Abstract
Introduction
Bariatric surgery treats morbid obesity resulting in long-lasting weight loss. Elevated body mass index (BMI) increases breast cancer risk. We hypothesized that patients undergoing bariatric surgery would have decreased overall and estrogen receptor (ER)-positive breast cancer incidences compared to a propensity-matched non-surgical cohort.
Methods
The bariatric population included all female patients who underwent weight loss surgery at a single institution from 1985 to 2015. Patients from all outpatient visits were propensity score matched 1:1 with bariatric patients using BMI, comorbidities, demographics, and insurance status. The primary outcome was breast cancer incidence. Univariate analyses compared the groups.
Results
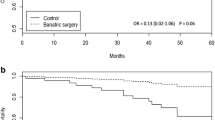
A total of 4860 patients were included, with 2430 in both groups. Median follow-up time from date of surgery or morbid obesity diagnosis was 5.7 years. There were no differences in age or comorbidities aside from gastroesophageal reflux disease. Seventeen (0.7%) patients in the surgery group were subsequently diagnosed with breast cancer versus 32 (1.3%) in the non-surgery group (p = 0.03). The non-surgery group had more ER-positive tumors [4 (36.4%) vs. 22 (71.0%); p = 0.04].
Conclusion
Female patients who underwent bariatric surgery were less frequently diagnosed with any breast cancer and ER-positive breast cancer versus a propensity-matched cohort suggesting a possible oncologic benefit to weight loss surgery.

Similar content being viewed by others
References
Flegal KM, Carroll MD, Kit BK, et al. Prevalence of obesity and trends in the distribution of body mass index among US adults, 1999-2010. JAMA. 2012;307(5):491–7.
Ogden CL, Carroll MD, Kit BK, et al. Prevalence of childhood and adult obesity in the United States, 2011-2012. JAMA. 2014;311(8):806–14.
Abdelaal M, le Roux CW, Docherty NG. Morbidity and mortality associated with obesity. Ann Transl Med. 2017;5(7):161.
Lauby-Secretan B, Scoccianti C, Loomis D, et al. Body fatness and cancer—viewpoint of the IARC Working Group. N Engl J Med. 2016;375(8):794–8.
Eheman C, Henley SJ, Ballard-Barbash R, et al. Annual Report to the Nation on the status of cancer, 1975-2008, featuring cancers associated with excess weight and lack of sufficient physical activity. Cancer. 2012;118(9):2338–66.
Calle EE, Rodriguez C, Walker-Thurmond K, et al. Overweight, obesity, and mortality from cancer in a prospectively studied cohort of U.S. adults. N Engl J Med. 2003;348(17):1625–38.
Reeves MJ, Newcomb PA, Remington PL, et al. Body mass and breast cancer. Relationship between method of detection and stage of disease. Cancer. 1996;77(2):301–7.
Chlebowski RT, Aiello E, McTiernan A. Weight loss in breast cancer patient management. J Clin Oncol. 2002;20(4):1128–43.
Breast Cancer Statistics. U.S. Department of Health & Human Services 2017; Available from: https://www.cdc.gov/cancer/breast/statistics/index.htm.
Owen JG, Yazdi F, Reisin E (2017) Bariatric surgery and hypertension. Am J Hypertens
Mehaffey JH, LaPar DJ, Clement KC, et al. 10-year outcomes after Roux-en-Y gastric bypass. Ann Surg. 2016;264(1):121–6.
Mehaffey JH, Mullen MG, Mehaffey RL, et al. Type 2 diabetes remission following gastric bypass: does diarem stand the test of time? Surg Endosc. 2017;31(2):538–42.
Adams TD, Stroup AM, Gress RE, et al. Cancer incidence and mortality after gastric bypass surgery. Obesity (Silver Spring). 2009;17(4):796–802.
Arterburn DE, Olsen MK, Smith VA, et al. Association between bariatric surgery and long-term survival. JAMA. 2015;313(1):62–70.
Anveden A, Taube M, Peltonen M, et al. Long-term incidence of female-specific cancer after bariatric surgery or usual care in the Swedish Obese Subjects Study. Gynecol Oncol. 2017;145(2):224–9.
Schauer DP, Feigelson HS, Koebnick C, Caan B, Weinmann S, Leonard AC, et al. (2017) Bariatric surgery and the risk of cancer in a large multisite cohort. Ann Surg
Winder AA, Kularatna M, MacCormick AD. Does bariatric surgery affect the incidence of breast Cancer development? A Systematic Review. Obes Surg. 2017;27(11):3014–20.
McMurry TL, Hu Y, Blackstone EH, et al. Propensity scores: methods, considerations, and applications in the Journal of Thoracic and Cardiovascular Surgery. J Thorac Cardiovasc Surg. 2015;150(1):14–9.
Casagrande DS, Rosa DD, Umpierre D, et al. Incidence of cancer following bariatric surgery: systematic review and meta-analysis. Obes Surg. 2014;24(9):1499–509.
Christou NV, Lieberman M, Sampalis F, et al. Bariatric surgery reduces cancer risk in morbidly obese patients. Surg Obes Relat Dis. 2008;4(6):691–5.
Renehan AG, Tyson M, Egger M, et al. Body-mass index and incidence of cancer: a systematic review and meta-analysis of prospective observational studies. Lancet. 2008;371(9612):569–78.
Calle EE, Kaaks R. Overweight, obesity and cancer: epidemiological evidence and proposed mechanisms. Nat Rev Cancer. 2004;4(8):579–91.
Bezemer ID, Rinaldi S, Dossus L, et al. C-peptide, IGF-I, sex-steroid hormones and adiposity: a cross-sectional study in healthy women within the European Prospective Investigation into Cancer and Nutrition (EPIC). Cancer Causes Control. 2005;16(5):561–72.
Simpson ER. Sources of estrogen and their importance. J Steroid Biochem Mol Biol. 2003;86(3–5):225–30.
Santen RJ, Boyd NF, Chlebowski RT, et al. Critical assessment of new risk factors for breast cancer: considerations for development of an improved risk prediction model. Endocr Relat Cancer. 2007;14(2):169–87.
Byers T, Sedjo RL. Does intentional weight loss reduce cancer risk? Diabetes Obes Metab. 2011;13(12):1063–72.
Fabian CJ, Kimler BF, Donnelly JE, et al. Favorable modulation of benign breast tissue and serum risk biomarkers is associated with > 10% weight loss in postmenopausal women. Breast Cancer Res Treat. 2013;142(1):119–32.
Modesitt SC, Hallowell PT, Slack-Davis JK, et al. Women at extreme risk for obesity-related carcinogenesis: baseline endometrial pathology and impact of bariatric surgery on weight, metabolic profiles and quality of life. Gynecol Oncol. 2015;138(2):238–45.
Funding
This work was financially supported by the National Institutes of Health [grant numbers T32HL007849 and T32CA163177].
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of Interest
The authors declare that they have no conflict of interest.
Ethical Statement
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards.
Consent Statement
For this type of study, format consent is not required.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Research reported in this publication was supported by the National Institutes of Health under Award Numbers T32HL007849 and T32CA163177.
Rights and permissions
About this article
Cite this article
Hassinger, T.E., Mehaffey, J.H., Hawkins, R.B. et al. Overall and Estrogen Receptor–Positive Breast Cancer Incidences Are Decreased Following Bariatric Surgery. OBES SURG 29, 776–781 (2019). https://doi.org/10.1007/s11695-018-3598-9
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11695-018-3598-9