Abstract
Purpose of review
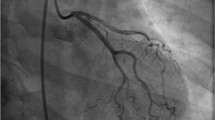
Spontaneous coronary artery dissection (SCAD) is a non-iatrogenic and non-traumatic separation of the coronary arterial wall. While SCAD represents an important cause of myocardial infarction, optimal diagnostic and therapeutic options remain challenging. We sought to review recent studies and provide an update on diagnosis and management of SCAD.
Recent findings
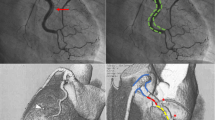
Coronary angiography is the first-line diagnostic modality for SCAD, with three angiographic features commonly observed in SCAD: type 1 (pathognomonic angiographic appearance with contrast staining of the arterial wall), type 2 (long coronary stenosis), and type 3 (focal tubular stenosis). In addition, adjunctive intracoronary imaging can aid in identifying coronary dissections. Conservative management with beta-blockers and aspirin remains the mainstay of therapy. However, patients with high-risk features and recurrent symptoms may require revascularization. Several techniques have been reported, such as long stents to seal the entire length of the dissection, stepwise stenting starting at the distal edge followed by proximal edge stenting, use of bioabsorbable stents, and cutting balloon angioplasty. Furthermore, cardiac rehabilitation appears to be safe and offers significant benefits for patients with SCAD.
Summary
Coronary angiographic classification contributed to the increased recognition of SCAD in recent years. Selecting the most suitable and appropriate therapy based on accurate diagnosis is the cornerstone of management in SCAD. Further studies are needed to establish optimal treatment of SCAD depending on anatomical and/or clinical features.

Similar content being viewed by others
References and Recommended Reading
Papers of particular interest, published recently, have been highlighted as: • Of importance •• Of major importance
Elkayam U, Jalnapurkar S, Barakkat MN, Khatri N, Kealey AJ, Mehra A, et al. Pregnancy-associated acute myocardial infarction: a review of contemporary experience in 150 cases between 2006 and 2011. Circulation. 2014;129(16):1695–702. https://doi.org/10.1161/circulationaha.113.002054.
Maehara A, Mintz GS, Castagna MT, Pichard AD, Satler LF, Waksman R, et al. Intravascular ultrasound assessment of spontaneous coronary artery dissection. Am J Cardiol. 2002;89(4):466–8.
Saw J, Ricci D, Starovoytov A, Fox R, Buller CE. Spontaneous coronary artery dissection: prevalence of predisposing conditions including fibromuscular dysplasia in a tertiary center cohort. JACC Cardiovasc Interv. 2013;6(1):44–52. https://doi.org/10.1016/j.jcin.2012.08.017.
Saw J, Aymong E, Sedlak T, Buller CE, Starovoytov A, Ricci D, et al. Spontaneous coronary artery dissection: association with predisposing arteriopathies and precipitating stressors and cardiovascular outcomes. Circ Cardiovasc Interv. 2014;7(5):645–55. https://doi.org/10.1161/circinterventions.114.001760.
Prasad M, Tweet MS, Hayes SN, Leng S, Liang JJ, Eleid MF, et al. Prevalence of extracoronary vascular abnormalities and fibromuscular dysplasia in patients with spontaneous coronary artery dissection. Am J Cardiol. 2015;115(12):1672–7. https://doi.org/10.1016/j.amjcard.2015.03.011.
Tweet MS, Hayes SN, Pitta SR, Simari RD, Lerman A, Lennon RJ, et al. Clinical features, management, and prognosis of spontaneous coronary artery dissection. Circulation. 2012;126(5):579–88. https://doi.org/10.1161/circulationaha.112.105718.
Luong C, Starovoytov A, Heydari M, Sedlak T, Aymong E, Saw J. Clinical presentation of patients with spontaneous coronary artery dissection. Catheter Cardiovasc Interv. 2017;89(7):1149–54. https://doi.org/10.1002/ccd.26977.
Tweet MS, Eleid MF, Best PJ, Lennon RJ, Lerman A, Rihal CS, et al. Spontaneous coronary artery dissection: revascularization versus conservative therapy. Circ Cardiovasc Interv. 2014;7(6):777–86. https://doi.org/10.1161/circinterventions.114.001659.
• Tweet MS, Hayes SN, Codsi E, Gulati R, Rose CH, Best PJM. Spontaneous coronary artery dissection associated with pregnancy. J Am Coll Cardiol. 2017;70(4):426–35. https://doi.org/10.1016/j.jacc.2017.05.055. This prospective observational study provides important information about the unique clinical presentation of pregnancy-associated SCAD.
Havakuk O, Goland S, Mehra A, Elkayam U. Pregnancy and the risk of spontaneous coronary artery dissection: an analysis of 120 contemporary cases. Circ Cardiovasc Interv. 2017;10(3). doi: 10.1161/circinterventions.117.004941.
Saw J. Coronary angiogram classification of spontaneous coronary artery dissection. Catheter Cardiovasc Interv. 2014;84(7):1115–22. https://doi.org/10.1002/ccd.25293.
Eleid MF, Guddeti RR, Tweet MS, Lerman A, Singh M, Best PJ, et al. Coronary artery tortuosity in spontaneous coronary artery dissection: angiographic characteristics and clinical implications. Circ Cardiovasc Interv. 2014;7(5):656–62. https://doi.org/10.1161/circinterventions.114.001676.
•• Saw J, Humphries K, Aymong E, Sedlak T, Prakash R, Starovoytov A, et al. Spontaneous Coronary Artery Dissection: Clinical Outcomes and Risk of Recurrence. J Am Coll Cardiol. 2017;70(9):1148–58. https://doi.org/10.1016/j.jacc.2017.06.053. This study of the prospectively followed largest cohort with SCAD provides insights on long-term clinical outcomes of SCAD. This series confirms the appropriateness of conservative medical management for clinically stable patients. Also, the finding of beta-blocker associated with reduced risk of recurrent SCAD is novel and directs future research.
Gornik HL. Spontaneous coronary artery dissection: the zebra has been spotted: now let’s study its stripes. J Am Coll Cardiol. 2017;70(4):436–8. https://doi.org/10.1016/j.jacc.2017.06.019.
Saw J, Mancini GB, Humphries K, Fung A, Boone R, Starovoytov A, et al. Angiographic appearance of spontaneous coronary artery dissection with intramural hematoma proven on intracoronary imaging. Catheter Cardiovasc Interv. 2016;87(2):E54–61. https://doi.org/10.1002/ccd.26022.
Paulo M, Sandoval J, Lennie V, Dutary J, Medina M, Gonzalo N, et al. Combined use of OCT and IVUS in spontaneous coronary artery dissection. JACC Cardiovasc Imaging. 2013;6(7):830–2. https://doi.org/10.1016/j.jcmg.2013.02.010.
Poon K, Bell B, Raffel OC, Walters DL, Jang IK. Spontaneous coronary artery dissection: utility of intravascular ultrasound and optical coherence tomography during percutaneous coronary intervention. Circ Cardiovasc Interv. 2011;4(2):e5–7. https://doi.org/10.1161/circinterventions.110.959593.
Ong DS, Jang IK. Fundamentals of optical coherence tomography: image acquisition and interpretation. Interv Cardiol Clin. 2015;4(3):225–37. https://doi.org/10.1016/j.iccl.2015.02.001.
Alfonso F, Paulo M, Gonzalo N, Dutary J, Jimenez-Quevedo P, Lennie V, et al. Diagnosis of spontaneous coronary artery dissection by optical coherence tomography. J Am Coll Cardiol. 2012;59(12):1073–9. https://doi.org/10.1016/j.jacc.2011.08.082.
Franco C, Eng L, Saw J. Optical coherence tomography in the diagnosis and management of spontaneous coronary artery dissection. Interv Cardiol Clin. 2015;4(3):309–20. https://doi.org/10.1016/j.iccl.2015.02.007.
Lowe HC, Narula J, Fujimoto JG, Jang IK. Intracoronary optical diagnostics current status, limitations, and potential. JACC Cardiovasc Interv. 2011;4(12):1257–70. https://doi.org/10.1016/j.jcin.2011.08.015.
Jang IK, Bouma BE, Kang DH, Park SJ, Park SW, Seung KB, et al. Visualization of coronary atherosclerotic plaques in patients using optical coherence tomography: comparison with intravascular ultrasound. J Am Coll Cardiol. 2002;39(4):604–9.
Prakash R, Starovoytov A, Heydari M, Mancini GB, Saw J. Catheter-induced iatrogenic coronary artery dissection in patients with spontaneous coronary artery dissection. JACC Cardiovasc Interv. 2016;9(17):1851–3. https://doi.org/10.1016/j.jcin.2016.06.026.
Russo V, Marrozzini C, Zompatori M. Spontaneous coronary artery dissection: role of coronary CT angiography. Heart. 2013;99(9):672–3. https://doi.org/10.1136/heartjnl-2012-303215.
Torres-Ayala SC, Maldonado J, Bolton JS, Bhalla S. Coronary computed tomography angiography of spontaneous coronary artery dissection: a case report and review of the literature. Am J Case Rep. 2015;16:130–5. https://doi.org/10.12659/ajcr.892805.
Eleid MF, Tweet MS, Young PM, Williamson E, Hayes SN, Gulati R. Spontaneous coronary artery dissection: challenges of coronary computed tomography angiography. Eur Heart J Acute Cardiovasc Care 2017:2048872616687098. doi:https://doi.org/10.1177/2048872616687098.
Roura G, Ariza-Sole A, Rodriguez-Caballero IF, Gomez-Lara J, Ferreiro JL, Romaguera R, et al. Noninvasive follow-up of patients with spontaneous coronary artery dissection with CT angiography. JACC Cardiovasc Imaging. 2016;9(7):896–7. https://doi.org/10.1016/j.jcmg.2015.06.011.
Hiratzka LF, Bakris GL, Beckman JA, Bersin RM, Carr VF, Casey DE Jr, et al. 2010 ACCF/AHA/AATS/ACR/ASA/SCA/SCAI/SIR/STS/SVM guidelines for the diagnosis and management of patients with thoracic aortic disease: executive summary: a report of the American College of Cardiology Foundation/American Heart Association Task Force on Practice Guidelines, American Association for Thoracic Surgery, American College of Radiology, American Stroke Association, Society of Cardiovascular Anesthesiologists, Society for Cardiovascular Angiography and Interventions, Society of Interventional Radiology, Society of Thoracic Surgeons, and Society for Vascular Medicine. Anesth Analg. 2010;111(2):279–315. https://doi.org/10.1213/ANE.0b013e3181dd869b.
Nienaber CA, Powell JT. Management of acute aortic syndromes. Eur Heart J. 2012;33(1):26–35b. https://doi.org/10.1093/eurheartj/ehr186.
Ryden L, Ariniego R, Arnman K, Herlitz J, Hjalmarson A, Holmberg S, et al. A double-blind trial of metoprolol in acute myocardial infarction. Effects on ventricular tachyarrhythmias. N Engl J Med. 1983;308(11):614–8. https://doi.org/10.1056/nejm198303173081102.
Roberts R, Rogers WJ, Mueller HS, Lambrew CT, Diver DJ, Smith HC, et al. Immediate versus deferred beta-blockade following thrombolytic therapy in patients with acute myocardial infarction. Results of the Thrombolysis in Myocardial Infarction (TIMI) II-B study. Circulation. 1991;83(2):422–37.
Amsterdam EA, Wenger NK, Brindis RG, Casey DE Jr, Ganiats TG, Holmes DR Jr, et al. 2014 AHA/ACC guideline for the management of patients with non-ST-elevation acute coronary syndromes: executive summary: a report of the American College of Cardiology/American Heart Association Task Force on Practice Guidelines. Circulation. 2014;130(25):2354–94. https://doi.org/10.1161/cir.0000000000000133.
Rogowski S, Maeder MT, Weilenmann D, Haager PK, Ammann P, Rohner F, et al. Spontaneous coronary artery dissection: angiographic follow-up and long-term clinical outcome in a predominantly medically treated population. Catheter Cardiovasc Interv. 2017;89(1):59–68. https://doi.org/10.1002/ccd.26383.
Lettieri C, Zavalloni D, Rossini R, Morici N, Ettori F, Leonzi O, et al. Management and long-term prognosis of spontaneous coronary artery dissection. Am J Cardiol. 2015;116(1):66–73. https://doi.org/10.1016/j.amjcard.2015.03.039.
O'Gara PT, Kushner FG, Ascheim DD, Casey DE Jr, Chung MK, de Lemos JA, et al. 2013 ACCF/AHA guideline for the management of ST-elevation myocardial infarction: a report of the American College of Cardiology Foundation/American Heart Association Task Force on Practice Guidelines. Circulation. 2013;127(4):e362–425. https://doi.org/10.1161/CIR.0b013e3182742cf6.
Leclercq F, Messner-Pellenc P, Carabasse D, Lucke N, Rivalland F, Grolleau R. Successful thrombolysis treatment of a spontaneous left main coronary artery dissection without subsequent surgery. Eur Heart J. 1996;17(2):320–1.
Zupan I, Noc M, Trinkaus D, Popovic M. Double vessel extension of spontaneous left main coronary artery dissection in young women treated with thrombolytics. Catheter Cardiovasc Interv. 2001;52(2):226–30.
Shamloo BK, Chintala RS, Nasur A, Ghazvini M, Shariat P, Diggs JA, et al. Spontaneous coronary artery dissection: aggressive vs. conservative therapy. J Invasive Cardiol. 2010;22(5):222–8.
Diez-Delhoyo F, Sanz-Ruiz R, Sarnago-Cebada F, Gutierrez-Ibanes E, Rivera-Juarez A, Elizaga J, et al. Spontaneous coronary artery dissection: failure of the conservative strategy due to predominance of the false lumen. JACC Cardiovasc Interv. 2017;10(15):e139–e40. https://doi.org/10.1016/j.jcin.2017.04.032.
Lempereur M, Fung A, Saw J. Stent mal-apposition with resorption of intramural hematoma with spontaneous coronary artery dissection. Cardiovasc Diagn Ther. 2015;5(4):323–9. https://doi.org/10.3978/j.issn.2223-3652.2015.04.05.
Macaya F, Peral V, Alameda M, Pascual M, Gomez-Jaume A, Asmarats L, et al. Bioresorbable scaffolds to treat spontaneous coronary artery dissection. Circ Cardiovasc Interv. 2016;9(1):e003133.
Watt J, Egred M, Khurana A, Bagnall AJ, Zaman AG. 1-year follow-up optical frequency domain imaging of multiple bioresorbable vascular scaffolds for the treatment of spontaneous coronary artery dissection. JACC Cardiovasc Interv. 2016;9(4):389–91. https://doi.org/10.1016/j.jcin.2015.11.030.
Cockburn J, Yan W, Bhindi R, Hansen P. Spontaneous coronary artery dissection treated with bioresorbable vascular scaffolds guided by optical coherence tomography. Can J Cardiol. 2014;30(11):1461.e1–3. https://doi.org/10.1016/j.cjca.2014.06.025.
Serruys PW, Chevalier B, Sotomi Y, Cequier A, Carrie D, Piek JJ, et al. Comparison of an everolimus-eluting bioresorbable scaffold with an everolimus-eluting metallic stent for the treatment of coronary artery stenosis (ABSORB II): a 3 year, randomised, controlled, single-blind, multicentre clinical trial. Lancet (London, England). 2016;388(10059):2479–91. https://doi.org/10.1016/s0140-6736(16)32050-5.
Kereiakes DJ, Ellis SG, Metzger C, Caputo RP, Rizik DG, Teirstein PS, et al. 3-year clinical outcomes with everolimus-eluting bioresorbable coronary scaffolds: the ABSORB III trial. J Am Coll Cardiol. 2017;70:2852–62. https://doi.org/10.1016/j.jacc.2017.10.010.
Abbott. Absorb GT1 bioresorbable vascular scaffold. Abbott. https://www.vascular.abbott/us/products/coronary-intervention/absorb-bioresorbable-scaffold-dissolving-stent.html. Accessed November 15 2017.
Quadri G, Tomassini F, Cerrato E, Varbella F. First reported case of magnesium-made bioresorbable scaffold to treat spontaneous left anterior descending coronary artery dissection. Catheter Cardiovasc Interv. 2017;90(5):768–72. https://doi.org/10.1002/ccd.27214.
Haude M, Ince H, Kische S, Abizaid A, Tolg R, Alves Lemos P, et al. Sustained safety and clinical performance of a drug-eluting absorbable metal scaffold up to 24 months: pooled outcomes of BIOSOLVE-II and BIOSOLVE-III. EuroInterv: J EuroPCR Collab Working Group Interv Cardiol Eur Soc Cardiol. 2017;13(4):432–9. https://doi.org/10.4244/eij-d-17-00254.
Yumoto K, Sasaki H, Aoki H, Kato K. Successful treatment of spontaneous coronary artery dissection with cutting balloon angioplasty as evaluated with optical coherence tomography. JACC Cardiovasc Interv. 2014;7(7):817–9. https://doi.org/10.1016/j.jcin.2013.10.027.
Motreff P, Barber-Chamoux N, Combaret N, Souteyrand G. Coronary artery fenestration guided by optical coherence tomograhy before stenting: new interventional option in rescue management of compressive spontaneous intramural hematoma. Circ Cardiovasc Interv. 2015;8(4):e002266. https://doi.org/10.1161/circinterventions.114.002266.
Alkhouli M, Cole M, Ling FS. Coronary artery fenestration prior to stenting in spontaneous coronary artery dissection. Catheter Cardiovasc Interv. 2016;88(1):E23–7. https://doi.org/10.1002/ccd.26161.
Ito T, Shintani Y, Ichihashi T, Fujita H, Ohte N. Non-atherosclerotic spontaneous coronary artery dissection revascularized by intravascular ultrasonography-guided fenestration with cutting balloon angioplasty. Cardiovasc Interv Ther. 2017;32(3):241–3. https://doi.org/10.1007/s12928-016-0397-x.
Krittanawong C, Tweet MS, Hayes SE, Bowman MJ, Gulati R, Squires RW, et al. Usefulness of cardiac rehabilitation after spontaneous coronary artery dissection. Am J Cardiol. 2016;117(10):1604–9. https://doi.org/10.1016/j.amjcard.2016.02.034.
Chou AY, Prakash R, Rajala J, Birnie T, Isserow S, Taylor CM, et al. The first dedicated cardiac rehabilitation program for patients with spontaneous coronary artery dissection: description and initial results. Can J Cardiol. 2016;32(4):554–60. https://doi.org/10.1016/j.cjca.2016.01.009.
Acknowledgements
We thank Amy Zhong, MA for her medical illustration of this article.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of Interest
Ilhwan Yeo and Luke K. Kim each declare no potential conflicts of interest.
Dmitriy N. Feldman is a section editor for Current Treatment Options in Cardiovascular Medicine.
Human and Animal Rights and Informed Consent
This article does not contain any studies with human or animal subjects performed by any of the authors.
Additional information
This article is part of the Topical Collection on Coronary Artery Disease
Rights and permissions
About this article
Cite this article
Yeo, I., Feldman, D.N. & Kim, L.K. Spontaneous Coronary Artery Dissection: Diagnosis and Management. Curr Treat Options Cardio Med 20, 27 (2018). https://doi.org/10.1007/s11936-018-0622-2
Published:
DOI: https://doi.org/10.1007/s11936-018-0622-2