, F. Schiavi, E. Ballotta, Surgical versus conservative management for subclinical Cushing syndrome in adrenal incidentalomas: a prospective randomized study. Ann. Surg. 249, 388–391 (2009). https://doi.org/10.1097/SLA.0b013e31819a47d2
M. Iacobone, M. Citton, G. Viel, R. Boetto, I. Bonadio, I. Mondi, S. Tropea, D. Nitti, G. Favia, Adrenalectomy may improve cardiovascular and metabolic impairment and ameliorate quality of life in patients with adrenal incidentalomas and subclinical Cushing’s syndrome. Surgery 152, 991–997 (2012). https://doi.org/10.1016/j.surg.2012.08.054
I. Perogamvros, D.A. Vassiliadi, O. Karapanou, E. Botoula, M. Tzanela, S. Tsagarakis, Biochemical and clinical benefits of unilateral adrenalectomy in patients with subclinical hypercortisolism and bilateral adrenal incidentalomas. Eur. J. Endocrinol. 173, 719–725 (2015). https://doi.org/10.1530/EJE-15-0566
I. Chiodini, A. Albani, A.G. Ambrogio, M. Campo, M.C. De Martino, G. Marcelli, V. Morelli, B. Zampetti, A. Colao, R. Pivonello, A.B.C. Group, Six controversial issues on subclinical Cushing’s syndrome. Endocrine 56, 262–266 (2017). https://doi.org/10.1007/s12020-016-1017-3
H. Raff, J.W. Findling, Biomarkers: Salivary cortisol or cortisone? Nat. Rev. Endocrinol. 6, 658–660 (2010). https://doi.org/10.1038/nrendo.2010.192
I. Perogamvros, B.G. Keevil, D.W. Ray, P.J. Trainer, Salivary cortisone is a potential biomarker for serum free cortisol. J. Clin. Endocrinol. Metab. 95, 4951–4958 (2010). https://doi.org/10.1210/jc.2010-1215
M. Debono, R.F. Harrison, M.J. Whitaker, D. Eckland, W. Arlt, B.G. Keevil, R.J. Ross, Salivary cortisone reflects cortisol exposure under physiological conditions and after hydrocortisone. J. Clin. Endocrinol. Metab. 101, 1469–1477 (2016). https://doi.org/10.1210/jc.2015-3694
G.Å. Ueland, P. Methlie, R. Kellmann, M. Bjørgaas, B.O. Åsvold, K. Thorstensen, O. Kelp, H.B. Thordarson, G. Mellgren, K. Løvås, E.S. Husebye, Simultaneous assay of cortisol and dexamethasone improved diagnostic accuracy of the dexamethasone suppression test. Eur. J. Endocrinol. 176, 705–713 (2017). https://doi.org/10.1530/EJE-17-0078
H. Raff, R.J. Singh, Measurement of late-night salivary cortisol and cortisone by LC-MS/MS to assess preanalytical sample contamination with topical hydrocortisone. Clin. Chem. 58, 947–948 (2012). https://doi.org/10.1373/clinchem.2012.182717
E. Valassi, I. Crespo, B.G. Keevil, A. Aulinas, E. Urgell, A. Santos, P.J. Trainer, S.M. Webb, Affective alterations in patients with Cushing’s syndrome in remission are associated with decreased BDNF and cortisone levels. Eur. J. Endocrinol. 176, 221–231 (2017). https://doi.org/10.1530/EJE-16-0779
S.A. Morgan, Z.K. Hassan-Smith, G.G. Lavery, Mechanisms in endocrinology: Tissue-specific activation of cortisol in Cushing’s syndrome. Eur. J. Endocrinol. 175, R83–R89 (2016). https://doi.org/10.1530/EJE-15-1237
B. Mariniello, V. Ronconi, S. Rilli, P. Bernante, M. Boscaro, F. Mantero, G. Giacchetti, Adipose tissue 11beta-hydroxysteroid dehydrogenase type 1 expression in obesity and Cushing’s syndrome. Eur. J. Endocrinol. 155, 435–441 (2006). https://doi.org/10.1530/eje.1.02228
J.E. Adaway, B.G. Keevil, L.J. Owen, Liquid chromatography tandem mass spectrometry in the clinical laboratory. Ann. Clin. Biochem. 52, 18–38 (2015). https://doi.org/10.1177/0004563214557678
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no competing interests.
Rights and permissions
About this article
Cite this article
Ceccato, F., Barbot, M., Albiger, N. et al. Daily salivary cortisol and cortisone rhythm in patients with adrenal incidentaloma. Endocrine 59, 510–519 (2018). https://doi.org/10.1007/s12020-017-1421-3
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12020-017-1421-3