Abstract
Background
Sleeve gastrectomy (SG) plus procedures have been developed to strengthen the effect of SG on diabetes control. The aim of this study was to compare diabetes control after SG plus bypass of the proximal small intestine with SG alone under adverse conditions for diabetes remission.
Methods
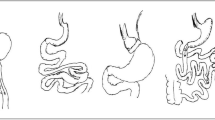
SG plus duodenojejunal bypass (SG-DJB), SG plus jejunojejunal bypass (SG-JJB), SG alone, and sham surgeries were performed in diabetic rats. A high-fat diet (HFD) was fed postoperatively to induce diabetes recurrence. Body weight, food intake, glucose tolerance, insulin sensitivity, serum hormones, hepatic function, and lipid profiles were measured postoperatively.
Results
SG-DJB, SG-JJB, and SG groups exhibited significant improvement in glucose tolerance and insulin sensitivity compared with the sham-operated group at 2 weeks postoperatively. Postoperative HFD induced obvious diabetes relapse and re-impaired insulin sensitivity at 16 weeks postoperatively. The SG-DJB and SG-JJB groups exhibited superior glucose tolerance and similar insulin sensitivity to SG alone at 16 weeks postoperatively. Compared with the SG alone, the SG-DJB and SG-JJB groups exhibited similar food intake, weight loss, fasting ghrelin, glucose-stimulated insulin secretion, and higher glucose-stimulated GLP-1 secretion.
Conclusion
SG-DJB and SG-JJB provided better diabetes control than SG alone in rats fed a HFD postoperatively. Further clinical studies are expected to confirm the superiority of SG plus bypass of proximal small intestine.






Similar content being viewed by others
References
Schauer PR, Bhatt DL, Kirwan JP, et al. Bariatric surgery versus intensive medical therapy for diabetes - 5-year outcomes. N Engl J Med. 2017;376(7):641–51.
Sjostrom L, Peltonen M, Jacobson P, et al. Association of bariatric surgery with long-term remission of type 2 diabetes and with microvascular and macrovascular complications. JAMA. 2014;311(22):2297–304.
Brito JP, Montori VM, Davis AM. Metabolic surgery in the treatment algorithm for type 2 diabetes: a joint statement by international diabetes organizations. JAMA. 2017;317(6):635–6.
Mingrone G, Panunzi S, De Gaetano A, et al. Bariatric-metabolic surgery versus conventional medical treatment in obese patients with type 2 diabetes: 5 year follow-up of an open-label, single-centre, randomised controlled trial. Lancet. 2015;386(9997):964–73.
Angrisani L, Santonicola A, Iovino P, et al. Bariatric surgery and endoluminal procedures: IFSO worldwide survey 2014. Obes Surg. 2017;27(9):2279–89.
Ponce J, DeMaria EJ, Nguyen NT, et al. American Society for Metabolic and Bariatric Surgery estimation of bariatric surgery procedures in 2015 and surgeon workforce in the United States. Surg Obes Relat Dis. 2016;12(9):1637–9.
Cho JM, Kim HJ, Lo Menzo E, et al. Effect of sleeve gastrectomy on type 2 diabetes as an alternative treatment modality to Roux-en-Y gastric bypass: systemic review and meta-analysis. Surg Obes Relat Dis. 2015;11(6):1273–80.
Jimenez A, Casamitjana R, Flores L, et al. Long-term effects of sleeve gastrectomy and Roux-en-Y gastric bypass surgery on type 2 diabetes mellitus in morbidly obese subjects. Ann Surg. 2012;256(6):1023–9.
Arterburn DE, Bogart A, Sherwood NE, et al. A multisite study of long-term remission and relapse of type 2 diabetes mellitus following gastric bypass. Obes Surg. 2013;23(1):93–102.
DiGiorgi M, Rosen DJ, Choi JJ, et al. Re-emergence of diabetes after gastric bypass in patients with mid- to long-term follow-up. Surg Obes Relat Dis. 2010;6(3):249–53.
Aminian A, Brethauer SA, Andalib A, et al. Can sleeve gastrectomy “cure” diabetes? Long-term metabolic effects of sleeve gastrectomy in patients with type 2 diabetes. Ann Surg. 2016;264(4):674–81.
Chikunguwo SM, Wolfe LG, Dodson P, et al. Analysis of factors associated with durable remission of diabetes after Roux-en-Y gastric bypass. Surg Obes Relat Dis. 2010;6(3):254–9.
Kashyap SR, Schauer P. Clinical considerations for the management of residual diabetes following bariatric surgery. Diabetes Obes Metab. 2012;14(9):773–9.
Buchwald H, Oien DM. Metabolic/bariatric surgery worldwide 2008. Obes Surg. 2009;19(12):1605–11.
Kasama K, Tagaya N, Kanehira E, et al. Laparoscopic sleeve gastrectomy with duodenojejunal bypass: technique and preliminary results. Obes Surg. 2009;19(10):1341–5.
Sun D, Liu S, Zhang G, et al. Type 2 diabetes control in a nonobese rat model using sleeve gastrectomy with duodenal-jejunal bypass (SGDJB). Obes Surg. 2012;22(12):1865–73.
Sanchez-Pernaute A, Rubio MA, Perez Aguirre E, et al. Single-anastomosis duodenoileal bypass with sleeve gastrectomy: metabolic improvement and weight loss in first 100 patients. Surg Obes Relat Dis. 2013;9(5):731–5.
Balibrea JM, Vilallonga R, Hidalgo M, et al. Mid-term results and responsiveness predictors after two-step single-anastomosis duodeno-ileal bypass with sleeve gastrectomy. Obes Surg. 2017;27(5):1302–8.
Hassn A, Luhmann A, Rahmani S, et al. Medium-term results of combined laparoscopic sleeve gastrectomy and modified Jejuno-Ileal bypass in bariatric surgery. Obes Surg. 2016;26(10):2316–23.
Alamo M, Sepulveda M, Gellona J, et al. Sleeve gastrectomy with jejunal bypass for the treatment of type 2 diabetes mellitus in patients with body mass index < 35 kg/m2. A cohort study. Obes Surg. 2012;22(7):1097–103.
Boza C, Munoz R, Yung E, et al. Sleeve gastrectomy with ileal transposition (SGIT) induces a significant weight loss and diabetes improvement without exclusion of the proximal intestine. J Gastrointest Surg. 2011;15(6):928–34.
Zhong MW, Liu SZ, Zhang GY, et al. Effects of sleeve gastrectomy with jejuno-jejunal or jejuno-ileal loop on glycolipid metabolism in diabetic rats. World J Gastroenterol. 2016;22(32):7332–41.
Liu SZ, Sun D, Zhang GY, et al. A high-fat diet reverses improvement in glucose tolerance induced by duodenal-jejunal bypass in type 2 diabetic rats. Chin Med J. 2012;125(5):912–9.
Karra E, Yousseif A, Batterham RL. Mechanisms facilitating weight loss and resolution of type 2 diabetes following bariatric surgery. Trends Endocrinol Metab. 2010;21(6):337–44.
Matthews DR, Hosker JP, Rudenski AS, et al. Homeostasis model assessment: insulin resistance and beta-cell function from fasting plasma glucose and insulin concentrations in man. Diabetologia. 1985;28(7):412–9.
Del Genio G, Gagner M, Cuenca-Abente F, et al. Laparoscopic sleeve gastrectomy with duodeno-jejunal bypass: a new surgical procedure for weight control. Feasibility and safety study in a porcine model. Obes Surg. 2008;18(10):1263–7.
Zachariah PJ, Chen CY, Lee WJ, et al. Compared to sleeve gastrectomy, duodenal-jejunal bypass with sleeve gastrectomy gives better glycemic control in T2DM patients, with a lower beta-cell response and similar appetite sensations: mixed-meal study. Obes Surg. 2016;26(12):2862–72.
Lee WJ, Almulaifi AM, Tsou JJ, et al. Duodenal-jejunal bypass with sleeve gastrectomy versus the sleeve gastrectomy procedure alone: the role of duodenal exclusion. Surg Obes Relat Dis. 2015;11(4):765–70.
Mitzman B, Cottam D, Goriparthi R, et al. Stomach intestinal pylorus sparing (SIPS) surgery for morbid obesity: retrospective analyses of our preliminary experience. Obes Surg. 2016;26(9):2098–104.
Sanchez-Pernaute A, Herrera MA, Perez-Aguirre ME, et al. Single anastomosis duodeno-ileal bypass with sleeve gastrectomy (SADI-S). one to three-year follow-up. Obes Surg. 2010;20(12):1720–6.
Sanchez-Pernaute A, Rubio MA, Conde M, et al. Single-anastomosis duodenoileal bypass as a second step after sleeve gastrectomy. Surg Obes Relat Dis. 2015;11(2):351–5.
Cottam A, Cottam D, Zaveri H, et al. An analysis of mid-term complications, weight loss, and type 2 diabetes resolution of stomach intestinal pylorus-sparing surgery (SIPS) versus Roux-En-Y gastric bypass (RYGB) with three-year follow-up. Obes Surg. 2018;28(9):2894–902.
Huang CK, Tai CM, Chang PC, et al. Loop duodenojejunal bypass with sleeve gastrectomy: comparative study with Roux-en-Y gastric bypass in type 2 diabetic patients with a BMI < 35 kg/m(2). First Year Results Obes Surg. 2016;26(10):2291–301.
Raj PP, Kumaravel R, Chandramaliteeswaran C, et al. Laparoscopic duodenojejunal bypass with sleeve gastrectomy: preliminary results of a prospective series from India. Surg Endosc. 2012;26(3):688–92.
Seki Y, Kasama K, Haruta H, et al. Five-year-results of laparoscopic sleeve gastrectomy with duodenojejunal bypass for weight loss and type 2 diabetes mellitus. Obes Surg. 2017;27(3):795–801.
Funding
This work was supported by the National Natural Science Foundation of China (81770795, 81300286, and 81700708), China Postdoctoral Science Foundation (2015M582096), Special Research Fund for the Doctoral Program of Higher Education (20130131120069), Special Research Fund for the Doctoral Program of Shandong Province (BS2013YY031), and the Taishan Scholar Foundation of Shandong Province.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of Interest
The authors declare that they have no conflict of interest.
Ethical Approval
This study was performed in accordance with the National Institutes of Health Guidelines on the Use of Laboratory Animals and was approved by the Ethics Committee on Experimental Animals of Qilu Hospital, Shandong University.
Statement of Informed Consent
Does not apply.
Rights and permissions
About this article
Cite this article
Cheng, Y., Huang, X., Wu, D. et al. Sleeve Gastrectomy with Bypass of Proximal Small Intestine Provides Better Diabetes Control than Sleeve Gastrectomy Alone Under Postoperative High-Fat Diet. OBES SURG 29, 84–92 (2019). https://doi.org/10.1007/s11695-018-3520-5
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11695-018-3520-5