Abstract
Background
The incidence of infection by methicillin-resistant Staphylococcus aureus (MRSA) in total knee arthroplasty (TKA) is becoming a more frequent concern, as increased morbidity following TKA has been reported for infections by resistant organisms. This study investigates whether MRSA infections are associated with decreased functional scores.
Questions/purposes
We therefore compared the functional scores, operative times, and rates of reinfection of revision TKA following MRSA infection versus other indications for revision.
Methods
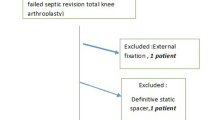
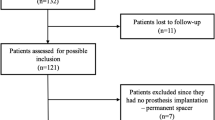
We retrospectively reviewed charts of 101 patients (103 knees) who underwent mobile bearing TKA revision from January 2003 to September 2006, with a minimum clinical followup of 2 years in 45 knees (44%). We obtained the following indices: WOMAC, Activities of Daily Living Score (ADLS), SF-36, and Knee Society scores (KSS). Three groups of revisions were compared: MRSA infection (n = 6), non-MRSA infection (n = 9), and aseptic failure (n = 30). The three groups were similar in demographics and comorbidities.
Results
The MRSA (166 minutes) and non-MRSA groups (149 minutes) had longer operative times than the aseptic group (121 minutes). With numbers available, there were no differences in ROM, WOMAC, ADLS, KSS, and SF-36, with MRSA separate or combined with all infections. Infection recurrence between MRSA-infected knees and non-MRSA-infected knees was similar.
Conclusions
While our study was underpowered to detect functional differences between MRSA-infected knees and non-MRSA-infected knees it does add data to the literature. Knees revised for infection have longer operative times and more frequent infection after revision. The reason for increased operative times is unclear.
Level of Evidence
Level III, therapeutic study. See the Guidelines for Authors for a complete description of levels of evidence.
Similar content being viewed by others
References
Al-Nammari SS, Bobak P, Venkatesh R. Methicillin resistant Staphylococcus aureus versus methicillin sensitive Staphylococcus aureus adult haematogenous septic arthritis. Arch Orthop Trauma Surg. 2007;127:537–542.
Barrack RL, Engh G, Rorabeck C, Sawhney J, Woolfrey W. Patient satisfaction and outcome measures after septic versus aseptic revision total knee arthroplasty. J Arthroplasty. 2000;15:990–993.
Classen DC, Evans RS, Pestotnik SL, Horn SD, Menlove RL, Burke JP. The timing of prophylactic administration of antibiotics and the risk of surgical-wound infection. N Engl J Med. 1992;326:281–286.
Deirmengian C, Greenbaum J, Lotke PA, Booth RE Jr, Lonner JH. Limited success with open débridement and retention of components in the treatment of acute Staphylococcus aureus infections after total knee arthroplasty. J Arthroplasty. 2003;18:22–26.
Engemann JJ, Carmeli Y, Cosgrove SE, Fowler VG, Bronstein MZ, Trivette SL, Briggs JP, Sexton DJ, Kaye KS. Adverse clinical and economic outcomes attributable to methicillin resistance among patients with Staphylococcus aureus surgical site infection. Clin Infect Dis. 2003;36:592–598.
Ghanem E, Restrepo C, Joshi A, Hozack W, Sharkey P, Parivizi J. Periprosthetic infection does not preclude good outcome for revision arthroplasty. Clin Orthop Relat Res. 2007;461:54–59.
Hartman MB, Fehring TK, Jordan L, Norton HJ. Periprosthetic knee sepsis. The role of irrigation and débridement. Clin Orthop Relat Res. 1991;273:113–118.
Hill C, Flamant R, Mazas F, Evrand J. Prophylactic cefazolin versus placebo in total hip replacement: report of a multicentre double-blind randomised trial. Lancet. 1981;1:795–796.
Hirakawa K, Stulberg BN, Wilde AH, Bauer TW, Secic M. Results of 2-stage reimplantation for infected total knee arthroplasty. J Arthroplasty. 1998;13:22–28.
Insall J, Thompson F, Brause B. Two-stage reimplantation for the salvage of infected total knee arthroplasty. J Bone Joint Surg Am. 1983;65:1087–1098.
Insall JN, Dorr LD, Scott RD, Scott N. Rationale of the Knee Society clinical rating system. Clin Orthop Relat Res. 1989;248:13–14.
Ip D, Yam SK, Chen CK. Implications of the changing pattern of bacterial infections following total joint replacement. J Orthop Surg (Hong Kong). 2005;13:125–130.
Irrgang JJ, Snyder-Mackler L, Wainner RS, Fu FH, Harner CD. Development of a patient-reported measure of function of the knee. J Bone Joint Surg Am. 1998; 80:1132–1145.
Kilgus DJ, Howe DJ, Strang A. Results of periprosthetic hip and knee infections caused by resistant bacteria. Clin Orthop Relat Res. 2002;404:116–124.
Leigh DA, Griggs J, Tighe CM, Powell HD, Church JC, Wise K, Channon G, Curtis LB. Pharmacokinetic study of ceftazidime in bone and serum of patients undergoing hip and knee arthroplasty. J Antimicrob Chemother. 1985;16:637–642.
Mittal Y, Fehring TK, Hanssen A, Marculescu C, Odum SM, Osmon D. Two-stage reimplantation for periprosthetic knee infection involving resistant organisms. J Bone Joint Surg Am. 2007;89:1227–1231.
Morrey B, Westholm F, Schoifet S, Rand J, Bryan R. Long-term results of various treatment options for infected total knee arthroplasty. Clin Orthop Relat Res. 1989;248:120–128.
Nixon M, Jackson B, Varghese P, Jenkins D, Taylor G. Methicillin-resistant Staphylococcus aureus on orthopaedic wards: incidence, spread, mortality, cost and control. J Bone Joint Surg Br. 2006;88:812–817.
Papagelopoulos PJ, Idusuyi OB, Wallrichs SL, Morrey BF. Long term outcome and survivorship analysis of primary total knee arthroplasty in patients with diabetes mellitus. Clin Orthop Relat Res. 1996;330:124–132.
Parvizi J, Assam K, Ghanem E, Austin MS, Rothman RH. Periprosthetic infection due to resistant staphylococci: serious problems on the horizon. Clin Orthop Relat Res. 2009;467:1732–1739.
Parvizi J, Sullivan TA, Pagnano MW, Trousdale RT, Bolander ME. Total joint arthroplasty in human immunodeficiency virus-positive patients: an alarming rate of early failure. J Arthroplasty. 2003;18:259–264.
Patel A, Calfee RP, Plante M, Fischer SA, Arcand N, Born C. Methicillin-resistant Staphylococcus aureus in orthopaedic surgery. J Bone Joint Surg Br. 2008;90:1401–1406.
Patel R, Osmon DR, Hanssen AD. The Diagnosis of Prosthetic Joint Infection. Current Techniques and Emerging Technologies. Clin Orthop Relat Res. 2005;437:55–58.
Peersman G, Laskin R, Davis J, Peterson M. Infection in total knee replacement. A retrospective review of 6489 total knee replacements. Clin Orthop Relat Res. 2001;392:15–23.
Raj D, Iyer S, Fergusson CM. Methicillin-resistant Staphylococcus aureus infection following arthroscopy of the knee joint. Ann R Coll Surg Engl. 2006;88:675–676.
Salgado CD, Dash S, Cantey JR, Marculescu CE. Higher risk of failure of methicillin resistant Staphylococcus aureus prosthetic joint infections. Clin Orthop Relat Res. 2007;461:48–53.
Sankar B, Hopgood P, Bell KM. The role of MRSA screening in joint-replacement surgery. International Orthopaedics (SICOT). 2005;29:160–163.
Silva M, Tharani R, Schmalzried TP. Results of direct exchange or débridement of the infected total knee arthroplasty. Clin Orthop Relat Res. 2002;404:125–131.
Tannenbaum DA, Matthews LS, Grady-Benson JC. Infection around joint replacements in patients who have a renal or liver transplantation. J Bone Joint Surg Am. 1997;79:36–43.
Volin SJ, Hinrichs SH, Garvin KL. Two-stage reimplantation of total joint infections: a comparison of resistant and non-resistant organisms. Clin Orthop Relat Res. 2004;427:94–100.
Wang CJ, Huang TW, Wang JW, Chen HS. The often poor clinical outcome of infected total knee arthroplasty. J Arthroplasty. 2002;17:608–614.
Ware JR Jr, Sherbourne CD. The MOS 36-item Short-Form health survey (SF-36): I. Conceptual framework and item selection. Med Care. 1992;30:473–483.
Winiarsky R, Barth P, Lotke P. Total knee arthroplasty in morbidly obese patients. J Bone Joint Surg Am. 1998;80:1770–1774.
Zimmerli W. Prosthetic-joint-associated infection. Best Prac Res Clin Rheumatol. 2006;20:1045–1063.
Acknowledgments
We thank Dr. Brian Klatt and Dr. Lawrence Crossett for their contributions to this project.
Author information
Authors and Affiliations
Corresponding author
Additional information
One of the authors (RLM) has received research funding from DePuy that was not related to this work. The institution of the authors (BAK, AH, NR, RLM) has received funding from DePuy.
Each author certifies that his or her institution approved the human protocol for this investigation, that all investigations were conducted in conformity with ethical principles of research; our ethical board did not require informed consent for participation in the chart review portion of this study. Informed consent for participation in the study was obtained for those patients participating in the clinic visit portion of the study.
This work was performed in the Divisions of Adult Reconstruction and Musculoskeletal Oncology, University of Pittsburgh School of Medicine, Pittsburgh, PA, USA.
About this article
Cite this article
Laudermilch, D.J., Fedorka, C.J., Heyl, A. et al. Outcomes of Revision Total Knee Arthroplasty After Methicillin-resistant Staphylococcus aureus Infection. Clin Orthop Relat Res 468, 2067–2073 (2010). https://doi.org/10.1007/s11999-010-1304-x
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11999-010-1304-x