Abstract
Purpose of Review
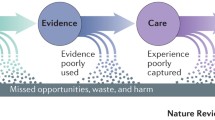
The past few decades have seen significant technologic innovation for the treatment and diagnosis of cardiovascular diseases. The subsequent growing complexity of modern medicine, however, is causing fundamental challenges in our healthcare system primarily in the spheres of patient involvement, data generation, and timely clinical implementation. The Institute of Medicine advocated for a learning health system (LHS) in which knowledge generation and patient care are inherently symbiotic. The purpose of this paper is to review how the advances in technology and big data have been used to further patient care and data generation and what future steps will need to occur to develop a LHS in cardiovascular disease.
Recent Findings
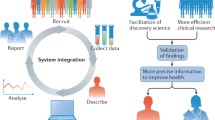
Patient-centered care has progressed from technologic advances yielding resources like decision aids. LHS can also incorporate patient preferences by increasing and standardizing patient-reported information collection. Additionally, data generation can be optimized using big data analytics by developing large interoperable datasets from multiple sources to allow for real-time data feedback.
Summary
Developing a LHS will require innovative technologic solutions with a patient-centered lens to facilitate symbiosis in data generation and clinical practice.

Similar content being viewed by others
References
Papers of particular interest, published recently, have been highlighted as: • Of importance •• Of major importance
Green LW, et al. Diffusion theory and knowledge dissemination, utilization, and integration in public health. Annu Rev Public Health. 2009;30:151–74.
Zikmund-Fisher BJ, et al. Deficits and variations in patients’ experience with making 9 common medical decisions: the decisions survey. Med Decis Making. 2010;30(5 Suppl):85S–95S.
Bevan GH, et al. Level of scientific evidence underlying the Current American College of Cardiology/American Heart Association clinical practice guidelines. Circ Cardiovasc Qual Outcomes. 2019;12(2):e005293.
•• Institute of Medicine. Best care at lower cost: the path to continuously learning health care in America: National Academies Press; 2013. This landmark report delves into the current barriers of effective evidence generation and implementation as well as recommendations to improve this system.
Elwyn G, et al. Investing in deliberation: a definition and classification of decision support interventions for people facing difficult health decisions. Med Decis Making. 2010;30(6):701–11.
Krumholz HM. Patient-centered medicine: the next phase in health care. Circ Cardiovasc Qual Outcomes. 2011;4(4):374–5.
Institute of Medicine. Crossing the quality chasm: a new health system for the 21st century. Washington, DC: National Academies Press; 2001.
Allen LA, et al. Decision making in advanced heart failure: a scientific statement from the American Heart Association. Circulation. 2012;125(15):1928–52.
Legare F, et al. Interventions for improving the adoption of shared decision making by healthcare professionals. Cochrane Database Syst Rev. 2014;9:CD006732.
Lalonde L, et al. Development and preliminary testing of a patient decision aid to assist pharmaceutical care in the prevention of cardiovascular disease. Pharmacotherapy. 2004;24(7):909–22.
Thomson RG, et al. A patient decision aid to support shared decision-making on anti-thrombotic treatment of patients with atrial fibrillation: randomised controlled trial. Qual Saf Health Care. 2007;16(3):216–23.
Mahler SA, et al. The HEART Pathway randomized trial: identifying emergency department patients with acute chest pain for early discharge. Circ Cardiovasc Qual Outcomes. 2015;8(2):195–203.
Coylewright M, et al. PCI choice decision aid for stable coronary artery disease: a randomized trial. Circ Cardiovasc Qual Outcomes. 2016;9(6):767–76.
Weymiller AJ, et al. Helping patients with type 2 diabetes mellitus make treatment decisions: statin choice randomized trial. Arch Intern Med. 2007;167(10):1076–82.
Man-Son-Hing M, et al. A patient decision aid regarding antithrombotic therapy for stroke prevention in atrial fibrillation: a randomized controlled trial. JAMA. 1999;282(8):737–43.
Hoefel L, et al. 20th Anniversary Update of the Ottawa Decision Support Framework Part 1: a systematic review of the decisional needs of people making health or social decisions. Med Decis Making. 2020;40(5):555–81.
Chewning B, et al. Patient preferences for shared decisions: a systematic review. Patient Educ Couns. 2012;86(1):9–18.
Wright JS, Wall HK, Ritchey MD. Million Hearts 2022: Small steps are needed for cardiovascular disease prevention. JAMA. 2018;320(18):1857–8.
• Rumsfeld JS, et al. Cardiovascular health: the importance of measuring patient-reported health status: a scientific statement from the American Heart Association. Circulation. 2013;127(22):2233–49 This scientific statement provides an overview of patient reported health methods and focuses on opportunities to broaden the inclusion of these metrics in research.
Hofer S, et al. The MacNew Heart Disease Health-Related Quality of Life Questionnaire in patients with angina and patients with ischemic heart failure. Value Health. 2012;15(1):143–50.
Spertus J, Dorian P, Bubien R, Lewis S, Godejohn D, Reynolds MR, et al. Development and validation of the Atrial Fibrillation Effect on QualiTy-of-Life (AFEQT) Questionnaire in patients with atrial fibrillation. Circ Arrhythm Electrophysiol. 2011;4(1):15–25.
Green CP, Porter CB, Bresnahan DR, Spertus JA. Development and evaluation of the Kansas City Cardiomyopathy Questionnaire: a new health status measure for heart failure. J Am Coll Cardiol. 2000;35(5):1245–55.
Beltrame JF, Weekes AJ, Morgan C, Tavella R, Spertus JA. The prevalence of weekly angina among patients with chronic stable angina in primary care practices: the Coronary Artery Disease in General Practice (CADENCE) Study. Arch Intern Med. 2009;169(16):1491–9.
Weintraub WS, S.J, Kolm P, Maron DJ, Zhang Z, Jurkovitz C, et al. COURAGE Trial Research Group. Effect of PCI on quality of life in patients with stable coronary disease. N Engl J Med. 2008;359:677–87.
Blumenthal DM, et al. Patient-reported outcomes in cardiology. Circ Cardiovasc Qual Outcomes. 2018;11(11):e004794.
Perez MV, Mahaffey KW, Hedlin H, Rumsfeld JS, Garcia A, Ferris T, et al. Large-scale assessment of a smartwatch to identify atrial fibrillation. N Engl J Med. 2019;381(20):1909–17.
ClinicalTrial.gov [Internet]. Bethesda (MD): National Library of Medicine (US). 2020 August - . Identifier NCT04468321, Effect of wearable devices on patient-reported outcomes and clinical utilization; cited 2020 October 6. Available from: https://clinicaltrials.gov/ct2/show/NCT04468321 .
Hoppe UC, Vanderheyden M, Sievert H, Brandt MC, Tobar R, Wijns W, et al. Chronic monitoring of pulmonary artery pressure in patients with severe heart failure: multicentre experience of the monitoring Pulmonary Artery Pressure by Implantable device Responding to Ultrasonic Signal (PAPIRUS) II study. Heart. 2009;95(13):1091–7.
Tricoci P, Allen JM, Kramer JM, Califf RM, Smith SC Jr. Scientific evidence underlying the ACC/AHA clinical practice guidelines. JAMA. 2009;301(8):831–41.
Angus DC. Fusing randomized trials with big data: the key to self-learning health care systems? JAMA. 2015;314(8):767–8.
• Institute of Medicine. Best care at lower cost: the path to continuously learning health care. Circ Cardiovasc Qual Outcomes. 2012;5(6):e93–4 This book explains the inefficiencies in healthcare that hinder improvements and advocates for transitioning to a continuously learning health care system.
• Raghupathi W, Raghupathi V. Big data analytics in healthcare: promise and potential. Health Inf Sci Syst. 2014;2:3 This article provides an overview of the advantages and disadvantages of using big data analytics in healthcare.
U.S. Food and Drug Administration. 21st Century Cures Act. Available at: https://www.fda.gov/RegulatoryInformation/LawsEnforcedbyFDA/SignificantAmendmentstotheFDCAct/21stCenturyCuresAct/default.htm . Accessed October 1, 2020.
Garvin JH, Y.K, Gobbel GT, et al. Automating quality measures for heart failure using natural language processing: a descriptive study in the Department of Veterans Affairs. JMIR Med Inform. 2018;6(1):e5.
Weiskopf NG, Hripcsak G, Swaminathan S, Weng C. Defining and measuring completeness of electronic health records for secondary use. J Biomed Inform. 2013;46(5):830–6.
Ackerman MJ. Computer briefs: big data. J Med Pract Manage. 2012;28(2):153–4.
Jensen PB, Jensen LJ, Brunak S. Mining electronic health records: towards better research applications and clinical care. Nat Rev Genet. 2012;13(6):395–405.
Ross MK, Wei W, Ohno-Machado L. “Big data” and the electronic health record. Yearb Med Inform. 2014;9:97–104.
Weis JM, Levy PC. Copy, paste, and cloned notes in electronic health records. Chest. 2014;145(3):632–8.
Connelly R, Playford CJ, Gayle V, Dibben C. The role of administrative data in the big data revolution in social science research. Soc Sci Res. 2016;59:1–12.
Frizzell JD, Liang L, Schulte PJ, Yancy CW, Heidenreich PA, Hernandez AF, et al. Prediction of 30-day all-cause readmissions in patients hospitalized for heart failure: comparison of machine learning and other statistical approaches. JAMA Cardiol. 2017;2(2):204–9.
Gavrielov-Yusim N, Friger M. Use of administrative medical databases in population-based research. J Epidemiol Community Health. 2014;68(3):283–7.
Shahian DM, Silverstein T, Lovett AF, Wolf RE, Normand SLT. Comparison of clinical and administrative data sources for hospital coronary artery bypass graft surgery report cards. Circulation. 2007;115(12):1518–27.
Sanborn TA, Tcheng JE, Anderson HV, Chambers CE, Cheatham SL, DeCaro MV, et al. ACC/AHA/SCAI 2014 health policy statement on structured reporting for the cardiac catheterization laboratory: a report of the American College of Cardiology Clinical Quality Committee. J Am Coll Cardiol. 2014;63(23):2591–623.
Carbo A, Gupta M, Tamariz L, Palacio A, Levis S, Nemeth Z, et al. Mobile technologies for managing heart failure: a systematic review and meta-analysis. Telemed J E Health. 2018;24:958–68.
Hung G, et al. Mobile health application platform ‘Corrie’ personalises and empowers the heart attack recovery patient experience in the hospital and at home for an underserved heart attack survivor. BMJ Case Rep. 2020;13(2).
ClinicalTrial.gov [Internet]. Bethesda (MD): National Library of Medicine (US). 2020 February - . Identifier NCT04276441, A study to investigate if early atrial fibrillation (AF) diagnosis reduces risk of events like stroke in the real-world; cited 2020 October 6. Available from: https://clinicaltrials.gov/ct2/show/NCT04276441.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Human and Animal Rights and Informed Consent
This article does not contain any studies with human or animal subjects performed by any of the authors.
Conflict of Interest
Khurram Nasir is on the Advisory Boards of Amgen, Novartis, and The Medicines Company, and his research is partly supported by the Jerold B. Katz Academy of Translational Research.
Seth Shay Martin reports personal fees from Amgen, AstraZeneca, Esperion, REGENXBIO, and 89bio; grants from Apple, Google, iHealth, Nokia, Maryland Innovation Initiative, American Heart Association, Aetna Foundation, PJ Schafer Memorial Fund, David and June Trone Family Foundation, Akcea Therapeutics,
and the National Institutes of Health; and is co-founder of Corrie Health, LLC. In addition, Dr. Martin has a pending patent on System of LDL-C Estimation.
The other authors declare no conflict of interest.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
This article is part of the Topical Collection on Evidence-Based Medicine, Clinical Trials and Their Interpretations
Rights and permissions
About this article
Cite this article
Wagle, A.A., Isakadze, N., Nasir, K. et al. Strengthening the Learning Health System in Cardiovascular Disease Prevention: Time to Leverage Big Data and Digital Solutions. Curr Atheroscler Rep 23, 19 (2021). https://doi.org/10.1007/s11883-021-00916-5
Accepted:
Published:
DOI: https://doi.org/10.1007/s11883-021-00916-5