Abstract
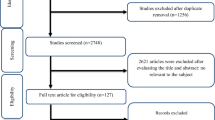
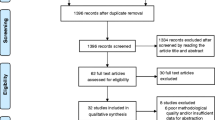
The prevalence of cardiometabolic risk factors has been increasing worldwide. The results of reported studies on the effects of zinc supplementation on cardiometabolic risk factors are unequivocal. This systematic review and meta-analysis of randomized controlled trials was conducted to evaluate the effects of zinc supplementation on cardiometabolic risk factors. A systematic search was conducted through international databases (PubMed/Medline, Institute of Scientific Information, and Scopus) until December 2018 to include all randomized controlled trials (RCT), quasi-RCT, and controlled clinical trials which assessed the effect of zinc supplementation on cardiometabolic risk factors including lipid profile, glycemic indices, blood pressure, and anthropometric indices. Random- or fixed-effects meta-analysis method was used to estimate the standardized mean difference (SMD) and 95% confidence interval (CI). A total of 20 studies were included in the meta-analysis, which included a total of 1141 participants in the intervention group. Meta-analysis showed that zinc supplementation significantly decreased plasma levels of triglyceride (SMD − 0.66, 95% CI − 1.27, − 0.06), very-low-density lipoprotein (SMD − 1.59, 95% CI − 2.86, − 0.31), and total cholesterol (SMD − 0.65, 95% CI − 1.15, − 0.15). Similarly, zinc supplementation significantly decreased fasting blood glucose (SMD − 0.52, 95% CI − 0.96, − 0.07) and HbA1c (SMD − 0.64, 95% CI − 1.27, − 0.02). The effects of zinc supplementation on blood pressure and anthropometric indices were not statistically significant (P > 0.05). Zinc supplements had beneficial effects on glycemic indices and lipid profile. Thus, it appeared that zinc supplementation might be associated with a decrease in cardiometabolic risk factors contributing to a reduction in risk of atherosclerosis.





Similar content being viewed by others
Availability of Data and Material
Yes.
References
Maret W, Li Y (2009) Coordination dynamics of zinc in proteins. Chem Rev 109(10):4682–4707
Kambe T, Tsuji T, Hashimoto A, Itsumura N (2015) The physiological, biochemical, and molecular roles of zinc transporters in zinc homeostasis and metabolism. Physiol Rev 95(3):749–784
Hara T, Takeda T-A, Takagishi T, Fukue K, Kambe T, Fukada T (2017) Physiological roles of zinc transporters: molecular and genetic importance in zinc homeostasis. J Physiol Sci 67(2):283–301
Olechnowicz J, Tinkov A, Skalny A, Suliburska J (2017) Zinc status is associated with inflammation, oxidative stress, lipid, and glucose metabolism. J Physiol Sci:1–13
Hambidge KM, Krebs NF (2007) Zinc deficiency: a special challenge. J Nutr 137(4):1101–1105
Black RE (2003) Zinc deficiency, infectious disease and mortality in the developing world. J Nutr 133(5):1485S–1489S
Gunasekara P, Hettiarachchi M, Liyanage C, Lekamwasam S (2011) Effects of zinc and multimineral vitamin supplementation on glycemic and lipid control in adult diabetes. Diabetes Metab Syndr Obes Targets Ther:4 [53–60 pp.]. Available from: http://onlinelibrary.wiley.com/o/cochrane/clcentral/articles/792/CN-00891792/frame.html
Foster M, Samman S (2010) Zinc and redox signaling: perturbations associated with cardiovascular disease and diabetes mellitus. Antioxid Redox Signal 13(10):1549–1573
Cooper GJ, Chan Y-K, Dissanayake AM, Leahy FE, Keogh GF, Frampton CM, Gamble GD, Brunton DH, Baker JR, Poppitt SD (2005) Demonstration of a hyperglycemia-driven pathogenic abnormality of copper homeostasis in diabetes and its reversibility by selective chelation: quantitative comparisons between the biology of copper and eight other nutritionally essential elements in normal and diabetic individuals. Diabetes. 54(5):1468–1476
Anderson RA, Roussel AM, Zouari N, Mahjoub S, Matheau JM, Kerkeni A (2001) Potential antioxidant effects of zinc and chromium supplementation in people with type 2 diabetes mellitus. J Am Coll Nutr 20(3) [212–8 pp.]. Available from: http://onlinelibrary.wiley.com/o/cochrane/clcentral/articles/223/CN-00373223/frame.html
Guler I, Himmetoglu O, Turp A, Erdem A, Erdem M, Onan MA, Taskiran C, Taslipinar MY, Guner H (2014) Zinc and homocysteine levels in polycystic ovarian syndrome patients with insulin resistance. Biol Trace Elem Res 158(3):297–304
Costarelli L, Muti E, Malavolta M, Cipriano C, Giacconi R, Tesei S, Piacenza F, Pierpaoli S, Gasparini N, Faloia E, Tirabassi G, Boscaro M, Polito A, Mauro B, Maiani F, Raguzzini A, Marcellini F, Giuli C, Papa R, Emanuelli M, Lattanzio F, Mocchegiani E (2010) Distinctive modulation of inflammatory and metabolic parameters in relation to zinc nutritional status in adult overweight/obese subjects. J Nutr Biochem 21(5):432–437
Yubero-Serrano EM, Delgado-Lista J, Pena-Orihuela P, Perez-Martinez P, Fuentes F, Marin C et al (2013) Oxidative stress is associated with the number of components of metabolic syndrome: LIPGENE study. Exp Mol Med 45(6):e28
Beattie JH, Gordon MJ, Rucklidge GJ, Reid MD, Duncan GJ, Horgan GW, Cho YE, Kwun IS (2008) Aorta protein networks in marginal and acute zinc deficiency. Proteomics 8(10):2126–2135
Ahn B-I, Kim MJ, Koo HS, Seo N, Joo N-S, Kim Y-S (2014) Serum zinc concentration is inversely associated with insulin resistance but not related with metabolic syndrome in nondiabetic Korean adults. Biol Trace Elem Res 160(2):169–175
Govindarajan G, Whaley-Connell A, Mugo M, Stump C, Sowers JR (2005) The cardiometabolic syndrome as a cardiovascular risk factor. Am J Med Sci 330(6):311–318
Afkhami-Ardekani M, Karimi M, Mohammadi SM, Nourani F (2008) Effect of zinc sulfate supplementation on lipid and glucose in type 2 diabetic patients. Pak J Nutr 7(4) [550–3 pp.]. Available from: http://onlinelibrary.wiley.com/o/cochrane/clcentral/articles/215/CN-00708215/frame.html
Partida-Hernández G, Arreola F, Fenton B, Cabeza M, Román-Ramos R, Revilla-Monsalve MC (2006) Effect of zinc replacement on lipids and lipoproteins in type 2-diabetic patients. Biomed Pharmacother 60(4) [161–8 pp]. Available from: http://onlinelibrary.wiley.com/o/cochrane/clcentral/articles/446/CN-00570446/frame.html
Momen-Heravi M, Barahimi E, Razzaghi R, Bahmani F, Gilasi HR, Asemi Z (2017) The effects of zinc supplementation on wound healing and metabolic status in patients with diabetic foot ulcer: a randomized, double-blind, placebo-controlled trial. Wound Repair Regen 25(3):512–520
Payahoo L, Ostadrahimi A, Mobasseri M, Bishak YK, Farrin N, Jafarabadi MA et al (2013) Effects of zinc supplementation on the anthropometric measurements, lipid profiles and fasting blood glucose in the healthy obese adults. Adv Pharm Bull 3(1) [161–5 pp]. Available from: http://onlinelibrary.wiley.com/o/cochrane/clcentral/articles/706/CN-00908706/frame.html
Kim J, Lee S (2012) Effect of zinc supplementation on insulin resistance and metabolic risk factors in obese Korean women. Nutr Res Pract 6(3):221–225
Seet RC, Lee C-YJ, Lim EC, Quek AM, Huang H, Huang SH et al (2011) Oral zinc supplementation does not improve oxidative stress or vascular function in patients with type 2 diabetes with normal zinc levels. Atherosclerosis 219(1):231–239
do Nascimento Marreiro D, Geloneze B, Tambascia MA, Lerário AC, Halpern A, Cozzolino SMF (2006) Effect of zinc supplementation on serum leptin levels and insulin resistance of obese women. Biol Trace Elem Res 112(2):109–118
Ranasinghe P, Wathurapatha W, Ishara M, Jayawardana R, Galappatthy P, Katulanda P, Constantine GR (2015) Effects of zinc supplementation on serum lipids: a systematic review and meta-analysis. Nutr Metab 12(1):26
Foster M, Petocz P, Samman S (2010) Effects of zinc on plasma lipoprotein cholesterol concentrations in humans: a meta-analysis of randomised controlled trials. Atherosclerosis. 210(2):344–352
Jayawardena R, Ranasinghe P, Galappatthy P, Malkanthi R, Constantine G, Katulanda P (2012) Effects of zinc supplementation on diabetes mellitus: a systematic review and meta-analysis. Diabetol Metab Syndr 4(1):13
de Carvalho GB, Brandão-Lima PN, Maia CSC, Barbosa KBF, Pires LV (2017) Zinc’s role in the glycemic control of patients with type 2 diabetes: a systematic review. Biometals 30(2):151–162
Peykari N, Tehrani F, Eftekhari M, Malekafzali H, Dejman M, Neot R, Djalalinia S (2011) A peer-based study on adolescence nutritional health: a lesson learned from Iran. J Pak Med Assoc 61(6):549–554
Peykari N, Sepanlou S, Djalalinia S, Kasaeian A, Parsaeian M, Ahmadvand A, Koohpayehzadeh J, Damari B, Jamshidi HR, Larijani B, Farzadfar F (2014) National and sub-national prevalence, trend, and burden of metabolic risk factors (MRFs) in Iran: 1990-2013, study protocol. Arch Iran Med 17(1):54–61
Hovsepian S, Kelishadi R, Djalalinia S, Farzadfar F, Naderimagham S, Qorbani M (2015) Prevalence of dyslipidemia in Iranian children and adolescents: a systematic review. J Res Med Sci 20(5):503
Mohammadi Y, Parsaeian M, Farzadfar F, Kasaeian A, Mehdipour P, Sheidaei A et al (2014) Levels and trends of child and adult mortality rates in the Islamic Republic of Iran, 1990-2013; protocol of the NASBOD study. Arch Iran Med 17(3):176
Kelishadi R, Heshmat R, Farzadfar F, Motlag ME, Bahreynian M, Safiri S et al (2017) Prevalence of cardio-metabolic risk factors in a nationally representative sample of Iranian adolescents: the CASPIAN-III study. J Cardiovasc Thorac Res 9(1):12–20
Tabatabaei-Malazy O, Qorbani M, Samavat T, Sharifi F, Larijani B, Fakhrzadeh H (2014) Prevalence of dyslipidemia in Iran: a systematic review and meta-analysis study. Int J Prev Med 5(4):373–393
Azadbakht L, Kelishadi R, Khodarahmi M, Qorbani M, Heshmat R, Motlagh M et al (2013) The association of sleep duration and cardiometabolic risk factors in a national sample of children and adolescents: the CASPIAN III study. Nutrition (Burbank) 29(9):1133
Shafiee G, Kelishadi R, Qorbani M, Motlagh ME, Taheri M, Ardalan G, Taslimi M, Poursafa P, Heshmat R, Larijani B (2013) Association of breakfast intake with cardiometabolic risk factors. J Pediatr 89(6):575–582
Foroozanfard F, Jamilian M, Jafari Z, Khassaf A, Hosseini A, Khorammian H et al (2015) Effects of zinc supplementation on markers of insulin resistance and lipid profiles in women with polycystic ovary syndrome: a randomized, double-blind, placebo-controlled trial. Exp Clin Endocrinol Diabetes 123(4) [215–20 pp]. Available from: http://onlinelibrary.wiley.com/o/cochrane/clcentral/articles/372/CN-01070372/frame.html
Mahmoodianfard S, Vafa M, Golgiri F, Khoshniat M, Gohari M, Solati Z, Djalali M (2015) Effects of zinc and selenium supplementation on thyroid function in overweight and obese hypothyroid female patients: a randomized double-blind controlled trial. J Am Coll Nutr 34(5):391–399
Karamali M, Heidarzadeh Z, Seifati SM, Samimi M, Tabassi Z, Hajijafari M et al (2015) Zinc supplementation and the effects on metabolic status in gestational diabetes: a randomized, double-blind, placebo-controlled trial. J Diabetes Complicat 29(8) [1314–9 pp]. Available from: http://onlinelibrary.wiley.com/o/cochrane/clcentral/articles/653/CN-01125653/frame.html
Parham M, Amini M, Aminorroaya A, Heidarian E (2008) Effect of zinc supplementation on microalbuminuria in patients with type 2 diabetes: a double blind, randomized, placebo-controlled, cross-over trial. Rev Diabet Stud 5(2) [102–9 pp]. Available from: http://onlinelibrary.wiley.com/o/cochrane/clcentral/articles/971/CN-00754971/frame.html
Payahoo L, Ostadrahimi A, Mobasseri M, Bishak YK, Jafarabadi MA (2014) Effects of zinc supplementation on serum leptin level and insulin sensitivity in obese people. Trace Elem Electrolytes 31(1) [27–32 pp]. Available from: http://onlinelibrary.wiley.com/o/cochrane/clcentral/articles/284/CN-00979284/frame.html
Islam MR, Attia J, Ali L, McEvoy M, Selim S, Sibbritt D, Akhter A, Akter S, Peel R, Faruque O, Mona T, Lona H, Milton AH (2016) Zinc supplementation for improving glucose handling in pre-diabetes: a double blind randomized placebo controlled pilot study. Diabetes Res Clin Pract 115:39–46
Jamilian M, Foroozanfard F, Bahmani F, Talaee R, Monavari M, Asemi Z (2016) Effects of zinc supplementation on endocrine outcomes in women with polycystic ovary syndrome: a randomized, double-blind, placebo-controlled trial. Biol Trace Elem Res 170(2):271–278
Dias PCS, Sena-Evangelista KCM, de Oliveira Paiva MSM, Ferreira DQC, Ururahy MAG, Rezende AA et al (2014) The beneficial effects of rosuvastatin are independent of zinc supplementation in patients with atherosclerosis. J Trace Elem Med Biol 28(2):194–199
Foster M, Petocz P, Caterson ID, Samman S (2013) Effects of zinc and α-linolenic acid supplementation on glycemia and lipidemia in women with type 2 diabetes mellitus: a randomized, double-blind, placebo-controlled trial. J Diabetes Res Clin Metab 2(1):3
Al-Maroof RA, Al-Sharbatti SS (2006) Serum zinc levels in diabetic patients and effect of zinc supplementation on glycemic control of type 2 diabetics. Saudi Med J 27(3):344–350
Oh H-M, Yoon J-S (2008) Glycemic control of type 2 diabetic patients after short-term zinc supplementation. Nutr Res Pract 2(4):283–288
Koba S, Hirano T (2011) Dyslipidemia and atherosclerosis. Nihon Rinsho Jpn J Clin Med 69(1):138–143
Cunnane S, Yang J (1995) Zinc deficiency impairs whole body accumulation of polyunsaturates and increases the utilization of [1-14C] linoleate for de novo lipid synthesis in pregnant rats. Can J Physiol Pharmacol 73(9):1246–1252
DiSilvestro RA, Blostein-Fujii A (1997) Moderate zinc deficiency in rats enhances lipoprotein oxidation in vitro. Free Radic Biol Med 22(4):739–742
Gomez N, Ojeda M, Gimenez M (2002) Lung lipid composition in zinc-deficient rats. Lipids 37(3):291–296
Sun W, Yang J, Wang W, Hou J, Cheng Y, Fu Y et al (2017) The beneficial effects of Zn on Akt-mediated insulin and cell survival signaling pathways in diabetes. J Trace Elem Med Biol
Gomez NN, Biaggio VS, Rozzen EJ, Alvarez SM, Gimenez MS (2006) Zn-limited diet modifies the expression of the rate-regulatory enzymes involved in phosphatidylcholine and cholesterol synthesis. Br J Nutr 96(6):1038–1046
Feige JN, Gelman L, Michalik L, Desvergne B, Wahli W (2006) From molecular action to physiological outputs: peroxisome proliferator-activated receptors are nuclear receptors at the crossroads of key cellular functions. Prog Lipid Res 45(2):120–159
Zhao Y, Tan Y, Dai J, Wang B, Li B, Guo L, Cui J, Wang G, Li W, Cai L (2012) Zinc deficiency exacerbates diabetic down-regulation of Akt expression and function in the testis: essential roles of PTEN, PTP1B and TRB3. J Nutr Biochem 23(8):1018–1026
Murakami H, Yasui H, Yoshikawa Y (2012) Pharmacological and pharmacokinetic studies of anti-diabetic tropolonato–Zn (II) complexes with Zn (S2O2) coordination mode. Chem Pharm Bull 60(9):1096–1104
Nishide M, Yoshikawa Y, Yoshikawa EU, Matsumoto K, Sakurai H, Kajiwara NM (2008) Insulinomimetic Zn (II) complexes as evaluated by both glucose-uptake activity and inhibition of free fatty acids release in isolated rat adipocytes. Chem Pharm Bull 56(8):1181–1183
Capdor J, Foster M, Petocz P, Samman S (2013) Zinc and glycemic control: a meta-analysis of randomised placebo controlled supplementation trials in humans. J Trace Elem Med Biol 27(2):137–142
Group AC (2008) Intensive blood glucose control and vascular outcomes in patients with type 2 diabetes. N Engl J Med 358(24):2560–2572
Balkau B, Shipley M, Jarrett RJ, Pyörälä K, Pyörälä M, Forhan A et al (1998) High blood glucose concentration is a risk factor for mortality in middle-aged nondiabetic men: 20-year follow-up in the Whitehall Study, the Paris Prospective Study, and the Helsinki Policemen Study. Diabetes Care 21(3):360–367
Vardatsikos G, Pandey NR, Srivastava AK (2013) Insulino-mimetic and anti-diabetic effects of zinc. J Inorg Biochem 120:8–17
Yoshikawa Y, Ueda E, Miyake H, Sakurai H, Kojima Y (2001) Insulinomimetic bis (maltolato) zinc (II) complex: blood glucose normalizing effect in KK-Ay mice with type 2 diabetes mellitus. Biochem Biophys Res Commun 281(5):1190–1193
Adachi Y, Yoshida J, Kodera Y, Kiss T, Jakusch T, Enyedy EA, Yoshikawa Y, Sakurai H (2006) Oral administration of a zinc complex improves type 2 diabetes and metabolic syndromes. Biochem Biophys Res Commun 351(1):165–170
Ezaki O (1989) IIb group metal ions (Zn2+, Cd2+, Hg2+) stimulate glucose transport activity by post-insulin receptor kinase mechanism in rat adipocytes. J Biol Chem 264(27):16118–16122
Tang X-H, Shay NF (2001) Zinc has an insulin-like effect on glucose transport mediated by phosphoinositol-3-kinase and Akt in 3T3-L1 fibroblasts and adipocytes. J Nutr 131(5):1414–1420
Quarterman J, Mills C, Humphries W (1966) The reduced secretion of, and sensitivity to insulin in zinc-deficient rats. Biochem Biophys Res Commun 25(3):354–358
Huber AM, Gershoff SN (1973) Effect of zinc deficiency in rats on insulin release from the pancreas. J Nutr 103(12):1739–1744
Rungby J (2010) Zinc, zinc transporters and diabetes. Diabetologia. 53(8):1549–1551
Wijesekara N, Chimienti F, Wheeler M (2009) Zinc, a regulator of islet function and glucose homeostasis. Diabetes Obes Metab 11(s4):202–214
Myers SA (2015) Zinc transporters and zinc signaling: new insights into their role in type 2 diabetes. Int J Endocrinol 2015:1–7
Solomou A, Meur G, Bellomo E, Hodson DJ, Tomas A, Li SM et al (2015) The zinc transporter Slc30a8/ZnT8 is required in a subpopulation of pancreatic α-cells for hypoglycemia-induced glucagon secretion. J Biol Chem 290(35):21432–21442
Little PJ, Bhattacharya R, Moreyra AE, Korichneva IL (2010) Zinc and cardiovascular disease. Nutrition 26(11–12):1050–1057
Miao X, Sun W, Fu Y, Miao L, Cai L (2013) Zinc homeostasis in the metabolic syndrome and diabetes. Front Med 7(1):31–52
Tubek S (2007) Role of zinc in regulation of arterial blood pressure and in the etiopathogenesis of arterial hypertension. Biol Trace Elem Res 117(1–3):39–51
Tomat AL, Weisstaub AR, Jauregui A, Piñeiro A, Balaszczuk AM, Costa MA, Arranz CT (2005) Moderate zinc deficiency influences arterial blood pressure and vascular nitric oxide pathway in growing rats. Pediatr Res 58(4):672–676
Kunutsor SK, Laukkanen JA (2016) Serum zinc concentrations and incident hypertension: new findings from a population-based cohort study. J Hypertens 34(6):1055–1061
Singh RB, Niaz MA, Rastogi SS, Bajaj S, Gaoli Z, Shoumin Z (1998) Current zinc intake and risk of diabetes and coronary artery disease and factors associated with insulin resistance in rural and urban populations of North India. J Am Coll Nutr 17(6):564–570
Bergomi M, Rovesti S, Vinceti M, Vivoli R, Caselgrandi E, Vivoli G (1997) Zinc and copper status and blood pressure. J Trace Elem Med Biol 11(3):166–169
Pachotikarn C, Medeiros D, Windham F (1985) Effect of oral zinc supplementation upon plasma lipids, blood pressure, and other variables in young adult white males. Nutr Rep Int (USA)
Frithz G, Ronquist G (1979) Increased red cell content of Zn2+ in essential hypertension. J Intern Med 205(1–6):647–649
Davydenko N, Smirnova I, Kvasha E, Koblianskaia A (1995) Interrelationship between dietary intake of minerals and prevalence of hypertension. Vopr Pitan 6:17–19
Vezzoli G, Elli AA, Tripodi G, Bianchi G, Carafoli E (1985) Calcium ATPase in erythrocytes of spontaneously hypertensive rats of the Milan strain. J Hypertens 3(6):645–648
Vapaatalo H, Mervaala E, Nurminen M-L (2000) Role of endothelium and nitric oxide in experimental hypertension. Physiol Res 49(1):1–10
Klein S, Allison DB, Heymsfield SB, Kelley DE, Leibel RL, Nonas C et al (2007) Waist circumference and cardiometabolic risk: a consensus statement from shaping America’s health: Association for Weight Management and Obesity Prevention; NAASO, the Obesity Society; the American Society for Nutrition; and the American Diabetes Association. Obesity 15(5):1061–1067
Després J-P, Lemieux I, Bergeron J, Pibarot P, Mathieu P, Larose E et al (2008) Abdominal obesity and the metabolic syndrome: contribution to global cardiometabolic risk. Arterioscler Thromb Vasc Biol 28(6):1039–1049
Ennes Dourado Ferro F, de Sousa Lima V, Mello Soares N, Franciscato Cozzolino S, do Nascimento Marreiro D (2011) Biomarkers of metabolic syndrome and its relationship with the zinc nutritional status in obese women. Nutr Hosp 26(3)
Kelishadi R, Hashemipour M, Adeli K, Tavakoli N, Movahedian-Attar A, Shapouri J et al (2010) Effect of zinc supplementation on markers of insulin resistance, oxidative stress, and inflammation among prepubescent children with metabolic syndrome. Metab Syndr Relat Disord 8(6) [505–10 pp]. Available from: http://onlinelibrary.wiley.com/o/cochrane/clcentral/articles/374/CN-00781374/frame.html
Haase H, Maret W (2005) Protein tyrosine phosphatases as targets of the combined insulinomimetic effects of zinc and oxidants. Biometals 18(4):333–338
Acknowledgments
The authors are thankful to the Emam Ali Clinical Research Development Unit for the assistance.
Funding
This study was funded by Alborz University of Medical Sciences.
Author information
Authors and Affiliations
Contributions
MQ, MGH, MKH, and SD designed the research; SM and HA conducted the research; PT analyzed the data; MN, AA, and FS wrote the paper. All authors read and approved the final manuscript.
Corresponding author
Ethics declarations
The present study was approved by the ethical committee of Alborz University of Medical Sciences.
Competing Interests
The authors declare that they have no competing interests.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic Supplementary Material
ESM 1
(PDF 124 kb)
Appendix
Appendix
Rights and permissions
About this article
Cite this article
Khazdouz, M., Djalalinia, S., Sarrafi Zadeh, S. et al. Effects of Zinc Supplementation on Cardiometabolic Risk Factors: a Systematic Review and Meta-analysis of Randomized Controlled Trials. Biol Trace Elem Res 195, 373–398 (2020). https://doi.org/10.1007/s12011-019-01870-9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12011-019-01870-9