Abstract
Purpose of Review
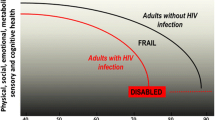
As a consequence of antiretroviral therapy, the proportion of older HIV-infected adults is increasing, with a concomitant shift in burden of illness to age-related syndromes and disease. Frailty is an age-related syndrome of increased vulnerability to stress, predictive of major adverse clinical outcomes among HIV-infected and uninfected persons alike. Understanding frailty pathogenesis is critical to developing interventions to improve health outcomes in HIV. Here, we review the current evidence for the relationship between inflammation and frailty in HIV, and the potential for novel, inflammation-targeted interventions.
Recent Findings
Dysregulated inflammation has been consistently associated with frailty in elderly HIV-uninfected persons. Dysregulated inflammation is also central to HIV pathophysiology and several recent studies have demonstrated the important association of inflammation with frailty in HIV. Some evidence suggests that anti-inflammatory therapies may be effective in ameliorating the adverse impact of frailty among aging HIV-infected adults, though further investigation is necessary.
Summary
Inflammation has been implicated in frailty in HIV infection, and improved understanding of the role that inflammation plays in frailty pathogenesis is key to the development of effective therapies to slow or prevent frailty in the vulnerable HIV-infected population.

Similar content being viewed by others
References
Papers of particular interest, published recently, have been highlighted as: • Of importance •• Of major importance
Smit M, Brinkman K, Geerlings S, Smit C, Thyagarajan K, Sighem A, et al. Future challenges for clinical care of an ageing population infected with HIV: a modelling study. Lancet Infect Dis. 2015;15(7):810–8. https://doi.org/10.1016/S1473-3099(15)00056-0.
Wing EJ. The aging population with HIV infection. Trans Am Clin Climatol Assoc. 2017;128:131–44.
Oursler KK, Sorkin JD, Smith BA, Katzel LI. Reduced aerobic capacity and physical functioning in older HIV-infected men. AIDS Res Hum Retrovir. 2006;22(11):1113–21. https://doi.org/10.1089/aid.2006.22.1113.
Desquilbet L, Jacobson LP, Fried LP, Phair JP, Jamieson BD, Holloway M, et al. HIV-1 infection is associated with an earlier occurrence of a phenotype related to frailty. J Gerontol A Biol Sci Med Sci. 2007;62(11):1279–86. https://doi.org/10.1093/gerona/62.11.1279.
Desquilbet L, Margolick JB, Fried LP, Phair JP, Jamieson BD, Holloway M, et al. Relationship between a frailty-related phenotype and progressive deterioration of the immune system in HIV-infected men. J Acquir Immune Defic Syndr. 2009;50(3):299–306. https://doi.org/10.1097/QAI.0b013e3181945eb0.
Onen NF, Agbebi A, Shacham E, Stamm KE, Onen AR, Overton ET. Frailty among HIV-infected persons in an urban outpatient care setting. J Inf Secur. 2009;59(5):346–52.
Terzian AS, Holman S, Nathwani N, Robison E, Weber K, Young M, et al. Factors associated with preclinical disability and frailty among HIV-infected and HIV-uninfected women in the era of cART. J Women’s Health (Larchmt). 2009;18(12):1965–74. https://doi.org/10.1089/jwh.2008.1090.
Sacktor N, Skolasky RL, Cox C, Selnes O, Becker JT, Cohen B, et al. Longitudinal psychomotor speed performance in human immunodeficiency virus-seropositive individuals: impact of age and serostatus. J Neuro-Oncol. 2010;16(5):335–41.
Desquilbet L, Jacobson LP, Fried LP, Phair JP, Jamieson BD, Holloway M, et al. A frailty-related phenotype before HAART initiation as an independent risk factor for AIDS or death after HAART among HIV-infected men. J Gerontol A Biol Sci Med Sci. 2011;66((9):1030–8.
Richert L, Dehail P, Mercié P, Dauchy FA, Bruyand M, Greib C, et al. High frequency of poor locomotor performance in HIV-infected patients. AIDS. 2011;25(6):797–805. https://doi.org/10.1097/QAD.0b013e3283455dff.
Young B, Dao CN, Buchacz K, Baker R, Brooks JT, Investigators HOSH. Increased rates of bone fracture among HIV-infected persons in the HIV Outpatient Study (HOPS) compared with the US general population, 2000-2006. Clin Infect Dis. 2011;52(8):1061–8. https://doi.org/10.1093/cid/ciq242.
Islam FM, Wu J, Jansson J, Wilson DP. Relative risk of cardiovascular disease among people living with HIV: a systematic review and meta-analysis. HIV Med. 2012;13(8):453–68. https://doi.org/10.1111/j.1468-1293.2012.00996.x.
Erlandson KM, Allshouse AA, Jankowski CM, Duong S, Mawhinney S, Kohrt WM, et al. Comparison of functional status instruments in HIV-infected adults on effective antiretroviral therapy. HIV Clin Trials. 2012;13(6):324–34. https://doi.org/10.1310/hct1306-324.
Walker Harris V, Brown TT. Bone loss in the HIV-infected patient: evidence, clinical implications, and treatment strategies. J Infect Dis. 2012;205(Suppl 3):S391–8. https://doi.org/10.1093/infdis/jis199.
Erlandson KM, Allshouse AA, Jankowski CM, Duong S, MaWhinney S, Kohrt WM, et al. Risk factors for falls in HIV-infected persons. J Acquir Immune Defic Syndr. 2012;61(4):484–9. https://doi.org/10.1097/QAI.0b013e3182716e38.
Ruiz MA, Reske T, Cefalu C, Estrada J. Falls in HIV-infected patients: a geriatric syndrome in a susceptible population. J Int Assoc Providers AIDS Care. 2013;12(4):266–9. https://doi.org/10.1177/2325957413488204.
Althoff KN, Jacobson LP, Cranston RD, Detels R, Phair JP, Li X, et al. Age, comorbidities, and AIDS predict a frailty phenotype in men who have sex with men. J Gerontol A Biol Sci Med Sci. 2014;69((2):189–98.
Buchman AS, Boyle PA, Wilson RS, Tang Y, Bennett DA. Frailty is associated with incident Alzheimer’s disease and cognitive decline in the elderly. Psychosom Med. 2007;69(5):483–9. https://doi.org/10.1097/psy.0b013e318068de1d.
Makary MA, Segev DL, Pronovost PJ, Syin D, Bandeen-Roche K, Patel P, et al. Frailty as a predictor of surgical outcomes in older patients. J Am Coll Surg. 2010;210(6):901–8. https://doi.org/10.1016/j.jamcollsurg.2010.01.028.
Robinson TN, Wu DS, Stiegmann GV, Moss M. Frailty predicts increased hospital and six-month healthcare cost following colorectal surgery in older adults. Am J Surg. 2011;202(5):511–4. https://doi.org/10.1016/j.amjsurg.2011.06.017.
Bortz WMA. Conceptual framework of frailty: a review. J Gerontol A Biol Sci Med Sci. 2002;57(5):M283–8. https://doi.org/10.1093/gerona/57.5.M283.
Hogan DB, MacKnight C, Bergman H, Steering Committee CnIoFaA. Models, definitions, and criteria of frailty. Aging Clin Exp Res. 2003;15(3 Suppl):1–29.
Fried LP, Ferrucci L, Darer J, Williamson JD, Anderson G. Untangling the concepts of disability, frailty, and comorbidity: implications for improved targeting and care. J Gerontol A Biol Sci Med Sci. 2004;59(3):255–63.
Bortz W. Understanding frailty. J Gerontol A Biol Sci Med Sci. 2010;65(3):255–6. discussion 7
Morley JE, Vellas B, van Kan GA, Anker SD, Bauer JM, Bernabei R, et al. Frailty consensus: a call to action. J Am Med Dir Assoc. 2013;14(6):392–7. https://doi.org/10.1016/j.jamda.2013.03.022.
Erlandson KM, Schrack JA, Jankowski CM, Brown TT, Campbell TB. Functional impairment, disability, and frailty in adults aging with HIV-infection. Curr HIV/AIDS Rep. 2014;11(3):279–90. https://doi.org/10.1007/s11904-014-0215-y.
Piggott DA, Erlandson KM, Yarasheski KE. Frailty in HIV: epidemiology, biology, measurement, interventions, and research needs. Curr HIV/AIDS Rep. 2016;13(6):340–8. https://doi.org/10.1007/s11904-016-0334-8.
Margolick JB, Chopra RK. Relationship between the immune system and frailty: pathogenesis of immune deficiency in HIV infection and aging. Aging (Milano). 1992;4(3):255–7.
Gustafson DR, Shi Q, Thurn M, Holman S, Minkoff H, Cohen M, et al. Frailty and constellations of factors in aging HIV-infected and uninfected women—the Women’s Interagency HIV Study. J Frailty Aging. 2016;5(1):43–8. https://doi.org/10.14283/jfa.2016.79.
Kooij KW, Wit FW, Schouten J, van der Valk M, Godfried MH, Stolte IG, et al. HIV infection is independently associated with frailty in middle-aged HIV type 1-infected individuals compared with similar but uninfected controls. AIDS. 2016;30(2):241–50. https://doi.org/10.1097/QAD.0000000000000910.
Önen NF, Patel P, Baker J, Conley L, Brooks JT, Bush T, et al. Frailty and pre-frailty in a contemporary cohort of HIV-infected adults. J Frailty Aging. 2014;3(3):158–65. https://doi.org/10.14283/jfa.2014.18.
Pathai S, Gilbert C, Weiss HA, Cook C, Wood R, Bekker LG, et al. Frailty in HIV-infected adults in South Africa. J Acquir Immune Defic Syndr. 2013;62(1):43–51. https://doi.org/10.1097/QAI.0b013e318273b631.
Piggott DA, Muzaale AD, Mehta SH, Brown TT, Patel KV, Leng SX, et al. Frailty, HIV infection, and mortality in an aging cohort of injection drug users. PLoS One. 2013;8(1):e54910. https://doi.org/10.1371/journal.pone.0054910.
Rees HC, Ianas V, McCracken P, Smith S, Georgescu A, Zangeneh T, et al. Measuring frailty in HIV-infected individuals. Identification of frail patients is the first step to amelioration and reversal of frailty. J Visual Exper: JoVE. 2013;77. https://doi.org/10.3791/50537
• Justice AC, Freiberg MS, Tracy R, Kuller L, Tate JP, Goetz MB, et al. Does an index composed of clinical data reflect effects of inflammation, coagulation, and monocyte activation on mortality among those aging with HIV. Clin Infect Dis. 2012;54(7):984–94. This study showed that an index of clinical variables was associated with inflammation and predictive of mortality in HIV-infected individuals.
Oursler KK, Tate JP, Gill TM, Crothers K, Brown TT, Crystal S, et al. Association of the veterans aging cohort study index with exercise capacity in HIV-infected adults. AIDS Res Hum Retrovir. 2013;29(9):1218–23. https://doi.org/10.1089/AID.2012.0388.
Womack JA, Goulet JL, Gibert C, Brandt CA, Skanderson M, Gulanski B, et al. Physiologic frailty and fragility fracture in HIV-infected male veterans. Clin Infect Dis. 2013;56(10):1498–504. https://doi.org/10.1093/cid/cit056.
Tate JP, Justice AC, Hughes MD, Bonnet F, Reiss P, Mocroft A, et al. An internationally generalizable risk index for mortality after one year of antiretroviral therapy. AIDS. 2013;27(4):563–72. https://doi.org/10.1097/QAD.0b013e32835b8c7f.
Brothers TD, Rockwood K. Biologic aging, frailty, and age-related disease in chronic HIV infection. Curr Opin HIV AIDS. 2014;9(4):412–8. https://doi.org/10.1097/COH.0000000000000070.
Marquine MJ, Umlauf A, Rooney AS, Fazeli PL, Gouaux BD, Paul Woods S, et al. The veterans aging cohort study index is associated with concurrent risk for neurocognitive impairment. J Acquir Immune Defic Syndr. 2014;65(2):190–7. https://doi.org/10.1097/QAI.0000000000000008.
Piggott DA, Muzaale AD, Varadhan R, Mehta SH, Westergaard RP, Brown TT, et al. Frailty and cause-specific hospitalization among persons aging with HIV infection and injection drug use. J Gerontol A Biol Sci Med Sci. 2017;72(3):389–94.
Buchner DM, Wagner EH. Preventing frail health. Clin Geriatr Med. 1992;8(1):1–17.
Clegg A, Young J, Iliffe S, Rikkert MO, Rockwood K. Frailty in elderly people. Lancet. 2013;381(9868):752–62. https://doi.org/10.1016/S0140-6736(12)62167-9.
Fedarko NS. The biology of aging and frailty. Clin Geriatr Med. 2011;27(1):27–37. https://doi.org/10.1016/j.cger.2010.08.006.
Fried LP, Hadley EC, Walston JD, Newman AB, Newman A, Guralnik JM, et al. From bedside to bench: research agenda for frailty. Sci Aging Knowl Environ. 2005;2005(31):pe24. https://doi.org/10.1126/sageke.2005.31.pe24.
Walston J, Hadley EC, Ferrucci L, Guralnik JM, Newman AB, Studenski SA, et al. Research agenda for frailty in older adults: toward a better understanding of physiology and etiology: summary from the American Geriatrics Society/National Institute on Aging research conference on frailty in older adults. J Am Geriatr Soc. 2006;54(6):991–1001. https://doi.org/10.1111/j.1532-5415.2006.00745.x.
Fried LP, Xue QL, Cappola AR, Ferrucci L, Chaves P, Varadhan R, et al. Nonlinear multisystem physiological dysregulation associated with frailty in older women: implications for etiology and treatment. J Gerontol A Biol Sci Med Sci. 2009;64((10):1049–57.
Ances BM, Vaida F, Yeh MJ, Liang CL, Buxton RB, Letendre S, et al. HIV infection and aging independently affect brain function as measured by functional magnetic resonance imaging. J Infect Dis. 2010;201(3):336–40. https://doi.org/10.1086/649899.
Walston J. Frailty—the search for underlying causes. Sci Aging Knowl Environ. 2004;2004:4):pe4.
Leng S, Chaves P, Koenig K, Walston J. Serum interleukin-6 and hemoglobin as physiological correlates in the geriatric syndrome of frailty: a pilot study. J Am Geriatr Soc. 2002;50(7):1268–71. https://doi.org/10.1046/j.1532-5415.2002.50315.x.
Hubbard RE, O’Mahony MS, Savva GM, Calver BL, Woodhouse KW. Inflammation and frailty measures in older people. J Cell Mol Med. 2009;13(9B):3103–9. https://doi.org/10.1111/j.1582-4934.2009.00733.x.
Walston J, MA MB, Newman A, Tracy RP, Kop WJ, Hirsch CH, et al. Frailty and activation of the inflammation and coagulation systems with and without clinical comorbidities: results from the Cardiovascular Health Study. Arch Intern Med. 2002;162(20):2333–41. https://doi.org/10.1001/archinte.162.20.2333.
Schmaltz HN, Fried LP, Xue QL, Walston J, Leng SX, Semba RD. Chronic cytomegalovirus infection and inflammation are associated with prevalent frailty in community-dwelling older women. J Am Geriatr Soc. 2005;53(5):747–54. https://doi.org/10.1111/j.1532-5415.2005.53250.x.
Leng SX, Xue QL, Tian J, Walston JD, Fried LP. Inflammation and frailty in older women. J Am Geriatr Soc. 2007;55(6):864–71. https://doi.org/10.1111/j.1532-5415.2007.01186.x.
Collerton J, Martin-Ruiz C, Davies K, Hilkens CM, Isaacs J, Kolenda C, et al. Frailty and the role of inflammation, immunosenescence and cellular ageing in the very old: cross-sectional findings from the Newcastle 85+ study. Mech Ageing Dev. 2012;133(6):456–66. https://doi.org/10.1016/j.mad.2012.05.005.
Singh T, Newman AB. Inflammatory markers in population studies of aging. Ageing Res Rev. 2011;10(3):319–29. https://doi.org/10.1016/j.arr.2010.11.002.
Yao X, Li H, Leng SX. Inflammation and immune system alterations in frailty. Clin Geriatr Med. 2011;27(1):79–87. https://doi.org/10.1016/j.cger.2010.08.002.
Ferrucci L, Penninx BW, Volpato S, Harris TB, Bandeen-Roche K, Balfour J, et al. Change in muscle strength explains accelerated decline of physical function in older women with high interleukin-6 serum levels. J Am Geriatr Soc. 2002;50(12):1947–54. https://doi.org/10.1046/j.1532-5415.2002.50605.x.
Maggio M, Guralnik JM, Longo DL, Ferrucci L. Interleukin-6 in aging and chronic disease: a magnificent pathway. J Gerontol A Biol Sci Med Sci. 2006;61(6):575–84. https://doi.org/10.1093/gerona/61.6.575.
Janssen SP, Gayan-Ramirez G, Van den Bergh A, Herijgers P, Maes K, Verbeken E, et al. Interleukin-6 causes myocardial failure and skeletal muscle atrophy in rats. Circulation. 2005;111(8):996–1005. https://doi.org/10.1161/01.CIR.0000156469.96135.0D.
van Hall G, Steensberg A, Fischer C, Keller C, Møller K, Moseley P, et al. Interleukin-6 markedly decreases skeletal muscle protein turnover and increases nonmuscle amino acid utilization in healthy individuals. J Clin Endocrinol Metab. 2008;93(7):2851–8. https://doi.org/10.1210/jc.2007-2223.
Bach E, Nielsen RR, Vendelbo MH, Møller AB, Jessen N, Buhl M, et al. Direct effects of TNF-α on local fuel metabolism and cytokine levels in the placebo-controlled, bilaterally infused human leg: increased insulin sensitivity, increased net protein breakdown, and increased IL-6 release. Diabetes. 2013;62(12):4023–9. https://doi.org/10.2337/db13-0138.
Chaves PH, Semba RD, Leng SX, Woodman RC, Ferrucci L, Guralnik JM, et al. Impact of anemia and cardiovascular disease on frailty status of community-dwelling older women: the Women’s health and aging studies I and II. J Gerontol A Biol Sci Med Sci. 2005;60(6):729–35. https://doi.org/10.1093/gerona/60.6.729.
Leng SX, Cappola AR, Andersen RE, Blackman MR, Koenig K, Blair M, et al. Serum levels of insulin-like growth factor-I (IGF-I) and dehydroepiandrosterone sulfate (DHEA-S), and their relationships with serum interleukin-6, in the geriatric syndrome of frailty. Aging Clin Exp Res. 2004;16(2):153–7. https://doi.org/10.1007/BF03324545.
Deeks SG. HIV infection, inflammation, immunosenescence, and aging. Annu Rev Med. 2011;62(1):141–55. https://doi.org/10.1146/annurev-med-042909-093756.
Hunt PW, Sinclair E, Rodriguez B, Shive C, Clagett B, Funderburg N, et al. Gut epithelial barrier dysfunction and innate immune activation predict mortality in treated HIV infection. J Infect Dis. 2014;210(8):1228–38. https://doi.org/10.1093/infdis/jiu238.
Tenorio AR, Zheng Y, Bosch RJ, Krishnan S, Rodriguez B, Hunt PW, et al. Soluble markers of inflammation and coagulation but not T-cell activation predict non-AIDS-defining morbid events during suppressive antiretroviral treatment. J Infect Dis. 2014;210(8):1248–59. https://doi.org/10.1093/infdis/jiu254.
Erlandson KM, Campbell TB. Inflammation in chronic HIV infection: what can we do? J Infect Dis. 2015;212(3):339–42. https://doi.org/10.1093/infdis/jiv007.
Zapata HJ, Shaw AC. Aging of the human innate immune system in HIV infection. Curr Opin Immunol. 2014;29:127–36.
•• Erlandson KM, Allshouse AA, Jankowski CM, Lee EJ, Rufner KM, Palmer BE, et al. Association of functional impairment with inflammation and immune activation in HIV type 1-infected adults receiving effective antiretroviral therapy. J Infect Dis. 2013;208(2):249–59. This study demonstrated that inflammation and immune activation were significantly associated with functional impairment in HIV-infected adults.
•• Piggott DA, Varadhan R, Mehta SH, Brown TT, Li H, Walston JD, et al. Frailty, inflammation, and mortality among persons aging with HIV infection and injection drug use. J Gerontol A Biol Sci Med Sci. 2015;70(12):1542-1547. This study found that an inflammatory index was significantly associated with frailty and mortality risk independent of HIV stage.
•• Erlandson KM, Ng DK, Jacobson LP, Margolick JB, Dobs AS, Palella FJ, et al. Inflammation, immune activation, immunosenescence, and hormonal biomarkers in the frailty-related phenotype of men with or at risk for HIV infection. J Infect Dis. 2017;215(2):228–37. This study demonstrated that frailty by the frailty-related phenotype was associated with increased markers of inflammation. Importantly, with an HIV-uninfected control group, this study demonstrated that frailty, not HIV serostatus was associated with inflammation.
•• Margolick JB, Bream JH, Martínez-Maza O, Lopez J, Li X, Phair JP, et al. Frailty and circulating markers of inflammation in HIV+ and HIV− men in the multicenter AIDS Cohort Study. J Acquir Immune Defic Syndr. 2017;74(4):407–17. This study expanded findings from the prior reference, using the full frailty phenotype. Using this definition of frailty, authors found that CRP levels were associated with frailty in HIV-infected men, independent of other comorbidities.
Yeoh HL, Cheng AC, Cherry CL, Weir JM, Meikle PJ, Hoy JF, et al. Immunometabolic and lipidomic markers associated with the frailty index and quality of life in aging HIV+ men on antiretroviral therapy. EBioMed. 2017;22:112–21. https://doi.org/10.1016/j.ebiom.2017.07.015.
Wallet MA, Buford TW, Joseph AM, Sankuratri M, Leeuwenburgh C, Pahor M, et al. Increased inflammation but similar physical composition and function in older-aged, HIV-1 infected subjects. BMC Immunol. 2015;16(43) https://doi.org/10.1186/s12865-015-0106-z.
Baranoski AS, Harris A, Michaels D, Miciek R, Storer T, Sebastiani P, et al. Relationship between poor physical function, inflammatory markers, and comorbidities in HIV-infected women on antiretroviral therapy. J Women's Health (Larchmt). 2014;23(1):69–76. https://doi.org/10.1089/jwh.2013.4367.
Crawford KW, Li X, Xu X, Abraham AG, Dobs AS, Margolick JB, et al. Lipodystrophy and inflammation predict later grip strength in HIV-infected men: the MACS body composition substudy. AIDS Res Hum Retrovir. 2013;29(8):1138–45. https://doi.org/10.1089/aid.2013.0020.
•• Piggott D, Bandeen-Roche K, Mehta S, Brown T, Yang H, Walston J, et al. Frailty progression and recovery among persons aging with HIV and substance use. Conference on Retroviruses and Opportunistic Infections; 2017; Seattle, Washington. This study demonstrated that reduced inflammation was significantly associated with reduced frailty progression and greater frailty recovery in HIV-infected and uninfected drug users.
Fried LP, Tangen CM, Walston J, Newman AB, Hirsch C, Gottdiener J, et al. Frailty in older adults: evidence for a phenotype. J Gerontol A Biol Sci Med Sci. 2001;56(3):M146–56. https://doi.org/10.1093/gerona/56.3.M146.
Buta BJ, Walston JD, Godino JG, Park M, Kalyani RR, Xue QL, et al. Frailty assessment instruments: systematic characterization of the uses and contexts of highly-cited instruments. Ageing Res Rev. 2016;26:53–61. https://doi.org/10.1016/j.arr.2015.12.003.
Walston JD, Bandeen-Roche K. Frailty: a tale of two concepts. BMC Med. 2015;13(185) https://doi.org/10.1186/s12916-015-0420-6.
• Mave V, Erlandson KM, Gupte N, Balagopal A, Asmuth DM, Campbell TB, et al. Inflammation and change in body weight with antiretroviral therapy initiation in a multinational cohort of HIV-infected adults. J Infect Dis. 2016;214(1):65–72. This study showed that low body weight, a domain of the frailty phenotype, was associated with increased levels of inflammatory markers in HIV-infected adults initiating ART.
• Lee KA, Gay CL, Lerdal A, Pullinger CR, Aouizerat BE. Cytokine polymorphisms are associated with fatigue in adults living with HIV/AIDS. Brain Behav Immun. 2014;40:95–103. This study found that fatigue, a domain of the frailty phenotype, was associated with inflammatory cytokine polymorphisms in HIV-infected individuals.
• Anzinger JJ, Butterfield TR, Angelovich TA, Crowe SM, Palmer CS. Monocytes as regulators of inflammation and HIV-related comorbidities during cART. J Immunol Res. 2014;2014:569819. Is frailty itself associated with inflammation, or are the comorbidities associated with inflammation? In this study, inflammation was associated with comorbidities related to HIV infection.
Yarasheski KE, Pak-Loduca J, Hasten DL, Obert KA, Brown MB, Sinacore DR. Resistance exercise training increases mixed muscle protein synthesis rate in frail women and men >/=76 yr old. Am J Phys. 1999;277(1 Pt 1):E118–25.
Liu CK, Fielding RA. Exercise as an intervention for frailty. Clin Geriatr Med. 2011;27(1):101–10.
de Labra C, Guimaraes-Pinheiro C, Maseda A, Lorenzo T, Millán-Calenti JC. Effects of physical exercise interventions in frail older adults: a systematic review of randomized controlled trials. BMC Geriatr. 2015;15(154) https://doi.org/10.1186/s12877-015-0155-4.
Fried LP. Interventions for human frailty: physical activity as a model. Cold Spring Harb Perspect Med. 2016;6(6) https://doi.org/10.1101/cshperspect.a025916.
Cameron ID, Fairhall N, Langron C, Lockwood K, Monaghan N, Aggar C, et al. A multifactorial interdisciplinary intervention reduces frailty in older people: randomized trial. BMC Med. 2013;11(65) https://doi.org/10.1186/1741-7015-11-65.
Chan DC, Tsou HH, Yang RS, Tsauo JY, Chen CY, Hsiung CA, et al. A pilot randomized controlled trial to improve geriatric frailty. BMC Geriatr. 2012;12(58) https://doi.org/10.1186/1471-2318-12-58.
Bonato M, Galli L, Passeri L, Longo V, Pavei G, Bossolasco S, et al. A pilot study of brisk walking in sedentary combination antiretroviral treatement (cART)-treated patients: benefit on soluble and cell inflammatory markers. BMC Infect Dis. 2017;17(1):61. https://doi.org/10.1186/s12879-016-2095-9.
Zanetti HR, Cruz LG, Lourenço CL, Neves FF, Silva-Vergara ML, Mendes EL. Non-linear resistance training reduces inflammatory biomarkers in persons living with HIV: a randomized controlled trial. Eur J Sport Sci. 2016;16(8):1232–9. https://doi.org/10.1080/17461391.2016.1167962.
Cutrono SE, Lewis JE, Perry A, Signorile J, Tiozzo E, Jacobs KA. The effect of a community-based exercise program on inflammation, metabolic risk, and fitness levels among persons living with HIV/AIDS. AIDS Behav. 2016;20(5):1123–31. https://doi.org/10.1007/s10461-015-1245-1.
Mondillo S, Ballo P, Barbati R, Guerrini F, Ammaturo T, Agricola E, et al. Effects of simvastatin on walking performance and symptoms of intermittent claudication in hypercholesterolemic patients with peripheral vascular disease. Am J Med. 2003;114(5):359–64. https://doi.org/10.1016/S0002-9343(03)00010-X.
Bielecka-Dabrowa A, Goch JH, Mikhailidis DP, Rysz J, Maciejewski M, Banach M. The influence of atorvastatin on parameters of inflammation and function of the left ventricle in patients with dilated cardiomyopathy. Med Sci Monit: Int Med J Exp Clin Res. 2009;15(12):Ms12–23.
Kerimkulova A, Noruzbaeva A, Lunegova O, Gotfrid I, Mirrakhimov A, Davydova N, et al. Influence of one-year treatment with lovastatin on myocardial remodeling and ischemia in patients with coronary artery disease. Anadolu Kardiyol Derg. 2011;11(1):16–21. https://doi.org/10.5152/akd.2011.004.
Laufs U, Wassmann S, Schackmann S, Heeschen C, Bohm M, Nickenig G. Beneficial effects of statins in patients with non-ischemic heart failure. Zeitschrift fur Kardiologie. 2004;93(2):103–8. https://doi.org/10.1007/s00392-004-1005-0.
Lee TM, Chen CC, Shen HN, Chang NC. Effects of pravastatin on functional capacity in patients with chronic obstructive pulmonary disease and pulmonary hypertension. Clin Sci (Lond). 2009;116(6):497–505. https://doi.org/10.1042/CS20080241.
Lee TM, Lin MS, Chang NC. Usefulness of C-reactive protein and interleukin-6 as predictors of outcomes in patients with chronic obstructive pulmonary disease receiving pravastatin. Am J Cardiol. 2008;101(4):530–5. https://doi.org/10.1016/j.amjcard.2007.09.102.
Liu M, Wang F, Wang Y, Jin R. Atorvastatin improves endothelial function and cardiac performance in patients with dilated cardiomyopathy: the role of inflammation. Cardiovasc Drugs Ther / Sponsored by the Int Soc Cardiovasc Pharmacother. 2009;23(5):369–76.
Mohler ER, Hiatt WR, Creager MA. Cholesterol reduction with atorvastatin improves walking distance in patients with peripheral arterial disease. Circulation. 2003;108(12):1481–6. https://doi.org/10.1161/01.CIR.0000090686.57897.F5.
Agostini JV, Tinetti ME, Han L, McAvay G, Foody JM, Concato J. Effects of statin use on muscle strength, cognition, and depressive symptoms in older adults. J Am Geriatr Soc. 2007;55(3):420–5. https://doi.org/10.1111/j.1532-5415.2007.01071.x.
Riechman SE, Andrews RD, Maclean DA, Sheather S. Statins and dietary and serum cholesterol are associated with increased lean mass following resistance training. J Gerontol A Biol Sci Med Sci. 2007;62(10):1164–71. https://doi.org/10.1093/gerona/62.10.1164.
Erlandson KM, Jiang Y, Debanne SM, McComsey GA. Effects of 96 weeks of rosuvastatin on bone, muscle, and fat in HIV-infected adults on effective antiretroviral therapy. AIDS Res Hum Retrovir. 2016;32(4):311–6. https://doi.org/10.1089/aid.2015.0191.
LaCroix AZ, Gray SL, Aragaki A, Cochrane BB, Newman AB, Kooperberg CL, et al. Statin use and incident frailty in women aged 65 years or older: prospective findings from the Women’s Health Initiative observational study. J Gerontol A Biol Sci Med Sci. 2008;63(4):369–75. https://doi.org/10.1093/gerona/63.4.369.
Looney RJ, Falsey A, Campbell D, Torres A, Kolassa J, Brower C, et al. Role of cytomegalovirus in the T cell changes seen in elderly individuals. Clin Immunol. 1999;90(2):213–9. https://doi.org/10.1006/clim.1998.4638.
Olsson J, Wikby A, Johansson B, Löfgren S, Nilsson BO, Ferguson FG. Age-related change in peripheral blood T-lymphocyte subpopulations and cytomegalovirus infection in the very old: the Swedish longitudinal OCTO immune study. Mech Ageing Dev. 2000;121(1–3):187–201.
Khan N, Shariff N, Cobbold M, Bruton R, Ainsworth JA, Sinclair AJ, et al. Cytomegalovirus seropositivity drives the CD8 T cell repertoire toward greater clonality in healthy elderly individuals. J Immunol. 2002;169(4):1984–92. https://doi.org/10.4049/jimmunol.169.4.1984.
Koch S, Larbi A, Ozcelik D, Solana R, Gouttefangeas C, Attig S, et al. Cytomegalovirus infection: a driving force in human T cell immunosenescence. Ann N Y Acad Sci. 2007;1114(1):23–35. https://doi.org/10.1196/annals.1396.043.
Wang GC, Kao WH, Murakami P, Xue QL, Chiou RB, Detrick B, et al. Cytomegalovirus infection and the risk of mortality and frailty in older women: a prospective observational cohort study. Am J Epidemiol. 2010;171(10):1144–52. https://doi.org/10.1093/aje/kwq062.
Mathei C, Vaes B, Wallemacq P, Degryse J. Associations between cytomegalovirus infection and functional impairment and frailty in the BELFRAIL cohort. J Am Geriatr Soc. 2011;59(12):2201–8. https://doi.org/10.1111/j.1532-5415.2011.03719.x.
Vallejo AN, Hamel DL, Mueller RG, Ives DG, Michel JJ, Boudreau RM, et al. NK-like T cells and plasma cytokines, but not anti-viral serology, define immune fingerprints of resilience and mild disability in exceptional aging. PLoS One. 2011;6(10):e26558. https://doi.org/10.1371/journal.pone.0026558.
• Freeman ML, Mudd JC, Shive CL, Younes SA, Panigrahi S, Sieg SF, et al. CD8 T-cell expansion and inflammation linked to CMV coinfection in ART-treated HIV infection. Clin Infect Dis. 2016;62(3):392–6. An important potential pathogen in frailty in HIV-uninfected persons, this study found that CMV coinfection was associated with increased inflammation in ART-treated HIV infection.
Erlandson KM, Allshouse AA, Rapaport E, Palmer BE, Wilson CC, Weinberg A, et al. Physical function impairment of older, HIV-infected adults is associated with cytomegalovirus immunoglobulin response. AIDS Res Hum Retrovir. 2015;31(9):905–12. https://doi.org/10.1089/aid.2015.0085.
Margolick J, Bream J, Li H, Nilles T, Leng S, Editors. T-cell reactivity to cytomegalovirus, inflammation, and frailty in HIV+ and HIV− men who have sex with men. 7th international workshop on HIV and aging; 26-27 September 2016; Washington, DC.
Hunt PW, Martin JN, Sinclair E, Epling L, Teague J, Jacobson MA, et al. Valganciclovir reduces T cell activation in HIV-infected individuals with incomplete CD4+ T cell recovery on antiretroviral therapy. J Infect Dis. 2011;203(10):1474–83. https://doi.org/10.1093/infdis/jir060.
Ancuta P, Kamat A, Kunstman KJ, Kim EY, Autissier P, Wurcel A, et al. Microbial translocation is associated with increased monocyte activation and dementia in AIDS patients. PLoS One. 2008;3(6):e2516. https://doi.org/10.1371/journal.pone.0002516.
Estes JD, Harris LD, Klatt NR, Tabb B, Pittaluga S, Paiardini M, et al. Damaged intestinal epithelial integrity linked to microbial translocation in pathogenic simian immunodeficiency virus infections. PLoS Pathog. 2010;6(8):e1001052. https://doi.org/10.1371/journal.ppat.1001052.
Nazli A, Chan O, Dobson-Belaire WN, Ouellet M, Tremblay MJ, Gray-Owen SD, et al. Exposure to HIV-1 directly impairs mucosal epithelial barrier integrity allowing microbial translocation. PLoS Pathog. 2010;6(4):e1000852. https://doi.org/10.1371/journal.ppat.1000852.
Klatt NR, Estes JD, Sun X, Ortiz AM, Barber JS, Harris LD, et al. Loss of mucosal CD103+ DCs and IL-17+ and IL-22+ lymphocytes is associated with mucosal damage in SIV infection. Mucosal Immunol. 2012;5(6):646–57. https://doi.org/10.1038/mi.2012.38.
Brenchley JM, Price DA, Schacker TW, Asher TE, Silvestri G, Rao S, et al. Microbial translocation is a cause of systemic immune activation in chronic HIV infection. Nat Med. 2006;12(12):1365–71. https://doi.org/10.1038/nm1511.
Bukh AR, Melchjorsen J, Offersen R, Jensen JM, Toft L, Støvring H, et al. Endotoxemia is associated with altered innate and adaptive immune responses in untreated HIV-1 infected individuals. PLoS One. 2011;6(6):e21275. https://doi.org/10.1371/journal.pone.0021275.
Pandrea I, Gaufin T, Brenchley JM, Gautam R, Monjure C, Gautam A, et al. Cutting edge: experimentally induced immune activation in natural hosts of simian immunodeficiency virus induces significant increases in viral replication and CD4+ T cell depletion. J Immunol. 2008;181(10):6687–91. https://doi.org/10.4049/jimmunol.181.10.6687.
Sandler NG, Wand H, Roque A, Law M, Nason MC, Nixon DE, et al. Plasma levels of soluble CD14 independently predict mortality in HIV infection. J Infect Dis. 2011;203(6):780–90. https://doi.org/10.1093/infdis/jiq118.
Reiner AP, Lange EM, Jenny NS, Chaves PH, Ellis J, Li J, et al. Soluble CD14: genomewide association analysis and relationship to cardiovascular risk and mortality in older adults. Arterioscler Thromb Vasc Biol. 2013;33(1):158–64. https://doi.org/10.1161/ATVBAHA.112.300421.
Reus S, Portilla J, Sánchez-Payá J, Giner L, Francés R, Such J, et al. Low-level HIV viremia is associated with microbial translocation and inflammation. J Acquir Immune Defic Syndr. 2013;62(2):129–34. https://doi.org/10.1097/QAI.0b013e3182745ab0.
Dinh DM, Volpe GE, Duffalo C, Bhalchandra S, Tai AK, Kane AV, et al. Intestinal microbiota, microbial translocation, and systemic inflammation in chronic HIV infection. J Infect Dis. 2015;211(1):19–27. https://doi.org/10.1093/infdis/jiu409.
Claesson MJ, Jeffery IB, Conde S, Power SE, O’Connor EM, Cusack S, et al. Gut microbiota composition correlates with diet and health in the elderly. Nature. 2012;488(7410):178–84. https://doi.org/10.1038/nature11319.
Jackson MA, Jackson M, Jeffery IB, Beaumont M, Bell JT, Clark AG, et al. Signatures of early frailty in the gut microbiota. Genome Med. 2016;8(1):8. https://doi.org/10.1186/s13073-016-0262-7.
Leng SX, Tian X, Matteini A, Li H, Hughes J, Jain A, et al. IL-6-independent association of elevated serum neopterin levels with prevalent frailty in community-dwelling older adults. Age Ageing. 2011;40(4):475–81. https://doi.org/10.1093/ageing/afr047.
• Villar-Garcia J, Hernandez JJ, Guerri-Fernandez R, Gonzalez A, Lerma E, Guelar A, et al. Effect of probiotics (Saccharomyces boulardii) on microbial translocation and inflammation in HIV-treated patients: a double-blind, randomized, placebo-controlled trial. J Acquir Immune Defic Syndr. 2015;68(3):256–63. This study demonstrated that S. boulardii probiotic treatment decreased inflammation parameters in virulogically suppressed HIV-infected individuals.
Jeffery CA, Shum DW, Hubbard RE. Emerging drug therapies for frailty. Maturitas. 2013;74(1):21–5. https://doi.org/10.1016/j.maturitas.2012.10.010.
Acknowledgements
Preparation of this work was supported, in part, by the National Institute of Aging and the National Institute of Allergy and Infectious Diseases of the National Institutes of Health (K23AG050260; R01AG054366 to KME; K23AI108357 to DAP) and the Robert Wood Johnson Foundation Harold Amos Award (to DAP). Contents are the authors’ sole responsibility and do not necessarily represent the official views of the National Institutes of Health or the Robert Wood Johnson Foundation.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of Interest
Stephanie M. Fukui declares no competing interests. Damani A. Piggott has received grants from the National Institute of Aging and the National Institute of Allergy and Infectious Diseases of the National Institutes of Health (K23AI108357) and the Robert Wood Johnson Foundation Harold Amos Award (to DAP). Kristine M. Erlandson has received grants from National Institute of Aging of the National Institutes of Health (K23AG050260; R01AG054366), Gilead Sciences, and Merck; research funding from Gilead Sciences; and has served as a consultant to Gilead Sciences, Serono, and Theratechnologies.
Human and Animal Rights and Informed Consent
This article does not contain any studies with human or animal subjects performed by any of the authors.
Additional information
This article is part of the Topical Collection on HIV Pathogenesis and Treatment
Rights and permissions
About this article
Cite this article
Fukui, S.M., Piggott, D.A. & Erlandson, K.M. Inflammation Strikes Again: Frailty and HIV. Curr HIV/AIDS Rep 15, 20–29 (2018). https://doi.org/10.1007/s11904-018-0372-5
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11904-018-0372-5