Abstract
Background
Percutaneous cholecystostomy is frequently used as a treatment option for acute calculous cholecystitis in patients unfit for surgery. There is sparse evidence on the long-term impact of cholecystostomy on gallstone-related morbidity and mortality in patients with acute calculous cholecystitis. This study describes the long-term outcome of acute calculous cholecystitis following percutaneous cholecystostomy compared to conservative treatment.
Methods
This was a cohort study of patients admitted at our institution from 2006 to 2015 with acute calculous cholecystitis without early or delayed cholecystectomy. Endpoints were gallstone-related readmissions, recurrent cholecystitis, and overall mortality.
Results
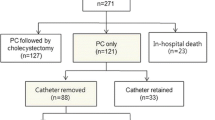
The investigation included 201 patients of whom 97 (48.2%) underwent percutaneous cholecystostomy. Patients in the cholecystostomy group had significantly higher age, comorbidity level, and inflammatory response at admission. The median duration of catheter placement in the cholecystostomy group was 6 days. The complication rate of cholecystostomy was 3.1% and the mortality during the index admission was 3.5%. The median follow-up was 1.6 years. The rate of gallstone-related readmissions was 38.6%, and 25.3% had recurrence of cholecystitis. Cox regression analyses revealed no significant differences in gallstone-related readmissions, recurrence of acute calculous cholecystitis, and overall mortality in the two groups.
Conclusions
Percutaneous cholecystostomy in the treatment of acute calculous cholecystitis was neither associated with long-term benefits nor complications. Based on the high gallstone-related readmission rates of this study population and todays perioperative improvements, we suggest rethinking the indications for non-operative management including percutaneous cholecystostomy in acute calculous cholecystitis.


Similar content being viewed by others
References
Okamoto K, Suzuki K, Takada T, et al. Tokyo Guidelines 2018 flowchart for the management of acute cholecystitis. J Hepatobiliary Pancreat Sci 2017. https://doi.org/10.1002/jhbp.516.
Itoi T, Tsuyuguchi T, Takada T, et al. TG13 indications and techniques for biliary drainage in acute cholangitis (with videos). J Hepatobiliary Pancreat Sci 2013; 20: 71–80.
Yamashita Y, Takada T, Kawarada Y, et al. Surgical treatment of patients with acute cholecystitis: Tokyo guidelines. J Hepatobiliary Pancreat Surg 2007; 14: 91–7.
Atar E, Bachar GN, Berlin S, et al. Percutaneous cholecystostomy in critically ill patients with acute cholecystitis: Complications and late outcome. Clin Radiol 2014; 69: e247–52.
Horn T, Christensen SD, Kirkegård J, Larsen LP, Knudsen AR, Mortensen F V. Percutaneous cholecystostomy is an effective treatment option for acute calculous cholecystitis: A 10-year experience. HPB (Oxford) 2015; 17: 326–31.
Zerem E, Omerović S. Can percutaneous cholecystostomy be a definitive management for acute cholecystitis in high-risk patients?. Surg Laparosc Endosc Percutaneous Tech 2014; 24: 187–91.
Granlund A, Karlson BM, Elvin A, Rasmussen I. Ultrasound-guided percutaneous cholecystostomy in high-risk surgical patients. Langenbeck’s Arch Surg 2001; 386: 212–7.
Sanjay P, Mittapalli D, Marioud A, White RD, Ram R, Alijani A. Clinical outcomes of a percutaneous cholecystostomy for acute cholecystitis: A multicentre analysis. Hpb 2013; 15: 511–6.
Smith TJ, Manske JG, Mathiason MA, Kallies KJ, Kothari SN. Changing trends and outcomes in the use of percutaneous cholecystostomy tubes for acute cholecystitis. Ann Surg 2013; 257: 1112–5.
Hatzidakis AA, Prassopoulos P, Petinarakis I, et al. Acute cholecystitis in high-risk patients: Percutaneous cholecystostomy vs conservative treatment. Eur Radiol 2002; 12: 1778–84.
Yokoe M, Takada T, Strasberg SM, et al. TG13 diagnostic criteria and severity grading of acute cholecystitis (with videos). J Hepatobiliary Pancreat Sci 2013; 20: 35–46.
Mazeh H, Mizrahi I, Dior U, et al. Role of antibiotic therapy in mild acute calculus cholecystitis: A prospective randomized controlled trial. World J Surg 2012;36:1750–59.
STROBE statement - Checklist of items that should be included in reports of observational studies (STROBE Initiative). Int J Public Health 2008; 53: 3–4.
Boland GW, Lee MJ, Leung J, Mueller PR. Percutaneous cholecystostomy in critically ill patients: Early response and final outcome in 82 patients. Am J Roentgenol 1994; 163: 339–42.
van Overhagen H, Meyers H, Tilanus HW, Jeekel J, Laméris JS. Percutaneous cholecystectomy for patients with acute cholecystitis and an increased surgical risk. Cardiovasc Intervent Radiol 1996; 19: 72–6.
Winbladh A, Gullstrand P, Svanvik J, Sandström P. Systematic review of cholecystostomy as a treatment option in acute cholecystitis. HPB (Oxford) 2009; 11: 183–93.
Ambe PC, Kaptanis S, Papadakis M, Weber SA, Jansen S, Zirngibl H. The treatment of critically Ill patients with acute cholecystitis. Dtsch Arztebl Int 2016; 113: 545–51.
Loozen CS, Van Ramshorst B, Van Santvoort HC, Boerma D. Early cholecystectomy for acute cholecystitis in the elderly population: A systematic review and meta-analysis. Dig. Surg 2017; 34: 371–9.
Kortram K, van Ramshorst B, Bollen TL, et al. Acute cholecystitis in high risk surgical patients: percutaneous cholecystostomy versus laparoscopic cholecystectomy (CHOCOLATE trial): study protocol for a randomized controlled trial. Trials 2012; 13: 7.
Paajanen H. Laparoscopic cholecystectomy or conservative treatment in the acute cholecystitis of the elderly patients. November 25, 2016. Available at: https://clinicaltrials.gov/ct2/show/NCT02972944?term=paajanen&rank=7. Accessed September 07, 2018
Author information
Authors and Affiliations
Contributions
Stine Ydegaard Turiño, Daniel Mønsted Shabanzadeh, Lars Tue Sørensen, Lars Nannestad Jørgensen: Conception or design of the work.
Stine Ydegaard Turiño, Daniel Mønsted Shabanzadeh, Nethe Malik Eichen, Stine Lundgaard Jørgensen: Acquisition, analysis of the work.
Stine Ydegaard Turiño, Daniel Mønsted Shabanzadeh, Lars Nannestad Jørgensen: Interpretation of data for the work.
Stine Ydegaard Turiño, Daniel Mønsted Shabanzadeh, Nethe Malik Eichen, Stine Lundgaard Jørgensen, Lars Tue Sørensen, Lars Nannestad Jørgensen: Drafting the work or revising it critically for important intellectual content.
Stine Ydegaard Turiño, Daniel Mønsted Shabanzadeh, Nethe Malik Eichen, Stine Lundgaard Jørgensen, Lars Tue Sørensen, Lars Nannestad Jørgensen: Final approval of the version to be published.
Agreement to be accountable for all aspects of the work in ensuring that questions related to the accuracy or integrity of any part of the work are appropriately investigated and resolved: Stine Ydegaard Turiño, Daniel Mønsted Shabanzadeh, Nethe Malik Eichen, Stine Lundgaard Jørgensen, Lars Tue Sørensen, Lars Nannestad Jørgensen.
Corresponding author
Additional information
This study was delivered as an oral presentation at the Annual Meeting of the Danish Surgical Society, 10 November 2017, Copenhagen.
Rights and permissions
About this article
Cite this article
Turiño, S.Y., Shabanzadeh, D.M., Eichen, N.M. et al. Percutaneous Cholecystostomy Versus Conservative Treatment for Acute Cholecystitis: a Cohort Study. J Gastrointest Surg 23, 297–303 (2019). https://doi.org/10.1007/s11605-018-4021-5
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11605-018-4021-5