Abstract
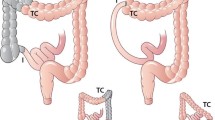
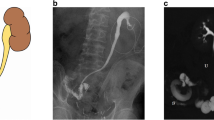
Radiologic imaging after urinary diversion is an essential part of the postoperative surveillance. Both early and late complications can be subtle. The primary goals are to evaluate for any upper tract abnormalities, tumor recurrence, or surgical complications. It is imperative that the urologist be aware of the radiologic evaluation of the most common urinary diversions, expected anatomic changes, and the various complications that may manifest following diversion.






Similar content being viewed by others
References
Papers of particular interest, published recently, have been highlighted as: • Of importance •• Of major importance
Hautmann RE, Abol-Enein H, Hafez K, et al. Urinary diversion. Urology. 2007;69:17–49.
Hautmann RE, Hautmann SH, Hautmann O. Complications associated with urinary diversion. Nat Rev Urol. 2011;8:667–77.
• Lee RK, Abol-Enein H, Artibani W, et al. Urinary diversion after radical cystectomy for bladder cancer: options, patient selection, and outcomes. BJU Int. 2014;113:11–23. A thorough analysis of peer reviewed studies that reviews diversion options and outcomes after urinary diversions.
Chong JT, Dolat MT, Klausner AP, et al. The role of cystectomy for non-malignant bladder conditions: a review. Can J Urol. 2014;21:7433–41.
Sudakoff GS, Guralnick M, Langenstroer P, et al. CT urography of urinary diversions with enhanced CT digital radiography: preliminary experience. AJR Am J Roentgenol. 2005;184:131–8.
Leyendecker JR, Barnes CE, Zagoria RJ. MR urography: techniques and clinical applications. Radiogr Rev Publ Radiol Soc N Am Inc. 2008;28:23–46. discussion 46–47.
Washburn ZW, Dillman JR, Cohan RH, et al. Computed tomographic urography update: an evolving urinary tract imaging modality. Semin Ultrasound CT MR. 2009;30:233–45.
Caoili EM, Cohan RH, Korobkin M, et al. Urinary tract abnormalities: initial experience with multi-detector row CT urography. Radiology. 2002;222:353–60.
McTavish JD, Jinzaki M, Zou KH, et al. Multi-detector row CT urography: comparison of strategies for depicting the normal urinary collecting system. Radiology. 2002;225:783–90.
Clark PE, Agarwal N, Biagioli MC, et al. Bladder cancer. J Natl Compr Cancer Netw JNCCN. 2013;11:446–75.
• Sudah M, Masarwah A, Kainulainen S, et al. Comprehensive MR urography protocol: equally good diagnostic performance and enhanced visibility of the upper urinary tract compared to triple-phase CT urography. PLoS One. 2016;11:e0158673. A comprehensive evaluation of the strengths and weaknesses of MRU and CTU.
Wang L-J, Wong Y-C, Huang C-C, et al. Multidetector computerized tomography urography is more accurate than excretory urography for diagnosing transitional cell carcinoma of the upper urinary tract in adults with hematuria. J Urol. 2010;183:48–55.
Sadowski EA, Bennett LK, Chan MR, et al. Nephrogenic systemic fibrosis: risk factors and incidence estimation. Radiology. 2007;243:148–57.
Childs DD, Leyendecker JR, Gianini J, et al. Contrast-enhanced magnetic resonance urography at 3T: clinical feasibility. J Comput Assist Tomogr. 2013;37:29–36.
Bricker EM. Bladder substitution after pelvic evisceration. Surg Clin North Am. 1950;30:1511–21.
Hautmann RE, Abol-Enein H, Lee CT, et al. Urinary diversion: how experts divert. Urology. 2015;85:233–8.
Kim SP, Shah ND, Weight CJ, et al. Population-based trends in urinary diversion among patients undergoing radical cystectomy for bladder cancer. BJU Int. 2013;112:478–84.
Williams O, Vereb MJ, Libertino JA. Noncontinent urinary diversion. Urol Clin North Am. 1997;24:735–44.
• Shimko MS, Tollefson MK, Umbreit EC, et al. Long-term complications of conduit urinary diversion. J Urol. 2011;185:562–7. A large informative review of complications in patients undergoing conduit urinary diversion.
•• Moomjian LN, Carucci LR, Guruli G, et al. Follow the stream: imaging of urinary diversions. Radiogr Rev Publ Radiol Soc N Am Inc. 2016;36:688–709. A notable review of imaging findings after urinary diversion.
Skinner, Eila C. and Daneshmand, Siamak: Orthotopic urinary diversion. In: Campbell-Walsh Urology. 11th ed.; pp 2344–2368. Available at: https://www-clinicalkey-com.laneproxy.stanford.edu/#!/content/book/3-s2.0-B9781455775675000996?scrollTo = %23b0045, accessed August 1, 2016.
Kock NG, Nilson AE, Nilsson LO, et al. Urinary diversion via a continent ileal reservoir: clinical results in 12 patients. J Urol. 1982;128:469–75.
Skinner EC. Continent cutaneous diversion. Curr Opin Urol. 2015;25:555–61.
DeCastro GJ, McKiernan, James M and Benson MC: Cutaneous continent urinary diversion. In: Campbell-Walsh Urology. 11th ed.; pp 2344–2368. Available at: https://www-clinicalkey-com.laneproxy.stanford.edu/#!/content/book/3-s2.0-B9781455775675000996?scrollTo = %23b0045, accessed August 1, 2016.
Sung DJ, Cho SB, Kim YH, et al. Imaging of the various continent urinary diversions after cystectomy. J Comput Assist Tomogr. 2004;28:299–310.
Hautmann RE, de Petriconi RC, Volkmer BG. 25 years of experience with 1,000 neobladders: long-term complications. J Urol. 2011;185:2207–12.
Stein JP, Esrig D, Freeman JA, et al. Prospective pathologic analysis of female cystectomy specimens: risk factors for orthotopic diversion in women. Urology. 1998;51:951–5.
Stenzl A, Draxl H, Posch B, et al. Original articles: bladder cancer: the risk of urethral tumors in female bladder cancer: can the urethra be used for orthotopic reconstruction of the lower urinary tract? J Urol. 1995;153:950–5.
Stein JP, Stenzl A, Esrig D, et al. Lower urinary tract reconstruction following cystectomy in women using the Kock ileal reservoir with bilateral ureteroileal urethrostomy: initial clinical experience. J Urol. 1994;152:1404–8.
Borirakchanyavat S, Aboseif SR, Carroll PR, et al. Continence mechanism of the isolated female urethra: an anatomical study of the intrapelvic somatic nerves. J Urol. 1997;158:822–6.
Konety BR, Allareddy V, Herr H. Complications after radical cystectomy: analysis of population-based data. Urology. 2006;68:58–64.
Chang SS, Cookson MS, Baumgartner RG, et al. Analysis of early complications after radical cystectomy: results of a collaborative care pathway. J Urol. 2002;167:2012–6.
Farnham SB, Cookson MS. Surgical complications of urinary diversion. World J Urol. 2004;22:157–67.
Person B and Wexner SD: In Brief. Curr. Probl. Surg. 2006; 43: 6–10
Bauer AJ, Boeckxstaens GE. Mechanisms of postoperative ileus. Neurogastroenterol Motil. 2004;16:54–60.
Hensle TW, Bredin HC, Dretler SP. Diagnosis and treatment of a urinary leak after ureteroileal conduit for diversion. J Urol. 1976;116:29–31.
Kanofsky JA, Godoy, Guilherme and Taneja, Samir S.: Complications of conduit urinary diversion. In: Complications of urologic surgery. 4th ed. Elsevier 2010; pp 533–546. Available at: https://www-clinicalkey-com.laneproxy.stanford.edu/#!/content/book/3-s2.0-B9781416045724000467, accessed July 29, 2016.
Chahal R, Sundaram SK, Iddenden R, et al. A study of the morbidity, mortality and long-term survival following radical cystectomy and radical radiotherapy in the treatment of invasive bladder cancer in Yorkshire. Eur Urol. 2003;43:246–57.
Catalá V, Solà M, Samaniego J, et al. CT findings in urinary diversion after radical cystectomy: postsurgical anatomy and complications. RadioGraphics. 2009;29:461–76.
Titton RL, Gervais DA, Hahn PF, et al. Urine leaks and urinomas: diagnosis and imaging-guided intervention. RadioGraphics. 2003;23:1133–47.
Skinner EC and Dunn: Complications of continent cutaneous diversions. In: Complications of urologic surgery. 4th ed. Elsevier 2010; pp 547–557. Available at: https://www-clinicalkey-com.laneproxy.stanford.edu/#!/content/book/3-s2.0-B9781416045724000467, accessed July 29, 2016.
Hedgire SS, Tabatabaei S, McDermott S, et al. Diversion ahead: imaging appearance of urinary diversions and reservoirs. Clin Imaging. 2014;38:418–27.
Msezane L, Reynolds WS, Mhapsekar R, et al. Open surgical repair of ureteral strictures and fistulas following radical cystectomy and urinary diversion. J Urol. 2008;179:1428–31.
Abol-Enein H, Ghoneim MA. Functional results of orthotopic ileal neobladder with serous-lined extramural ureteral reimplantation: experience with 450 patients. J Urol. 2001;165:1427.
Steven K, Poulsen AL. The orthotopic Kock ileal neobladder: functional results, urodynamic features, complications and survival in 166 men. J Urol. 2000;164:288–95.
Beiko DT, Razvi H. Stones in urinary diversions: update on medical and surgical issues. Curr Opin Urol. 2002;12:297–303.
Pantuck AJ, Han KR, Perrotti M, et al. Ureteroenteric anastomosis in continent urinary diversion: long-term results and complications of direct versus nonrefluxingtechniques. J Urol. 2000;163:450–5.
Ardelt PU, Woodhouse CRJ, Riedmiller H, et al. The efferent segment in continent cutaneous urinary diversion: a comprehensive review of the literature. BJU Int. 2012;109:288–97.
Keogan MT. Radiology of urinary diversions. Curr Opin Urol. 2000;10:117–22.
Tarter TH, Kawachi MH, Wilson TG. Entero-pouch fistula: a rare complication of right colon continent urinary diversion. J Urol. 1995;154:364–6.
Ali-El-Dein B, Ashamallah A. Vaginal repair of pouch-vaginal fistula after orthotopic bladder substitution in women. Urology. 2013;81:198–203.
Ali-El-Dein B, Shaaban AA, Abu-Eideh RH, et al. Surgical complications following radical cystectomy and orthotopic neobladders in women. J Urol. 2008;180:206–10.
Simon J, Bartsch Jr G, Küfer R, et al. Neobladder emptying failure in males: incidence, etiology and therapeutic options. J Urol. 2006;176:1468–72.
Kulkarni J n, Pramesh C s, Rathi S, et al. Long-term results of orthotopic neobladder reconstruction after radical cystectomy. BJU Int. 2003;91:485–8.
Shaaban AA, Abdel-Latif M, Mosbah A, et al. A randomized study comparing an antireflux system with a direct ureteric anastomosis in patients with orthotopic ileal neobladders. BJU Int. 2006;97:1057–62.
Hautmann RE, de Petriconi R, Gottfried HW, et al. The ileal neobladder: complications and functional results in 363 patients after 11 years of follow-up. J Urol. 1999;161:422–7.
McCallion WA, Wilson BG, Kennedy JA, et al. Ileal conduit-enteric fistula. Brit J Urol. 1993;71:230.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of Interest
Drs. Davenport and Enemchukwu declare no conflicts of interest.
Human and Animal Rights and Informed Consent
This article does not contain studies with human or animal subjects performed by the author.
Additional information
This article is part of the Topical Collection on Reconstructed Bladder Function & Dysfunction
Rights and permissions
About this article
Cite this article
Davenport, M.T., Enemchukwu, E.A. Abdominal Imaging Following Urinary Reconstruction: Recommendations and Pitfalls. Curr Bladder Dysfunct Rep 11, 291–299 (2016). https://doi.org/10.1007/s11884-016-0394-z
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11884-016-0394-z