Abstract
Background
The association between obesity and rising incidence of hepatocellular carcinoma (HCC) in the USA has been documented; however, the role of bariatric surgery remains less clear.
Aim
To evaluate the cross-sectional association of prior-bariatric surgery and HCC.
Methods
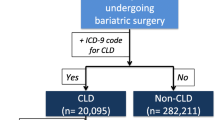
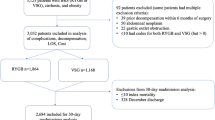
The United States Nationwide Inpatient Sample (NIS) database was queried from 2004 to 2014 for discharges with a diagnosis of morbid obesity. Primary outcomes of interest were HCC and in-hospital mortality rate. Secondary outcomes were length of stay and cost. Baseline characteristics were balanced using propensity score matching (PSM). Using Poisson and logistic regressions, adjusted HCC prevalence ratio (PR) and mortality odds ratio (OR) were derived in patients with prior-bariatric surgery compared to those without bariatric surgery.
Results
Of the 2,881,414 patients included in our study, 267,082 (9.3%) underwent bariatric surgery. From 2004 to 2014, there was a threefold increase in age-adjusted prevalence of HCC from 27 per 100,000 to 72 per 100,000 (PTrend < 0.001). After PSM, 230,956 patients with prior-bariatric surgery were matched with 230,956 patients without bariatric surgery. Prior-bariatric surgery was associated with lower prevalence of HCC (PR 0.11; 95% CI, 0.03–0.48; P < 0.001). In-hospital mortality was also lower for patients with surgery (OR 0.22; 95% CI, 0.20–0.26; P < 0.001). The occurrence of HCC added $18,840 extra cost, increased mean length of stay by 2 (95% CI; 1–3) days, and increased risk of death by 65% (aOR 1.65; 95% CI 1.18–2.29).
Conclusion
In this nationwide study of morbidly obese patients, prior-bariatric surgery was associated with a lower prevalence of HCC and lower in-patient mortality.




Similar content being viewed by others
References
El-Serag HB. Hepatocellular carcinoma. N Engl J Med. 2011;365:1118–27.
El-Serag HB, Kanwal F. Epidemiology of hepatocellular carcinoma in the United States: where are we? Where do we go? Hepatology. 2014;60:1767–75.
Njei B, Rotman Y, Ditah I, et al. Emerging trends in hepatocellular carcinoma incidence and mortality. Hepatology. 2015;61:191–9.
El-Serag HB, Davila JA, Petersen NJ, et al. The continuing increase in the incidence of hepatocellular carcinoma in the United States: an update. Ann Intern Med. 2003;139:817–23.
Caldwell SH, Crespo DM, Kang HS, et al. Obesity and hepatocellular carcinoma. Gastroenterology. 2004;127:S97–103.
Mitchell NS, Catenacci VA, Wyatt HR, et al. Obesity: overview of an epidemic. Psychiatr Clin N Am. 2011;34:717–32.
Calle EE, Rodriguez C, Walker-Thurmond K, et al. Overweight, obesity, and mortality from cancer in a prospectively studied cohort of U.S. adults. N Engl J Med. 2003;348:1625–38.
Moller H, Mellemgaard A, Lindvig K, et al. Obesity and cancer risk: a Danish record-linkage study. Eur J Cancer. 1994;30A:344–50.
Wolk A, Gridley G, Svensson M, et al. A prospective study of obesity and cancer risk (Sweden). Cancer Causes Control. 2001;12:13–21.
Heggie SJ, Wiseman MJ, Cannon GJ, et al. Defining the state of knowledge with respect to food, nutrition, physical activity, and the prevention of cancer. J Nutr. 2003;133(11 Suppl 1):3837S–42S. https://doi.org/10.1093/jn/133.11.3837S.
Dudekula A, Rachakonda V, Shaik B, et al. Weight loss in nonalcoholic fatty liver disease patients in an ambulatory care setting is largely unsuccessful but correlates with frequency of clinic visits. PLoS One. 2014;9:e111808.
Colquitt JL, Pickett K, Loveman E, et al. Surgery for weight loss in adults. Cochrane Database Syst Rev. 2014;(8):CD003641. https://doi.org/10.1002/14651858.CD003641.pub4.
Rapp K, Schroeder J, Klenk J, et al. Obesity and incidence of cancer: a large cohort study of over 145,000 adults in Austria. Br J Cancer. 2005;93:1062–7.
Yang B, Yang HP, Ward KK, et al. Bariatric surgery and liver cancer in a consortium of academic medical centers. Obes Surg. 2016;26:696–700.
Lam PH, Obirieze AC, Ortega G, et al. Characterization of hepatitis B and C among liver transplant recipients with hepatocellular carcinoma: an analysis of the nationwide inpatient sample database. Transplant Proc. 2016;48:123–7.
McCarty TR, Echouffo-Tcheugui JB, Lange A, et al. Impact of bariatric surgery on outcomes of patients with nonalcoholic fatty liver disease: a nationwide inpatient sample analysis, 2004-2012. Surg Obes Relat Dis. 2018;14:74–80.
Sharma P, McCarty TR, Njei B. Impact of bariatric surgery on outcomes of patients with inflammatory bowel disease: a nationwide inpatient sample analysis, 2004–2014. Obes Surg. 2018;28(4):1015–24. https://doi.org/10.1007/s11695-017-2959-0.
Abbas A, Medvedev S, Shores N, et al. Epidemiology of metastatic hepatocellular carcinoma, a nationwide perspective. Dig Dis Sci. 2014;59:2813–20.
Deyo RA, Cherkin DC, Ciol MA. Adapting a clinical comorbidity index for use with ICD-9-CM administrative databases. J Clin Epidemiol. 1992;45:613–9.
Austin PC. Statistical criteria for selecting the optimal number of untreated subjects matched to each treated subject when using many-to-one matching on the propensity score. Am J Epidemiol. 2010;172:1092–7.
Funk MJ, Westreich D, Wiesen C, et al. Doubly robust estimation of causal effects. Am J Epidemiol. 2011;173:761–7.
Hales CM, Fryar CD, Carroll MD, et al. Trends in obesity and severe obesity prevalence in US youth and adults by sex and assge, 2007–2008 to 2015–2016. JAMA. 2018;319(16):1723–25. https://doi.org/10.1001/jama.2018.3060.
Marengo A, Rosso C, Bugianesi E. Liver cancer: connections with obesity, fatty liver, and cirrhosis. Annu Rev Med. 2016;67:103–17.
Larsson SC, Wolk A. Overweight, obesity and risk of liver cancer: a meta-analysis of cohort studies. Br J Cancer. 2007;97:1005–8.
Hassan MM, Abdel-Wahab R, Kaseb A, et al. Obesity early in adulthood increases risk but does not affect outcomes of hepatocellular carcinoma. Gastroenterology. 2015;149:119–29.
Schutte K, Balbisi F, Malfertheiner P. Prevention of hepatocellular carcinoma. Gastrointest Tumors. 2016;3:37–43.
Sun B, Karin M. Obesity, inflammation, and liver cancer. J Hepatol. 2012;56:704–13.
Reeves HL, Zaki MY, Day CP. Hepatocellular carcinoma in obesity, type 2 diabetes, and NAFLD. Dig Dis Sci. 2016;61:1234–45.
Font-Burgada J, Sun B, Karin M. Obesity and Cancer: the oil that feeds the flame. Cell Metab. 2016;23:48–62.
Sakai H, Shirakami Y, Shimizu M. Chemoprevention of obesity-related liver carcinogenesis by using pharmaceutical and nutraceutical agents. World J Gastroenterol. 2016;22:394–406.
Shimizu M, Tanaka T, Moriwaki H. Obesity and hepatocellular carcinoma: targeting obesity-related inflammation for chemoprevention of liver carcinogenesis. Semin Immunopathol. 2013;35:191–202.
Bougoulia M, Triantos A, Koliakos G. Effect of weight loss with or without orlistat treatment on adipocytokines, inflammation, and oxidative markers in obese women. Hormones (Athens). 2006;5:259–69.
Colquitt JL, Picot J, Loveman E, et al. Surgery for obesity. Cochrane Database Syst Rev. 2009;(2):CD003641. https://doi.org/10.1002/14651858.CD003641.pub3.
Sjostrom L, Narbro K, Sjostrom CD, et al. Effects of bariatric surgery on mortality in Swedish obese subjects. N Engl J Med. 2007;357:741–52.
Fischer L, Hildebrandt C, Bruckner T, et al. Excessive weight loss after sleeve gastrectomy: a systematic review. Obes Surg. 2012;22:721–31.
Khan S, Rock K, Baskara A, et al. Trends in bariatric surgery from 2008 to 2012. Am J Surg. 2016;211:1041–6.
O'Brien PE, McPhail T, Chaston TB, et al. Systematic review of medium-term weight loss after bariatric operations. Obes Surg. 2006;16:1032–40.
Phillips E, Ponce J, Cunneen SA, et al. Safety and effectiveness of realize adjustable gastric band: 3-year prospective study in the United States. Surg Obes Relat Dis. 2009;5:588–97.
Davila JA, El-Serag H. The rising incidence of hepatocellular carcinoma in the United States: an update. Gastroenterology. 2012;142(5):Supp 1:S–914.
Saunders D, Seidel D, Allison M, et al. Systematic review: the association between obesity and hepatocellular carcinoma - epidemiological evidence. Aliment Pharmacol Ther. 2010;31:1051–63.
Financial Support
This study is financially supported by NIH 5 T32 DK 7356-37 (BN).
Author information
Authors and Affiliations
Contributions
Study concept and design—Njei B, McCarty TR, and Sharma P
Paper preparation—Njei B, McCarty TR, and Sharma P
Statistical analysis—Njei B
Critical revisions—McCarty TR, Sharma P, Lange A, Najafian N, Ngu JN, VE Ngomba, Echouffo-Tcheugui JB
Corresponding author
Ethics declarations
All authors approved of the final version of the manuscript.
This article has not been published and is not under consideration elsewhere.
Conflict of Interest
The authors declare that they have no conflicts of interest.
Ethical Approval Statement
For this type of study formal consent is not required.
Informed Consent Statement
Does not apply.
STROBE Statement
All checklist items for cross-sectional studies have been completed.
Additional information
Basile Njei, Thomas R. McCarty, and Prabin Sharma are co-first authors
Electronic supplementary material
Supplemental Figure 1
Graph of Propensity Score Densities before and after 1:1 Fixed Ratio nearest Neighbor Matching (PNG 1113 kb)
Rights and permissions
About this article
Cite this article
Njei, B., McCarty, T.R., Sharma, P. et al. Bariatric Surgery and Hepatocellular Carcinoma: a Propensity Score-Matched Analysis. OBES SURG 28, 3880–3889 (2018). https://doi.org/10.1007/s11695-018-3431-5
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11695-018-3431-5