Abstract
Purpose
This review and meta-analysis aimed to evaluate the effects of high-intensity interval training (HIIT) compared to usual care (UC) or moderate-intensity training (MIE) on physical fitness and health-related outcomes in cancer patients across all stages of therapy and aftercare.
Methods
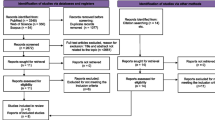
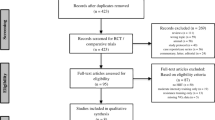
Databases were systematically searched in accordance with the PRISMA guidelines until October 4th, 2018. Eligibility criteria included adult patients of various cancer types, performing HIIT vs. UC or MIE. Outcomes of interest included physical fitness (cardiorespiratory fitness [VO2peak] and functional capacity) and health-related outcomes (body composition, quality of life, cancer-related fatigue, and blood-borne biomarkers). Mean differences (MD) were calculated and pooled to generate effect sizes for VO2peak.
Results
The search identified 1453 studies, out of which 12 articles were included. The average duration of interventions was 6.7 ± 3.0 weeks, with 2.8 ± 0.5 sessions per week. The meta-analysis for VO2peak showed superiority of HIIT compared to UC (MD 3.73; 95% CI 2.07, 5.39; p < 0.001) but not MIE (MD 1.36; 95% CI − 1.62, 4.35; p = 0.370). Similarly, no superior effects of HIIT compared to MIE were found for quality of life or changes in lean mass, while evidence was provided for a larger reduction in fat mass.
Conclusion
This systematic review showed that short-term HIIT induces similar positive effects on physical fitness and health-related outcomes as MIE but seems to be superior compared to UC. Thus, HIIT might be a time-efficient intervention for cancer patients across all stages of therapy and aftercare.
Implications for Cancer Survivors
High-intensity interval training (HIIT) is superior compared to usucal care in improving physical fitness and health-related outcomes in cancer patients across all stages of therapy and aftercare. Currently, there is no evidence for the benefits of HIIT compared to aerobic training of moderate intensity (MIE) for changes in cardiorespiratory fitness, lean mass and patient-reported outcomes. Reductions in fat mass may be more pronounced in HIIT compared to MIE when training is performed in aftercare.



Similar content being viewed by others
References
Silver JK. Cancer prehabilitation and its role in improving health outcomes and reducing healthcare costs. Semin Oncol Nurs 2015;1–49. doi:https://doi.org/10.1016/j.soncn.2014.11.003.
Silver JK, Raj VS, Fu JB, Wisotzky EM, Smith SR, Kirch RA. Cancer rehabilitation and palliative care: critical components in the delivery of high-quality oncology services. Support Care Cancer. 2015;23:3633–43. https://doi.org/10.1007/s00520-015-2916-1.
Cormie P, Atkinson M, Bucci L, Cust A, Eakin E, Hayes S, et al. Clinical Oncology Society of Australia position statement on exercise in cancer care. Med J Aust 2018;1–4. doi:https://doi.org/10.5694/mja18.00199.
Segal R, Zwaal C, Green E, Tomasone JR, Loblaw A, Petrella T, et al. Exercise for people with cancer: a clinical practice guideline. Curr Oncol. 2017;24:40–7. https://doi.org/10.3747/co.24.3376.
Fong DYT, Ho JWC, Hui BPH, Lee AM, Macfarlane DJ, Leung SSK, et al. Physical activity for cancer survivors: meta-analysis of randomised controlled trials. BMJ. 2012;344:e70. https://doi.org/10.1136/bmj.e70.
Kripp M, Heußer A-L, Belle S, Gerhardt A, Merx K, Hofmann W-K, et al. Does physical activity improve quality of life in cancer patients undergoing chemotherapy? Oncol Res Treat. 2015;38:230–6. https://doi.org/10.1159/000381734.
Buffart LM, Galvão DA, Brug J, Chinapaw MJM, Newton RU. Evidence-based physical activity guidelines for cancer survivors: current guidelines, knowledge gaps and future research directions. Cancer Treat Rev. 2014;40:327–40. https://doi.org/10.1016/j.ctrv.2013.06.007.
Cormie P, Zopf EM, Zhang X, Schmitz KH. The impact of exercise on cancer mortality, recurrence, and treatment-related adverse effects. Epidemiol Rev. 2017;39:71–92. https://doi.org/10.1093/epirev/mxx007.
Scott JM, Li N, Liu Q, Yasui Y, Leisenring W, Nathan PC, et al. Association of exercise with mortality in adult survivors of childhood cancer. JAMA Oncol. 2018:1–7. https://doi.org/10.1001/jamaoncol.2018.2254.
Hannan A, Hing W, Simas V, Climstein M, Coombes J, Jayasinghe R, et al. High-intensity interval training versus moderate-intensity continuous training within cardiac rehabilitation: a systematic review and meta-analysis. Oajsm. 2018;9:1–17. https://doi.org/10.2147/OAJSM.S150596.
Koelwyn GJ, Quail DF, Zhang X, White RM, Jones LW. Exercise-dependent regulation of the tumour microenvironment. Nat Publ Group. 2017;17:620–32. https://doi.org/10.1038/nrc.2017.78.
Batacan RB Jr, Duncan MJ, Dalbo VJ, Tucker PS, Fenning AS. Effects of high-intensity interval training on cardiometabolic health: a systematic review and meta-analysis of intervention studies. Br J Sports Med. 2017;51:494–503. https://doi.org/10.1136/bjsports-2015-095841.
Wahl P, Hägele M, Zinner C, Bloch W, Mester J. High intensity training (HIT) for the improvement of endurance capacity of recreationally active people and in prevention & rehabilitation. Wien Med Wochenschr. 2010;160:627–36. https://doi.org/10.1007/s10354-010-0857-3.
Weston KS, Wisløff U, Coombes JS. High-intensity interval training in patients with lifestyle-induced cardiometabolic disease: a systematic review and meta-analysis. BMJ 2014;1–10. doi:https://doi.org/10.1136/bjsports-2013-092576.
Mijwel S, Backman M, Bolam KA, Jervaeus A, Sundberg CJ, Margolin S, et al. Adding high-intensity interval training to conventional training modalities: optimizing health-related outcomes during chemotherapy for breast cancer: the OptiTrain randomized controlled trial. Breast Cancer Res Treat. 2017;168:79–93. https://doi.org/10.1007/s10549-017-4571-3.
Devin JL, Sax AT, Hughes GI, Jenkins DG, Aitken JF, Chambers SK, et al. The influence of high-intensity compared with moderate-intensity exercise training on cardiorespiratory fitness and body composition in colorectal cancer survivors: a randomised controlled trial. J Cancer Surviv. 2016;10:467–79. https://doi.org/10.1007/s11764-015-0490-7.
Adams SC, DeLorey DS, Davenport MH, Stickland MK, Fairey AS, North S, et al. Effects of high-intensity aerobic interval training on cardiovascular disease risk in testicular cancer survivors: a phase 2 randomized controlled trial. Cancer. 2017;123:4057–65. https://doi.org/10.1002/cncr.30859.
Kampshoff CS, Dongen JM, Mechelen W, Schep G, Vreugdenhil A, Twisk JWR, et al. Long-term effectiveness and cost-effectiveness of high versus low-to-moderate intensity resistance and endurance exercise interventions among cancer survivors. 2018;1–13. doi:https://doi.org/10.1007/s11764-018-0681-0.
Hofmann P. Cancer and exercise: Warburg hypothesis, tumour metabolism and high-intensity anaerobic exercise. Sports. 2018;6:10–21. https://doi.org/10.3390/sports6010010.
Toohey K. High-intensity exercise interventions in cancer survivors: a systematic review exploring the impact on health outcomes. J Cancer Res Clin Oncol. 2017. https://doi.org/10.1007/s00432-017-2552-x.
Moher D, Liberati A, Tetzlaff J, Altman DG, PRISMA Group. Preferred reporting items for systematic reviews and meta-analyses: the PRISMA statement. BMJ. 2009;339:b2535. https://doi.org/10.1136/bmj.b2535.
Karlsen T, Aamot I-L, Haykowsky M, Rognmo Ø. High intensity interval training for maximizing health outcomes. Prog Cardiovasc Dis. 2017;(1):–29. https://doi.org/10.1016/j.pcad.2017.03.006.
Borg GA. Psychophysical bases of perceived exertion. Med Sci Sports Exerc. 1982;14:377–81.
Deshpande P, Sudeepthi B, Rajan S, Abdul Nazir CP. Patient-reported outcomes: a new era in clinical research. Perspect Clin Res. 2011;2:137–9. https://doi.org/10.4103/2229-3485.86879.
Higgins JPT, Thompson SG. Quantifying heterogeneity in a meta-analysis. Stat Med. 2002;21:1539–58. https://doi.org/10.1002/sim.1186.
Gliner JA, Morgan GA, Harmon RJ. Pretest-posttest comparison group designs: analysis and interpretation. J Am Acad Child Adolesc Psychiatry. 2003;42:500–3. https://doi.org/10.1097/01.CHI.0000046809.95464.BE.
Sterne JA, Egger M, Smith GD. Systematic reviews in health care investigating and dealing with publication and other biases in meta-analysis. BMJ. 2001;323:101–5. https://doi.org/10.1136/bmj.323.7304.101.
Sterne JA, Gavaghan D, Egger M. Publication and related bias in meta-analysis: power of statistical tests and prevalence in the literature. J Clin Epidemiol. 2000;53:1119–29.
Higgins JPT, Altman DG, Gotzsche PC, Juni P, Moher D, Oxman AD, et al. The Cochrane Collaboration’s tool for assessing risk of bias in randomised trials. BMJ. 2011;343:d5928. https://doi.org/10.1136/bmj.d5928.
Sterne JA, Hernán MA, Reeves BC, Savović J, Berkman ND, Viswanathan M, et al. ROBINS-I: a tool for assessing risk of bias in non-randomised studies of interventions. BMJ. 2016:i4919–7. https://doi.org/10.1136/bmj.i4919.
Hwang C-L, Yu C-J, Shih J-Y, Yang P-C, Wu Y-T. Effects of exercise training on exercise capacity in patients with non-small cell lung cancer receiving targeted therapy. Support Care Cancer. 2012;20:3169–77. https://doi.org/10.1007/s00520-012-1452-5.
West MA, Loughney L, Lythgoe D, Barben CP, Sripadam R, Kemp GJ, et al. Effect of prehabilitation on objectively measured physical fitness after neoadjuvant treatment in preoperative rectal cancer patients: a blinded interventional pilot study. Br J Anaesth. 2015;114:244–51. https://doi.org/10.1093/bja/aeu318.
Dolan LB, Campbell K, Gelmon K, Neil-Sztramko S, Holmes D, McKenzie DC. Interval versus continuous aerobic exercise training in breast cancer survivors—a pilot RCT. Support Care Cancer. 2016;24:119–27. https://doi.org/10.1007/s00520-015-2749-y.
Licker M, Karenovics W, Diaper J, Frésard I, Triponez F, Ellenberger C, et al. Short-term preoperative high-intensity interval training in patients awaiting lung cancer surgery: a randomized controlled trial. J Thorac Oncol. 2016:1–30. https://doi.org/10.1016/j.jtho.2016.09.125.
Brunet J, Burke S, Grocott MPW, West MA, Jack S. The effects of exercise on pain, fatigue, insomnia, and health perceptions in patients with operable advanced stage rectal cancer prior to surgery: a pilot trial. BMC Cancer. 2017;17:153. https://doi.org/10.1186/s12885-017-3130-y.
Karenovics W, Licker M, Ellenberger C, Christodoulou M, Diaper J, Bhatia C, et al. Short-term preoperative exercise therapy does not improve long-term outcome after lung cancer surgery: a randomized controlled study. Eur J Cardiothorac Surg. 2017;52:47–54. https://doi.org/10.1093/ejcts/ezx030.
Adams SC, DeLorey DS, Davenport MH, Fairey AS, North S, Courneya KS. Effects of high-intensity interval training on fatigue and quality of life in testicular cancer survivors. Br J Cancer 2018;1–9. doi:https://doi.org/10.1038/s41416-018-0044-7.
Schmitt J, Lindner N, Reuss Borst M, Holmberg HC, Sperlich B. A 3-week multimodal intervention involving high-intensity interval training in female cancer survivors: a randomized controlled trial. Physiol Rep. 2016;4:e12693–8. https://doi.org/10.14814/phy2.12693.
Toohey K, Pumpa KL, Arnolda L, Cooke J, Yip D, Craft PS, et al. A pilot study examining the effects of low-volume high-intensity interval training and continuous low to moderate intensity training on quality of life, functional capacity and cardiovascular risk factors in cancer survivors. PeerJ. 2016;4:e2613–20. https://doi.org/10.7717/peerj.2613.
Devin JL, Jenkins DG, Sax AT, Hughes GI, Aitken JF, Chambers SK, et al. Cardiorespiratory fitness and body composition responses to different intensities and frequencies of exercise training in colorectal cancer survivors. Clin Colorectal Cancer. 2018:1–26. https://doi.org/10.1016/j.clcc.2018.01.004.
Ramos JS, Dalleck LC, Tjonna AE, Beetham KS, Coombes JS. The impact of high-intensity interval training versus moderate-intensity continuous training on vascular function: a systematic review and meta-analysis. Sports Med. 2015;45:679–92. https://doi.org/10.1007/s40279-015-0321-z.
Schmitz KH, Courneya KS, Matthews C, Demark-Wahnefried W, GALVÃO DA, Pinto BM, et al. American College of Sports Medicine roundtable on exercise guidelines for cancer survivors. Med Sci Sports Exerc. 2010;42:1409–26. https://doi.org/10.1249/MSS.0b013e3181e0c112.
Scharhag-Rosenberger F, Kuehl R, Klassen O, Schommer K, Schmidt ME, Ulrich CM, et al. Exercise training intensity prescription in breast cancer survivors: validity of current practice and specific recommendations. J Cancer Surviv. 2015;9:612–9. https://doi.org/10.1007/s11764-015-0437-z.
Moon H-G, Ju Y-T, Jeong C-Y, Jung E-J, Lee Y-J, Hong S-C, et al. Visceral obesity may affect oncologic outcome in patients with colorectal cancer. Ann Surg Oncol. 2008;15:1918–22. https://doi.org/10.1245/s10434-008-9891-4.
Britton KA, Massaro JM, Murabito JM, Kreger BE, Hoffmann U, Fox CS. Body fat distribution, incident cardiovascular disease, cancer, and all-cause mortality. J Am Coll Cardiol. 2013;62:921–5. https://doi.org/10.1016/j.jacc.2013.06.027.
Griggs JJ, Mangu PB, Anderson H, Balaban EP, Dignam JJ, Hryniuk WM, et al. Appropriate chemotherapy dosing for obese adult patients with cancer: American Society of Clinical Oncology clinical practice guideline. JCO. 2012;30:1553–61. https://doi.org/10.1200/JCO.2011.39.9436.
Prado CMM, Baracos VE, McCargar LJ, Mourtzakis M, Mulder KE, Reiman T, et al. Body composition as an independent determinant of 5-fluorouracil-based chemotherapy toxicity. Clin Cancer Res. 2007;13:3264–8. https://doi.org/10.1158/1078-0432.CCR-06-3067.
Ferrer RA, Huedo-Medina TB, Johnson BT, Ryan S, Pescatello LS. Exercise interventions for cancer survivors: a meta-analysis of quality of life outcomes. Ann Behav Med. 2010;41:32–47. https://doi.org/10.1007/s12160-010-9225-1.
Papadopoulos E. Can we HIIT cancer if we attack inflammation? Cancer Causes Control. 2017. https://doi.org/10.1007/s10552-017-0983-y.
Submission declaration and verification
The authors declare that this manuscript is not under consideration for publication elsewhere, that its publication is approved by all authors and tacitly or explicitly by the responsible authorities where the work was carried out, and that, if accepted, it will not be published elsewhere in the same form, in English or in any other language, including electronically without the written consent of the copyright holder.
Author information
Authors and Affiliations
Contributions
HM contributed to the design of the study, the literature search, data screening and extraction, statistical analyses, manuscript preparation and editing, and submission. NF contributed to the design of the study, the literature search, data screening and extraction, statistical analyses, manuscript preparation and editing, and submission. JW contributed to the design of the study as well as data screening and extraction. YY contributed to the data extraction, statistical analyses, and manuscript preparation. SC contributed to the data extraction and statistical analyses and contributed theoretical expertise and writing and editing of the manuscript. WB contributed to the data extraction and statistical analyses and contributed theoretical expertise and writing and editing of the manuscript. MS contributed to the design of the study, the literature search, data screening and extraction, and statistical analyses; provided methodological input and theoretical expertise; and contributed to writing and editing of the manuscript and submission.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Ethical approval
This manuscript does not contain any studies with human participants or animal subjects performed by any of the authors.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Mugele, H., Freitag, N., Wilhelmi, J. et al. High-intensity interval training in the therapy and aftercare of cancer patients: a systematic review with meta-analysis. J Cancer Surviv 13, 205–223 (2019). https://doi.org/10.1007/s11764-019-00743-3
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11764-019-00743-3