Abstract
Background
In bariatric surgery patients, weight loss and long-term weight maintenance are related to food intake and eating patterns. To improve the diet orientation in the bariatric surgery postoperative period, we assessed the postoperative eating patterns and related them to weight loss.
Methods
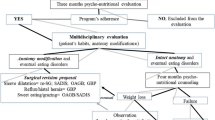
This was a transversal, analytical, and descriptive study that assessed body mass index (BMI) values and percentage of excess weight loss (%EWL) in patients who had undergone Roux-en-Y gastric bypass (RYGBP) surgery. The eating pattern and energy intake were investigated based on data collected through a 4-day food intake record. From these records, we assessed the number of daily meals, the quantity of food per meal, and calorie value of snacks between main meals. Based on these records, patients were classified under sweet-eating, snack-eating, or normal-eating patterns.
Results
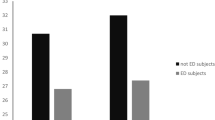
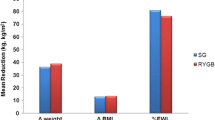
Seventy-five patients met our inclusion criteria. The normal-eating pattern group was the one with the greatest weight loss with an average %EWL of 71.4 ± 21%, followed by the sweet-eating pattern with 69.9 ± 16.8%, and the snack-eating pattern with 56.4 ± 16.7%. This difference was significant only between the first and the third group (p = 0.04). The snack-eating patients had the highest caloric intake and highest number of daily meals (p < 0.01).
Conclusion
Postoperative eating pattern influenced postbariatric surgery weight loss. In the present study, the snack-eating pattern was associated with the worst weight loss outcome, followed by the sweet-eating and normal-eating patterns. A screening and a differential approach to patients according to their eating patterns may lead to better results of weight loss.

Similar content being viewed by others
References
Colles SL, Dixon JB, O’Brien PE. Grazing and loss of control related to eating: two high-risk factors following bariatric surgery. Obesity 2008;16(3):615–22.
Togo P, Osler M, Sorensen TI. Food intake patterns and body mass index in observational studies. Int J Obes Relat Metab Disord 2001;25:1741–51.
Brolin RE, Robertson LB, Kenler HA, et al. Weight loss and dietary intake after vertical banded gastroplasty and Y-en-Roux gastric bypass. Ann Surg 1994;220(6):782–90.
Sugerman HJ, Kellum JM, Engle KM, et al. Gastric bypass for treating severe obesity. Am J Clin Nutr 1992;55:560S–6S.
Kenler HA, Brolin RE, Cody RP. Changes in eating behavior after horizontal gastroplasty and Roux-en-Y gastric bypass. Am J Clin Nutr 1990;52:87–92.
Shah M, Simha V, Garg A. Review: long-term impact of bariatric surgery on body weight, comorbidities and nutritional status. J Clin Endocrinol Metab 2006;91:4223–31.
Kolanowski J. Surgical treatment for morbid obesity. Br Med Bull 1997;53(2):433–44.
Andersen T, Pedersen BH. Pouch volume, stoma diameter, and clinical outcome after gastroplasty for morbid obesity. Scand J Gastroenterol 1984;19(5):643–9.
Metropolitan Life Foundation. Metropolitan height and weight tables. Metropolitan Life Foundation, Statistical Bulletin 1983;64(1):2–9.
Nutrisurvey. Available at http://www.nutrisurvey.de/. Accessed December 2002.
Moize V, Geliebter A, Gluck ME, et al. Obese patients have inadequate protein intake related to protein intolerance up to 1 year following Roux-en-Y gastric bypass. Obes Surg 2003;13:23–8.
Blake M, Fazio V, O’Brien P. Assessment of nutrient in association with weight loss after gastric restrictive procedures for morbid obesity. Aust N Z J Surg 1991;61:195–9.
Wardé-Kamar J, Rogers M, Flancbaum L, et al. Calorie intake and meal patterns up to 4 years after gastric bypass surgery. Obes Surg 2004;14:1070–9.
Saunders R. Grazing: a high risk behavior. Obes Surg 2004;14:98–102.
Kersten S. Mechanisms of nutritional and hormonal regulation of lipogenesis. EMBO Rep 2001;2(4):282–6.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Leite Faria, S., de Oliveira Kelly, E., Pereira Faria, O. et al. Snack-Eating Patients Experience Lesser Weight Loss after Roux-En-Y Gastric Bypass Surgery. OBES SURG 19, 1293–1296 (2009). https://doi.org/10.1007/s11695-008-9704-7
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11695-008-9704-7