Opinion statement
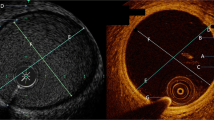
The use of intracoronary imaging modalities has seen a significant increase over the past decade, as both imaging quality and delivery systems have improved. Generally accepted best practice indications for using intracoronary imaging include assessment of lesion characteristics prior to stent placement, optimization of stent placement with respect to appropriate sizing, adequate apposition, and expansion and exclusion of edge dissection. Intracoronary imaging plays a particular role in the setting of contemporary left main and bifurcation stenting. Stent interrogation using intracoronary imaging to exclude mechanical causes in the management of in-stent thrombosis has also become conventional. Current clinical guideline recommendations, however, have lagged behind contemporary practice patterns and the use of intravascular ultrasound only carries a class IIa recommendation in the appropriate clinical setting. We discuss the currently available intracoronary imaging modalities and their applications, including intravascular ultrasound (IVUS) and optical coherence tomography (OCT), and review the data supporting their use.

Similar content being viewed by others
References and Recommended Reading
Papers of particular interest, published recently, have been highlighted as:• Of importance
Bom N, Lancee CT, Van Egmond FC. An ultrasonic intracardiac scanner. Ultrasonics. 1972;10(2):72–6.
Yock PG, Linker DT, Angelsen BA. Two-dimensional intravascular ultrasound: technical development and initial clinical experience. J Am Soc Echocardiogr. 1989;2(4):296–304.
Mintz GS, Nissen SE, Anderson WD, Bailey SR, Erbel R, Fitzgerald PJ, et al. American College of Cardiology clinical expert consensus document on standards for acquisition, measurement and reporting of intravascular ultrasound studies (ivus): A report of the american college of cardiology task force on clinical expert consensus documents developed in collaboration with the european society of cardiology endorsed by the society of cardiac angiography and interventions. J Am Coll Cardiol. 2001;37(5):1478–92. doi:10.1016/S0735-1097(01)01175-5.
Nair A, Kuban BD, Tuzcu EM, Schoenhagen P, Nissen SE, Vince DG. Coronary plaque classification with intravascular ultrasound radiofrequency data analysis. Circulation. 2002;106(17):2200–6.
Nair A, Margolis MP, Kuban BD, Vince DG. Automated coronary plaque characterisation with intravascular ultrasound backscatter: ex vivo validation. EuroIntervention : J EuroPCR Collab Work Group Interv Cardiol Eur Soc Cardiol. 2007;3(1):113–20.
Huang D, Swanson EA, Lin CP, Schuman JS, Stinson WG, Chang W, et al. Optical coherence tomography. Science. 1991;254(5035):1178–81.
Mogensen M, Jorgensen TM, Thrane L, Nurnberg BM, Jemec GB. Improved quality of optical coherence tomography imaging of basal cell carcinomas using speckle reduction. Exp Dermatol. 2010;19(8):e293–5. doi:10.1111/j.1600-0625.2009.00979.x.
Chen Y, Aguirre AD, Hsiung PL, Desai S, Herz PR, Pedrosa M, et al. Ultrahigh resolution optical coherence tomography of Barrett's esophagus: preliminary descriptive clinical study correlating images with histology. Endoscopy. 2007;39(7):599–605. doi:10.1055/s-2007-966648.
Tearney GJ, Waxman S, Shishkov M, Vakoc BJ, Suter MJ, Freilich MI, et al. Three-dimensional coronary artery microscopy by intracoronary optical frequency domain imaging. JACC Cardiovasc Imaging. 2008;1(6):752–61. doi:10.1016/j.jcmg.2008.06.007.
Brezinski ME, Tearney GJ, Bouma BE, Izatt JA, Hee MR, Swanson EA, et al. Optical coherence tomography for optical biopsy. Properties and demonstration of vascular pathology. Circulation. 1996;93(6):1206–13.
Barlis P, Schmitt JM. Current and future developments in intracoronary optical coherence tomography imaging. EuroIntervention : J EuroPCR Collab Work Group Int Cardiol Eur Soc Cardiol. 2009;4(4):529–33.
Prati F, Regar E, Mintz GS, Arbustini E, Di Mario C, Jang IK, et al. Expert review document on methodology, terminology, and clinical applications of optical coherence tomography: physical principles, methodology of image acquisition, and clinical application for assessment of coronary arteries and atherosclerosis. Eur Heart J. 2010;31(4):401–15. doi:10.1093/eurheartj/ehp433.
Kawase Y, Hoshino K, Yoneyama R, McGregor J, Hajjar RJ, Jang IK, et al. In vivo volumetric analysis of coronary stent using optical coherence tomography with a novel balloon occlusion-flushing catheter: a comparison with intravascular ultrasound. Ultrasound Med Biol. 2005;31(10):1343–9. doi:10.1016/j.ultrasmedbio.2005.05.010.
White CW, Wright CB, Doty DB, Hiratza LF, Eastham CL, Harrison DG, et al. Does visual interpretation of the coronary arteriogram predict the physiologic importance of a coronary stenosis? New Engl J Med. 1984;310(13):819–24. doi:10.1056/NEJM198403293101304.
Tobis J, Azarbal B, Slavin L. Assessment of intermediate severity coronary lesions in the catheterization laboratory. J Am Coll Cardiol. 2007;49(8):839–48. doi:10.1016/j.jacc.2006.10.055.
Jensen LO, Thayssen P, Mintz GS, Egede R, Maeng M, Junker A, et al. Comparison of intravascular ultrasound and angiographic assessment of coronary reference segment size in patients with type 2 diabetes mellitus. Am J Cardiol. 2008;101(5):590–5. doi:10.1016/j.amjcard.2007.10.020.
Nishioka T, Amanullah AM, Luo H, Berglund H, Kim CJ, Nagai T, et al. Clinical validation of intravascular ultrasound imaging for assessment of coronary stenosis severity: comparison with stress myocardial perfusion imaging. J Am Coll Cardiol. 1999;33(7):1870–8.
Abizaid A, Mintz GS, Pichard AD, Kent KM, Satler LF, Walsh CL, et al. Clinical, intravascular ultrasound, and quantitative angiographic determinants of the coronary flow reserve before and after percutaneous transluminal coronary angioplasty. Am J Cardiol. 1998;82(4):423–8.
Briguori C, Anzuini A, Airoldi F, Gimelli G, Nishida T, Adamian M, et al. Intravascular ultrasound criteria for the assessment of the functional significance of intermediate coronary artery stenoses and comparison with fractional flow reserve. Am J Cardiol. 2001;87(2):136–41.
Waksman R, Legutko J, Singh J, Orlando Q, Marso S, Schloss T, et al. FIRST: Fractional Flow Reserve and Intravascular Ultrasound Relationship Study. J Am Coll Cardiol. 2013;61(9):917–23. doi:10.1016/j.jacc.2012.12.012. This was the first prospective study to assess the correlation between IVUS-derived MLA and FFR. VH-IVS was also compared to FFR to determine lesion characteristics that affect FFR results.
Leesar MA, Masden R, Jasti V. Physiological and intravascular ultrasound assessment of an ambiguous left main coronary artery stenosis. Cathet Cardiovasc Interv. 2004;62(3):349–57. doi:10.1002/ccd.20038.
Jasti V, Ivan E, Yalamanchili V, Wongpraparut N, Leesar MA. Correlations between fractional flow reserve and intravascular ultrasound in patients with an ambiguous left main coronary artery stenosis. Circulation. 2004;110(18):2831–6. doi:10.1161/01.CIR.0000146338.62813.E7.
de la Torre Hernandez JM, Hernandez Hernandez F, Alfonso F, Rumoroso JR, Lopez-Palop R, Sadaba M, et al. Prospective application of pre-defined intravascular ultrasound criteria for assessment of intermediate left main coronary artery lesions results from the multicenter LITRO study. J Am Coll Cardiol. 2011;58(4):351–8. doi:10.1016/j.jacc.2011.02.064.
Fassa AA, Wagatsuma K, Higano ST, Mathew V, Barsness GW, Lennon RJ, et al. Intravascular ultrasound-guided treatment for angiographically indeterminate left main coronary artery disease: a long-term follow-up study. J Am Coll Cardiol. 2005;45(2):204–11. doi:10.1016/j.jacc.2004.09.066.
Dodge Jr JT, Brown BG, Bolson EL, Dodge HT. Lumen diameter of normal human coronary arteries. Influence of age, sex, anatomic variation, and left ventricular hypertrophy or dilation. Circulation. 1992;86(1):232–46.
Ambrose JA, Tannenbaum MA, Alexopoulos D, Hjemdahl-Monsen CE, Leavy J, Weiss M, et al. Angiographic progression of coronary artery disease and the development of myocardial infarction. J Am Coll Cardiol. 1988;12(1):56–62.
Glaser R, Selzer F, Faxon DP, Laskey WK, Cohen HA, Slater J, et al. Clinical progression of incidental, asymptomatic lesions discovered during culprit vessel coronary intervention. Circulation. 2005;111(2):143–9. doi:10.1161/01.CIR.0000150335.01285.12.
Virmani R, Kolodgie FD, Burke AP, Farb A, Schwartz SM. Lessons from sudden coronary death: a comprehensive morphological classification scheme for atherosclerotic lesions. Arterioscler, Thromb, and Vasc Biol. 2000;20(5):1262–75.
Cheruvu PK, Finn AV, Gardner C, Caplan J, Goldstein J, Stone GW, et al. Frequency and distribution of thin-cap fibroatheroma and ruptured plaques in human coronary arteries: a pathologic study. J Am Coll Cardiol. 2007;50(10):940–9. doi:10.1016/j.jacc.2007.04.086.
Finn AV, Nakano M, Narula J, Kolodgie FD, Virmani R. Concept of vulnerable/unstable plaque. Arterioscler Thromb Vasc Biol. 2010;30(7):1282–92. doi:10.1161/ATVBAHA.108.179739.
Kolodgie FD, Virmani R, Burke AP, Farb A, Weber DK, Kutys R, et al. Pathologic assessment of the vulnerable human coronary plaque. Heart. 2004;90(12):1385–91. doi:10.1136/hrt.2004.041798.
Stone GW, Maehara A, Lansky AJ, de Bruyne B, Cristea E, Mintz GS, et al. A prospective natural-history study of coronary atherosclerosis. New Engl J Med. 2011;364(3):226–35. doi:10.1056/NEJMoa1002358. In this study of a cohort of patients with ACS who underwent PCI, the authors used VH-IVUS to detail lesion characteristics in culprit and non-culprit lesions that were associated with future major adverse cardiovascular events.
Calvert PA, Obaid DR, O'Sullivan M, Shapiro LM, McNab D, Densem CG, et al. Association between IVUS findings and adverse outcomes in patients with coronary artery disease: the VIVA (VH-IVUS in Vulnerable Atherosclerosis) Study. JACC Cardiovasc Imaging. 2011;4(8):894–901. doi:10.1016/j.jcmg.2011.05.005.
Garcia-Garcia HM, Gogas BD, Serruys PW, Bruining N. IVUS-based imaging modalities for tissue characterization: similarities and differences. Int J Card Imag. 2011;27(2):215–24. doi:10.1007/s10554-010-9789-7.
Raffel OC, Akasaka T, Jang IK. Cardiac optical coherence tomography. Heart. 2008;94(9):1200–10. doi:10.1136/hrt.2007.130765.
Kume T, Akasaka T, Kawamoto T, Okura H, Watanabe N, Toyota E, et al. Measurement of the thickness of the fibrous cap by optical coherence tomography. Am Heart J. 2006;152(4):755 e1–4. doi:10.1016/j.ahj.2006.06.030.
Uemura S, Ishigami K, Soeda T, Okayama S, Sung JH, Nakagawa H, et al. Thin-cap fibroatheroma and microchannel findings in optical coherence tomography correlate with subsequent progression of coronary atheromatous plaques. Eur Heart J. 2012;33(1):78–85. doi:10.1093/eurheartj/ehr284.
Takarada S, Imanishi T, Kubo T, Tanimoto T, Kitabata H, Nakamura N, et al. Effect of statin therapy on coronary fibrous-cap thickness in patients with acute coronary syndrome: assessment by optical coherence tomography study. Atherosclerosis. 2009;202(2):491–7. doi:10.1016/j.atherosclerosis.2008.05.014.
Kastrati A, Schomig A, Elezi S, Schuhlen H, Dirschinger J, Hadamitzky M, et al. Predictive factors of restenosis after coronary stent placement. J Am Coll Cardiol. 1997;30(6):1428–36.
Dussaillant GR, Mintz GS, Pichard AD, Kent KM, Satler LF, Popma JJ, et al. Small stent size and intimal hyperplasia contribute to restenosis: a volumetric intravascular ultrasound analysis. J Am Coll Cardiol. 1995;26(3):720–4. doi:10.1016/0735-1097(95)00249-4.
Albiero R, Rau T, Schluter M, Di Mario C, Reimers B, Mathey DG, et al. Comparison of immediate and intermediate-term results of intravascular ultrasound versus angiography-guided Palmaz-Schatz stent implantation in matched lesions. Circulation. 1997;96(9):2997–3005.
Kasaoka S, Tobis JM, Akiyama T, Reimers B, Di Mario C, Wong ND, et al. Angiographic and intravascular ultrasound predictors of in-stent restenosis. J Am Coll Cardiol. 1998;32(6):1630–5.
Parise H, Maehara A, Stone GW, Leon MB, Mintz GS. Meta-analysis of randomized studies comparing intravascular ultrasound versus angiographic guidance of percutaneous coronary intervention in pre-drug-eluting stent era. Am J Cardiol. 2011;107(3):374–82. doi:10.1016/j.amjcard.2010.09.030. This meta-analysis of eight randomized trials comparing IVUS versus angiographic guidance of PCI with BMS showed that IVUS use reduced angiographic restenosis, repeat revascularization, and major adverse cardiac events; there was no significant effect on death and myocardial infarction during follow-up of 6 months to 2.5 years.
Russo RJ, Silva PD, Teirstein PS, Attubato MJ, Davidson CJ, DeFranco AC, et al. A randomized controlled trial of angiography versus intravascular ultrasound-directed bare-metal coronary stent placement (the AVID Trial). Circ Cardiovasc Interv. 2009;2(2):113–23. doi:10.1161/CIRCINTERVENTIONS.108.778647.
Blasini R, Neumann FJ, Schmitt C, Walter H, Schomig A. Restenosis rate after intravascular ultrasound-guided coronary stent implantation. Cathet Cardiovasc Diagn. 1998;44(4):380–6.
Fitzgerald PJ, Oshima A, Hayase M, Metz JA, Bailey SR, Baim DS, et al. Final results of the Can Routine Ultrasound Influence Stent Expansion (CRUISE) study. Circulation. 2000;102(5):523–30.
Choi JW, Goodreau LM, Davidson CJ. Resource utilization and clinical outcomes of coronary stenting: a comparison of intravascular ultrasound and angiographical guided stent implantation. Am Heart J. 2001;142(1):112–8. doi:10.1067/mhj.2001.115793.
Jakabcin J, Spacek R, Bystron M, Kvasnak M, Jager J, Veselka J, et al. Long-term health outcome and mortality evaluation after invasive coronary treatment using drug eluting stents with or without the IVUS guidance. Randomized control trial. HOME DES IVUS. Cathet Cardiovasc Interv. 2010;75(4):578–83. doi:10.1002/ccd.22244.
Fujii K, Mintz GS, Kobayashi Y, Carlier SG, Takebayashi H, Yasuda T, et al. Contribution of stent underexpansion to recurrence after sirolimus-eluting stent implantation for in-stent restenosis. Circulation. 2004;109(9):1085–8. doi:10.1161/01.CIR.0000121327.67756.19.
Park SM, Kim JS, Ko YG, Choi D, Hong MK, Jang Y, et al. Angiographic and intravascular ultrasound follow up of paclitaxel- and sirolimus-eluting stent after poststent high-pressure balloon dilation: from the poststent optimal stent expansion trial. Cathet Cardiovasc Interv. 2011;77(1):15–21. doi:10.1002/ccd.22635.
Roy P, Steinberg DH, Sushinsky SJ, Okabe T, Pinto Slottow TL, Kaneshige K, et al. The potential clinical utility of intravascular ultrasound guidance in patients undergoing percutaneous coronary intervention with drug-eluting stents. Eur Heart J. 2008;29(15):1851–7. doi:10.1093/eurheartj/ehn249.
Tanaka A, Imanishi T, Kitabata H, Kubo T, Takarada S, Tanimoto T, et al. Lipid-rich plaque and myocardial perfusion after successful stenting in patients with non-ST-segment elevation acute coronary syndrome: an optical coherence tomography study. Eur Heart J. 2009;30(11):1348–55. doi:10.1093/eurheartj/ehp122.
Lee T, Yonetsu T, Koura K, Hishikari K, Murai T, Iwai T, et al. Impact of coronary plaque morphology assessed by optical coherence tomography on cardiac troponin elevation in patients with elective stent implantation. Circ Cardiovasc Interv. 2011;4(4):378–86. doi:10.1161/CIRCINTERVENTIONS.111.962506.
Kume T, Okura H, Miyamoto Y, Yamada R, Saito K, Tamada T, et al. Natural history of stent edge dissection, tissue protrusion and incomplete stent apposition detectable only on optical coherence tomography after stent implantation - preliminary observation. Circ J. 2012;76(3):698–703.
Park SJ, Kim YH, Park DW, Lee SW, Kim WJ, Suh J, et al. Impact of intravascular ultrasound guidance on long-term mortality in stenting for unprotected left main coronary artery stenosis. Circ Cardiovasc Interv. 2009;2(3):167–77. doi:10.1161/CIRCINTERVENTIONS.108.799494.
Patel Y, Depta JP, Novak E, Yeung M, Lavine K, Banerjee S, et al. Long-term outcomes with use of intravascular ultrasound for the treatment of coronary bifurcation lesions. Am J Cardiol. 2012;109(7):960–5. doi:10.1016/j.amjcard.2011.11.022.
Serruys PW, Ormiston JA, Onuma Y, Regar E, Gonzalo N, Garcia-Garcia HM, et al. A bioabsorbable everolimus-eluting coronary stent system (ABSORB): 2-year outcomes and results from multiple imaging methods. Lancet. 2009;373(9667):897–910. doi:10.1016/S0140-6736(09)60325-1.
Attizzani GF, Bezerra HG, Chamie D, Fujino Y, Spognardi AM, Stanley JR, et al. Serial Evaluation of Vascular Response After Implantation of a New Sirolimus-Eluting Stent With Bioabsorbable Polymer (MISTENT): an optical coherence tomography and histopathological study. J Invasive Cardiol. 2012;24(11):560–8.
Onuma Y, Serruys PW, Perkins LE, Okamura T, Gonzalo N, Garcia-Garcia HM, et al. Intracoronary optical coherence tomography and histology at 1 month and 2, 3, and 4 years after implantation of everolimus-eluting bioresorbable vascular scaffolds in a porcine coronary artery model: an attempt to decipher the human optical coherence tomography images in the ABSORB trial. Circulation. 2010;122(22):2288–300. doi:10.1161/CIRCULATIONAHA.109.921528.
Navarro F, Sullivan TM, Bacharach JM. Intravascular ultrasound assessment of iliac stent procedures. J Endovasc Ther. 2000;7(4):315–9. doi:10.1583/1545-1550(2000)007<0315:IUAOIS>2.3.CO;2.
Buckley CJ, Arko FR, Lee S, Mettauer M, Little D, Atkins M, et al. Intravascular ultrasound scanning improves long-term patency of iliac lesions treated with balloon angioplasty and primary stenting. J Vasc Surg. 2002;35(2):316–23.
Krishnamurthy VN, Eliason JL, Henke PK, Rectenwald JE. Intravascular ultrasound-guided true lumen reentry device for recanalization of unilateral chronic total occlusion of iliac arteries: technique and follow-up. Ann Vasc Surg. 2010;24(4):487–97. doi:10.1016/j.avsg.2009.12.002.
Levine GN, Bates ER, Blankenship JC, Bailey SR, Bittl JA, Cercek B, et al. 2011 ACCF/AHA/SCAI Guideline for Percutaneous Coronary Intervention. A report of the American College of Cardiology Foundation/American Heart Association Task Force on Practice Guidelines and the Society for Cardiovascular Angiography and Interventions. J Am Coll Cardiol. 2011;58(24):e44–122. doi:10.1016/j.jacc.2011.08.007.
Task Force on Myocardial Revascularization of the European Society of C, the European Association for Cardio-Thoracic S, European Association for Percutaneous Cardiovascular I, Wijns W, Kolh P, Danchin N, et al. Guidelines on myocardial revascularization. Eur Heart J. 2010;31(20):2501–55. doi:10.1093/eurheartj/ehq277.
Goldstein J, Dixon SR, Stone GW. NIRS-IVUS Imaging Identifies Lesions at High Risk of Peri-Procedural Myocardial Infarction. J Invasive Cardiol. 2013;25(Supplement A):14A–6A.
Sanidas E, Dangas G. Evolution of intravascular assessment of coronary anatomy and physiology: from ultrasound imaging to optical and flow assessment. Eur J Clin Investig. 2013;43(9):996–1008. doi:10.1111/eci.12119.
Compliance with Ethics Guidelines
Conflict of Interest
Dr. Paul M. Johnson, Dr. Jigar Patel, and Dr. Michael Yeung each declare no potential conflicts of interest relevant to this article.
Dr. Prashant Kaul received honoraria and travel/accommodations expenses covered for reimbursed from Volcano Corp (unrelated to intra-coronary imaging).
Human and Animal Rights and Informed Consent
This article does not contain any studies with human or animal subjects performed by any of the authors.
Author information
Authors and Affiliations
Corresponding author
Additional information
This article is part of the Topical Collection on Coronary Artery Disease
Rights and permissions
About this article
Cite this article
Johnson, P.M., Patel, J., Yeung, M. et al. Intra-Coronary Imaging Modalities. Curr Treat Options Cardio Med 16, 304 (2014). https://doi.org/10.1007/s11936-014-0304-7
Published:
DOI: https://doi.org/10.1007/s11936-014-0304-7