Abstract
Background
Average percent excess weight loss data is commonly discussed preoperatively to guide patient expectations following surgery. However, there is a wide range and variation in weight loss following vertical sleeve gastrectomy (SG). Unfortunately, most surgeons and even fewer patients have heard of using predictive models to help guide their decisions on procedure choice. We have developed a predictive model for SG to help patient choice prior to this major life-changing decision.
Objective
Predict weight loss results for SG patients at 1 year using preoperative data.
Setting
Private practice.
Methods
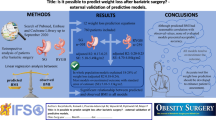
Three hundred and seventy-one SG patients met the criteria for our study. These patients underwent surgery between October 2008 and June 2016. Non-linear regressions were performed to interpolate individual patient weights at 1 year. Multivariate analysis was used to find factors that affected weight loss. A model was constructed to predict weight loss performance.
Results
Variables that affect weight loss were found to be preoperative body mass index (BMI), age, hypertension, and diabetes. Diabetes and hypertension together were found to significantly affect weight loss.
Conclusion
Patient weight loss can be accurately predicted by simple preoperative factors. These findings should be used to help patients and surgeons decide if the SG is an appropriate surgery for each patient. Using this model, most patients can avoid failure by choosing an appropriate surgical approach for their personal circumstances.
Similar content being viewed by others
References
Esteban Varela J, Nguyen NT. Laparoscopic sleeve gastrectomy leads the U.S. utilization of bariatric surgery at academic medical centers. Surg Obes Relat Dis. 2015;11(5):987–90. https://doi.org/10.1016/j.soard.2015.02.008.
Cottam A, Billing J, Cottam D, et al. Long-term success and failure with sleeve gastrectomy is predictable by 3 months: a multivariate model using simple office markers. Surg Obes Relat Dis. 2017;13(8):1266–70. https://doi.org/10.1016/j.soard.2017.03.016.
Manning S, Pucci A, Carter NC, et al. Early postoperative weight loss predicts maximal weight loss after sleeve gastrectomy and Roux-en-Y gastric bypass. Surg Endosc. 2015;29(6):1484–91. https://doi.org/10.1007/s00464-014-3829-7.
Hansen N, Hardin E, Bates C, et al. Preoperative change in 6-minute walk distance correlates with early weight loss after sleeve gastrectomy. JSLS. 2014;18(3):e2014.00383. https://doi.org/10.4293/JSLS.2014.00383.
Gras-Miralles B, Haya JR, Moros JM, et al. Caloric intake capacity as measured by a standard nutrient drink test helps to predict weight loss after bariatric surgery. Obes Surg. 2014;24(12):2138–44. https://doi.org/10.1007/s11695-014-1306-y.
Goitein D, Zendel A, Westrich G, et al. Postoperative swallow study as a predictor of intermediate weight loss after sleeve gastrectomy. Obes Surg. 2013;23(2):222–5. https://doi.org/10.1007/s11695-012-0836-4.
Ortega E, Morínigo R, Flores L, et al. Predictive factors of excess body weight loss 1 year after laparoscopic bariatric surgery. Surg Endosc. 2012;26(6):1744–50. https://doi.org/10.1007/s00464-011-2104-4.
Otto M, Kautt S, Kremer M, et al. Handgrip strength as a predictor for post bariatric body composition. Obes Surg. 2014;24(12):2082–8. https://doi.org/10.1007/s11695-014-1299-6.
Käkelä P, Jääskeläinen T, Torpström J, et al. Genetic risk score does not predict the outcome of obesity surgery. Obes Surg. 2014;24(1):128–33. https://doi.org/10.1007/s11695-013-1080-2.
Balasar Ö, Çakır T, Erkal Ö, et al. The effect of rs9939609 FTO gene polymorphism on weight loss after laparoscopic sleeve gastrectomy. Surg Endosc. 2016;30(1):121–5. https://doi.org/10.1007/s00464-015-4169-y.
Weiner RA, Weiner S, Pomhoff I, et al. Laparoscopic sleeve gastrectomy--influence of sleeve size and resected gastric volume. Obes Surg. 2007;17(10):1297–305.
Spivak H, Rubin M, Sadot E, et al. Laparoscopic sleeve gastrectomy using 42-French versus 32-French bougie: the first-year outcome. Obes Surg. 2014;24(7):1090–3. https://doi.org/10.1007/s11695-014-1199-9.
Hawasli A, Jacquish B, Almahmeed T, et al. Early effects of bougie size on sleeve gastrectomy outcome. Am J Surg. 2015;209(3):473–7. https://doi.org/10.1016/j.amjsurg.2014.10.011.
Becouarn G, Topart P, Ritz P. Weight loss prior to bariatric surgery is not a pre-requisite of excess weight loss outcomes in obese patients. Obes Surg. 2010;20(5):574–7. https://doi.org/10.1007/s11695-010-0083-5.
Dilektasli E, Erol MF, Cayci HM, et al. Low educational status and childhood obesity associated with insufficient mid-term weight loss after sleeve gastrectomy: a retrospective observational cohort study. Obes Surg. 2017;27(1):162–8. https://doi.org/10.1007/s11695-016-2273-2.
Mackey ER, Olson A, Merwin S, et al. Perceived social support for exercise and weight loss in adolescents undergoing sleeve gastrectomy. Obes Surg. 2017;28:421–6. https://doi.org/10.1007/s11695-017-2853-9.
Kulendran M, Borovoi L, Purkayastha S, et al. Impulsivity predicts weight loss after obesity surgery. Surg Obes Relat Dis. 2017;13(6):1033–40. https://doi.org/10.1016/j.soard.2016.12.031.
Figura A, Ahnis A, Stengel A, et al. Determinants of weight loss following laparoscopic sleeve gastrectomy: the role of psychological burden, coping style, and motivation to undergo surgery. J Obes. 2015;2015:1–10. https://doi.org/10.1155/2015/626010.
Pekkarinen T, Mustonen H, Sane T, et al. Long-term effect of gastric bypass and sleeve gastrectomy on severe obesity: do preoperative weight loss and binge eating behavior predict the outcome of bariatric surgery? Obes Surg. 2016;26(9):2161–7. https://doi.org/10.1007/s11695-016-2090-7.
Lemanu DP, Singh PP, Rahman H, et al. Five-year results after laparoscopic sleeve gastrectomy: a prospective study. Surg Obes Relat Dis. 2015;11(3):518–24. https://doi.org/10.1016/j.soard.2014.08.019.
Cottam D, Qureshi FG, Mattar VSG, et al. Laparoscopic sleeve gastrectomy as an initial weight-loss procedure for high-risk patients with morbid obesity. Surg Endosc. 2006;20(6):859–63.
Gibson SC, Le Page PA, Taylor CJ. Laparoscopic sleeve gastrectomy: review of 500 cases in single surgeon Australian practice. ANZ J Surg. 2015;85(9):673–7. https://doi.org/10.1111/ans.12483.
Rawlins L, Rawlins MP, Brown CC, et al. Sleeve gastrectomy: 5-year outcomes of a single institution. Surg Obes Relat Dis. 2013;9(1):21–5. https://doi.org/10.1016/j.soard.2012.08.014.
Yaghoubian A, Tolan A, Stabile BE, et al. Laparoscopic Roux-en-Y gastric bypass and sleeve gastrectomy achieve comparable weight loss at 1 year. Am Surg. 2012;78(12):1325–8.
Martin DJ, Lee CM, Rigas G, et al. Predictors of weight loss 2 years after laparoscopic sleeve gastrectomy. Asian J Endosc Surg. 2015;8(3):328–32. https://doi.org/10.1111/ases.12193.
Contreras JE, Santander C, Court I, et al. Correlation between age and weight loss after bariatric surgery. Obes Surg. 2013;23(8):1286–9. https://doi.org/10.1007/s11695-013-0905-3.
Benoit SC, Hunter TD, Francis DM, et al. Use of bariatric outcomes longitudinal database (BOLD) to study variability in patient success after bariatric surgery. Obes Surg. 2014;24(6):936–43. https://doi.org/10.1007/s11695-014-1197-y.
DuPree CE, Blair K, Steele SR, et al. Laparoscopic sleeve gastrectomy in patients with preexisting gastroesophageal reflux disease: a national analysis. JAMA Surg. 2014;149(4):328–34. https://doi.org/10.1001/jamasurg.2013.4323.
Andersen JR, Aadland E, Nilsen RM, et al. Predictors of weight loss are different in men and women after sleeve gastrectomy. Obes Surg. 2014;24(4):594–8. https://doi.org/10.1007/s11695-013-1124-7.
de Raaff CA, Bindt DM, de Vries N, et al. Positional obstructive sleep apnea in bariatric surgery patients: risk factor for postoperative cardiopulmonary complications? Sleep Breath. 2016;20(1):113–9. https://doi.org/10.1007/s11325-015-1192-0.
Perugini RA, Mason R, Czerniach DR, et al. Predictors of complication and suboptimal weight loss after laparoscopic Roux-en-Y gastric bypass: a series of 188 patients. Arch Surg. 2003;138(5):541–5. discussion 545-6
Hunter Mehaffey J, Turrentine FE, Miller MS, et al. Roux-en-Y gastric bypass 10 year follow-up: the found population. Surg Obes Relat Dis. 2016;12(4):778–82. https://doi.org/10.1016/j.soard.2015.11.012.
Goldenshluger A, Elazary R, Cohen MJ, et al. Predictors for adherence to multidisciplinary follow-up care after sleeve gastrectomy. Obes Surg. 2018; https://doi.org/10.1007/s11695-018-3296-7.
Abd Ellatif ME, Abdallah E, Askar W, et al. Long term predictors of success after laparoscopic sleeve gastrectomy. Int J Surg. 2014;12(5):504–8. https://doi.org/10.1016/j.ijsu.2014.02.008.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of Interest
Author one has no conflicts of interest to declare.
Author two, the corresponding author, reports personal fees from Medtronic, outside the submitted work.
Author three has no conflict of interest to declare.
Author four has no conflicts of interest to declare.
Author five has no conflicts of interest to declare.
Author six has no conflicts of interest to declare.
Statement of Human and Animal Rights
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards.
Since this is a retrospective study, formal consent is not required.
Rights and permissions
About this article
Cite this article
Cottam, S., Cottam, D., Cottam, A. et al. The Use of Predictive Markers for the Development of a Model to Predict Weight Loss Following Vertical Sleeve Gastrectomy. OBES SURG 28, 3769–3774 (2018). https://doi.org/10.1007/s11695-018-3417-3
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11695-018-3417-3