Abstract
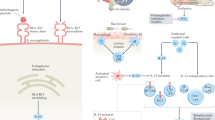
During the past decade, the well-known disease called ankylosing spondylitis has come to be considered as a subset of the broader entity referred as axial spondyloarthritis (axSpA), which also includes non-radiographic axSpA. The need of this new classification was aimed to improve the sensitivity for an early diagnosis, to reduce diagnostic delay, and to allow an early treatment. Although there is improvement in the recognition, the management of patients, and the treatment strategies of axSpA, unmet needs persist. There is still a substantial gap of 5–8 years between the onset of symptoms and the diagnosis of axSpA and, even in patients diagnosed early, 20–40% of them do not respond or have a loss of response to anti-TNF treatment. Moreover, the pathogenesis of the disease and, in particular, the mechanisms of new bone formation are far to be completely understood. Nevertheless, the discovery of IL-23/IL-17 axis with the development of biologic inhibitors, the identification of new subsets of effector cells, together with the interest in the detection of potential biomarkers of bone formation brought the approach to axSpA into a new era. This review is intended to enhance awareness and understanding of axSpA and to identify and discuss the current unmet needs in axSpA, including diagnosis, classification, biomarkers, pathogenesis, management, and treatment strategies.

Similar content being viewed by others
References
Gladman DD, Antoni C, Mease P et al (2005) Psoriatic arthritis: epidemiology, clinical features, course and outcome. Ann Rheum Dis 64:14–17
Palazzi C, D’Angelo S, Lubrano E, Olivieri I (2008) Aortic involvement in ankylosing spondylitis. Clin Exp Rheumatol 26:S131–S134
Rudwaleit M, van der Heijde D, Landewé R, Listing J, Akkoc N, Brandt J et al (2009) The development of Assessment of SpondyloArthritis international Society classification criteria for axial spondyloarthritis (part II): validation and final selection. Ann Rheum Dis 68:777–783
Van der Linden S, Valkenburg HA, Cats A (1984) Evaluation of diagnostic criteria for ankylosing spondylitis. A proposal for modification of the New York criteria. Arthritis Rheum 27:361–368
Masson Behar V, Dougados M, Etcheto A, Kreis S, Fabre S, Hudry C, Dadoun S, Rein C, Pertuiset E, Fautrel B, Gossec L (2016) Diagnostic delay in axial spondyloarthritis: a cross-sectional study of 432 patients. Joint Bone Spine 84:467–471. doi:10.1016/j.jbspin.2016.06.005
Rudwaleit M, Khan MA, Sieper J (2005) The challenge of diagnosis and classification in early ankylosing spondylitis: do we need new criteria? Arthritis Rheum 52:1000–1008
Sieper J, van der Heijde D (2013) Review: nonradiographic axial spondyloarthritis: new definition of an old disease? Arthritis Rheum 65:543–551
van der Linden S, Akkoc N, Brown MA, Robinson PC, Khan MA (2015) The ASAS criteria for axial spondyloarthritis: strengths, weaknesses, and proposals for a way forward. Curr Rheumatol Rep. doi:10.1007/s11926-015-0535-y
Wallman JK, Kapetanovic MC, Petersson IF, Geborek P, Kristensen LE (2015) Comparison of non-radiographic axial spondyloarthritis and ankylosing spondylitis patients baseline characteristics, treatment adherence, and development of clinical variables during three years of anti-TNF therapy in clinical practice. Arthritis Res Ther 17:378. doi:10.1186/s13075-015-0897-6
Moltó A, Paternotte S, van der Heijde D, Claudepierre P, Rudwaleit M, Dougados M (2015) Evaluation of the validity of the different arms of the ASAS set of criteria for axial spondyloarthritis and description of the different imaging abnormalities suggestive of spondyloarthritis: data from the DESIR cohort. Ann Rheum Dis 74:746–751
Akkoc N, Khan MA (2016) ASAS classification criteria for axial spondyloarthritis: time to modify. Clin Rheumatol 35:1415–1423
Poddubnyy D, Rudwaleit M, Haibel H, Listing J, Märker-Hermann E, Zeidler H, Braun J, Sieper J (2011) Rates and predictors of radiographic sacroiliitis progression over 2 years in patients with axial spondyloarthritis. Ann Rheum Dis 70:1369–1374
Dean LE, Jones GT, MacDonald AG, Downham C, Sturrock RD, Macfarlane GJ (2014) Global prevalence of ankylosing spondylitis. Rheumatology (Oxford) 53:650–657
Hamilton L, Macgregor A, Toms A, Warmington V, Pinch E, Gaffney K (2015) The prevalence of axial spondyloarthritis in the UK: a cross-sectional cohort study. BMC Musculoskelet Disord 16:392. doi:10.1186/s12891-015-0853-2
Poddubnyy D, van Tubergen A, Landewé R, Sieper J, van der Heijde D (2015) Assessment of SpondyloArthritis international Society (ASAS). Development of an ASAS-endorsed recommendation for the early referral of patients with a suspicion of axial spondyloarthritis. Ann Rheum Dis 74:1483–1487
Feldtkeller E, Khan MA, van der Heijde D et al (2003) Age at disease onset and diagnosis delay in HLA-B27 negative vs. positive patients with ankylosing spondylitis. Rheumatol Int 23:61–66
Poddubnyy D, Vahldiek J, Spiller I et al (2011) Evaluation of 2 screening strategies for early identification of patients with axial spondyloarthritis in primary care. J Rheumatol 38:2452–2460
Sieper J, Srinivasan S, Zamani O et al (2013) Comparison of two referral strategies for diagnosis of axial spondyloarthritis: the Recognising and Diagnosing Ankylosing Spondylitis Reliably (RADAR) study. Ann Rheum Dis 72:1621–1627
Rudwaleit M, van der Heijde D, Khan MA, Braun J, Sieper J (2004) How to diagnose axial spondyloarthritis early. Ann Rheum Dis 63:535–543
van den Berg R, de Hooge M, Rudwaleit M, et al (2013) ASAS modification of the Berlin algorithm for diagnosing axial spondyloarthritis: results from the SPondyloArthritis Caught Early (SPACE)-cohort and from the Assessment of SpondyloArthritis international Society (ASAS)-cohort. Ann Rheum Disb72:1646–1653
Reveille JD, Hirsch R, Dillon CF, Carroll MD, Weisman MH (2012) The prevalence of HLA-B27 in the US: data from the US National Health and Nutrition Examination Survey, 2009. Arthritis Rheum 64:1407–1411
Cortes A, Hadler J, Pointon JP, Robinson PC, Karaderi T, Leo P et al (2013) Identification of multiple risk variants for ankylosing spondylitis through high-density genotyping of immune-related loci. Nat Genet 45:730–738
Robinson PC, Claushuis TA, Cortes A, Martin TM, Evans DM, Leo P et al (2015) Genetic dissection of acute anterior uveitis reveals similarities and differences in associations observed with ankylosing spondylitis. Arthritis Rheumatol 67:140–151
Cortes A, Maksymowych WP, Wordsworth BP, Inman RD, Danoy P, Rahman P et al (2015) Association study of genes related to bone formation and resorption and the extent of radiographic change in ankylosing spondylitis. Ann Rheum Dis 74:1387–1393
Rudwaleit M, Haibel H, Baraliakos X, Listing J, Marker-Hermann E, Zeidler H et al (2009) The early disease stage in axial spondylarthritis: results from the German Spondyloarthritis Inception Cohort. Arthritis Rheum 60:717–727
Turina MC, Yeremenko N, van Gaalen F, van Oosterhout M, Berg IJ, Ramonda R, Lebre CM, Landewé R, Baeten D (2017) Serum inflammatory biomarkers fail to identify early axial spondyloarthritis: results from the SpondyloArthritis Caught Early (SPACE) cohort. RMD Open. doi:10.1136/rmdopen-2016-000319
Poddubnyy D, Haibel H, Listing J, Märker-Hermann E, Zeidler H, Braun J, Sieper J, Rudwaleit M (2012) Baseline radiographic damage, elevated acute-phase reactant levels, and cigarette smoking status predict spinal radiographic progression in early axial spondylarthritis. Arthritis Rheum 64:1388–1398
Glintborg B, Ostergaard M, Krogh NS, Dreyer L, Kristensen HL, Hetland ML (2010) Predictors of treatment response and drug continuation in 842 patients with ankylosing spondylitis treated with anti-tumour necrosis factor: results from 8 years’ surveillance in the Danish nationwide DANBIO registry. Ann Rheum Dis 69:2002–2008
Vastesaeger N, van der Heijde D, Inman RD, Wang Y, Deodhar A et al (2011) Predicting the outcome of ankylosing spondylitis therapy. Ann Rheum Dis 70:973–981
Perrotta FM, Addimanda O, Ramonda R, D'Angelo S, Lubrano E, Marchesoni A, Olivieri I, Punzi L, Salvarani C, Spadaro A (2014) Predictive factors for partial remission according to the Ankylosing Spondylitis Assessment Study working group in patients with ankylosing spondylitis treated with anti-TNFα drugs. Reumatismo 66:208–214. doi:10.4081/reumatismo.2014.756
Sieper J, van der Heijde D, Dougados M, Mease PJ, Maksymowych WP, Brown MA, Arora V, Pangan AL (2013) Efficacy and safety of adalimumab in patients with non-radiographic axial spondyloarthritis: results of a randomized placebo-controlled trial (ABILITY-1). Ann Rheum Dis 72:815–822
Klingberg E, Nurkkala M, Carlsten H, Forsblad-d'Elia H (2014) Biomarkers of bone metabolism in ankylosing spondylitis in relation to osteoproliferation and osteoporosis. J Rheumatol 41:1349–1356
Appel H, Ruiz-Heiland G, Listing J, Zwerina J, Herrmann M, Mueller R, Haibel H, Baraliakos X, Hempfing A, Rudwaleit M, Sieper J, Schett G (2009) Altered skeletal expression of sclerostin and its link to radiographic progression in ankylosing spondylitis. Arthritis Rheum 60:3257–3262
Shi J, Ying H, Du J, Shen B (2017) Serum sclerostin levels in patients with ankylosing spondylitis and rheumatoid arthritis: a systematic review and meta-analysis. Biomed Res Int. doi:10.1155/2017/9295313
Mattey DL, Packham JC, Nixon NB, Coates L, Creamer P, Hailwood S, Taylor GJ, Bhalla AK (2012) Association of cytokine and matrix metalloproteinase profiles with disease activity and function in ankylosing spondylitis. Arthritis Res Ther. doi:10.1186/ar3857
Arends S, van der Veer E, Groen H, Houtman PM, Jansen TL, Leijsma MK et al (2011) Serum MMP-3 level as a biomarker for monitoring and predicting response to etanercept treatment in ankylosing spondylitis. J Rheumatol 38:1644–1650
Keyszer G, Lambiri I, Nagel R, Keysser C, Keysser M, GromnicaIhle E et al (1999) Circulating levels of matrix metalloproteinases MMP-3 and MMP-1, tissue inhibitor of metalloproteinases 1 (TIMP-1), and MMP-1/TIMP-1 complex in rheumatic disease. Correlation with clinical activity of rheumatoid arthritis versus other surrogate markers. J Rheumatol 26:251–258
Maksymowych WP, Landewé R, Conner-Spady B, Dougados M, Mielants H, van der Tempel H, Poole AR, Wang N, van der Heijde D (2007) Serum matrix metalloproteinase 3 is an independent predictor of structural damage progression in patients with ankylosing spondylitis. Arthritis Rheum 56:1846–1853
Matzkies FG, Targan SR, Berel D, Landers CJ, Reveille JD, McGovern DP, Weisman MH (2012) Markers of intestinal inflammation in patients with ankylosing spondylitis: a pilot study. Arthritis Res Ther 14:R261. doi:10.1186/ar4106
Hammer HB, Kvien TK, Glennås A, Melby K (1995) A longitudinal study of calprotectin as an inflammatory marker in patients with reactive arthritis. Clin Exp Rheumatol 13:59–64
Turina MC, Yeremenko N, Paramarta JE, De Rycke L, Baeten D (2014) Calprotectin (S100A8/9) as serum biomarker for clinical response in proof-of-concept trials in axial and peripheral spondyloarthritis. Arthritis Res Ther 16:413. doi:10.1186/s13075-014-0413-4
Reveille JD (2015) Biomarkers for diagnosis, monitoring of progression, and treatment responses in ankylosing spondylitis and axial spondyloarthritis. Clin Rheumatol 34:1009–1018
Kim YG, Sohn DH, Zhao X, Sokolove J, Lindstrom TM, Yoo B, Lee CK, Reveille JD, Taurog JD, Robinson WH (2014) Role of protein phosphatase magnesium-dependent 1A and anti-protein phosphatase magnesium-dependent 1A autoantibodies in ankylosing spondylitis. Arthritis Rheumatol 66:2793–2803
Baraliakos X, Baerlecken N, Witte T, Heldmann F, Braun J (2014) High prevalence of anti-CD74 antibodies specific for the HLA class II-associated invariant chain peptide (CLIP) in patients with axial spondyloarthritis. Ann Rheum Dis 73:1079–1082
van der Linden SM, Valkenburg HA, de Jongh BM, Cats A (1984) The risk of developing ankylosing spondylitis in HLA-B27 positive individuals. A comparison of relatives of spondylitis patients with the general population. Arthritis Rheum 27:241–249
Brewerton DA, Hart FD, Nicholls A, Caffrey M, James DC, Sturrock RD (1973) Ankylosing spondylitis and HL-A 27. Lancet 1:904–907
Khan MA (2013) Polymorphism of HLAB27: 105 subtypes currently known. Curr Rheumatol Rep 15:362. doi:10.1007/s11926-013-0362-y
Lin H, Gong YZ (2017) Association of HLA-B27 with ankylosing spondylitis and clinical features of the HLA-B27-associated ankylosing spondylitis: a meta-analysis. Rheumatol Int oi. doi:10.1007/s00296-017-3741-3742
Taurog JD, Chhabra A, Colbert RA (2016) Ankylosing spondylitis and axial spondyloarthritis. N Engl J Med 374:2563–2574
Tran TM, Hong S, Edwan JH, Colbert RA (2016) ERAP1 reduces accumulation of aberrant and disulfide-linked forms of HLA-B27 on the cell surface. Mol Immunol 74:10–17
Miossec P, Kolls JK (2012) Targeting IL-17 and TH17 cells in chronic inflammation. Nat Rev Drug Discov 11:763–776
Kolls JK, Linden A (2004) Interleukin-17 family members and inflammation. Immunity 21:467–476
Marinoni B, Ceribelli A, Massarotti MS et al (2014) The Th17 axis in psoriatic disease: pathogenetic and therapeutic implications. Auto Immun Highlights 5:9–19
Trinchieri G (2003) Interleukin-12 and the regulation of innate resistance and adaptive immunity. Nat Rev Immunol 3:133–146
Oppmann B, Lesley R, Blom B et al (2000) Novel p19 protein engages IL-12p40 to form a cytokine, IL-23, with biological activities similar as well as distinct from IL-12. Immunity 13:715–725
Smith JA, Colbert RA (2014) Review: the interleukin-23/interleukin-17 axis in spondyloarthritis pathogenesis: Th17 and beyond. Arthritis Rheumatol 66:231–241
Ciccia F, Ferrante A, Triolo G (2016) Intestinal dysbiosis and innate immune responses in axial spondyloarthritis. Curr Opin Rheumatol 28:352–358
Lories RJ, Luyten FP, de Vlam K (2009) Progress in spondylarthritis. Mechanisms of new bone formation in spondyloarthritis. Arthritis Res Ther 11:221. doi:10.1186/ar2642
van Duivenvoorde LM, Dorris ML, Satumtira N, van Tok MN, Redlich K, Tak PP, Taurog JD, Baeten DL (2012) Relationship between inflammation, bone destruction, and osteoproliferation in the HLA-B27/human β2 -microglobulin-transgenic rat model of spondylarthritis. Arthritis Rheum 64:3210–3219
Sieper J, Listing J, Poddubnyy D, Song IH, Hermann KG, Callhoff J, Syrbe U, Braun J, Rudwaleit M (2016) Effect of continuous versus on-demand treatment of ankylosing spondylitis with diclofenac over 2 years on radiographic progression of the spine: results from a randomised multicentre trial (ENRADAS). Ann Rheum Dis 75:1438–1443
Spadaro A, Punzi L, Marchesoni A et al (2010) Switching from infliximab or etanercept to adalimumab in resistant or intollerant patients with spondyloarthritis: a 4-year study. Rheumatology (Oxford) 49:1107–1111. doi:10.1093/rheumatology/keq008
Lubrano E, Parsons WJ, Perrotta FM (2016) Assessment of response to treatment, remission, and minimal disease activity in axial psoriatic arthritis treated with tumor necrosis factor inhibitors. J Rheumatol 43:918–923. doi:10.3899/jrheum.151404
Spadaro A, Lubrano E, Marchesoni A et al (2013) Remission in ankylosing spondylitis treated with anti-TNF-α drugs: a national multicentre study. Rheumatology (Oxford) 52:1914–1919
Callhoff J, Sieper J, Weiß A, Zink A, Listing J (2015) Efficacy of TNFα blockers in patients with ankylosing spondylitis and non-radiographic axial spondyloarthritis: a meta-analysis. Ann Rheum Dis 74:1241–1248
Sieper J, Kivitz A, van Tubergen A, Deodhar A, Coteur G, Woltering F, Landewé R (2015) Impact of certolizumab pegol on patient-reported outcomes in patients with axial spondyloarthritis. Arthritis Care Res (Hoboken) 67:1475–1480
van der Heijde D, Joshi A, Pangan AL, Chen N, Betts K, Mittal M, Bao Y (2016). ASAS40 and ASDAS clinical responses in the ABILITY-1 clinical trial translate to meaningful improvements in physical function, health-related quality of life and work productivity in patients with non-radiographic axial spondyloarthritis Rheumatology (Oxford) 55:80–88
Wu C, Wang S, Xian P, Yang L, Chen Y, Mo X (2016) Effect of anti-TNF antibodies on clinical response in rheumatoid arthritis patients: a meta-analysis. Biomed Res Int. doi:10.1155/2016/7185708
Maneiro JR, Souto A, Salgado E, Mera A, Gomez-Reino JJ (2015) Predictors of response to TNF antagonists in patients with ankylosing spondylitis and psoriatic arthritis: systematic review and meta-analysis. RMD Open. doi:10.1136/rmdopen-2014-0000171
Ritchlin C, Rahman P, Kavanaugh A et al (2014) PSUMMIT 2 Study Group. Efficacy and safety of the anti-IL-12/23 p40 monoclonal antibody, ustekinumab, in patients with active psoriatic arthritis despite conventional non-biological and biological anti-tumour necrosis factor therapy: 6-month and 1-year results of the phase 3, multicentre, double-blind, placebo controlled, randomized PSUMMIT 2 trial. Ann Rheum Dis 73:990–999
Deodhar A, Gottlieb AB, Boehncke WB et al (2016) Efficacy and safety results of guselkumab, an anti-IL23 monoclonal antibody, in patients with active psoriatic arthritis over 24 weeks: a phase 2a, randomized, double-blind, placebo-controlled study. Poster session presented at ACR/ARHP Annual Meeting; 2016; Washington, DC.
Poddubnyy D, Hermann KG, Callhoff J, Listing J, Sieper J (2014) Ustekinumab for the treatment of patients with active ankylosing spondylitis: results of a 28-week, prospective, open-label, proof-of-concept study (TOPAS). Ann Rheum Dis 73:817–823
Baeten D, Baraliakos X, Braun J et al (2013) Anti-interleukin-17A monoclonal antibody secukinumab in treatment of ankylosing spondylitis: a randomised, double-blind, placebo-controlled trial. Lancet 382:1705–1713
Baeten D, Sieper J, Braun J et al (2015) MEASURE 1 study group; MEASURE 2 study group. Secukinumab, an interleukin-17A inhibitor, in ankylosing spondylitis. N Engl J Med 373:2534–2548
Baraliakos X, Deodhar A, Braun J et al (2015) Effect of interleukin-17A inhibition on spinal radiographic changes through 2 years in patients with active ankylosing spondylitis: results of a phase 3 study with secukinumab [abstract]. Arthritis Rheumatol; 67 (suppl 10)
Smolen JS, Braun J, Dougados M, Emery P, Fitzgerald O, Helliwell P et al (2014) Treating spondyloarthritis, including ankylosing spondylitis and psoriatic arthritis, to target: recommendations of an international task force. Ann Rheum Dis 73:6–16
Perrotta FM, Guerra G, De Socio A, Scriffignano S, Lubrano E (2017) Mesenchimal stem cells: a possible role in the pathogenesis and treatment of spondyloarthritis. Reumatismo 69:1–8
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflicts of Interest
The authors declare that there is no conflict of interest. No funds were used or accepted for the preparation of this manuscript.
Research Involving Human Participants and/or Animals
Not applicable.
Informed Consent
Not applicable.
Rights and permissions
About this article
Cite this article
Lubrano, E., De Socio, A. & Perrotta, F.M. Unmet Needs in Axial Spondyloarthritis. Clinic Rev Allerg Immunol 55, 332–339 (2018). https://doi.org/10.1007/s12016-017-8637-0
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12016-017-8637-0